Dr Rajiv Desai
An Educational Blog
EXERCISE
EXERCISE:
_
_
Prologue:
The big four “proximate” causes of preventable ill-health are: smoking, poor nutrition, lack of physical activity and alcohol excess. Of these, the importance of regular exercise is the least well-known. However, exercise is not a new concept. In 300 BC, Aristotle suggested that “a man falls into ill health as a result of not caring for exercise.” These factors (smoking, nutrition, lack of physical activity and alcohol) are often described as lifestyle choices, yet many people do not have the finances, self-efficacy, environment or knowledge to be able to practice lifestyle choices correctly. We have moved towards a sedentary society with changing work and domestic habits & patterns. We now drive cars, sit in front of computers or TVs and use domestic appliances. There are far fewer manual jobs. This means that physical activity is not routine for most people. In 1949, 34% of miles travelled using mechanical modes were by bicycle; today only 1-2% are. Now half of all adults spend more than 5 hours sedentary every day. Being active has enormous health and well-being benefits. Physical activity is important in the management of long-term diseases, but it is even more important in the prevention of many other common diseases. Over 50% of adults do not reach the minimum recommended level of 30 minutes of moderate intensity exercise five times per week. The exercise should be moderate enough to get a person slightly out of breath and/or sweaty, and with an increased heart rate. Those achieving even this minimum level of activity can reduce their risk of developing heart disease, stroke, dementia, diabetes and some cancers by at least 30%. This is better than many drugs. The need to encourage individuals to participate in physical activity has never been greater. A society-wide increase in moderate physical activity could help reduce health inequalities and improve physical as well as mental health. There are greater intangible costs too, to individuals, families and communities. I have already discussed nicotine addiction, alcohol and food in my earlier articles and exercise was also discussed briefly in my articles on obesity, yoga and diabetes. Today I dedicate full article on exercise.
______
Note:
Exercise means physical exercise in this article. Physical fitness means health related physical fitness in this article. It is beyond the scope of this article to discuss in detail specific exercise to prevent or treat specific illness. It is also beyond the scope of this article to discuss sports. All I discuss is utility of exercise to common man and scientific basis of exercise.
_____
Better to hunt in fields, for health unbought,
Than fee the doctor for a nauseous draught,
The wise, for cure, on exercise depend;
God never made his work for man to mend.
John Dryden
_
Life is like riding a bicycle—in order to keep your balance, you must keep moving.
Albert Einstein
______
______
History of exercise:
_
Prehistoric period:
Hominids—human beings and their immediate ancestors—have existed on Earth for at least 2,000,000 years. For more than 99 percent of that time, hominids lived a nomadic existence and survived by hunting and gathering food. It is obvious that this way of life was enormously different from the way people live today in developed countries. Thus, evolutionary history has prepared humankind for one kind of life, but modern people lead another. This fact has profound implications for patterns of disease and for the association between living habits and health. Observation of the few remaining nomadic groups in the world indicates that they are relatively free of chronic diseases and that, in comparison to the populations in developed countries, they are leaner, have a higher level of physical fitness, eat a very different diet, and have different physical activity patterns. Data from the distant past are not available, but it is reasonable to speculate that early humans had considerably higher caloric expenditures per unit of body weight than do modern individuals.
_
The exercise prescription for health and disease prevention has roots that began in antiquity more than two millennia ago. According to medical historians such as Gordon and Lyons and Petrucelli, breathing exercises, regarded as medical gymnastics, were being practiced in China as early as 2600 BCE. During the era of the Yellow Emperor (1050–256 BCE), these exercises were used for subjects experiencing chills, fevers, or complete paralysis. In addition, massage with exercise of the extremities was also being recommended. During this same time period, the yin-yang doctrine was prevalent, with yang being identified with life and health, whereas disease and death were associated with yin. Susruta of India was the first “recorded” physician to prescribe moderate daily exercise, Hippocrates of Greece was the first “recorded” physician to provide a written exercise prescription for a patient suffering from consumption, and Galen from Rome recommended the use of exercise for patients in the management of disease. Susruta was the first recorded physician to prescribe exercise for his patients and to indicate that “it should be taken every day” but taken “only to half extent of his capacity” as otherwise “it may prove fatal”. In addition, before prescribing exercise, it was essential for the physician to consider the age, strength, physique, exercise terrain, and diet of the patient. Susruta advocated exercise because it made the body stout, strong, firm, compact, and light, enhanced the growth of limbs and muscles, improved digestion and complexion, prevented laziness, and reduced senility while being “absolutely conducive to a better preservation of health”. Hippocrates (460–370 BCE) wrote that “eating alone will not keep a man well, he must also take exercise”. Hippocrates also stated that “. . . food and exercise, while possessing opposite qualities, yet work together to produce health”. Although Hippocrates was not the first physician to prescribe exercise for patients, he was the first recorded physician to provide a written exercise prescription for a patient suffering from consumption. Specifically, in Diseases III and internal affections, Hippocrates provided a detailed written exercise prescription of walking for a patient with consumption. To Galen, work and exercise were equivalent terms, whereas motion had to be vigorous and cause labored breathing if it was to be designated as exercise. He classified exercise as being slow, swift, atony, vigorous, gentle, and violent; select examples are as follows: running was swift, lifting a heavy weight was vigorous, and continuous jumping was violent. However, if exercise was to be prescribed for health reasons, it was to be moderate. Of the exercises being mentioned, Galen’s favourite exercise comprised games in which a small ball was used. Historically intertwined with these concepts was exercise being advocated by select physicians to minimize the health problems associated with obesity, diabetes, and inactivity. Hippocrates wrote the following: “All parts of the body, if used in moderation and exercised in labors to which each is accustomed, become thereby healthy and well developed and age slowly; but if they are unused and left idle, they become liable to disease, defective in growth and age quickly.” With the decline of the Hellenic civilization, this concept faded. For centuries, physical activity and fitness were considered largely for military purposes and associated with youth sports and athletics even through the post–World War II era.
_
Movement or locomotion is perhaps the most meaningful behavior animals engage in. Humans are no exception, and approximately 2 million years ago evolved an ability to run sustained long distances. Independent of the necessity to procure food or find reproductive partners, it has been well documented that humans and mammals frequently engage in play behavior, or specifically within human populations – leisure time activity or “sport.” The need for or social implications of play behavior are beyond the scope of this article. A more relevant aspect is the importance of play behavior in facilitating exercise training, which may allow individuals to acclimatize to physical activity. Regardless of the specific benefits of physical activity or exercise, organized sport has perhaps always had a place in human society. Although the relative importance of sport or leisure physical activity and its perceived impact on the body has fluctuated over time, exercise, and specifically jogging, became a cultural phenomenon in the late 1960s and 1970s. This sensation was initiated and perpetuated by promotion of the health benefits of physical activity programs accessible to all ages, and marketing and profits related to promotion of sport. In addition to running, over the past four decades enormous volumes of heath-centered programs (both psychological and physiological) based on a variety of activities have seen gains in popularity. Ironically, as insights into the benefits of regular physical activity have increased dramatically since inception of the jogging revolution, total physical activity has been on a global downward trend since 1965. Today many people remain largely inactive; some are only irregularly active, whereas others do engage in enough activity to realize the health benefits.
________
Exercise in animals:
Physical exercise has been shown to benefit a wide range of other mammals, as well as salmon, juvenile crocodiles, and at least one species of bird. However, several studies have shown that lizards display no benefit from exercise, leading them to be termed “metabolically inflexible”. Regular exercise is important to avoid illness and encourage normal behaviour patterns in most pet animals. If you accept the responsibility of keeping a pet you must appreciate that, for most animals, regular exercise is very important for their well-being. To deny an animal the space and opportunity it needs to exercise can result in abnormal behavioural patterns as well as ill health. Reptiles and insects are a few of the species which prefer confined spaces and do not take the opportunity to exercise if allowed to do so.
_
Typical examples of pets being deprived of exercise are:
•cats kept in flats – where there is simply no opportunity for them to exercise properly
•dog owners who work all day and play at nights and weekends – without building an exercise period for their dog into their daily routine
•rabbits and guinea pigs that are kept confined to a cage or hutch all year round without access to an exercise run
•hamsters that are kept in a small cage and not provided with a wheel or an exercise ball, and
•birds without enough flight space in their cage.
_
Studies in humans have clearly shown the psychological and physical benefits of regular exercise, resulting in an improved quality of life, reduced susceptibility to illness and increased life-span. Exercise is important as it allows our pets to express their normal instinctive behavioural traits including inquisitive exploration, the use of scent, sight and hearing, tracking, stalking, play-fighting, play-defensive behaviour, hiding, attacking, chasing, greeting members of the same species, dealing with strange objects and dealing with animals from different species. Exercise also encourages the development of a normal daily toilet routine. Cats and dogs deprived of regular exercise and confined to the home may develop anti-social behaviour patterns including destructive behaviour, aggressive territorial guarding, house soiling and vocalisation when left alone without human companionship. A degree of exercise (but not excessive exercise) is needed for normal muscular and skeletal development in young, growing animals. Animals deprived of exercise will develop poor muscle conformation (due to muscle atrophy) and a sedentary life-style which will predispose them to develop obesity and other disorders. The most common adverse effect of insufficient exercise is obesity and all pets can develop this if they are fed too many calories. Millions of pet dogs, cats, rabbits, guinea pigs, hamsters, rats, ponies and birds (which are “loved” by their owners) are obese simply because owners do not control calorie intake and provide insufficient exercise, or because they have encouraged or enforced the development of a sedentary lifestyle. Obesity has all sorts of negative effects on the body – and it can make various diseases worse (e.g. heart disease, orthopaedic disease, skin disease). Obesity also plays an important role in the cause of some common diseases – including diabetes mellitus.
_
Physical inactivity reduced life span of elephant by third:
Elephants born and raised in zoos live less than half as long as those living in their native Africa and Asia, despite being protected from predators and having better care, according to one of the reports. Many of the deaths are thought to be linked to obesity, because the animals are well fed but get very little exercise in their small enclosures. Scientists also blamed high stress levels, which the animals suffer most after being transferred between zoos and being separated from their mothers. Scientists called on zoos to introduce immediate health checks on elephants to identify obese and stressed animals. In one study, researchers led by Ros Clubb, a wildlife scientific officer at the Royal Society for the Prevention of Cruelty to Animals, analysed records of 786 Asian and African female elephants kept in European zoos between 1960 and 2005. They then compared the lifespans of the captive animals with Asian elephants used by a logging company in Burma, and African elephants living in the Amboseli national park in Kenya. Asian elephants born in captivity typically lived for 18.9 years, while those used as working animals in Burma survived for 41.7 years. African elephants also fared worse, living for 16.9 years in captivity and 35.9 years in the wild. When the scientists discounted African elephants killed by people in the national park, the typical lifespan reached 56 years, more than three times as long as those kept in zoos. “You would expect captive elephants to live at least as long, if not longer, than those in the wild because they are better cared for, but that is not the case. The difference is massive,” said Clubb, whose study appears in the US journal Science. A second report, commissioned by the Department for Environment, Food and Rural Affairs, examined the welfare of 77 elephants in 13 UK zoos. It found that the animals spent 83% of their time indoors and 71 were overweight. Only 11 were able to walk normally. “We often hear that zoos play a vital role in conserving elephants but patently this is not the case,” said Rob Atkinson, head of wildlife science at the RSPCA. “The new data shows elephants die young in Europe’s zoos, and those Asian elephants born in captivity have a poor chance of survival. Surely the way forward is to encourage conservation programmes in native habitats rather than condemn elephants to a shortened and unhealthy existence in our zoos.” He added: “Elephants are having a torrid time in our zoos, judging by this overwhelming evidence, and action must be taken to alleviate their welfare problems as a matter of urgency.” Zoo enclosures for elephants are typically 60 to 100 times smaller than the smallest wild territories. African elephants can roam over 2,000 square miles, and Asian elephants 300 square miles. In captivity, researchers said, elephants are also at risk from infanticide, tuberculosis, herpes and lameness.
_________
_________
Introduction to exercise:
Physical exercise is any bodily activity that enhances or maintains physical fitness and overall health and wellness. It is performed for various reasons, including strengthening muscles and the cardiovascular system, honing athletic skills, weight loss or maintenance, and merely enjoyment. Frequent and regular physical exercise boosts the immune system and helps prevent the “diseases of affluence” such as cardiovascular disease, Type 2 diabetes, and obesity. It may also help prevent depression, help to promote or maintain positive self-esteem, improve mental health generally, and can augment an individual’s sex appeal or body image, which has been found to be linked with higher levels of self-esteem. To enjoy a long and healthy life, everyone should make lifestyle choices that include a healthy diet, regular exercise, and maintaining normal weight. The combination of inactivity and eating the wrong foods is the second most common preventable cause of death in the United States (smoking is the first). Most research on the benefits of exercise focuses on heart protection. Studies clearly show that exercise helps the heart. In addition, studies are reporting that even people with heart disease may gain important benefits from exercising, though they need medical clearance and special precautions. Childhood obesity is a growing global concern, and physical exercise may help decrease some of the effects of childhood and adult obesity. Health care providers often call exercise the “miracle” or “wonder” drug—alluding to the wide variety of proven benefits that it can provide.
_
Appropriate exercise improves muscular strength and endurance, body composition, flexibility, and cardiorespiratory endurance. The level of maximal oxygen intake or cardiorespiratory endurance is not by itself of great importance to most individuals. What is important is that one’s sustained energy-spending ability is directly related to maximal levels of performance. For example, consider the simple task of walking at a rate of three miles per hour. This task involves an energy expenditure of approximately three times the resting metabolic rate. Extremely unfit individuals may have a maximal aerobic power of only six times their resting metabolic rate. For such individuals, a three-mile-per-hour walk requires half of their maximal capacity. A middle-aged person who exercises regularly will have a maximal aerobic power 10 to 12 times resting, so the same walk will represent only 25 to 30 percent of maximal capacity. This example illustrates how any submaximal task is relatively much easier for the conditioned individual. Moreover, a person cannot work throughout the day at much more than about 20 percent of maximal capacity without becoming chronically fatigued. The deconditioned person who has a maximal aerobic power of six times resting can comfortably sustain a work level of only about 1.2 times resting throughout the day (6 × 0.20 = 1.2). This low capability for sustained energy expenditure can support only a very sedentary existence: for example, 20 hours of sleep and rest, two hours of personal care, one hour of housework and shopping, and one hour of activity at three times the resting rate each day. The point of the preceding discussion is that the average energy-expenditure requirement of anyone’s life can be calculated, and a person’s maximal cardiorespiratory endurance determines how active a life-style can be sustained. Individuals who attempt to lead more active lives than their fitness level will support become chronically fatigued. Persons with adequate or optimal fitness levels, on the other hand, are able to meet the physical demands of an active life relatively easily. One of the most frequent observations made by individuals who have begun an exercise program is that they feel better, and research studies document an improvement in feelings of general well-being in more active people.
_
The health benefits of regular participation in sports and aerobic fitness have been well recognized for more than 30 years. However, over the past decade new scientific evidence has shown that physical activity need not be strenuous to be beneficial to health. In fact, 30 minutes of moderate-intensity physical activity every day or on most days of the week provides important health benefits. This modest but regular amount of activity can greatly reduce or prevent the risk of cardiovascular disease, type 2 diabetes, osteoporosis, colon cancer, and breast cancer. Regular, moderate physical activity, including daily activities such as climbing stairs, brisk walking, and biking, can reduce stress, alleviate depression and anxiety, enhance self-esteem, and increase mental alertness. Moreover, school-age children who are regularly active demonstrate enhanced school performance and a better sense of personal and social responsibility than those who are more sedentary.
_
The benefits of exercise include:
•Decreased risk of cardiovascular (heart) disease, high blood pressure, and stroke
•Decreased risk of colon and breast cancers
•Decreased risk of diabetes
•Decreased risk of osteoporosis
•Decreased risk of depression and dementia
•Decreased body fat
•Improved metabolic processes — the way the body breaks down and builds necessary substances
•Improved movement of joints and muscles
•Improved oxygen delivery throughout the body
•Improved sense of well-being
•Improved strength and endurance
In addition, exercise can help change other dangerous lifestyle habits. A 2007 review of existing studies found that moderate exercise, for as little as 5 minutes at a time, can help combat the nicotine withdrawal symptoms people have when they try to stop smoking. No one is too young or too old to exercise. The United States Surgeon General recommends at least 30 minutes of moderate exercise, such as brisk walking, nearly every day.
_
Couch potato:
While the term couch potato usually refers to a lazy person who prefers to just sit around and watch TV, an active couch potato refers to someone who is inactive for the majority of the day, but regularly makes sure to get in 30 minutes of exercise on most days. An active couch potato is not necessarily lazy, but spend most of his or her time sitting during leisure time, work (and commuting to and from work) and while eating meals. In other words, they’re almost completely physically inactive throughout the day, with the exception of that 30 or minutes of daily exercise. Although 30 minutes of exercise is absolutely beneficial and healthful, the rest of the day is causing tremendous health hazards. In fact, the World Health Organization (WHO) has identified physical inactivity as an independent risk factor for chronic disease development, and it is now the fourth leading cause of death worldwide.
_
_
Sedentary lifestyle:
A sedentary lifestyle is a type of lifestyle with no or irregular physical activity. A person who lives a sedentary lifestyle may colloquially be known as a slob or couch potato. It is commonly found in both the developed and developing world. Sedentary activities include sitting, reading, watching television, playing video games, and computer use for much of the day with little or no vigorous physical exercise. A sedentary lifestyle can contribute to many preventable causes of death. Screen time is the amount of time a person spends watching a screen such as a television, computer monitor, or mobile device. Excessive screen time is linked to negative health consequences.
_
Sedentary behaviour:
_
Myth: You have to be athletic to exercise.
Fact: Most physical activities don’t require any special athletic skills. In fact, many people who have bad memories of difficult school sports have discovered a whole world of enjoyable, healthful activities that involve no special talent or training. A perfect example is brisk walking—a superb, heart healthy activity. Others include bicycling, gardening, or yard work, as long as they’re done at a brisk pace. Just do more of the activities you already like and already know how to do. It’s that simple.
_
What are some tips to help me get moving?
•If you can’t set aside one block of time, do short activities throughout the day, such as three 10-minute walks.
•Create opportunities for activity. Try parking your car farther away from where you are headed. If you ride the bus or train, get off one or two stops early and walk.
•Walk or bike to work or to the store.
•Use stairs instead of the elevator or escalator.
•Take breaks at work to stretch or take quick walks, or do something active with co-workers at lunch.
•Walk while you talk, if you’re using a cellphone or cordless phone.
•Doing yard work or household chores counts as physical activity. Turn on some upbeat music to help you do chores faster and speed up your heart rate.
Experts say that for a physically inactive person to become active, and remain active for the long-term, the activity needs to be convenient and enjoyable. The activity needs to be something you can easily fit into your routine for several days each week. Even if you end up adding just 30 minutes of physical activity to your day, that is fine. Some of the examples below are the easiest to fit into a daily routine:
•Go for a brisk 30-minute walk five times each week. Ideally, it should be done in one session. If you can’t, two 15-minute sessions would also be good.
•Walk you dog more often. If you do not have a dog but know a nearby friend who has one, offer to walk it for him/her.
•Find out whether there are any swimming pools nearby. Try to add some swimming to your weekly routine. This does not have to be every day.
•During your lunch break at work go for a walk.
•Join some exercise classes.
•Beginners must remember that the secret is “little and often”. A little bit every day is great – one big session once a week is not. Make sure your progress is gradual.
•Experts say an exercise program should include both aerobic and anaerobic activities. This is true. However, if you are currently inactive, anything is better than nothing.
_
Make it fun:
•Choose activities that you enjoy.
•Vary your activities, so you don’t get bored. For instance, use different jogging, walking, or biking paths. Or bike one day, and jog the next.
•Reward yourself when you achieve your weekly goals. For instance, reward yourself by going to a movie.
•If you have children, make time to play with them outside. Set a good example!
•Plan active vacations that will keep you moving, such as taking tours and sightseeing on foot.
_
Make it social:
•Join a hiking or running club.
•Go dancing with your partner or friends.
•Turn activities into social occasions — for example, go to a movie after you and a friend work out.
_
Overcome challenges:
•Don’t let cold weather keep you on the couch. You can find activities to do in the winter, such as indoor fitness classes or exercising to a workout video.
•If you live in a neighbourhood where it is unsafe to be active outdoors, contact your local recreational center or church to see if they have indoor activity programs that you can join. You can also find ways to be active at home. For instance, you can do push-ups or lift hand weights. If you don’t have hand weights, you can use canned foods or bottles filled with water or sand.
Don’t expect to notice body changes right away. It can take weeks or months before you notice some of the changes from being physically active, such as weight loss. And keep in mind, many benefits of physical activity are happening inside you and you cannot see them.
_
Key Points to remember when exercising:
1. Listen to your body.
You must be careful with your exercise as if it is done improperly it may actually worsen your health. So, if exercise worsens your symptoms, modify your program or, if need be, stop. Because even though your body desperately needs exercise to improve, you will only get worse if you violate your current limitations. So you may have to start with as little as one or two minutes a day, and work your way up from there. As your energy and health improve, you will be able to tolerate larger amounts of exercise, which will lead to weight loss and increased energy.
2. Be consistent.
Research has shown that to lose 10 percent of your body weight, and keep it off, you need to exercise for one hour, five days a week. This level of exercise is only required if you are overweight, as you have an accumulated an exercise debt that must be “repaid” to regain your health.
3. Increase your intensity regularly.
Ideally you should exercise at an intensity that makes it somewhat difficult to talk to the person next to you. This prevents you from having to measure your pulse or use a heart-rate monitor. If you can comfortably talk to the person next to you, you aren’t working hard enough to produce the benefits you need to lose weight. However, if you are breathing so heavily that you cannot carry on a conversation at all, then you are exercising too hard and need to cut back a bit. Using this simple technique as a guide will assure that you’re constantly increasing your intensity as your fitness level increases.
4. Don’t rely solely on cardio.
You will need to incorporate interval-type training, along with strength training to develop a far more rounded and comprehensive exercise program. You may also want to integrate something to promote flexibility and core muscles, such as yoga, which has been proven particularly beneficial if you suffer from back pains.
_
A few simple rules are helpful as you develop your own routine.
•Don’t eat for 2 hours before vigorous exercise.
•Drink plenty of fluids before, during, and after a workout.
•Adjust your activity level according to the weather, and reduce it when you are fatigued or ill.
When exercising, listen to the body’s warning symptoms, and consult a doctor if exercise causes chest pain, irregular heartbeat, unusual fatigue, nausea, unexpected breathlessness, or light-headedness.
_
Every exercise session should include a warm-up, conditioning phase, and a cooldown:
Warming up and cooling down are important parts of every exercise routine. They help the body make the transition from rest to activity and back again, and can help prevent soreness or injury, especially in older people. Warming up before exercise and cooling down after is just as important as the exercise itself. By properly warming up the muscles and joints with low-level aerobic movement for 5 – 10 minutes one may avoid injury. Cooling down after exercise by walking slowly, then stretching muscles, may also prevent strains and blood pressure fluctuation.
• Warm-up. Take it easy for a few minutes as your body gets used to what you’re asking it to do. Perform warm-up exercises for 5 – 10 minutes at the beginning of an exercise session. Older people need a longer period to warm up their muscles. Stretching exercises, gentle calisthenics, and walking are ideal. In a meta-study of 32 high quality studies, about 4/5ths of the studies showed improvements in performance after warm-up.
• Conditioning. This is the main part of your workout.
• Cool-down. You’re transitioning out of your workout. Don’t sit, standstill, or lie down right after exercise, or you may feel dizzy or lightheaded or have heart palpitations (fluttering in your chest). The best cool-down is to ease up on the intensity of your activity. To cool down, you should walk slowly until the heart rate is 10 – 15 beats above your resting heart rate. Stopping too suddenly can sharply reduce blood pressure, and is dangerous for older people. It may also cause muscle cramping. Stretching may be appropriate for the cooling down period, but it must be done carefully for warming up because it can injure cold muscles.
_
Shoes:
All that’s really necessary for a workout is a good pair of shoes that are made well and fit well. They should be broken in, but not worn down. They should support the ankle and provide cushioning for walking as well as for impact sports such as running or aerobic dancing. Airing out the shoes and feet after exercising reduces chances for skin conditions such as athlete’s foot.
_
| Shoes for exercise: | |
| Aerobic dancing | Sufficient cushioning to absorb shock and pressure that are many times greater than ordinary walking. Arches that maintain side-to-side stability. Thick upper leather support. Toe-box. Orthotics may be required for people with ankles that over-turn inward or outward. Soles should allow for twisting and turning. |
| Cycling | Rigid support across the arch to distribute pressure during pedalling. Heel lift. Cross-training or combination hiking/cycling shoes may be sufficient for casual bikers. Toe clips or specially designed shoe cleats for serious cyclers. In some cases, orthotics may be needed to control arch and heel and balance forefoot. |
| Running | Sufficient cushioning to absorb shock and pressure. Flexible at the ball of the foot. Sufficient traction on sole to prevent slipping. Consider insoles or orthotics with arch support for problem feet. |
| Tennis | Low-traction soles. Snug fitting heels with cushioning. Padded toe box with adequate depth. Soft-support arch. |
| Walking | Lightweight. Breathable upper material (leather or mesh). Wide enough to accommodate ball of the foot. Firm padded heel counter that does not bite into heel or touch ankle bone. Low heel close to ground for stability. Good arch support. Front provides support and flexibility. |
_
Clothing:
Comfort and safety are the key words for workout clothing. For outdoor night-time exercise, a reflective vest and light-coloured clothing must be worn. Bikers, inline skaters, and equestrians should always wear safety devices such as helmets, wrist guards, and knee and elbow pads. Goggles are mandatory for indoor racquet sports. For vigorous athletic activities, such as football, ankle braces may be more effective than tape in preventing ankle injuries.
_______
Motivation for exercise:
Physical exercise is an effective approach in health promotion wherein the physical conditioning of those who regularly participate in physical activities increases and/or improves both their physical and psychological capacities. People in technologically developed societies understand the benefits of physical exercise as a healthy behavior, yet they have amongst the highest inactivity rates. This paradox is revealing of a strong, yet poorly characterized mechanism underlying the current lack of motivation and engagement in physical activity. As many as 50% of people who start an exercise program will drop out during the first 6 months. Eight weeks are needed for an initiate exerciser to become a regular exerciser, but even after 6 months, the motivation of initiating exercisers remains significantly lower than long-term regular exercisers. Low levels of motivation and self-efficacy, time-shortage, low familiarity with exercise, and poor social and cultural support are considered the primary reasons why individuals fail to adhere to physical exercise programs after they begin. A study by Brière et al. (2003), found many individuals to believe that exercise will not bring any benefit or that they are not able to perform exercise satisfactorily. This raises questions as to role and durability of existing rational arguments about the benefits of being physically active in changing the behavior of inactive individuals. Motivation factors may differ by gender, and women appear to have a harder time. In one study, weight loss was the greatest motivator to exercise for women, and muscle tone was the primary motivator for men. Unfortunately, effects on appearances may take a long time to show, discouraging people from continuing an exercise program even though their health is improving.
_
Motivation, or a lack thereof, is one reason many people stop exercising. Here are some tips for avoiding burnout:
•Think of exercise as a menu rather than a prescription. Choose a number of different physical activities that are personally enjoyable such as sports, dancing, or biking. Although experts say you should get 30 minutes of aerobic exercises at least five times a week, those times can be divided into shorter periods — such as 10 minute sessions. In addition, people can achieve health benefits from other exercise programs, including weight training, yoga, or Tai chi.
•Stick to a prepared schedule and record progress.
•Develop an interest or hobby that requires physical activity.
•Adopt simple routines such as climbing the stairs instead of taking the elevator, walking instead of driving to the local newsstand, or canoeing instead of zooming along in a powerboat.
•Try cross training (alternating between exercise types). Studies suggest it is more beneficial than focusing only on one form of exercise.
•Exercise with friends.
•Join a gym or take classes. Many affordable programs are available.
•For those who can afford them, personal trainers can be very helpful and are available in many gyms and exercise clubs. Personal trainers without any connection to a well-reputed gym or fitness club should be certified by a major fitness organization, such as the Aerobics and Fitness Association of America (AFAA) or the American Council on Exercise.
•Exercise videos may also be helpful, but people should be sure they are suited to their individual age and health needs, and bear the AFAA seal.
•Consider getting a dog. Studies show that dog owners walk up to twice as much as those who do not own a dog. Regular walking is a good way to improve health.
______
Finding the time to exercise:
Many people who do not exercise say they do not have the time. However, it is possible to increase the amount of time you are physically active, even if you are extremely busy. For example:
•See how many trips you take by car and decide which ones could be replaced by walking or cycling. Traffic experts throughout most of the world say that the majority of car trips are very short ones.
•If you are using public transport try getting off at an earlier stop and walking the rest of the way.
•A study found that interactive video games – such those played on the Nintendo Wii – may raise heart rate and provide exercise intensity levels high enough to meet federal physical activity guidelines.
•When you are in a building and want to go upstairs, try walking it, rather than taking the elevator or escalator.
•There are several gentle exercises you can do while watching TV. Even short bursts of 30 second exercises are good for improving metabolism, a study found.
•Migraine – there are many safe exercises for migraine sufferers.
•If you do housework, see if you can do it a bit more vigorously and turn it into an exercise session.
_
Myth: Physical activity takes too much time.
Fact: Physical activity does take some time, but there are ways to make it manageable. If you don’t have 30 minutes in your daily schedule for an activity break, try to find three 10-minute periods. Fitting regular exercise into your daily schedule may seem difficult at first. But even ten minutes at a time is fine. The key is to find the right exercise for you. It should be fun and should match your abilities. If you’re aiming for 60 minutes daily—a good goal if you’re trying to avoid weight gain—perhaps you can carve out some “fitness time” early in the day, before your schedule gets too busy. Another idea is to combine physical activity with a task that’s already part of your daily routine, such as walking the dog or doing yard chores.
_
Time of exercise:
Fitness experts have long said that exercising in the morning can help you stay consistent with your workouts. But there hasn’t been much research to back up that claim — until now. Jawbone crunched the data from more than 1 million people who track their steps and workouts using Jawbone’s fitness tracking products and apps. The results confirm that people who exercise in the morning are more likely to work out consistently (defined as three or more workouts per week). The magic hour for workouts? Six o’clock in the morning, according to the data. About 11 percent of the people who sweat three or more days a week exercised at 6 a.m. — a far greater percentage than any other hour of the day. Five a.m. was the second most popular time for consistent exercisers, followed by 9 a.m. People who were inconsistent with their workouts, in contrast, tended to hit the gym around 6 p.m.
________
Safety tips for beginning exercisers:
If you’ve never exercised before, or it’s been a significant amount of time since you’ve attempted any strenuous physical activity, keep in mind the following general health precautions:
• Get medical clearance. If you have special health issues such as an existing heart condition or high blood pressure, talk with your doctor or health practitioner and let him or her know your plans.
• Stretch. No matter what form of exercise you choose, you’ll benefit from adding stretching exercises to gain flexibility and range of motion. Stretching gently to warm up and cool down is the best form of injury-prevention for new exercisers.
• Drink plenty of water. Your body performs best when it’s properly hydrated. Failing to drink enough water when you are exerting yourself over a prolonged period of time, especially in hot conditions, can be dangerous.
_
Warnings regarding exercise:
Do not exercise:
•If your blood counts are low and you are at risk for infection, anemia, or bleeding.
•If the electrolytes in your blood, such as sodium and potassium, are not normal (this is likely to be the case if you have been vomiting or having diarrhoea).
•If you are taking treatments that affect your lungs or heart, or are at risk for lung or heart disease. Instead, consult your doctor first, and then watch for swollen ankles, sudden weight gain, or shortness of breath.
•If you have unrelieved pain, nausea, vomiting, or other health concerns. Always consult your doctor before beginning any exercise program.
_
Precautions to consider as you exercise:
•Do not overexert your body if you are taking blood pressure medication that controls your heart rate.
•Do not hold your breath, as this may put a strain on your heart.
•Do not exercise on uneven surfaces that could cause you to fall.
•If you have bone disease, poor vision, poor balance, or weakness, do not use heavy weights or perform excessive weight bearing exercises.
•Watch for signs of internal or external bleeding if you are taking antiplatelet or anticoagulant.
•If you have swelling, pain, dizziness, or blurred vision, discontinue all exercise and call your doctor immediately.
__
Consult doctor before exercise:
You should always check with your doctor before starting a new exercise program, especially if you have any of the following risk factors:
•A symptom you have never told your doctor about
•Arthritis of the hips or knees
•Blood clots
•Chest pain
•Chronic lung disease
•Diabetes
•Eye injury or recent eye surgery
•Family history of a cardiovascular disease
•Foot or ankle sores that won’t heal
•Heart disease or stroke
•Heart palpitations
•Hernia
•High blood pressure
•History of smoking
•Infections
•Joint swelling
•Obesity
•Pain or trouble walking after a fall
•Shortness of breath
• Injury or disability
• Pregnancy
• Recent hip surgery
_
Exercise programs for High-Risk Individuals:
Anyone with heart disease or risk factors for developing heart disease or stroke should seek medical advice before beginning a workout program. Patients with heart disease can nearly always exercise safely as long as they are evaluated beforehand. Some will need to begin their workout under medical supervision. Still, it is often difficult for a doctor to predict health problems that might arise as the result of an exercise program. At-risk individuals should be very aware of any symptoms warning of harmful complications while they exercise.
_
Can I stay active if I have a disability?
A disability may make it harder to stay active, but it shouldn’t stop you. In most cases, people with disabilities can improve their flexibility, mobility, and coordination by becoming physically active. Getting regular physical activity can also help you stay independent by preventing illnesses, such as heart disease, that can make caring for yourself more difficult. Even though you have a disability, you should still aim to meet the physical activity goals. Work with a doctor to develop a physical activity plan that works for you.
_
Exercise in sickness:
Should you really exercise when your body doesn’t feel 100 percent?
Most clinicians recommend that if your symptoms mirror a common cold without a fever – in other words, the illness remains above the neck – you can exercise moderately by doing activities like walking. The American Council on Exercise supports low-impact physical activity of 30 minutes or less when exercising with a cold. Exercising while sick may even be beneficial, since working up a sweat causes immune cells to circulate through the body more quickly and better kill bacteria and viruses. In a classic study published in the journal of Medicine & Science in Sports & Exercise, researchers recruited 45 18- to 29-year-olds of various fitness levels who agreed to be infected with rhinovirus, the culprit of most common colds. In two days, when symptoms reached their peak, the participants ran on treadmills at moderate and intense levels. The researchers reported that having a cold had no effect on participants’ lung function or ability to exercise. Researchers also tested the runners at different points in the exercise sessions and found that their colds had no effect on the way their body responded to activity. That said, these findings won’t hold true with symptoms more severe than a common cold. With the flu or a more severe illness, when symptoms maybe include a fever, extreme tiredness, muscle aches or swollen lymph glands, you should rest and postpone intense exercise until at least two weeks after symptoms disappear. If you have doubts or think you may have a more serious illness, talk to your doctor.
_______
Rest after exercise:
Rest is part of recovery. Recovery is everything that happens after the end of one workout and before the start of the next one. So rest includes sleep, time for stillness—both mental and physical—as well as participation in activities that provide mental and/or physical rejuvenation. The body repairs and strengthens itself in the time between workouts, and continuous training can actually weaken the strongest athletes. Rest days are critical to sports performance for a variety of reasons. Some are physiological and some are psychological. Rest is physically necessary so that the muscles can repair, rebuild and strengthen. For recreational athletes, building in rest days can help maintain a better balance between home, work and fitness goals. Recovery allows the body to replenish energy stores and repair damaged tissues. Exercise or any other physical work causes changes in the body such as muscle tissue breakdown and the depletion of energy stores (muscle glycogen) as well as fluid loss. Recovery time allows these stores to be replenished and allows tissue repair to occur. Without sufficient time to repair and replenish, the body will continue to breakdown from intensive exercise. In the worst-case scenario, too few rest and recovery days can lead to overtraining syndrome – a difficult condition to recover from. Symptoms of overtraining often occur from a lack of recovery time. Signs of overtraining include a feeling of general malaise, staleness, depression, decreased sports performance and increased risk of injury, among others.
_
Rest days are an essential part of an exercise program. Your body needs about 48 hours to recover between exercises targeting the same muscle group. You can still exercise every day, just not the same muscle. Youth baseball pitchers need at least 24 hours rest after a game. Some runners rest once a week. Everyone is different. Rest needed depends on many factors including your age, activity, and nutrition, but everyone needs some. If you work out intensely but don’t allow for down time, your body will be less apt to reap the benefits. Exercise puts stress on the body, including the joints, which don’t have much padding for projection from injury. The knee, ankle and hip joints take a particular beating with respect to the repetitive nature of running. Without regular rest breaks, they may become sore and swollen. A much needed rest between bouts of exercise will help avoid this problem and keep your joints healthy. An appropriately challenging workout will, in general, require one to two recovery days.
_
Nutrition and exercise:
Proper nutrition is at least as important to health as exercise. When exercising, it becomes even more important to have good diet to ensure the body has the correct ratio of macronutrients whilst providing ample micronutrients, in order to aid the body with the recovery process following strenuous exercise. You can help your body to exercise better by eating the right foods. You know that muscle metabolism involves the phosphagen system, glycogen-lactic acid system and aerobic respiration. The major fuels used are glucose and glycogen. So, if you want to do well, whether you are competing or just exercising for well-being, you should try to increase the stores of glycogen in your liver and your muscles. Athletes eat solid, high-carbohydrate diets (breads, pasta) the night before competition, and liquid, high-glucose diets in the morning before competition. Sports drinks containing glucose are good to drink during competition to replace fluid and help to maintain blood glucose levels.
_
Vitamins and exercise:
Although no conclusive evidence exists to suggest that vitamin supplementation improves athletic performance in nutritionally adequate individuals, exercise may increase requirements for certain vitamins in individuals with marginal vitamin stores. Exercise increased the requirement for riboflavin and vitamin C; however, vitamin supplementation improved the ability to train only in vitamin C-depleted individuals. No measurable effect of supplemental thiamine, riboflavin, or vitamin B6 on performance was observed in any of the reported studies. Exercise acutely affected vitamin B6 metabolism. Confusion regarding vitamin supplementation and exercise performance may stem from a lack of adequate research data.
_
Adaptation to Exercise:
The Principle of Adaptation states that when we undergo the stress of physical exercise, our body adapts and becomes more efficient. It’s just like learning any new skill; at first it’s difficult, but over time it becomes second-nature. Once you adapt to a given stress, you require additional stress to continue to make progress. There are limits to how much stress the body can tolerate before it breaks down and risks injury. Doing too much work too quickly will result in injury or muscle damage, but doing too little, too slowly will not result in any improvement. This is why personal trainers set up specific training programs that increase time and intensity at a planned rate and allow rest days throughout the program.
________
________
Exercise statistics and trends:
Most of the health benefits of exercise have been widely publicized and to some extent enjoy popular recognition. Nevertheless, sedentary lifestyles are predominant in most urban areas worldwide. Indeed, inactivity constitutes an important risk factor behind the epidemic rates of non-communicable diseases (NCDs). In its 2002 World Health Report the World Health Organization (WHO) reported that 76% of all deaths in the Americas in the year 2000 were due to NCDs, a proportion similar to that found in the developed regions of Europe (86%) and the Western Pacific (75%). In that same year in Latin America alone there were an estimated 119 000 deaths due to inactive lifestyles.
_
Latin America and the Caribbean have become the most urbanized region in the developing world, with over 60% of the population residing in urban centers. This rapid urban population growth has outpaced the development of social and physical infrastructure, employment, health services, and housing. Together, these various trends have contributed to inadequate public transportation systems, increased traffic congestion and environmental pollution, decreased activity levels in both work and leisure time, and changes to the physical and social urban landscape. Data from 24 countries in the Region of the Americas indicate that over half the population are inactive, that is, not performing the minimum recommended 30 minutes of moderate-intensity activity on at least 5 days of the week. In several of the countries of the Americas the proportion of the population at risk due to inactive lifestyles is close to 60%. This situation may be especially critical among persons 60 and older. These persons make up the fastest growing segment of the population in Latin America and the Caribbean, with a growth rate that is 3.5 times that of the population overall. In addition, these older persons have the highest prevalence of NCDs. For this large and growing population with decreased mobility and other health concerns, environments that support a physically active lifestyle and greater access to public transportation are becoming increasingly important.
_
The figure below shows finding of exercise survey conducted by CDC in the U.S.
_
The American Heart Association recommends 150 minutes of moderate intensity aerobic exercise per week for most adults, yet according to the Center for Disease Control and Prevention, only 1 in 5 adults meets these overall physical activity guidelines. The estimated economic burden of physical inactivity in the United States in 2005 was $24 billion, which accounted for 2.4% of total health expenditures. Strategies to promote recruitment and retention in an exercise program have been met with limited success. In 2007, the American College of Sports Medicine, with endorsement from the American Medical Association and the Office of the Surgeon General, launched a global initiative to mobilize physicians, healthcare professionals and providers, and educators to promote exercise in their practice or activities to prevent, reduce, manage, or treat diseases that impact health and the quality of life in humans. Emerging from this initiative, termed ‘Exercise is Medicine’, has been an extensively documented position stand by the American College of Sports Medicine that recommended healthy adults perform 150 min of moderate dynamic exercise per week. Complying with the ACSM-AHA guidelines offers a considerable return on a minimal investment. Yet in spite of the evidence of health benefits and the minimal time investment, almost half of American adults fail to meet these levels of activity. The numbers are likely similar in Canada. Fifty percent of all people who begin a vigorous training program drop out within a year. The key to reaching and maintaining physical fitness is to find activities that are exciting, challenging, and satisfying.
________
________
Physical activity versus Exercise:
_
Some definitions:
Health:
In humans it is the ability of individuals or communities to adapt and self-manage when facing physical, mental or social challenges.
Physical activity:
Any bodily movement produced by the contraction of skeletal muscle that increases energy expenditure above a basal level. Physical activity generally refers to the subset of physical activity that enhances health.
Health-enhancing physical activity:
Activity that, when added to baseline activity, produces health benefits. Brisk walking, jumping rope, dancing, playing tennis or soccer, lifting weights, climbing on playground equipment at recess, and doing yoga are all examples of health-enhancing physical activity.
Exercise:
A subcategory of physical activity that is planned, structured, repetitive, and purposive in the sense that the improvement or maintenance of one or more components of physical fitness is the objective.
Workout:
A “workout” is a term that refers to the period of time spent exercising — the exercise event. That makes “working out” the same thing as “exercise.”
Training:
“Training” is the process of moving from one state of physical preparedness to another. The individual workouts that compose the elements of the process are important not in and of themselves, but because their cumulative effect accomplishes a specific definable physical goal. To an athlete who is “training” for a performance goal, be it a marathon or a weightlifting meet, the accumulated, increasing stress that characterizes “training” must be specific to the performance goal. This means that “training” must be carefully planned in advance to produce a specific adaptation at a specific point in time. This planning differentiates “training” from “exercise.”
Exercise training:
Physical activity performed during leisure time with the primary purpose of improving or maintaining physical fitness, physical performance, or health.
Physical inactivity:
Physical inactivity means physical activity levels less than those required for optimal health and prevention of premature death.
_
“Physical activity,” “exercise,” and “physical fitness” are terms that describe different concepts. However, they are often confused with one another, and the terms are sometimes used interchangeably. Physical activity is defined as any bodily movement produced by skeletal muscles that result in energy expenditure. The energy expenditure can be measured in kilocalories. Physical activity in daily life can be categorized into occupational, sports, conditioning, household, or other activities. Exercise is a subset of physical activity that is planned, structured, and repetitive and has as a final or an intermediate objective the improvement or maintenance of physical fitness. Physical fitness is a set of attributes that are either health- or skill-related. The degree to which people have these attributes can be measured with specific tests.
_
_
Physical activity is movement that is carried out by the skeletal muscles that requires energy. In other words, any movement one does is actually physical activity. This simply means getting up and moving around – doing household chores, raking leaves or walking the dog – is physical activity. Exercise, however, is planned, structured, repetitive and intentional movement intended to improve or maintain physical fitness. Exercise is a subcategory of physical activity. Physical activity is an inclusive term that refers to any expenditure of energy brought about by bodily movement via the skeletal muscles; as such, it includes the complete spectrum of activity from very low resting levels to maximal exertion. Exercise is a component of physical activity. The distinguishing characteristic of exercise is that it is a structured activity specifically planned to develop and maintain physical fitness. Examples of physical activity are housework, gardening, moving up and down on stairs leaving elevators, and walking. Examples of exercises are cardio exercises, weightlifting, brisk walking, running, etc. If you are not fond of going to the gym, you can engage in swimming, cycling, running, and sports such as golf and tennis. They can also serve as good exercise for your body. Physical conditioning refers to the development of physical fitness through the adaptation of the body and its various systems to an exercise program. Physical fitness includes cardiorespiratory fitness, muscle strength, body composition, and flexibility, comprising a set of attributes that people have or achieve that relates to the ability to perform physical activity.
_
_
The term “physical activity” describes many forms of movement, including activities that involve the large skeletal muscles. Activities that involve the small skeletal muscles (e.g. playing board games, drawing, writing) are important, but they do not provide the health benefits of activities that involve the large skeletal muscles and require substantial energy expenditure.
Physical activity is defined by its duration, intensity, and frequency
1. Duration is the amount of time spent participating in a physical activity session
2. Intensity is the rate of energy expenditure
3. Frequency is the number of physical activity sessions during a specific time period (e.g. one week).
_
Types of Physical Activity:
1. Aerobic – light to vigorous-intensity physical activity that requires more oxygen than sedentary behavior and thus promotes cardiovascular fitness and other health benefits (e.g., jumping rope, biking, swimming, running; playing soccer, basketball, or volleyball).
2. Anaerobic – intense physical activity that is short in duration and requires a breakdown of energy sources in the absence of sufficient oxygen. Energy sources are replenished as an individual recovers from the activity. Anaerobic activity (e.g. weight lifting) requires maximal performance during the brief period.
3. Lifestyle – physical activity typically performed on a routine basis (e.g., walking, climbing stairs, mowing or raking the yard), which is usually light to moderate in intensity.
4. Physical activity play – play activity that requires substantial energy expenditure (e.g., playing tag, jumping rope).
5. Play – activity with flexible rules, usually self-selected, for the purpose of having fun.
6. Sports – physical activity that involves competition, scorekeeping, rules, and an outcome that cannot be predetermined. There are two categories of sports: individual and team.
7. Weight-bearing – physical activity that requires people to move their own weight.
_
What counts as exercise?
In the UK, regular exercise is defined by the NHS as completing 150 minutes of moderate intensity aerobic activity a week. Aerobic activity at moderate intensity basically means exercising at a level that raises your heart rate and makes you sweat. This includes a multitude of sports. For example;
•Fast paced walking
•Light jogging
•Bike riding
•Rowing
•Playing doubles tennis or badminton
•Water aerobics
Cutting the grass, cleaning your home and other daily chores such as shopping don’t count towards your 150 minutes of weekly exercise as advances in technology have made these activities far less demanding on the body than for previous generations, who were active naturally more active through work and manual labour. However, the less time you spend sitting down, the better it will be for your health. Sedentary behaviour, such as sitting or lying down for long periods, increases your risk of weight gain and obesity, which in turn, may also up your risk of chronic diseases such as heart disease and diabetes.
__
Physical activity vs physical fitness:
Some people incorrectly use physical fitness and physical activity interchangeably. The CDC defines physical fitness as “The ability to carry out daily tasks with vigor and alertness, without undue fatigue, and with ample energy to enjoy leisure-time pursuits and respond to emergencies. Physical Fitness has a more specific definition by Kilgore and Rippetoe in the Journal of Exercise Physiology “Possession of adequate levels of strength, endurance, and mobility to provide for successful participation in occupational effort, recreational pursuits, familial obligation, and that is consistent with a functional phenotypic expression of the human genotype.” This is a description of what fitness entails, and describes a reason to be fit based on the genetics we possess. But it doesn’t say anything about how to accomplish this task, either the process or the components thereof. Physical fitness includes a number of components consisting of cardiorespiratory endurance (aerobic power), skeletal muscle endurance, skeletal muscle strength, skeletal muscle power, flexibility, balance, speed of movement, reaction time, and body composition”. Inherited genes and their interaction with physical activity levels determine physical fitness. However, chronic physical activity levels themselves modulate fitness. Further, the levels of physical activity themselves modulate whether fitness improves. For example, Sisson et al. concluded that the most important finding of their study was that greater volumes of exercise were associated with a lower probability of being a non-responder. The percentage of non-responders at a given level of training progressively decreased as the exercise volume increased.
_
Physical fitness refers to a physiologic state of well-being that allows one to meet the demands of daily living or that provides the basis for sport performance, or both. Health-related physical fitness involves the components of physical fitness related to health status, including cardiovascular fitness, musculoskeletal fitness, body composition and metabolism. In large epidemiologic investigations, physical activity and physical fitness are often used interchangeably, with fitness commonly being treated as a more accurate (albeit indirect) measure of physical activity than self-report. Physical fitness appears to be similar to physical activity in its relation to morbidity and mortality but is more strongly predictive of health outcomes than physical activity. Most analyses have shown a reduction of at least 50% in mortality among highly fit people compared with low-fit people. Nonetheless, both physical activity and fitness are strong predictors of risk of death. To obtain accurate estimates of physical activity, many fitness consultants rely on primary criterion (gold standard) for the measurement of energy expenditure, such as direct observation of movement or, in the laboratory, the doubly labelled water technique or indirect calorimetry. On a practical basis, however, measures of physical activity and energy expenditure are obtained by using heart rate monitors and motion sensors (pedometers and accelerometers). The assessment of physical fitness is often not feasible or practical in large population-based investigations. Fortunately such studies have consistently shown an inverse gradient of health risk across self-reported physical activity groups. From a public health perspective, Blair and colleagues have argued that it is preferable to encourage people to become more physically active rather than to become physically fit, since, as they stated, sedentary people will likely achieve the latter if they do the former.
____
Health-related physical fitness:
Health-related physical fitness is defined as fitness related to some aspect of health. This type of physical fitness is primarily influenced by an individual’s exercise habits; thus, it is a dynamic state and may change. Physical characteristics that constitute health-related physical fitness include strength and endurance of skeletal muscles, joint flexibility, body composition, and cardiorespiratory endurance. All these attributes change in response to appropriate physical conditioning programs, and all are related to health. Health related physical fitness consists of four specific components:
-Cardiorespiratory fitness
-Muscular strength/endurance fitness
-Flexibility fitness
-Body composition
_
1. Cardiorespiratory endurance/fitness, or aerobic fitness, is probably what most people identify as physical fitness. Aerobic fitness refers to the integrated functional capacity of the heart, lungs, vascular system, and skeletal muscles to expend energy. The basic activity that underlies this type of fitness is aerobic metabolism in the muscle cell, a process in which oxygen is combined with a fuel source (fats or carbohydrates) to release energy and produce carbon dioxide and water. The energy is used by the muscle to contract, thereby exerting force that can be used for movement. For the aerobic reaction to take place, the cardiorespiratory system (i.e., the circulatory and pulmonary systems) must constantly supply oxygen and fuel to the muscle cell and remove carbon dioxide from it. The maximal rate at which aerobic metabolism can occur is thus determined by the functional capacity of the cardiorespiratory system and is measured in the laboratory as maximal oxygen intake. Cardiorespiratory fitness (CRF) is the capacity of the cardiovascular (heart and blood vessels) and respiratory (lungs) systems to supply oxygen-rich blood to the working skeletal muscles and the capacity of the muscles to use oxygen to produce energy for movement. The gold standard to determine CRF is VO2max, or maximum aerobic fitness. However in large clinical human studies, an acceptable surrogate for VO2max is the length of time running or cycling in standardized test, assuming appropriate physiological/ biochemical/ psychological proof of exhaustion is obtained. The majority of data about fitness and physical activity is focused on aerobic fitness. Data indicates that rapid, severe physical inactivity can rapidly decrease CRF. For instance, in the Dallas Bed Rest study, healthy, young males’ VO2max decreased 27% after 20 days of continuous bed rest and another study in Denmark 2 weeks of reducing daily step number from 10,501 to 1344 VO2max decreased 7%. Aerobic fitness is inversely related to the incidence of coronary heart disease and hypertension.
_
2. Strength fitness is the capacity of the skeletal muscle to move an external load. Strength is highly dependent upon skeletal muscle mass, which contains a major genetic component, and is sensitive to decreased mechanical loading resulting in skeletal muscle atrophy regardless of endowed muscle mass. Strength and endurance of skeletal muscles of the trunk help maintain correct posture and prevent such problems as low back pain. Minimal levels of muscular strength and endurance are needed for routine tasks of living, such as carrying bags of groceries or picking up a young child. Individuals with very low levels of muscular strength and endurance are limited in the performance of routine tasks and have to lead a restricted life. Such limitations are perhaps only indirectly related to health, but individuals who cannot pick up and hug a grandchild or must struggle to get up from a soft chair surely have a lower quality of life than that enjoyed by their fitter peers.
_
3. Flexibility, or range of motion around the joints, also ranks as an important component of health-related fitness. Lack of flexibility in the lower back and posterior thigh is thought to contribute to low back pain. Extreme lack of flexibility also has a deleterious effect on the quality of life by limiting performance. Balance fitness is the ability to control the body’s position throughout movement, and flexibility fitness is the ability to achieve an extended range of motion. Both have components of genetic inheritability and are also trainable.
_
4. Body composition refers to the ratio between fat and lean tissue in the body. Excess body fat is clearly related to several health problems, including cardiovascular disease, type II diabetes mellitus, and certain forms of cancer. Body composition is affected by diet, but exercise habits play a crucial role in preventing obesity and maintaining acceptable levels of body fat.
_
Musculoskeletal fitness: a paradigm shift:
Improvements in indicators of health status can occur as a result of increasing physical activity levels in the absence of changes in aerobic fitness. This is particularly evident in elderly populations, where regular physical activity can lead to reductions in risk factors for chronic disease and disability without markedly changing traditional physiologic performance markers (e.g., cardiac output and oxidative potential). Furthermore, routine physical activity can improve musculoskeletal fitness. There is increasing evidence that enhanced musculoskeletal fitness is associated with an improvement in overall health status and a reduction in the risk of chronic disease and disability. This research has led to a shift in focus in research related to the health benefits of activities that tax the musculoskeletal system.
_
Musculoskeletal fitness appears to be particularly important for elderly people and their ability to maintain functional independence. In fact, many activities of daily living do not require a large aerobic output but depend on one or more of the musculoskeletal fitness components. Many healthy elderly people may be at or near the functional threshold for dependence, wherein they are in jeopardy of losing the capacity to carry out the activities of daily living. With further worsening of musculoskeletal fitness, an individual may lose the capacity to perform daily activities, such as getting out of a chair or climbing stairs. This represents a cycle of decline, where reduced musculoskeletal fitness leads to inactivity and further dependence. As illustrated in figure below, improvements in musculoskeletal function have an enormous potential for delaying or eliminating the onset of disability, dependence and chronic disease. For instance, previous longitudinal investigations have revealed that people with high levels of muscular strength have fewer functional limitations and lower incidences of chronic diseases such as diabetes, stroke, arthritis, coronary artery disease and pulmonary disorders.
_
Improvements in musculoskeletal fitness delays or eliminate disability:
_
Two recent systematic reviews have revealed that enhanced musculoskeletal fitness is positively associated with functional independence, mobility, glucose homeostasis, bone health, psychological well-being and overall quality of life and is negatively associated with the risk of falls, illness and premature death. Interventions that improve musculoskeletal fitness appear to be particularly important for improving the health status of frail elderly people (who have a low musculoskeletal reserve). This research has revealed clearly the importance of engaging in activities that tax the musculoskeletal system and is supported by findings from a recent epidemiologic investigation. This evidence provides direct support for the recent recommendation that resistance training and flexibility exercises be performed at least twice a week to maintain functional status, promote lifelong physical activity and enhance overall quality of life.
____
Fitness and training program:
Supercompensation:
_
The fitness level of a human body in training can be broken down into four periods: initial fitness, training, recovery, and supercompensation. During the initial fitness period, the target of the training has a base level of fitness (shown by the first time sector in the graph). Upon entering the training period, the target’s level of fitness decreases (shown by the second time sector in the graph). After training, the body enters the recovery period during which level of fitness increases up to the initial fitness level (shown by the third time sector in the graph). Because the human body is an adjustable organism, it will feel the need to adjust itself to a higher level of fitness in anticipation of the next training session. Accordingly, the increase in fitness following a training session does not stop at the initial fitness level. Instead the body enters a period of supercompensation during which fitness surpasses the initial fitness level (shown by the fourth time sector in the graph). If there are no further workouts, the body’s fitness level will slowly decline back towards the initial fitness level (shown by the last time sector in the graph). First put forth by Russian scientist Nikolai N. Yakovlev (1911–1992) in 1949-1959, this theory is a basic principle of athletic training. If the next workout takes place during the recovery period, overtraining may occur. If the next workout takes place during the supercompensation period, the body will advance to a higher level of fitness. If the next workout takes place after the supercompensation period, the body will remain at the base level. More complex variations are possible; for instance, sometimes a few workouts are intentionally made in the recovery period to achieve greater supercompensation effects.
_________
_________
Types of exercise:
Exercises are generally grouped into three types depending on the overall effect they have on the human body:
• Aerobic exercise is any physical activity that uses large muscle groups and causes your body to use more oxygen than it would while resting. Aerobic exercises, such as cycling, walking, running, hiking, and playing tennis, focus on increasing cardiovascular endurance.
•Anaerobic exercise is also called strength or resistance training and can firm, strengthen, and tone your muscles, as well as improve bone strength, balance, and coordination. Examples of strength moves are pushups, lunges, and bicep curls using dumbbells. Anaerobic exercise also includes weight training, functional training, eccentric training, Interval training, sprinting and high-intensity interval training increase short-term muscle strength.
•Flexibility exercises such as stretching improve the range of motion of muscles and joints. The goal is to improve the range of motion which can reduce the chance of injury.
A balanced program should include all three. Physical exercise can also include training that focuses on accuracy, agility, power, and speed. Speed training is a major category, but generally only competitive athletes practice it.
_
_
Dynamic vs static exercise:
‘Dynamic’ exercises such as steady running tend to produce a lowering of the diastolic blood pressure during exercise, due to the improved blood flow. Conversely, static exercise (such as weight-lifting) can cause the systolic pressure to rise significantly (during the exercise).
_
Aerobic exercise (also known as cardio or cardiovascular exercise, a term attributed to this kind of exercise because of its various benefits in cardiovascular health):
A physical therapist, Col Pauline Potts, and an exercise physiologist, Kenneth Cooper M.D., both in the US Air Force, were the first to use the term aerobic exercise during the 1960s. Dr. Cooper wanted to find out why some very strong people were poor at long-distance running, swimming and cycling. He researched people’s performance in terms of their ability to use oxygen with the use of a bicycle ergometer. In 1968 Dr. Cooper published his book Aerobics. The book included scientific programs using aerobic exercises, such as swimming, running, cycling and walking. The book became a bestseller. All present aerobic programs use Cooper’s data as a baseline.
_
Aerobic exercise (also known as cardio) is physical exercise of low to moderate intensity that depends primarily on the aerobic energy-generating process. Aerobic literally means “relating to, involving, or requiring free oxygen”, and refers to the use of oxygen to adequately meet energy demands during exercise via aerobic metabolism. Generally, light-to-moderate intensity activities that are sufficiently supported by aerobic metabolism can be performed for extended periods of time. Most aerobic exercises are done at moderate levels of intensity for longer periods, compared to other categories of exercise. An aerobic exercise session involves warming up, exercising for at least 20 minutes, and then cooling down. Aerobic exercise involves mainly the large muscle groups. Running for 20 minutes is an aerobic exercise, while sprinting 200 meters is not. Playing badminton for 30 minutes is an aerobic activity if the movements of the players are fairly continuous. Golf, on the other hand, is not seen as aerobic because the heart rate has not been raised at a sustained level for long enough. Some sports are thus inherently “aerobic”, while other aerobic exercises, such as fartlek training or aerobic dance classes, are designed specifically to improve aerobic capacity and fitness. It is most common for aerobic exercises to involve the leg muscles, primarily or exclusively. There are some exceptions. For example, rowing to distances of 2,000 m or more is an aerobic sport that exercises several major muscle groups, including those of the legs, abdominals, chest, and arms. Common kettlebell exercises combine aerobic and anaerobic aspects. Many types of exercise are aerobic, and by definition are performed at moderate levels of intensity for extended periods of time. This intensity can vary from 50-80% of maximum heart rate.
_
Among the recognized benefits of doing regular aerobic exercise are:
•Strengthening the muscles involved in respiration, to facilitate the flow of air in and out of the lungs
•Strengthening and enlarging the heart muscle, to improve its pumping efficiency and reduce the resting heart rate, known as aerobic conditioning
•Improving circulation efficiency and reducing blood pressure
•Increasing the total number of red blood cells in the body, facilitating transport of oxygen
•Improved mental health, including reducing stress and lowering the incidence of depression, as well as increased cognitive capacity.
•Reducing the risk for diabetes. One meta-analysis has shown, from multiple conducted studies, that aerobic exercise does help lower HbA1C levels for type 2 diabetics.
As a result, aerobic exercise can reduce the risk of death due to cardiovascular problems. In addition, high-impact aerobic activities (such as jogging or using a skipping rope) can stimulate bone growth, as well as reduce the risk of osteoporosis for both men and women.
_
Both the health benefits and the performance benefits, or “training effect”, require a minimum duration and frequency of exercise. Most authorities suggest at least twenty minutes performed at least three times per week. The average healthy person should engage in 150–200 minutes of moderate aerobic exercise every week. This amount of physical activity should help with maintaining a healthy weight and keeping the cardiovascular system in good condition.
_
In addition to the health benefits of aerobic exercise, there are numerous performance benefits:
•Increased storage of energy molecules such as fats and carbohydrates within the muscles, allowing for increased endurance
•Neovascularization of the muscle sarcomeres to increase blood flow through the muscles
•Increasing speed at which aerobic metabolism is activated within muscles, allowing a greater portion of energy for intense exercise to be generated aerobically
•Improving the ability of muscles to use fats during exercise, preserving intramuscular glycogen
•Enhancing the speed at which muscles recover from high intensity exercise
•Neurobiological effects: improvements in brain structural connections and increased grey matter density, new neuron growth, improved cognitive function (cognitive control and various forms of memory), and improvement or maintenance of mental health
_
Some downfalls of aerobic exercise include:
•Overuse injuries because of repetitive, high-impact exercise such as distance running.
•Is not an effective approach to building muscle.
•Only effective for fat loss when used consistently.
_
Aerobic conditioning:
Aerobic conditioning is a process whereby the heart and lungs are trained to pump blood more efficiently, allowing more oxygen to be delivered to muscles and organs. Aerobic condition is usually achieved through cardiovascular exercise such as running, swimming, aerobics, etc. A stronger heart does not pump more blood by beating faster but by beating more efficiently. Trained endurance athletes can have resting heart rates as low as the reported 28 beats per minute in people such as Miguel Indurain or 32 beats per minute of Lance Armstrong, both of whom were professional cyclists at the highest level. Although exercising at lower intensities will improve aerobic conditioning, the most rapid gains are made when exercising close to an individual’s anaerobic threshold. This is the intensity at which the heart and lungs can no longer provide adequate oxygen to the working muscles and an oxygen debt begins to accrue; at this point the exercise becomes anaerobic. Anaerobic training intensity for most individuals will be <85-92% of maximum heart rate. Once improvement in aerobic conditioning is apparent, for example in metabolism and oxygen uptake, the body will progressively adapt to further training. Aerobic conditioning can be anywhere from walking on the treadmill to mowing the lawn. Aerobic conditioning has many advantages over anaerobic as it can increase physical endurance and lifespan. During aerobic training, the aim is to improve the blood flow to the lungs, heart, and blood vessels. This particular type of training targets large muscle groups so that as the intensity of physical activity is increased, overall fitness is improved. There are many benefits to aerobic training, and the outcomes can be very rewarding. Aerobic conditioning can increase the duration that one can endure physical activity. This type of conditioning can help with heart disease, diabetes, or anxiety. Aerobic conditioning also has many non-medical benefits, such as improving mood, alleviating fatigue and stabilizing sleeping patterns. This overall type of conditioning has the most longevity to its practice and can improve a person’s health and general well-being immensely.
_______
_______
Anaerobic exercise:
Anaerobic means without air. Oxygen is not used for energy generation during anaerobic exercise. Anaerobic exercise is an exercise intense enough to trigger lactate formation. It is used by athletes in non-endurance sports to promote strength, speed and power and by body builders to build muscle mass. Muscle energy systems trained using anaerobic exercise develop differently compared to aerobic exercise, leading to greater performance in short duration, high intensity activities, which last from mere seconds to up to about 2 minutes. The muscles are exercised at high intensity for short durations. A short duration usually means no more than about two minutes. Any activity lasting longer than about two minutes has a large aerobic metabolic component.
Anaerobic exercises include:
•Weight lifting
•Sprinting
•Intensive and fast skipping (with a rope)
•Interval training
•Isometrics
•Any rapid burst of hard exercise
During this type of exercise a by-product – lactic acid – is produced. Lactic acid contributes to muscle fatigue and must be used up during recovery before that muscle can be subjected to another anaerobic session. During the recovery period oxygen is used to give the muscle a “refill” – to replenish the muscle’s energy that was used up during the intensive exercise. Overall, anaerobic exercise uses up fewer calories than aerobic exercise. The cardiovascular benefits of aerobic exercises are greater than the cardiovascular benefits of anaerobic exercises. However, anaerobic exercise is better at building strength and muscle mass, while still benefitting the heart and lungs. As you build more muscle you will burn more fat, even at rest. Muscles burn more calories per unit volume than any other tissue in the body. A muscly person burns more calories than a non-muscly person, even if while he/she is resting. A study found that resistance training may aid in weight loss.
_
Anaerobic exercises offer the following benefits:
•The exerciser gets stronger
•The exerciser experiences growth in muscle mass
•Strengthens bones
•Strengthens and protects the joints
•Helps control bodyweight
•The exerciser can withstand a greater buildup of lactic acid (improved lactate tolerance) and other waste substances, and can eliminate them more rapidly
_
Strength training:
Strength training is a type of physical exercise specializing in the use of resistance to induce muscular contraction which builds the strength, anaerobic endurance, and size of skeletal muscles. When properly performed, strength training can provide significant functional benefits and improvement in overall health and well-being, including increased bone, muscle, tendon and ligament strength and toughness, improved joint function, reduced potential for injury, increased bone density, increased metabolism, increased fitness, improved cardiac function, and improved lipoprotein lipid profiles, including elevated HDL (“good”) cholesterol. Training commonly uses the technique of progressively increasing the force output of the muscle through incremental weight increases and uses a variety of exercises and types of equipment to target specific muscle groups. Strength training is primarily an anaerobic activity, although some proponents have adapted it to provide the benefits of aerobic exercise through circuit training.
_
Benefits of strength/resistance exercise/training:
While aerobic exercise increases endurance and helps the heart, it does not build upper body strength or tone muscles. Strength-training exercises provide the following benefits:
•Build muscle strength while burning fat
•Help maintain bone density
Strength-training exercises are also associated with a lower risk for heart disease, possibly because it lowers LDL (the so-called “bad” cholesterol) levels. Strength exercise is beneficial for everyone, even people in their 90s. It is the only form of exercise that can slow and even reverse the decline in muscle mass, bone density, and strength that occur with aging.
Please note: People at risk for cardiovascular disease should not perform strength exercises without checking with a doctor.
_
Weighted clothing:
Weighted clothing is clothing that adds weight to various parts of the body, usually as part of resistance training. The effect is achieved through attaching weighted pieces to the body (or to other garments) which leave the hands free to grasp objects. The method may increase muscle mass or lose weight; however, there have been concerns about the safety of some uses of weights, such as wrist and ankle weights. It is normally done in the form of small weights, attached to increase endurance when performed in long repetitive events, such as running, swimming, punching, kicking or jumping. Heavier weighted clothing can also be used for slow, controlled movements, and as a way to add resistance to body-weight exercises.
_
How does Anaerobic Exercise work?
When a short, intensive burst of activity occurs there is a temporary shortage of oxygen being delivered to the working muscles at first. The production of anaerobic energy creates a by-product; lactic acid and lactic acid causes muscle fatigue, which is the reason the session cannot last long. However, after regular training the person’s body becomes better equipped to handle lactic acid. After several practice sessions the body becomes better at getting rid of lactic acid – it also learns how to produce less of it. The body also produces buffers that postpone the onset of fatigue during an anaerobic session.
_
Anaerobic Metabolism:
Anaerobic metabolism, or anaerobic energy expenditure, is a natural part of whole-body metabolic energy expenditure. Fast twitch muscle (as compared to slow twitch muscle) operates using anaerobic metabolic systems, such that any recruitment of fast twitch muscle fibers leads to increased anaerobic energy expenditure. Intense exercise lasting upwards of about four minutes (e.g., a mile race) may still have a considerable anaerobic energy expenditure component. High-intensity interval training, although based on aerobic exercises like running, cycling and rowing, effectively become anaerobic when performed in excess of 90% maximum heart rate. Anaerobic energy expenditure is difficult to accurately quantify, although several reasonable methods to estimate the anaerobic component to exercise are available. In contrast, aerobic exercise includes lower intensity activities performed for longer periods of time. Activities such as walking, long slow runs, rowing, and cycling require a great deal of oxygen to generate the energy needed for prolonged exercise (i.e., aerobic energy expenditure). In sports which require repeated short bursts of exercise however, the anaerobic system enables muscles to recover for the next burst. Therefore training for many sports demands that both energy producing systems be developed.
_
The two types of anaerobic energy systems are: 1) high energy phosphates, ATP adenosine triphosphate and CP creatine phosphate; and 2) anaerobic glycolysis. High energy phosphates are stored in limited quantities within muscle cells. Anaerobic glycolysis exclusively uses glucose (and glycogen) as a fuel in the absence of oxygen, or more specifically when ATP is needed at rates that exceed those provided by aerobic metabolism. The consequence of such rapid glucose breakdown is the formation of lactic acid (or more appropriately, its conjugate base lactate at biological pH levels). Physical activities that last up to about thirty seconds rely primarily on the former, ATP-CP phosphagen system. Beyond this time both aerobic and anaerobic glycolysis-based metabolic systems begin to predominate. The by-product of anaerobic glycolysis, lactate, has traditionally been thought to be detrimental to muscle function. However, this appears likely only when lactate levels are very high. Elevated lactate levels are only one of many changes that occur within and around muscle cells during intense exercise that can lead to fatigue. Fatigue, that is muscle failure, is a complex subject. Elevated muscle and blood lactate concentrations are a natural consequence of any physical exertion. The effectiveness of anaerobic activity can be improved through training.
_
Aerobic versus anaerobic exercise:
The figure above illustrates Fox and Haskell formula showing the split between aerobic (light orange) and anaerobic (dark orange) exercise and heart rate. During aerobic exercise, target heart rate is 70-80 % of maximum heart rate while during anaerobic exercise, target heart rate is 80-90 % of maximum heart rate. Aerobic exercise and fitness can be contrasted with anaerobic exercise, of which strength training and short-distance running are the most salient examples. The two types of exercise differ by the duration and intensity of muscular contractions involved, as well as by how energy is generated within the muscle.
_
In almost all conditions, anaerobic exercise is accompanied by aerobic exercises because the less efficient anaerobic metabolism must supplement the aerobic system due to energy demands that exceed the aerobic system’s capacity. What is generally called aerobic exercise might be better termed “solely aerobic”, because it is designed to be low-intensity enough not to generate lactate via pyruvate fermentation, so that all carbohydrate is aerobically turned into energy. Initially during increased exertion, muscle glycogen is broken down to produce glucose, which undergoes glycolysis producing pyruvate which then reacts with oxygen (Krebs cycle) to produce carbon dioxide and water and releases energy. If there is a shortage of oxygen (anaerobic exercise, explosive movements), carbohydrate is consumed more rapidly because the pyruvate ferments into lactate. If the intensity of the exercise exceeds the rate with which the cardiovascular system can supply muscles with oxygen, it results in buildup of lactate and quickly makes it impossible to continue the exercise. Unpleasant effects of lactate buildup initially include the burning sensation in the muscles, and may eventually include nausea and even vomiting if the exercise is continued without allowing lactate to clear from the bloodstream. As glycogen levels in the muscle begin to fall, glucose is released into the bloodstream by the liver, and fat metabolism is increased so that it can fuel the aerobic pathways. Aerobic exercise may be fuelled by glycogen reserves, fat reserves, or a combination of both, depending on the intensity. Prolonged moderate-level aerobic exercise at 65% VO2 max (the heart rate of 150 bpm for a 30-year-old human) results in the maximum contribution of fat to the total energy expenditure. At this level, fat may contribute 40% to 60% of total, depending on the duration of the exercise. Vigorous exercise above 75% VO2max (160 bpm) primarily burns glycogen. Major muscles in a rested, untrained human typically contain enough energy for about 2 hours of vigorous exercise. Exhaustion of glycogen is a major cause of what marathon runners call “hitting the wall”. Training lowers intensity levels, and carbohydrate loading may allow postponement of the onset of exhaustion beyond 4 hours.
_
The figure above shows that during maximum effort exercise, anaerobic metabolism dominates up to 2 minutes and then aerobic metabolism dominates in the large skeletal muscles.
_
Interval training:
Interval training is a type of physical training that involves a series of low- to high-intensity exercise workouts interspersed with rest or relief periods. The high-intensity periods are typically at or close to anaerobic exercise, while the recovery periods involve activity of lower intensity aerobic exercise. This can mean simply speeding up your walk to a jog for a few minutes. The high intensity portion are called Sprint Intervals. Sprint intervals are measured either by time or distance. The periods of recovery are called Rest Intervals. During a rest interval athletes do not stop the activity but generally exercise at a low intensity which allows the body to recover from the sprint interval. The intervals are important; the basis of the interval training is to ensure that your sprints are done at an optimal intensity, without sufficient rest your interval training will resort back to an aerobic type of activity. High-intensity interval training attempts to decrease the overall volume of training by increasing the effort expended during the high-intensity intervals. The idea is short explosions of exercise that get your heart rate up followed by periods of rest or lower intensity providing a greater benefit.
_
_
Our body has three types of muscle fibers: slow, fast, and super-fast twitch muscles, and these muscles have two different metabolic processes:
•The aerobic, which requires oxygen for fuel burning
•The anaerobic, which does not require any oxygen
Slow twitch muscles are the red muscles, which are activated by traditional strength training and cardio exercises. The fast and super-fast twitch muscles are white muscle fibers, which are only activated during high intensity interval exercises or sprints. Activating the fast and super-fast muscles is also what causes the production of therapeutic levels of growth hormone. Now, traditional cardio exercises work primarily the aerobic process, associated with your red, slow-twitch muscles. High-intensity interval training, on the other hand, work both your aerobic and your anaerobic processes, which is what you need for optimal cardiovascular benefit. Quite simply, if you don’t actively engage and strengthen all three muscle fiber types and energy systems, then you’re not going to work both processes of your heart muscle. Many mistakenly believe that cardio works out your heart muscle, but what you’re really working is your slow twitch muscle fibers, associated with the aerobic process only. You’re not effectively engaging the anaerobic process of your heart… By changing up exercises in a single period, exercisers are improving both their endurance and speed during one exercise session. There is also thought to be a benefit of reaching your “total maximum capability”—basically working your body as hard as you can—which is hard to do for a long period of time. You increase your heart rate and total intensity to a higher level than you could during continuous activity. Almost everyone can do something continuously at 50% of their maximum ability. But, you if you can take it to a higher intensity in short bouts, your body gets stimulated in ways it wouldn’t otherwise. The research on interval training—regardless of ultimate level of intensity—is encouraging. It shows that mixing it up provides more benefits, and keeps things interesting. It’s not for everyone, since some people may find upping their fitness levels in various cycles too challenging, while someone running a marathon needs to dedicate lots of time to continuous exercise and long runs.
__
Circuit training:
With circuit workouts a number of exercises are performed back to back. They are performed in a set order, with a specific time or number of repetitions for each one, and rest periods are allotted between them. An exercise “circuit” is one completion of all prescribed exercises in the program. When one circuit is complete, one begins the first exercise again for the next circuit. Traditionally, the time between exercises in circuit training is short, often with rapid movement to the next exercise. Circuit training is great for burning extra calories in a short amount of time. Since they are more intense, training in this manor is very effective for losing weight or increasing your cardiovascular capacity or muscle endurance. Circuits are also great for increasing your muscular strength.
_
Cross-training:
Cross-training refers to the combining of exercises to work various parts of the body. Often one particular activity works certain muscle groups, but not others; cross-training aims to eliminate this. Cross-training is a technique where you alternate exercise modes (activities) in order to use different muscles. This helps to make sure that all of your muscles get a work-out during the week and also helps to prevent overuse injuries. For example, a cross-training regimen may include swimming two days a week, jogging two days a week, and using exercise gym equipment such as an elliptical trainer or stair stepper two days a week. It is standard practice to have athletes cross train in order to optimize their fitness levels and to minimize their risk of being sidelined by an injury.
_
Isometric exercise:
During isometric exercises, muscles contract. However, there is no motion in the affected joints. The muscle fibers maintain a constant length throughout the entire contraction. The exercises usually are performed against an immovable surface or object such as pressing one’s hand against a wall. The muscles of the arm are contracting but the wall is not reacting or moving in response to the physical effort. Isometric training is effective for developing total strength of a particular muscle or group of muscles. It often is used for rehabilitation since the exact area of muscle weakness can be isolated and strengthening can be administered at the proper joint angle. This kind of training can provide a relatively quick and convenient method for overloading and strengthening muscles without any special equipment and with little chance of injury.
_
Isotonic exercise:
Isotonic exercise differs from isometric exercise in that there is movement of a joint during the muscle contraction. A classic example of an isotonic exercise is weight training with dumbbells and barbells. As the weight is lifted throughout the range of motion, the muscle shortens and lengthens. Calisthenics are also an example of isotonic exercise. These would include chin-ups, push-ups, and sit-ups, all of which use body weight as the resistance force.
_
Calisthenics:
Calisthenics are a form of exercise that consists of a variety of gross motor movements, often rhythmical, generally without using equipment or apparatus, thus in all essence body-weight training. They are intended to increase body strength, body fitness and flexibility through movements such as pulling or pushing yourself up, bending, jumping, or swinging, using only one’s body weight for resistance. They are usually conducted in concert with stretches. When performed vigorously and with variety, calisthenics can provide the benefits of muscular and aerobic conditioning, in addition to improving psychomotor skills such as balance, agility and coordination.
_
Isokinetic exercise:
Isokinetic exercise utilizes machines that control the speed of contraction within the range of motion. Isokinetic exercise attempts to combine the best features of both isometrics and weight training. It provides muscular overload at a constant preset speed while a muscle mobilizes its force through the full range of motion. For example, an isokinetic stationary bicycle set at 90 revolutions per minute means that no matter how hard and fast the exerciser works, the isokinetic properties of the bicycle will allow the exerciser to pedal only as fast as 90 revolutions per minute. Machines known as Cybex and Biodex provide isokinetic results; they generally are used by physical therapists.
_______
_______
Flexibility Training (Stretching):
Flexibility training uses stretching exercises. Stretching is a form of physical exercise in which a specific muscle or tendon (or muscle group) is deliberately flexed or stretched in order to improve the muscle’s felt elasticity and achieve comfortable muscle tone. The result is a feeling of increased muscle control, flexibility, and range of motion. Stretching is also used therapeutically to alleviate cramps. In its most basic form, stretching is a natural and instinctive activity; it is performed by humans and many other animals. It can be accompanied by yawning. Stretching often occurs instinctively after waking from sleep, after long periods of inactivity, or after exiting confined spaces and areas. Increasing flexibility through stretching is one of the basic tenets of physical fitness. It is common for athletes to stretch before and after exercise in order to reduce injury and increase performance. It is suggested that one stretching exercise may not be enough to prevent all types of injury, and that, multiple stretching exercises should be used to gain the full effects of stretching. It has also been suggested that proprioceptive neuromuscular facilitation (PNF) stretching yields the greatest change in range of motion, especially short-term benefits. It is also has reduced chance of injury because it allows for the stretched muscle time to adapt to the stretched position. If done properly, stretching can prevent injury, relax the muscles, increase range of motion and flexibility, and better one’s performance, especially athletes. Stretching increases blood flow which prevents hardening of the arteries and it also produces synovial fluid, which lubricates the joints that are surrounded by the muscles; which in turn helps prevent arthritis. Stretching stabilizes the body’s natural balance and posture, and aligns the joints leading to better coordination. Certain flexibility practices, such as yoga and tai chi, also involve meditation and breathing techniques that reduce stress. Such practices appear to have many health and mental benefits. They may be very suitable and highly beneficial for older people, and for patients with certain chronic diseases.
_______
Incorporate variety of exercise for optimal health:
For optimal health, add variety to your fitness routine. Ideally, to truly optimize all aspects of your health, you’d be wise to design a well-rounded fitness program that incorporates a variety of different exercises. Without variety, your body will quickly adapt, so as a general rule, as soon as an exercise becomes easy to complete, you’ll want to increase the intensity and/or try another exercise to keep it challenging. Incorporate various types of exercise in your routine cardio; interval training, strength training, core exercise, stretching and avoid prolonged sitting.
________
________
Gymnasium (gym) vs. home exercise:
To go to gym, you have to get dressed, drive to the gym, and change into your workout clothes. Then, after working out, you have to do it all again in the opposite order. All of this can take more time than the actual workout. The appeal of gyms is further hampered by rising membership costs and the limited amount of time you can exercise as the result of crowds during busy hours. Because of these factors, Delavier and co-author Michael Gundill think there are six major reasons why working out at home is the right choice for anyone looking to build mass:
1. Home offers a place that fits your program.
Sometimes gym patrons think it’s strange to see people who are seriously working out. Gyms certainly have a more social quality than your home can offer, but being social does not make your workout effective. Often, the opposite is true.
2. Home offers a place to get the results you desire.
Strength training must be practiced seriously and not taken lightly. Unfortunately, most gyms do not want people who think that way as members. Gyms emphasize the fun aspects of exercising and do not focus on effectiveness. This is why gyms often choose equipment that looks nice over equipment that works well.
3. Home offers a chance to use effective equipment.
In many gyms, the equipment choices were made based on cost rather than effectiveness. At home, people have the option of using high-quality equipment that works well with human anatomy and is not dangerous for muscles and joints.
4. Home offers an environment where you can better concentrate.
At home, no one will disturb you while you are exercising. You’ll be able to remain focused and have a faster, more productive workout.
5. Home offers the best way to achieve the workout you planned.
In a gym, your time spent resting is largely determined by other gym members, as is your choice of exercises and equipment. Circuit training, which is indispensable for an athlete’s bodybuilding, is next to impossible in a gym. Working out at home grants you this freedom.
6. Home offers the chance to exercise without ego.
In front of other people, weightlifters often perform their repetitions haphazardly with the goal of lifting as much as possible. This leads to slower progress and a greater risk of injury. At home, with no one to impress, you can focus on effective work and not worry about what others think.
_
Gym positives:
•Friendly atmosphere
•Competition between lifters
•Extra motivation
•Lots of equipment
•People willing to help out/ Spotters
•Room for stretching, lifting etc..
•Random equipment such as belts, chalk and chains
•Sauna and pool to relax in
•Juice bar that offers variety of protein rich foods
•Personal trainers and special help
•People to socialize with
_
Gym negatives:
•Annoying people
•Lack of motivation
•Jerks in the gym
•Crowded gym
•Too far away
•High expenses
•People with no goals
•Not enough free weights
______
______
Does household work count as Exercise?
No.
If you think doing household chores will save you a trip to the gym, you might want to think again. A new study from Northern Ireland finds that people who report housework as part of their weekly exercise tend to be heavier than those who get their exercise through more traditional means. In fact, the more time people said they spent performing housework as exercise (which they considered moderate to vigorous physical activity), the heavier they tended to be. The findings are counterintuitive, the researchers said, because more physical activity — no matter what the form — should be linked with a lower weight, as long as people keep their calorie intake in check. The researchers speculated that people who say they exercise by doing housework are overestimating the intensity or duration of the activity. Or, it could be that people overestimate how many calories they burn doing chores, and eat too much, the researchers said. When you’re doing housework, you often end up snacking more, since you’re home and the fridge is right there. So even though doing housework does burn calories, it often doesn’t make up for the extra calories you take in while munching in the process. The findings suggest that housework “may not be sufficient to provide all of the benefits normally associated with meeting the physical-activity guidelines,” the researchers wrote in the journal BMC Public Health. In recent years, public health messages regarding physical activity have shifted from a focus on traditional exercises, such as running, to activities that can be performed as you go about your day, such as cycling to work, or gardening. However, these messages should instead emphasize the importance of practicing many different kinds of physical activity, and make sure that housework “is not seen as the main method” of exercising, another group of researchers said. The study, conducted by researchers at the University of Ulster, analyzed information from more than 4,600 people who were interviewed about their weekly physical activity. If the researchers excluded housework as a type of physical activity, only 20 percent of women met the physical-activity guidelines.
_____
Dancing:
Dancing is a fun and sociable way to obtain 30 mins of exercise a day. It is an aerobic exercise if done for more than
10 minutes, can strengthen the heart and encourage weight loss. More importantly it can improve muscle strength and balance and reduce mental and physical stress.
_______
_______
Exercise in children:
Exercise is essential for improving overall health, maintaining fitness, and helping to prevent the development of obesity, hypertension, and cardiovascular disease. Surveys conducted by the Center for Disease Control and Prevention (CDC) indicate that 61.5 percent of children aged nine to 13 years do not participate in any organized physical activity (for example, sports, dance classes) and 22.6 percent are not physically active during their free time. According to the American Obesity Association, approximately 30 percent of children and adolescents aged six to 19 years are overweight and 15 percent are obese. A sedentary lifestyle and excess caloric consumption are the primary causes of this increase in overweight and obesity; regular exercise is considered an important factor in controlling weight. Given the increasing prevalence of overweight and obesity in children and adolescents, it is important for parents to encourage regular exercise and also serve as role models by exercising themselves. Television, computers, and video games have replaced physical activity for playtime for the majority of children. Parents should make a commitment to replacing sedentary activities with active indoor and outdoor games. Overweight and obese children and adolescents are at higher risk of developing several medical conditions, including the following:
• Asthma
• Diabetes
• Hypertension
• Orthopaedic complications, such as hip and knee pain and limited range of motion
• Cardiovascular disease
• High cholesterol
• Sleep apnea
• Psychosocial disorders, such as depression, negative body image, and eating disorders
For children and adolescents just beginning an exercise program, results (including weight loss, increased muscle strength, and aerobic capacity) will be noticeable in four to six weeks.
_
_
The National Association for Sport and Physical Education (NASPE) offers these activity guidelines for infants, toddlers, and preschoolers:
| Age | Minimum Daily Activity | Comments |
| Infant | No specific requirements | Physical activity should encourage motor development |
| Toddler | 1½ hours | 30 minutes planned physical activity and 60 minutes unstructured physical activity (free play) |
| Preschooler | 2 hours | 60 minutes planned physical activity and 60 minutes unstructured physical activity (free play) |
| School age | 1 hour or more | Break up into bouts of 15 minutes or more |
Infants and young children should not be inactive for prolonged periods of time — no more than 1 hour unless they’re sleeping. And school-age children should not be inactive for periods longer than 2 hours.
___
Role of Schools:
Early school physical education (PE) programs can make a significant difference, and the earlier these routines are learned the more likely they will be carried forth into a healthy adulthood. There are also physical benefits to PE programs that are just now becoming known. For example, a study found that incorporating jumping exercises into an elementary school’s PE program increased children’s bone densities, a measure of bone strength. Schools should emphasize team cooperation or individual improvement and self-mastery. Studies have shown that people tend to give up more quickly and feel less competent if their perceptions of success are based only on comparison to their peers.
_
Myth: Children by nature have so much energy. They hardly sit still. There’s no need to spend time or energy teaching them about physical activity. They are already so active.
Fact: Each day children and youth aged 5 to 17, should accumulate at least 60 minutes of moderate- to vigorous-intensity physical activity to ensure healthy development. However, physical activity levels are decreasing among young people in countries around the world, especially in poor urban areas. This decline is largely due to increasingly common sedentary ways of life. For example fewer children walk or cycle to school and excessive time is devoted to watching television, playing computer games, and using computers – often at the expense of time and opportunities for physical activity and sports. Physical education and other school-based physical activities have also been decreasing. Importantly, patterns of physical activity and healthy lifestyles acquired during childhood and adolescence are more likely to be maintained throughout the life-span. Consequently, improving physical activity levels in young people is imperative for the future health of all populations.
_
Proof that physical activity improves kids’ lives:
A study summarizes many studies that investigated the effect of physical activity and sport on health, fitness, lifestyle, educational success, social skills and the psychological well-being of children and teenagers. The many beneficial effects of physical activity and sport are represented in the diagram above. It’s a good visual representation of the fact that children who are running and jumping and physically competent are also better off cognitively, emotionally and socially. The fact that too many young people are not active enough has become a cause of great concern, and rightly so. As a spontaneous form of entertainment and a source of well-being, sports and physical activities:
•help improve and maintain all physical fitness determinants as well as several components of physical and mental health
•contribute to educational success
•go hand in hand with other healthy lifestyle habits
In addition, they can help foster a feeling of belonging to the community and create social networks. It is therefore important that all stakeholders work together to offer young people attractive opportunities for physical exercise.
_________
_________
Exercise in elderly:
Physical activity and exercise can help you stay healthy, energetic and independent as you get older. Many adults aged 65 and over spend, on average, 10 hours or more each day sitting or lying down, making them the most sedentary age group. They’re paying a high price for their inactivity, with higher rates of falls, obesity, heart disease and early death compared with the general population. As you get older, it becomes even more important to remain active if you want to stay healthy and maintain your independence. If you don’t stay active, all the things you’ve always enjoyed doing and taken for granted may start to become that little bit harder. You may struggle to pursue simple pleasures, such as playing with the grandchildren, walking to the shops, leisure activities and meeting up with friends. You might start to get aches and pains that you never had before, and have less energy to go out. You may also be more vulnerable to falling. This can all lead to being less able to look after yourself and do the things you enjoy. The benefits for elderly individuals of regular participation in both cardiovascular and resistance-training programmes are great. Health benefits include a significant reduction in risk of coronary heart disease, diabetes mellitus and insulin resistance, hypertension and obesity as well as improvements in bone density, muscle mass, arterial compliance and energy metabolism. Additionally, increases in cardiovascular fitness (maximal oxygen consumption and endurance), muscle strength and overall functional capacity are forthcoming allowing elderly individuals to maintain their independence, increase levels of spontaneous physical activity and freely participate in activities associated with daily living. Taken together, these benefits associated with involvement in regular exercise can significantly improve the quality of life in elderly populations. It is noteworthy that the quality and quantity of exercise necessary to elicit important health benefits will differ from that needed to produce significant gains in fitness.
_
Studies continue to show that it is never too late to start exercising. Elderly adults who exercise twice a week can significantly increased their body strength, flexibility, balance, and agility. Studies show that even small improvements in physical fitness and activity can prolong life and independent living. A recent study based on a 35-year follow-up showed that in men who increased their physical activity at age 50, the reduction in mortality rate was similar to that of smoking cessation. In fact, after 10 years of increased physical activity, these men had the same mortality rate for their age group as men who were highly physically active throughout entire adult their lives. Still, according to the 2010 Healthy People report by the Center for Disease Control and Prevention, 46% of people aged 65 – 74 did not engage in any leisure time physical activity in 2008, the last year for which figures were available. In people over age 75, the percentage of those not engaged in any leisure time physical activity was 56%.
_
Ample evidence exists that physical activity intervention programmes are effective in preventing disease, injury, and other undesirable health conditions in elderly:
1. moderate to vigorous intensity aerobic endurance interventions can be effective in preventing osteoporosis, hypertension, type 2 diabetes, disability, and hospitalisation
2. resistance training, done at a moderate to high intensity, has effectiveness in preventing osteoporosis and disability
3. mobility and balance interventions are effective in preventing falls
4. interventions combining mixed types of moderate to vigorous intensity physical activity can be effective in preventing falls, physical disability, osteoporosis, hospitalisation, hypertension, and type 2 diabetes.
_
In order to improve cardiorespiratory and muscular fitness, bone and functional health, reduce the risk of NCDs, depression and cognitive decline:
•Older adults should do at least 150 minutes of moderate-intensity aerobic physical activity throughout the week or do at least 75 minutes of vigorous-intensity aerobic physical activity throughout the week or an equivalent combination of moderate- and vigorous-intensity activity.
•Aerobic activity should be performed in bouts of at least 10 minutes duration.
•For additional health benefits, older adults should increase their moderate-intensity aerobic physical activity to 300 minutes per week, or engage in 150 minutes of vigorous-intensity aerobic physical activity per week, or an equivalent combination of moderate-and vigorous-intensity activity.
•Older adults, with poor mobility, should perform physical activity to enhance balance and prevent falls on 3 or more days per week.
•Muscle-strengthening activities, involving major muscle groups, should be done on 2 or more days a week.
•When older adults cannot do the recommended amounts of physical activity due to health conditions, they should be as physically active as their abilities and conditions allow.
_
Myth: Physical activity is for people in the “prime of life”. At old age, we don’t need to be concerned with it…
Fact: Regular physical activity has been shown to improve the functional status and quality of life of older adults. It is recommended that adults aged 65 and above do at least 150 minutes of moderate-intensity aerobic physical activity throughout the week or do at least 75 minutes of vigorous-intensity aerobic physical activity throughout the week or an equivalent combination of moderate- and vigorous-intensity activity. Many non-communicable diseases (NCDs) prevalent in older adults can benefit from participation in regular physical activity (cardiovascular disease, osteoarthritis, osteoporosis, hypertension, falls prevention). Physical activity has also been shown to improve mental health and cognitive function in older adults and has been found to contribute to the management of disorders such as depression and anxiety. Active lifestyles often provide older persons with regular occasions to make new friendships, maintain social networks, and interact with other people of all ages. While being active from an early age can help prevent many diseases, regular movement and activity can also help relieve the disability and pain associated with these conditions. Importantly, the benefits of physical activity can be enjoyed even if regular practice starts late in life.
_
Myth: The older you are the less physical activity you need.
Fact: Most people become less physically active as they age, but keeping fit is important throughout life. Regular physical activity increases older people’s ability to perform routine daily tasks and to stay independent longer. No matter what your age, you can find a physical activity program that is tailored to your particular fitness level and needs.
________
________
Quantum of exercise:
How much exercise is enough?
The questions, “How much exercise is enough?” and “What type of exercise is best for developing and maintaining fitness?” are frequently asked. It is recognized that the term “physical fitness” is composed of a variety of characteristics included in the broad categories of cardiorespiratory fitness, body composition including regional fat distribution, muscular strength and endurance, and flexibility. In this context, fitness is defined as the ability to perform moderate-to-vigorous levels of physical activity without undue fatigue and the capability of maintaining this capacity throughout life. It is also recognized that the adaptive response to training is complex and includes peripheral, central, structural, and functional factors. Although many such variables and their adaptive responses to training have been documented, the lack of sufficient in-depth and comparative data relative to frequency, intensity, and duration of training makes them inadequate to use as models for quantifying benefits.
_
The combination of frequency, intensity, and duration of chronic exercise has been found to be effective for producing a training effect. The interaction of these factors provide the overload stimulus. In general, the lower the stimulus the lower the training effect, and the greater the stimulus the greater the effect. As a result of specificity of training and the need for maintaining muscular strength and endurance, and flexibility of the major muscle groups, a well-rounded training program including aerobic and resistance training, and flexibility exercises is recommended. Although age in itself is not a limiting factor to exercise training, a more gradual approach in applying the prescription at older ages seems prudent. It has also been shown that aerobic endurance training of fewer than 2 days per week, at less than 40 % of VO2 max, and for less than 10 min duration is generally not a sufficient stimulus for developing and maintaining fitness in healthy adults. Even so, many health benefits from physical activity can be achieved at lower intensities of exercise if frequency and duration of training are increased appropriately. In this regard, physical activity can be accumulated through the day in shorter bouts of 10-min durations.
___
It is apparent that physical activity is essential in the prevention of chronic disease and premature death. However, doubt remains over the optimal “volume” (frequency, duration and intensity of exercise) and the minimum volume for health benefits, in particular the effects of intensity (e.g., moderate v. vigorous) on health status. There is evidence that intensity of physical activity is inversely and linearly associated with mortality. Early work by Paffenbarger and associates revealed that regular physical activity (expending > 2000 kcal [8400 kJ] per week) was associated with an average increase in life expectancy of 1 to 2 years by the age of 80 and that the benefits were linear even at lower levels of energy expenditure. Subsequent studies have shown that an average energy expenditure of about 1000 kcal (4200 kJ) per week is associated with a 20%–30% reduction in all-cause mortality. Currently, most health and fitness organizations and professionals advocate a minimum volume of exercise that expends 1000 kcal (4200 kJ) per week and acknowledge the added benefits of higher energy expenditures. Recently, investigators have postulated that even lower levels of weekly energy expenditure may be associated with health benefits. A volume of exercise that is about half of what is currently recommended may be sufficient, particularly for people who are extremely deconditioned or are frail and elderly. Future research is required to determine whether expending as little as 500 kcal (2100 kJ) per week offers health benefits. If so, then previously sedentary people may be more likely to engage in physical activity and maintain an active lifestyle.
_
The dose–response relation between physical activity and health status outlined above generally relates to cardiovascular disease and premature death from any cause. However, the same may hold true for other activity-associated health benefits. For instance, as mentioned earlier, moderately intense levels of exercise (≥ 5.5 METs for at least 40 minutes per week) and of cardiovascular fitness (> 31 mL oxygen per kilogram per minute) are effective preventive strategies against type 2 diabetes. In patients with type 2 diabetes, walking more than 2 hours per week has also been shown to reduce the risk of premature death. With respect to cancer, a review of the literature revealed that moderate physical activity (> 4.5 METs) for about 30–60 minutes per day had a greater protective effect against colon and breast cancer than activities of low intensity. The greatest benefit for reducing the incidence of breast cancer was observed among women who engaged in 7 or more hours of moderate-to-vigorous activity per week. Among patients with established cancer, physical activity equivalent to walking 1 or more hours per week was associated with improved survival compared with no exercise. The greatest benefit was observed among cancer survivors who performed exercise equivalent to 3–5 hours per week at an average pace. With respect to osteoporosis, the dose–response relation of physical activity is less clear. However, osteogenic adaptations appear to be load-dependent and site-specific. Accordingly, physical activities that require impact or significant loading are therefore advocated for optimal bone health. Running distances of up to 15–20 miles (24–32 km) per week has been associated with the accrual or maintenance of bone mineral density, but longer distances may be associated with reduced bone mineral density.
_
Updated recommendation for adults from the American College of Sports Medicine and the American Heart Association: 2007:
To promote and maintain health, all healthy adults aged 18 to 65 yr need moderate-intensity aerobic (endurance) physical activity for a minimum of 30 min on five days each week or vigorous-intensity aerobic physical activity for a minimum of 20 min on three days each week. Combinations of moderate- and vigorous-intensity activity can be performed to meet this recommendation. For example, a person can meet the recommendation by walking briskly for 30 min twice during the week and then jogging for 20 min on two other days. Moderate-intensity aerobic activity, which is generally equivalent to a brisk walk and noticeably accelerates the heart rate, can be accumulated toward the 30-min minimum by performing bouts each lasting 10 or more minutes. Vigorous-intensity activity is exemplified by jogging, and causes rapid breathing and a substantial increase in heart rate. In addition, every adult should perform activities that maintain or increase muscular strength and endurance a minimum of two days each week. Because of the dose-response relation between physical activity and health, persons who wish to further improve their personal fitness, reduce their risk for chronic diseases and disabilities or prevent unhealthy weight gain may benefit by exceeding the minimum recommended amounts of physical activity.
_
In the 2008 Physical Activity Guidelines for Americans, the national Center for Disease Control and Prevention CDC recommends at least 150 minutes of moderate-intensity aerobic activity per week for most adults. Doctors routinely encourage their patients to exercise aerobically to keep their heart healthy. And classes of all forms and stripes try to push people — if not to their limit — at least enough to make them sweat for extended periods. Even those likely to give up their fitness goals after a jog or two buy heart-rate monitors to ensure they’re wringing the most cardiovascular benefit possible from their workouts.
_
Can’t find 30 minutes in your busy schedule?
That is okay, two 15-minute workouts or three 10-minute workouts can be just as effective. If that still seems like a daunting amount of time to spend exercising, don’t despair. Even just a little physical activity is better than none at all. Try starting by taking a short walk on most days, and gradually build up the length of your sessions from there. It takes about 4 weeks for an activity to become a habit so commit to maintaining your schedule for at least that long. As exercising becomes habit, you can slowly add extra minutes or try different types of activities. If you keep at it, the benefits you experience will begin to mount.
_
American Heart Association Recommendations for Physical Activity in Adults 2015:
For Overall Cardiovascular Health:
•At least 30 minutes of moderate-intensity aerobic activity at least 5 days per week for a total of 150
or
•At least 25 minutes of vigorous aerobic activity at least 3 days per week for a total of 75 minutes; or a combination of moderate- and vigorous-intensity aerobic activity
and
•Moderate- to high-intensity muscle-strengthening activity at least 2 days per week for additional health benefits.
For lowering Blood Pressure and Cholesterol
•An average 40 minutes of moderate- to vigorous-intensity aerobic activity 3 or 4 times per week
_
WHO recommendation for exercise:
Children and adolescents aged 5-17years:
•Should do at least 60 minutes of moderate to vigorous-intensity physical activity daily.
•Physical activity of amounts greater than 60 minutes daily will provide additional health benefits.
•Should include activities that strengthen muscle and bone, at least 3 times per week.
Adults aged 18–64 years:
•Should do at least 150 minutes of moderate-intensity physical activity throughout the week, or do at least 75 minutes of vigorous-intensity physical activity throughout the week, or an equivalent combination of moderate- and vigorous-intensity activity.
•For additional health benefits, adults should increase their moderate-intensity physical activity to 300 minutes per week, or equivalent.
•Muscle-strengthening activities should be done involving major muscle groups on 2 or more days a week.
_
The intensity of different forms of physical activity varies between people. In order to be beneficial for cardiorespiratory health, all activity should be performed in bouts of at least 10 minutes duration.
____
Using a pedometer:
A pedometer is a small device, usually worn on a belt, that counts the number of steps that you have taken, by sensing the motion of your hips. Many people find it a useful tool to help with motivation and monitoring when trying to increase their physical activity levels. Wearing a pedometer on an average day can give you a baseline for the number of steps that you generally take. A very sedentary person will take between 1,000-3,000 steps per day. However, most people are in the range of 4,000-6,000 steps per day. About 30 minutes of brisk walking should be around 3,000 steps. So, a good target could be to add 3,000 steps to your baseline number and aim for this. You may want gradually to build up by increments of 500-1,000 steps. The magic number to aim for in the end is at least 10,000 steps per day. It is thought that if you can manage this, it will help to keep you fit and healthy.
________
________
Walking:
Behavior change affects our private life and relationships. Exercise therapy takes place in the wrong setting because you have to attend a gym as if you are going to a physician—often things you would like to avoid. On the other hand, walking steps is something that we do every day and in all situations of our life; it is already part of our daily lifestyle. Walking is a refreshing alternative to complicated aerobic routines and overpriced gym memberships. It is free, enjoyable and already a part of everyday life. All you need to do is correct your technique, walk faster and for longer and you will lose weight. Walking is one of the best forms of physical activity – it is low impact (so does not put stress on the joints), weight-bearing (so it can improve bone density) and a 60kg individual walking briskly will burn about 300kcal an hour, so it can assist with weight loss. Additional benefits include stress reduction and improved sleep. And the long-term health benefits of walking are startling.
_
Evolution has prepared us to “walk.” We are not “exercise” machines, but 10,000 years ago we had to walk probably >20,000 steps/day for our daily survival. What is the situation today? We usually walk <5,000 steps/day, burn less energy, gain visceral adiposity, and accumulate chronic diseases like diabetes. Therefore, increasing the daily number of steps, supported by a group-based program, could be the most adequate intervention to increase physical activity and to improve glycemic control for all of our patients with diabetes and many other diseases. We can extrapolate that walking 10,000 steps/day from the age of 25 years may prevent many chronic diseases. Yates and co-workers have shown that a pragmatic structured education program that incorporates pedometer use is effective for improving glucose tolerance in subjects with impaired glucose tolerance. Interestingly, walking 1,000 steps more than your average per day—for a diabetic patient—reduces postprandial blood glucose by1.6 mmol/L over a period of 2 years. This has the same effect on postprandial blood glucose as 1,000 mg metformin and can help to reduce the daily medication in diabetes treatment and associated therapies such as blood pressure medication or lipid-lowering drugs. There is much evidence of the benefits of walking. Scientists from Lawrence Berkeley National Laboratory, Life Science Division in Berkeley, California reported in the journal Arteriosclerosis, Thrombosis and Vascular Biology that brisk walking is as effective as running in reducing a person’s risk of hypertension (high blood pressure), high cholesterol and diabetes. Scientists at the University of Pittsburgh recently revealed that overweight people who walked briskly for 30 to 60 minutes a day lost weight even if they didn’t change any other lifestyle habits. Another American study found that people who walked for at least four hours a week gained less weight (an average nine pounds less) than couch potatoes as they got older. Researchers at the University of Colorado found that regular walking helped to prevent peripheral artery disease (which impairs blood flow in the legs and causes leg pain in one-fifth of elderly people). Researchers at the University of Massachusetts medical school found that people who walked every day had 25 percent fewer colds than those who were sedentary.
_
It seems that the most simple exercise, walking, could be the best way to improve mental power. People who walk for fitness have improved communication between the various regions of the brain. This is caused by enhanced neural connectivity. This in turn improves skills such as planning, prioritizing, strategizing, and multitasking. The great thing about walking is that nearly everyone can do it, no matter their age or physical condition. It requires no equipment, and most people find it enjoyable so are likely to stick with it. Many people report that their daily walk “clears their head” and helps them think clearly. Walking seems to be the perfect kind of exercise for your brain. Because walking is a weight-bearing exercise, it can also help prevent the bone disease osteoporosis. Bones are like muscles in the way that they get stronger and denser the more demands you place on them. The pull of a muscle against a bone, together with the force of gravity when you walk, will stress the bone — which responds by stimulating tissue growth and renewal. Best of all, walking makes you feel good about yourself. For people suffering from depression, walking three to four times a week for 30 minutes has been shown to enhance their mood. Even if a 20 minute power walk at lunchtime is all you manage, after six weeks it could be comparable to a course of psychotherapy, psychologists at the University of Illinois found.
_
How much, how often?
Health experts recommend that we should walk 10,000 steps a day (about five miles) to stay healthy, yet most Britons walk only 4,500 steps. You would probably need to tot up at least 16,000 steps a day to lose weight.
_
Brisk Walking means Moderate Intensity aerobic exercise:
Walking provides a low-intensity workout that does not elevate your heart rate as high or use as much energy as higher-intensity forms of exercise. In order to improve your cardiovascular health, you must exercise at an intensity that increases your heart rate and causes you to breathe more rapidly than you normally do. Walking at 3 miles per hour can provide a moderate-intensity workout, but not a vigorous-intensity workout. Brisk walking actually refers to your exertion. For your walking pace to be brisk, you need to be breathing harder than usual. While you should still be able to speak in full sentences, you shouldn’t be able to sing. The moderate intensity zone is defined by the CDC as being from 50% to 70% of their maximum heart rate. This varies by age.
_
How fast is Brisk Walking?
Rule of Thumb:
The Center for Disease Control and Prevention (CDC) says that brisk walking is at a pace of three miles per hour or more or roughly 20 minutes per mile. That comes to an average of about 100 steps per minute. That equates to about five kilometers per hour or 12 minutes per kilometre. However, fitter people still will not be in a moderately intense exercise zone at that pace. A pace of 15 minutes per mile, or four miles per hour, is more likely to put fitter people into a moderately intense exercise zone. That equates to 9 minutes, 15 seconds per kilometer or 6.5 kilometers per hour. Walking speedometers and apps may give a readout in either minutes per mile/kilometers per mile or in miles per hour/kilometers per hour.
_
How many steps would make one mile?
The answer to this question varies depending on the size of your stride. A step for a 7ft tall runner will be very much longer than that of a 4ft tall dwarf enjoying a casual walk. A widely quoted estimate of stride length is 42% of height, although further research shows that ratio is only moderately accurate. However, it is commonly said that, on average, 2,000 walking steps make up a mile. This means that 10,000 steps converts to around 5 miles, with average stride length. If you want the figure for one kilometer, you’re looking at 1,250 walking steps.
A rough average for walking steps:
1 mile = 2,000 steps
1 km = 1,250 steps
10,000 steps = 5 miles.
_
For jogging or running:
Jogging/running 1 mile = 4,000 steps
_
Is walking just as good as running?
Walking may seem like more of a mode of transport than a form of exercise, but it really is one of the best things you can do for your body, your beauty and your long-term health. While you thought you were just getting from here to there, those steps were improving your cardiovascular strength, strengthening your muscles (which means more fat-burning power) and decreasing your chances of disease. A May 2013 study by researchers in the Life Science Division at Lawrence Berkeley National Laboratory looked at data from 33,000 runners and nearly 16,000 walkers to compare the relative health benefits of each activity. From the outside it might seem like running – which is considered a vigorous intensity exercise – must be better for you than walking, a moderate form of exercise. But the results bore out differently, with walking taking a slight edge in the end. Both walking and running had positive effects. When the researchers checked in with participants six years after the start of the study, they found that running significantly reduced the risk of high blood pressure (by 4.2 percent), high cholesterol (4.3 percent), diabetes (12.1 percent) and cardiovascular heart disease (4.5 percent), for every MET h/d, which is a standard measure of metabolic energy expenditure. Participants who walked regularly saw even better results. Walking decreased risk by 7.2 percent for high blood pressure, 7 percent for high cholesterol, 12.3 percent for diabetes and 9.3 percent for cardiovascular heart disease. The more someone walked or ran, the greater the benefit. The runners and walkers had to expend the same energy to get the same benefits. Equivalent energy expenditures by moderate walking and vigorous running exercise produced similar risk reductions for hypertension, hypercholesterolemia, diabetes mellitus, and possibly CHD. That means you’d have to walk longer than you’d have to run for the same effect.
_
Which is right for you?
Walking stresses your joints considerably less than running and many people find it easier to incorporate a regular walking regime into their lives, than other forms of exercise. If you have a history of lower limb joint injuries then you may benefit more from a brisk walking programme than from running. If weight loss is your goal, research shows that a brisk walk gives similar results to a gentle jog over the same distant. Running at a fast pace however, burns more calories. Running is a great choice of exercise for a person with finer bone structure and a lighter build. Conversely, if you have a heavier build then you would probably be better to follow a walking or interval training programme. The impact of running on your joints can be more than three times your body weight, with every step being triple the impact of walking, so it’s important to train your body to get used to the jarring. And a decent pair of walking or running shoes is a must.
_
Are there times when is walking better than running?
1. Running can damage your heart. Read over-exercise later on in the article. In the journal Circulation, researchers performed echocardiographic measurements of cardiac function in 60 recreational runners before and 20 minutes after the 2004 and 2005 Boston Marathon. What they found was that before the race, none of the runners had elevated serum markers for cardiac stress. After the race, 36 runners, or 60 percent, had elevated markers of a certain triplet of proteins called troponin. Troponin is a major component of cardiac muscle but elevated levels of subtypes of these proteins can lead to cardiovascular damage. If that’s not enough to discourage a long-distance run, consider that the researchers also discovered that 24 runners (40 percent) developed signs of myocardial necrosis, irreversible damage to heart muscle cells. The researchers also discovered at least 10 studies from 2004 to 2006 alone that documented increases in myocardial damage; there is no evidence that brisk walking can destroy heart muscle or cells.
2. Running may cause osteoarthritis. It seems that at a certain “dose,” as researchers put it in a study published in the Journal of the American Osteopathic Association, running does not cause osteoarthritis, but after a certain point, reduced risk of disease is offset by an increased risk of injury and osteoarthritis. If you’ve been running for a long time and have had injuries — and most runners have — then you’re more likely to “to deplete the joint of the lubricating glycoproteins, disrupt the collagen network, slowly wear away the cartilage, and cause numerous microfractures in the underlying bones.”
3. Running can also damage cartilage. Although authors of a study published in the American Journal of Sports Medicine state that there is continuing controversy as to whether long-distance running results in irreversible articular cartilage damage, this specific study concluded that through the use of magnetic resonance imaging (MRI), biochemical changes in articular cartilage remained elevated after three months of reduced activity. The patellofemoral joint and medial compartment of the knee showed the greatest wear and tear, suggesting higher risk for degeneration.
______
______
No time for a workout, try micro-workout.
Micro-exercise (micro-workouts):
As the name suggests, micro workouts are small, quick workouts that can be done anytime, anywhere. A micro workout doesn’t last longer than ten minutes. A usual micro-workout is 7 minutes long. From brisk walks to jumping jacks, you can use any exercise that can take your heart up. Simple, effective and time-efficient, micro workouts help overcome the constraints of time and space. These are ideal for those who are hard-pressed for time. The trend is fast catching up. Lunch time classes and drop-in classes in gyms are springing up. Also, corporate groups are providing micro workouts as part of their workplace wellness. People who lack time should go for it. The recommended 150-minute figure is the equivalent of 21 micro workouts a week. The focus is kept on the speed and intensity of the exercises while working out. The rule is simple — the faster you go the better results you get. The concept has come from Tabata training practiced by Japanese athletes. The idea is to take the heart rate up for a few seconds and then cool down for another few, and repeating the same for a couple of minutes. The variation of heart rate makes the body burn more fat for energy. These workouts enhance the muscular as well as cardiovascular abilities. The calorie burn in micro workouts is not as much as in the normal workouts, but it boosts the metabolism. You only burn 40-50 calories in a four minute micro workout. But it enhances your calorie burning capacity through-out the day. So your body can burn 400-500 calories over the next 5-6 hours. There’s a catch. These workouts are short, but not easy. Since they are done at high speed and intensity, you need to push yourself harder than in a normal workout. You push your body with all the power your body can possibly have so that each and every muscle of your body gets worked up, which means you may end up with a heavy head, which is the ideal level of a micro workout session. You must do it so fast and so hard that by the end of it you feel totally wiped out. I would call is fast workout rather than micro workout. It is micro in time but fast in intensity. This is pretty impossible to sustain for most people. Moreover, for the best results, you need to do it 3-4 times in a day. Micro workouts help you move more and beat the negative impact of excessive sitting on the body. So you need to spread these workouts throughout the day. These workouts can’t be used as a substitute to normal workouts. But as the saying goes, something is better than nothing.
_______
_______
Exercise in women:
Reasons for physical inactivity in women:
Physical inactivity is generally more prevalent among girls and women than their male counterparts. Many factors hinder the participation of women in physical activity and their access to health care:
•The income of women is often lower than that of men and therefore the costs of access to physical activity facilities may be a barrier.
•Agreement may be required from senior members of the household who control household resources before a woman can engage in physical activity.
•Women often have a workload in the home and care-giving roles for other family members which may limit the time available for them to engage in physical activity.
•Women who have limited mobility may be unable to travel to health centres or physical activity facilities.
•Cultural expectations may restrict the participation of women in certain forms of physical activity.
Social inequality, poverty and inequitable access to resources, including health care, result in a high burden of noncommunicable diseases (NCDs) among women worldwide. Although women generally tend to live longer with NCDs than men, they are often in poor health. Regular physical activity can improve women’s’ health and help prevent many of the diseases and conditions that are major causes of death and disability for women around the world. Many women suffer from disease processes that are associated with inadequate participation in physical activity:
•Cardiovascular diseases account for one-third of deaths among women around the world and half of all deaths in women over 50 years old in developing countries.
•Diabetes affects more than 70 million women in the world and its prevalence is projected to double by 2025.
•Osteoporosis is a disease in which bones become fragile and more likely to break and is most prevalent in post-menopausal women.
•Breast cancer is the mostly commonly diagnosed cancer in women.
Physical activity has also been associated with improved psychological health by reducing levels of stress, anxiety and depression. This is particularly important for women who demonstrate an incidence of depression that is reported to be almost double that of men in both developed and developing countries. It has also been suggested that physical activity can contribute to building self-esteem and confidence and can provide a vehicle for social integration and equality for women in society.
____
Exercise and menses:
Too little exercise:
If you have a sedentary lifestyle and your daily routine includes little or no exercise, you are likely to experience painful, long and irregular menstruation cycles. You are also more likely to have irregular periods if you are overweight or obese.
Moderate exercise:
Research shows that menstruating females who are doing moderate exercises on a regular basis usually have less extreme and shorter cycles. Simply put, regular exercising will lead to regular menstruation. Moderate physical activities might actually improve a number of the severe side effects that women experience during menstruation. These include side effects such as uterine cramping, back pain, nausea and vomiting.
Over exercising:
Too much exercise can put excessive amount of stress on your body to produce the regular hormones that is needed to complete a menstrual cycle. Menstruation is important because it is connected to reproduction. When you exercise, your body will go in a survival mode and might shut down unnecessary functions such as menstruation to help save energy and keep your body going in its current condition. Your body will actually hold unto every ounce of energy that it can to allow the vital functions to perform properly. It is also important to know that intense physical activity and a lower caloric intake can cause your period to stop. This condition is called amenorrhea and it occurs more frequently in menstruating females who take part in extreme fitness, distance running or bodybuilding, but it can also develop in persons who participate in various other sports which emphasize slimness, like figure skating, gymnastics and ballet. In general, women who suffer from amenorrhea experiences a continuous energy deficit that ultimately leads to the hypothalamus to suppress the discharge of hormones which regulates the ovarian function. If your ovaries fail to discharge an egg for fertilization, this will put a stop to your period. A woman’s body is expected to menstruate until pregnancy or menopause, so you should take care of yourself to avoid amenorrhea. Furthermore, it is important to menstruate every month because this is the time when the uterine lining sheds. Studies show that most women experience a total absence of menstruation whenever their body fat levels drop below twenty percent. Besides that, women with twenty to twenty-five percent of body fat are more likely to have problems with irregular menstruation.
_____
Exercise and pregnancy:
According to international guidelines, exercise with moderate intensity is safe pregnancy. Moderate exercise in healthy pregnant women does not increase the risk for miscarriage, preterm labor, or rupture of the membrane. Healthy women with normal pregnancies should exercise at least three times a week, being careful to warm up, cool down, and drink plenty of liquids. Many prenatal calisthenics programs are available.
_
The pregnant woman experiences many physiological and anatomical changes, particularly during the second half of the pregnancy. Some of these changes, including postural changes, a shift in the centre of gravity, weight gain and hormonal changes, can increase a pregnant woman’s susceptibility to injury. Moreover, balance and co-ordination skills can be affected, and activities requiring these skills may become more difficult for a pregnant woman, and can be associated with increased risk of sustaining injury. The release of the hormone relaxin causes all joints, particularly the pelvic joints, to become more mobile. Instability and injury to the sacroiliac and pubic symphis joints can potentially arise.
_
Physical exercise has gained increasing popularity among women in the fertile age, and as a result, many women ask for medical advice on whether or not they can continue to exercise throughout their pregnancy. Guidelines in countries such as the USA, Great Britain and Denmark are currently recommending physical activity during pregnancy at a level similar to that of the nonpregnant population. Physical exercise during pregnancy is known to have beneficial effects on numerous health outcomes, including a decreased risk of pre-eclampsia and gestational diabetes, but whether or not such effects apply to the health of the fetus remains unclear. The effect of leisure time physical activity during pregnancy should therefore be investigated to make antenatal care counselling on this subject as evidence based as possible. Pathways which have been suggested to mediate a potential effect of maternal exercise on fetal health include: (1) reduction of placental blood flow due to redistribution of blood to the working muscles, (2) exercise-induced hyperthermia, (3) exercise-induced release of hormones stimulating uterine contractility, and (4) fetal hypoglycaemia as a result of increased glucose uptake in exercising muscles. All of these physical responses may potentially have adverse effects on pregnancy outcome. Several animal experiments have given support to these hypotheses, while human studies are less conclusive. Only few studies have specifically addressed the association between exercise during pregnancy and miscarriage. In the existing body of literature, exercise during pregnancy has generally not been associated with miscarriage, and one case–control study has even reported a protective effect of exercise during pregnancy. In contrast, Hjollund et al. found an increased risk of early miscarriage among women who reported a high physical strain around the time of implantation of the embryo. Furthermore, lay people have tried to use excessive physical exercise as abortificant, and older literature mentions physical activity (e.g. jumping, running, and horseback riding) as a cause of miscarriage. Some studies have demonstrated that women who exercise intensely more than three times a week during the third trimester of pregnancy give birth to significantly small birth weight babies. Exercise of light intensity, three times a week or less, is therefore recommended.
_
The following are specific exercises that may benefit the pregnant woman:
•Swimming and water aerobics may be the best option for most pregnant women. Water exercises involve no impact, overheating is unlikely, and swimming face down promotes optimum blood flow to the uterus.
•Performing yoga exercises under the guidance of informed instructors can be very helpful.
•Walking is also beneficial.
To strengthen pelvic muscles, women should perform Kegel exercises at least six times a day. This involves contracting the muscles around the vagina and urethra for three seconds 12 – 15 times in a row.
_
The following precautions are generally recommended for pregnant women who exercise:
•Fit women who have exercised regularly before pregnancy may work out intensely as long as the doctor approves and no discomfort occurs. However, excessive exercise can cause undernourishment of the fetus.
•As a rule for previously sedentary, low-risk expectant mothers, the pulse rate should not exceed 70 – 75% of the maximum heart rate, or more than 150 beats per minute. Any sedentary expectant mother should check with her doctor before starting an exercise program.
•Vigorous exercise may improve the chances for a timely delivery. All pregnant women, however, should avoid high-impact, jerky, and jarring exercises, such as aerobic dancing, which can weaken the pelvic floor muscles that support the uterus.
•During exercise, women should monitor their temperature to avoid overheating, a side effect that can damage the fetus. (Pregnant women should also not use hot tubs or steam baths, which can cause fetal damage and miscarriage.)
_
Physical exercise during pregnancy: a systematic review of 2012.
Exercises during pregnancy are associated with higher cardiorespiratory fitness, prevention of urinary incontinence and low back pain, reduced symptoms of depression, gestational weight gain control, and for cases of gestational diabetes, reduced number of women who required insulin. There is no association with reduction in birth weight or preterm birth rate. The type of exercise shows no difference on results, and its intensity should be mild or moderate for previous sedentary women and moderate to high for active women. The exercise recommendations still are based on the current guidelines on moderate-intensity, low-impact, aerobic exercise at least three times a week. Yet, new guidelines propose increasing weekly physical-activity expenditure while incorporating vigorous exercise and adding light strength training to the exercise routine of healthy pregnant women. In the case of other chronic diseases like hypertension, there are still few data, and therefore more studies should be performed to assess the safety of the intervention.
_
When Mom exercises in Pregnancy, her Baby’s heart benefits: 2015 study:
Previous research has indicated that exercise in the first trimester, when the placenta is formed, helps forge extra blood vessels so that there is more opportunity to exchange nutrients between mom and baby. Linda May, an exercise physiologist and anatomist at Kansas City University of Medicine and Biosciences, figured there were bound to be sustained benefits for the baby too. May and colleagues collected noninvasive fetal heart measurements from 66 fetuses when their mothers reached 28, 32 and 36 weeks of a typical 40-week pregnancy. Some of the mothers engaged in moderate to vigorous aerobic activity for 30 minutes at least three times a week; others didn’t exercise. Researchers then assessed fetal heart rate and heart rate variability, which is the span between beats. Heart rate variability is indicative of heart health, which is associated with better overall health: people with increased variability are exercisers, and their hearts function more efficiently; those with decreased variability may be cardiac patients or, at the least, couch potatoes. At 32 weeks, researchers started to see changes in heart response in the fetuses of the exercising moms. By 36 weeks, they noted what May calls a “big, significant change” — lower heart rate and increased heart rate variability. When researchers analyzed the frequency with which Mom exercised, they found that the more activity, the lower the fetal heart rate and the higher the heart rate variability.
______
Is physical activity safe for all pregnant women?
No. Not every woman should exercise during pregnancy.
Don’t exercise if you have:
•Heart problems that affect blood flow
•Preterm labor. Preterm labor is labor that happens too early, before 37 weeks of pregnancy.
•An incompetent cervix. This is a cervix that opens too early, before the baby is full term.
•Lung disease
•A pregnancy with twins, triplets or more (also called multiples). Being pregnant with multiples increases your chances for having preterm labor.
•Vaginal bleeding during the second or third trimesters (from 4 months of pregnancy on) that doesn’t go away
•Ruptured membranes (when your water breaks)
•Preeclampsia. This is a condition that can happen after the 20th week of pregnancy or right after pregnancy. It’s when a pregnant woman has high blood pressure and signs that some of her organs like her kidneys and liver, may not be working properly. Some of these signs include having protein in the urine, changes in vision and severe headache.
•Placenta previa. This is when the placenta sits low in the uterus and covers all or part of the cervix. The placenta supplies the baby with food and oxygen through the umbilical cord. The cervix is the opening to the uterus that sits at the top of the vagina.
_
According to the American College of Sports Medicine, to maintain safety for you and your child, do not continue intense exercise if you have vaginal bleeding, severe chest pain, calf swelling, decreased fetal movement and amniotic fluid leakage. Refrain from exercise if you have orthopedic limitations, are a heavy smoker, extremely underweight, morbidly obese, have heart disease, have lung disease, are at risk for premature labor or have pregnancy-induced hypertension.
_
Activities that should be avoided during pregnancy include:
•Scuba diving
•Water skiing
•Martial arts
•Gymnastics
•Trampolining
•Weight lifting
_
Note: Strenuous exercise may affect the flavor of breast milk for a short time afterward. Nursing mothers who engage in such activity might want to wait about an hour after exercising before they feed their infant.
__________
__________
Physiology of exercise:
Exercise physiology is the physiology of physical exercise, that is, study of the acute responses and chronic adaptations to a wide range of exercise conditions. Exercise represents one the highest levels of extreme stresses to which the body can be exposed. For example, in a person who has an extremely high fever approaching the level of lethality, the body metabolism increases to approximately 100% above normal; by comparison, the metabolism of the body during a marathon race increases to 2000% above normal.
_
Energy expenditure:
Humans have a high capacity to expend energy for many hours during sustained exertion. For example, one individual cycling at a speed of 26.4 km/h (16.4 mph) through 8,204 km (5,098 mi) over 50 consecutive days expended a total of 1,145 MJ (273,850 kcal; 273,850 dieter calories) with an average power output of 182.5 W. Skeletal muscle burns 90 mg (5 mmol) of glucose each minute during continuous activity (such as when repetitively extending the human knee), generating ≈24 W of mechanical energy, and since muscle energy conversion is only 22–26% efficient, ≈76 W of heat energy. Resting skeletal muscle has a resting metabolic rate of 0.63 W/kg making a 160 fold difference between the energy consumption of inactive and active muscles. For short duration muscular exertion, energy expenditure can be far greater: an adult human male when jumping up from a squat can mechanically generate 314 W/kg. Such rapid movement can generate twice this amount in nonhuman animals such as bonobos, and in some small lizards. This energy expenditure is very large compared to the resting metabolic rate of the adult human body. This rate varies somewhat with size, gender and age but is typically between 45 W and 85 W. Total energy expenditure (TEE) due to muscular expended energy is much higher and depends upon the average level of physical work and exercise done during a day. Thus exercise, particularly if sustained for very long periods, dominates the energy metabolism of the body. Physical activity energy expenditure correlates strongly with the gender, age, weight, heart rate, and VO2 max of an individual, during physical activity.
Sex Differences:
In general, the exercise-related measurements established for women follow the same general principles as those established for men, except for the quantitative differences caused by differences in body size, body composition, and levels of testosterone. In women, the values of muscle strength, pulmonary ventilation, and cardiac output (all variables related with muscle mass) are generally 60-75% of the exercise physiology values recorded in men. When measured in terms of strength per square centimeter, the female muscle can achieve the same force of contraction as that of a male.
_
Muscle Metabolic Systems during Exercise:
Exercise and ATP:
For your muscles — in fact, for every cell in your body — the source of energy that keeps everything going is called ATP. Adenosine triphosphate (ATP) is the biochemical way to store and use energy. The entire reaction that turns ATP into energy is a bit complicated, but here is a good summary:
•Chemically, ATP is an adenine nucleotide bound to three phosphates.
•There is a lot of energy stored in the bond between the second and third phosphate groups that can be used to fuel chemical reactions.
•When a cell needs energy, it breaks this bond to form adenosine diphosphate (ADP) and a free phosphate molecule.
•In some instances, the second phosphate group can also be broken to form adenosine monophosphate (AMP).
•When the cell has excess energy, it stores this energy by forming ATP from ADP and phosphate.
ATP is required for the biochemical reactions involved in any muscle contraction. As the work of the muscle increases, more and more ATP gets consumed and must be replaced in order for the muscle to keep moving. Because ATP is so important, the body has several different systems to create ATP. These systems work together in phases. The interesting thing is that different forms of exercise use different systems, so a sprinter is getting ATP in a completely different way from a marathon runner!
_
ATP comes from three different biochemical systems in the muscle, in this order:
1. phosphagen system
2 .glycogen-lactic acid system
3. aerobic respiration
___
__
Exercise and the Phosphagen System:
A muscle cell has some amount of ATP floating around that it can use immediately, but not very much — only enough to last for about three seconds. To replenish the ATP levels quickly, muscle cells contain a high-energy phosphate compound called creatine phosphate. The phosphate group is removed from creatine phosphate by an enzyme called creatine kinase, and is transferred to ADP to form ATP. The cell turns ATP into ADP, and the phosphagen rapidly turns the ADP back into ATP. As the muscle continues to work, the creatine phosphate levels begin to decrease. Together, the ATP levels and creatine phosphate levels are called the phosphagen system. The phosphagen system can supply the energy needs of working muscle at a high rate, but only for 8 to 10 seconds.
_
Exercise and the Glycogen-Lactic Acid System:
Muscles also have big reserves of a complex carbohydrate called glycogen. Glycogen is a chain of glucose molecules. A cell splits glycogen into glucose. Then the cell uses anaerobic metabolism (anaerobic means “without oxygen”) to make ATP and a byproduct called lactic acid from the glucose. For this system, each glucose molecule is split into 2 pyruvic acid molecules, and energy is released to form several ATP molecules, providing the extra energy. Then, the pyruvic acid partially breaks down further to produce lactic acid. About 12 chemical reactions take place to make ATP under this process, so it supplies ATP at a slower rate than the phosphagen system. The system can still act rapidly and produce enough ATP to last about 90 seconds. This system does not need oxygen, which is handy because it takes the heart and lungs some time to get their act together. It is also handy because the rapidly contracting muscle squeezes off its own blood vessels, depriving itself of oxygen-rich blood.
_
Exercise and Aerobic Respiration:
By two minutes of exercise, the body responds to supply working muscles with oxygen. When oxygen is present, glucose can be completely broken down into carbon dioxide and water in a process called aerobic respiration. The aerobic system in the body is used for sports that require an extensive and enduring expenditure of energy, such as a marathon race. Endurance sports absolutely require aerobic energy. A large amount of ATP must be provided to muscles to sustain the muscle power needed to perform such events without an excessive production of lactic acid. This can only be accomplished when oxygen in the body is used to break down the pyruvic acid (that was produced anaerobically) into carbon dioxide, water, and energy by way of a very complex series of reactions known as the citric acid cycle. This cycle supports muscle usage for as long as the nutrients in the body last. The glucose can come from three different places:
•remaining glycogen supplies in the muscles
•breakdown of the liver’s glycogen into glucose, which gets to working muscle through the bloodstream
•absorption of glucose from food in the intestine, which gets to working muscle through the bloodstream
Aerobic respiration can also use fatty acids from fat reserves in muscle and the body to produce ATP. In extreme cases (like starvation), proteins can also be broken down into amino acids and used to make ATP. Aerobic respiration would use carbohydrates first, then fats and finally proteins, if necessary. Aerobic respiration takes even more chemical reactions to produce ATP than either of the above systems. Aerobic respiration produces ATP at the slowest rate of the three systems, but it can continue to supply ATP for several hours or longer, so long as the fuel supply lasts.
_
Three energy systems in muscles:
_
Post-exercise Recovery:
Oxygen debt:
During muscular exercise, blood vessels in muscles dilate and blood flow is increased in order to increase the available oxygen supply. Up to a point, the available oxygen is sufficient to meet the energy needs of the body. However, when muscular exertion is very great, oxygen cannot be supplied to muscle fibers fast enough, and the aerobic breakdown of pyruvic acid cannot produce all the ATP required for further muscle contraction. During such periods, additional ATP is generated by anaerobic glycolysis. In the process, most of the pyruvic acid produced is converted to lactic acid. Although approximately 80% of the lactic acid diffuses from the skeletal muscles and is transported to the liver for conversion back to glucose or glycogen, some lactic acid accumulates in muscle tissue, making muscle contraction painful and causing fatigue. Ultimately, once adequate oxygen is available, lactic acid must be catabolized completely into carbon dioxide and water. After exercise has stopped, extra oxygen is required to metabolize lactic acid; to replenish ATP, phosphocreatine, and glycogen; and to replace (“pay back”) any oxygen that has been borrowed from hemoglobin, myoglobin (an iron-containing substance similar to hemoglobin that is found in muscle fibers), air in the lungs, and body fluids. The additional oxygen that must be taken into the body after vigorous exercise to restore all systems to their normal states is called oxygen debt. The debt is paid back by labored breathing that continues after exercise has stopped. Thus, the accumulation of lactic acid causes hard breathing and sufficient discomfort to stop muscle activity until homeostasis is restored.
Recovery of muscle glycogen post-exercise:
Eventually, muscle glycogen must also be restored. Restoration of muscle glycogen is accomplished through diet and may take several days, depending on the intensity of exercise.
___
Pulmonary Physiology during Exercise:
The purpose of respiration is to provide oxygen to the tissues and to remove carbon dioxide from the tissues. To accomplish this, 4 major events must be regulated, as follows:
• Pulmonary ventilation
• Diffusion of oxygen and carbon dioxide between the alveoli and the blood
• Transport of oxygen and carbon dioxide in the blood and body fluids and to and from the cells
• Regulation of ventilation and other aspects of respiration
Exercise causes these factors to change, but the body is designed to maintain homeostasis. When one goes from a state of rest to a state of maximal intensity of exercise, oxygen consumption, carbon dioxide formation, and total pulmonary and alveolar ventilation increase by approximately 20-fold. A linear relationship exists between oxygen consumption and ventilation. At maximal exercise, pulmonary ventilation is 100-110 L/min, whereas maximal breathing capacity is 150-170 L/min. Thus, the maximal breathing capacity is approximately 50% greater than the actual pulmonary ventilation during maximal exercise. This extra ventilation provides an element of safety that can be called on if the situation demands it (e.g., at high altitudes, under hot conditions, abnormality in the respiratory system). Therefore, the respiratory system itself is not usually the most limiting factor in the delivery of oxygen to the muscles during maximal muscle aerobic metabolism.
________
Cardiovascular System and Exercise:
Regular exercise makes the cardiovascular system more efficient at pumping blood and delivering oxygen to the exercise muscles. Exercises increase some of the different components of the cardiovascular system, such as stroke volume (SV), heart rate (HR), cardiac output, systolic blood pressure (BP), and mean arterial pressure. A greater percentage of the cardiac output goes to the exercising muscles. At rest, muscles receive approximately 20% of the total blood flow, but during exercise, the blood flow to muscles increases to 80-85%. To meet the metabolic demands of skeletal muscle during exercise, 2 major adjustments to blood flow must occur. First, cardiac output from the heart must increase. Second, blood flow from inactive organs and tissues must be redistributed to active skeletal muscle. Generally, the longer the duration of exercise, the greater the role the cardiovascular system plays in metabolism and performance during the exercise bout. An example would be the 100-meter sprint (little or no cardiovascular involvement) versus a marathon (maximal cardiovascular involvement).
_
Changes in oxygen delivery to muscle during exercise:
• BP increases as exercise intensity increases, rising from approximately 120 mm Hg to approximately 200 mm Hg.
• SV increases during exercise until 40% of VO2max (maximum oxygen uptake level) is reached, rising from approximately 80 mL/beat to approximately 120 mL/beat.
• HR increases with intensity until VO2max is reached, rising from approximately 70 beats per minute to approximately 200 beats per minute.
• Cardiac output increases with intensity until VO2max is reached, rising from approximately 5 L/min to approximately 25-30 L/min.
The arterial-venous oxygen difference is the amount of oxygen extracted from the blood as it passes through the capillary bed. This difference rises from approximately 4 mL of oxygen per 100 mL of blood at rest to approximately 18 mL of oxygen per 100 mL of blood during high-intensity aerobic exercise.
_
Redistribution of blood flow during exercise:
At rest, 15-20% of blood goes to skeletal muscle; during exercise, this amount increases to 80-85%. The percentage of blood to the brain decreases, but the absolute amount increases. The same percentage of blood goes to cardiac muscle, but the absolute amount increases. Blood flow to visceral tissues and inactive skeletal muscle reduces. In addition, the cutaneous blood flow initially decreases, but it later increases during the course of exercise. The redistribution of the blood is brought about by several mechanisms. During exercise, generalized vasodilatation occurs because of the accumulation of vasodilatory metabolites. As ATP gets used up in working muscle, the muscle produces several metabolic by-products (such as adenosine, hydrogen ions and carbon dioxide). These by-products leave the muscle cells and cause the capillaries (small, thin-walled blood vessels) within the muscle to expand or dilate (vasodilation). The increased blood flow delivers more oxygenated blood to the working muscle. This leads to a decrease in the peripheral resistance, which, in turn, elicits a strong increase in the sympathetic activity through the activation of baroreceptors. The increase in sympathetic activity leads to vasoconstriction in the visceral organs, whereas the vasodilatation predominates in the blood vessels of the muscles and the coronary circulation because of the local vasodilatory metabolites. The cutaneous blood vessels initially respond to the sympathetic activity by vasoconstriction. As the exercise continues, temperature reflexes are activated and cause cutaneous vasodilatation to dissipate the heat produced by the muscle activity, resulting in an increase in the cutaneous blood flow.
_
Regulation of blood flow at the local level:
The local blood flow is controlled by chemical factors, metabolites, paracrines, physical factors such as heat or cold, stretch effects on endothelial membrane, active hyperemia, and reactive hyperemia. The paracrine regulation is mainly regulated by nitric oxide, histamine release, and prostacyclin. Nitric oxide diffuses to smooth muscle and causes vasodilation by reducing calcium entry into smooth muscle.
_
Haemoglobin’s Role in Exercise:
Your body has increased the flow of oxygen-rich blood to your muscles, but your muscles still need to get the oxygen out of the blood. An exchange of oxygen and carbon dioxide is the key to this. A protein called hemoglobin, which is found in red blood cells, carries most of the oxygen in the blood. As you exercise, though, the metabolic activity is high, more acids (hydrogen ions, lactic acid) are produced and the local pH is lower than normal. The low pH reduces the attraction between oxygen and hemoglobin and causes the hemoglobin to release more oxygen than usual. This increases the oxygen delivered to the muscle. Your exercising body is using energy and producing waste, such as lactic acid, carbon dioxide, adenosine and hydrogen ions. Your muscles need to dump these metabolic wastes to continue exercise. All that extra blood that is flowing to the muscles and bringing more oxygen can also take the wastes away. The hemoglobin in the blood will carry away the carbon dioxide, for example.
_
Athlete’s heart:
The heart undergoes certain morphologic changes in response to chronic exercise, commonly seen via echocardiography. These morphologic changes define what is commonly referred to as an “athletic heart.” Athletic heart syndrome is characterized by hypertrophy of the myocardium (i.e., an increase in the mass of the myocardium). Although the hypertrophy in athlete’s heart is morphologically similar to that seen in patients with hypertension, several important differences exist. In contrast to the hypertension-induced hypertrophy, the hypertrophy in the athletic heart is noted in absence of any diastolic dysfunction, with a normal isovolumetric relaxation time, with no decrease in the peak rate of left ventricular filling, and with no decrease in the peak rate of left ventricular cavity enlargement and wall thinning. Because the wall stress in the athlete’s heart is normal, sometimes the hypertrophy seems to be disproportionate to the level of resting BP. In addition, the rate of decline in the left ventricular hypertrophy and mass is much more rapid when the training is stopped compared with the regression in the same parameters in treated hypertension. On average, the decline in these parameters is seen 3 weeks after stopping exercise, and these morphologic changes can be seen on echocardiograms. Sometimes, these morphologic changes are confused with the changes seen in patients with hypertrophic cardiomyopathy (HCM). A few important morphologic differences exist. In athletic heart syndrome, the hypertrophy is usually symmetrical, as opposed to the asymmetrical hypertrophy in HCM. Also, the left ventricular size is generally normal or increased, and the left atrial size is normal, as opposed to a small left ventricular cavity with a larger left atrial cavity size (usually >4.5 cm) in HCM. Despite these differences, sometimes making a distinction between 2 conditions is a challenge.
______
Dehydration vis-à-vis exercise:
Dehydration refers both to hypohydration (dehydration induced prior to exercise) and to exercise-induced dehydration (dehydration that develops during exercise). The latter reduces aerobic endurance performance and results in increased body temperature, heart rate, perceived exertion, and possibly increased reliance on carbohydrate as a fuel source. Although the negative effects of exercise-induced dehydration on exercise performance were clearly demonstrated in the 1940s, athletes continued to believe for years thereafter that fluid intake was not beneficial. More recently, negative effects on performance have been demonstrated with modest (<2%) dehydration, and these effects are exacerbated when the exercise is performed in a hot environment. The effects of hypohydration may vary, depending on whether it is induced through diuretics or sauna exposure, which substantially reduce plasma volume, or prior exercise, which has much less impact on plasma volume. Hypohydration reduces aerobic endurance, but its effects on muscle strength and endurance are not consistent and require further study. Intense prolonged exercise produces metabolic waste heat, and this is removed by sweat-based thermoregulation. A male marathon runner loses each hour around 0.83 L in cool weather and 1.2 L in warm (losses in females are about 68 to 73% lower). People doing heavy exercise may lose two and half times as much fluid in sweat as urine. This can have profound physiological effects. Cycling for 2 hours in the heat (35 °C) with minimal fluid intake causes body mass decline by 3 to 5%, blood volume likewise by 3 to 6%, body temperature to rise constantly, and in comparison with proper fluid intake, higher heart rates, lower stroke volumes and cardiac outputs, reduced skin blood flow, and higher systemic vascular resistance. These effects are largely eliminated by replacing 50 to 80% of the fluid lost in sweat.
_
Hyperthermia vis-à-vis exercise:
Humans use sweat thermoregulation for body heat removal, particularly to remove the heat produced during exercise. Moderate dehydration as a consequence of exercise and heat is reported to impair cognition. These impairments can start after body mass lost that is greater than 1%. Cognitive impairment, particularly due to heat and exercise is likely to be due to loss of integrity to the blood brain barrier. Hyperthermia also can lower cerebral blood flow, and raise brain temperature.
_
Other physiological changes in exercise:
•Plasma catecholamine concentrations increase 10-fold in whole body exercise.
•Ammonia is produced by exercised skeletal muscles from ADP (the precursor of ATP) by purine nucleotide deamination and amino acid catabolism of myofibrils.
•interleukin-6 (IL-6) increases in blood circulation due to its release from working skeletal muscles. This release is reduced if glucose is taken, suggesting it is related to energy depletion stresses.
•Sodium absorption is affected by the release of interleukin-6 as this can cause the secretion of arginine vasopressin which, in turn, can lead to exercise-associated dangerously low sodium levels (hyponatremia). This loss of sodium in blood plasma can result in swelling of the brain. This can be prevented by awareness of the risk of drinking excessive amounts of fluids during prolonged exercise.
_______
In a nutshell, exercise is accomplished by alteration in the body response to the physical stress (exercise physiology). These responses to exercise include an increase in the HR, BP, SV, cardiac output, ventilation, and VO2. The metabolism at the cellular level is also modulated to accommodate the demands of exercise. These changes occur temporarily during the exercise. Long-term changes also occur in the body metabolism and function.
_______
Hormones involved in regulating exercise are depicted in the table below:
__
__
How hormones regulate fuels for exercise is depicted in the figure below:
_______
Fuel used for exercise:
The body uses different amounts of energy substrates (carbohydrates or fats) depending on the intensity of the exercise and the heart rate of the exerciser. Protein is a third energy substrate, but it contributes minimally and is therefore discounted in the percent contribution graphs reflecting different intensities of exercise. Carbohydrate and fat are the main substrates for the muscle used during aerobic exercise. Carbohydrates are stored in the body as muscle glycogen, liver glycogen and circulating as plasma glucose. Fat is stored as adipose tissue and as intramuscular triglyceride (IMTG). In addition, some fat is present in the circulation as plasma free fatty acids (FFA) and as triglycerides (TG) incorporated in lipoproteins. During aerobic exercise there is a mixture of fat and carbohydrate utilisation. However, the relative contribution of fat and carbohydrate utilisation to total substrate metabolism is dependent on exercise intensity, exercise duration, dietary and training status. The fuel provided by the body dictates an individual’s capacity to increase the intensity level of a given activity. In other words, the intensity level of an activity determines the order of fuel recruitment. Specifically, exercise physiology dictates that low intensity, long duration exercise provides a larger percentage of fat contribution in the calories burned because the body does not need to quickly and efficiently produce energy (i.e., adenosine triphosphate) to maintain the activity. On the other hand, high intensity activity utilizes a larger percentage of carbohydrates in the calories expended because its quick production of energy makes it the preferred energy substrate for high intensity exercise. High intensity activity also yields a higher total caloric expenditure.
_
This table outlines the estimated distribution of energy consumption at different intensity levels for a healthy 20-year-old with a Max Heart Rate (MHR) of 200.
| Intensity (%MHR) | Heart Rate (bpm) | % Carbohydrate | % Fat |
| 65-70 | 130-140 | 15 | 85 |
| 70-75 | 140-150 | 35 | 65 |
| 75-80 | 150-160 | 65 | 35 |
| 80-85 | 160-170 | 80 | 20 |
| 85-90 | 170-180 | 90 | 10 |
| 90-95 | 180-190 | 95 | 5 |
| 100 | 190-200 | 100 | – |
These estimates are valid only when glycogen reserves are able to cover the energy needs. If a person depletes glycogen reserves after a long workout (a phenomenon known as “hitting the wall”) or during a low carbohydrate diet, the body will shift into ketosis and use mostly fat and ketones for energy. Intermittent fasting can be used to train the body to shift easily into ketosis.
____
Fuel usage (light exercise):
The best examples of light exercise are walking and light jogging. The muscles that are recruited during this type of exercise are those that contain a large amount of type I muscle cells, and, because these cells have a good blood supply, it is easy for fuels and oxygen to travel to the muscle. ATP consumption makes ADP available for new ATP synthesis. The presence of ADP (and the resulting synthesis of ATP) simulates the movement of hydrogen (H+) into the mitochondria; this, in turn, reduces the proton gradient and thus stimulates electron transport. The hydrogen on the reduced form of nicotinamide adenine dinucleotide (NADH) is used up, nicotinamide adenine dinucleotide (NAD) becomes available, and fatty acids and glucose are oxidized. Incidentally, the calcium released during contraction stimulates the enzymes in the Krebs cycle and stimulates the movement of the glucose transporter 4 (GLUT-4) from inside of the muscle cell to the cell membrane. Both these exercise-induced responses augment the elevation in fuel oxidation caused by the increase in ATP consumption.
_
Fuel usage (moderate exercise):
An increase in the pace of running simply results in an increased rate of fuel consumption, an increased fatty acid release, and, therefore, an increase in the rate of muscle fatty acid oxidation. However, if the intensity of the exercise increases even further, a stage is reached in which the rate of fatty acid oxidation becomes limited. The reasons why the rate of fatty acid oxidation reaches a maximum are not clear, but it is possible that the enzymes in the beta-oxidation pathway are saturated (i.e., they reach a stage in which their maximal velocity [Vmax] is less than the rate of acetyl-coenzyme A [acetyl-CoA] consumption in the Krebs cycle). Alternatively, it may be that the availability of carnitine (the chemical required to transport the fatty acids into the mitochondria) becomes limited. Whatever the reason, the consequence is that as the pace rises, the demand for acetyl-CoA cannot be met by fatty acid oxidation alone. The accumulation of acetyl-CoA that was so effective at inhibiting the oxidation of glucose is no longer present, so pyruvate dehydrogenase starts working again and pyruvate is converted into acetyl-CoA. In other words, more of the glucose that enters the muscle cell is oxidized fully to carbon dioxide. Therefore, the energy used during moderate exercise is derived from a mixture of fatty acid and glucose oxidation.
_
Fuel usage (strenuous exercise):
As the intensity of the exercise increases even further (i.e., running at the pace of middle-distance races), the rate at which the muscles can extract glucose from the blood becomes limited. In other words, the rate of glucose transport reaches Vmax, either because the blood cannot supply the glucose fast enough or the number of GLUT-4s becomes limited. ATP generation cannot be serviced completely by exogenous fuels, and ATP levels decrease. Not only does this stimulate phosphofructokinase, it also stimulates glycogen phosphorylase. This means that glycogen stored within the muscle cells is broken down to provide glucose. Therefore, the fuel mix during strenuous exercise is composed of contributions from blood-borne glucose and fatty acids and from endogenously stored glycogen.
_
Fuel usage in individuals who are unfit:
Being fit (biochemically speaking) means that the individual has a well-developed cardiovascular system that can efficiently supply nutrients and oxygen to the muscles. Fit people have muscle cells that are well perfused with capillaries (i.e., they have a good muscle blood supply). Their muscle cells also have a large number of mitochondria, and those mitochondria have a high activity of Krebs cycle enzymes, electron transport carriers, and oxidation enzymes. Individuals who are unfit must endure the consequences of a poorer blood supply, fewer mitochondria, less electron transport units, a lower activity of the Krebs cycle, and poorer activity of beta-oxidation enzymes. To generate ATP in the mitochondria, a steady supply of fuel and oxygen and decent activity of the oxidizing enzymes and carriers are needed. If any of these components are lacking, the rate at which ATP can be produced by mitochondria is compromised. Under these circumstances, the production of ATP by aerobic means is not sufficient to provide the muscles with sufficient ATP to sustain contractions. The result is anaerobic ATP generation using glycolysis. Increasing the flux through glycolysis but not increasing the oxidative consumption of the resulting pyruvate increases the production of lactate.
______
Metabolic adaptation in trained individuals:
Endurance trained humans rely less on muscle glycogen and plasma glucose and more on fats as an energy source during exercise at any given absolute or even relative intensity as compared to untrained humans. These differences are due to physiologic, biochemical and hormonal adaptations to endurance training. It is evident that the metabolic adaptations to training are largely mediated by an increase in mitochondrial density and muscle capillary density. The increase in mitochondrial density is explained by an increase in both number and size of the mitochondria. This increase following endurance training leads to an increase of the mitochondrial enzymes responsible for the activation, mitochondrial transport, β-oxidation of fatty acids, and enzymes of the tricarboxylic (TCA)-cycle. The alterations in substrate utilisation with endurance training are likely explained by a lesser disturbance of energetic homeostasis. With a greater mitochondrial volume after training, smaller decreases in ATP, phosphocreatine (PCr) and smaller increases in ADP and inorganic phosphate (Pi) are required during exercise to balance the rate of ATP synthesis with the rate of ATP hydrolysis. The smaller increase in ADP, results in less of an increase in AMP formation by AMPK (=adenylate kinase) and, therefore, also less of an increase in IMP and NH4+ formation by AMP deaminase. These metabolic alterations, especially the smaller increases in Pi and AMP, play a major role in reducing glycogenolytic rate in muscle that has been adapted to endurance training. Although important, the augmention of muscle respiratory capacity is not the only mechanism by which training affects substrate metabolism during exercise. Neuro-endocrine responses, which are modified by endurance training, play a major role in regulating substrate mobilisation and utilisation. For example plasma norepinephrine, epinephrine, growth hormone, cortisol, and adrenocorticotropic hormone increase less during exercise at the same absolute exercise intensity in the trained state, compared to the untrained state. Reduced catecholamine levels after training may contribute to many of the previously described alterations in substrate metabolism during exercise. For example, the slower rate of muscle glycogenolysis during exercise after training may be due, in part, to lower catecholamine levels. Similarly, lower catecholamine levels, in conjunction with less of a decline in insulin secretion, seem likely to contribute to the reduced rates of hepatic glucose production during exercise after training. It is now quite clear that endurance training leads to decreased reliance on carbohydrate oxidation and an increased reliance on fat oxidation at any given exercise intensity. However, the relative contribution of the different fat sources used during exercise remains debated.
____
Myth of fat burning exercise:
A recurring question has been whether you should run or walk in order to burn as much fat as possible. Put differently, what is better – high- or low-intensity exercise? The background for this question is that during low-intensity muscular work (30-40% of maximum oxygen uptake, a measure of physical fitness), the metabolism of fat comprises roughly half the total energy, while only 20-30% of the energy (or less) comes from fat during high-intensity physical activity like interval training. While 55% of the energy comes from fat at 40 % of maximum oxygen uptake, this is reduced to 20% at an intensity of 80%. This knowledge has led to recommendations that people desiring to burn as much fat as possible should do low-intensity exercise – a message amplified by the use of terms like “fat burning exercise.” However, claims like these are based on a misunderstanding. In reality, it is the total energy spent, as opposed to the percentage of energy from fat that should be the concern. Under high-intensity exercise, not only is the energy expenditure per unit of time greater, but totally, more fat is metabolized compared to low-intensity exercise, even if the percentage of energy from carbohydrate is greater. For instance, at 75% of maximum oxygen uptake, the energy from fat and carbohydrates can be, respectively, approximately 30 and 70%, while at 40% of maximum oxygen uptake (so-called “fat burning exercise”), they might be roughly 50-50. If in the first case the energy expenditure were 12 kcal/min, and in the second it were 6 kcal/min, in the course of an hour one would use 720 kcal and 360 kcal, respectively. Of these, respectively 216 kcal and 180 kcal would be from fat. This shows that during high-intensity exercise, not only is more energy spent, but more fat is also burned per unit of time. Similarly, you don’t lose more fat if you bike a given distance at a relaxed rate versus biking the same distance at a higher speed in a shorter amount of time.
______
Myth of muscle converting into fat tissue:
Some people incorrectly believe that muscle tissue will turn into fat tissue once a person stops exercising. This is not literally true — fat tissue and muscle tissue are fundamentally different — but the common expression that “muscle will turn to fat” is truthful in the sense that catabolism of muscle fibers for energy can result in excess glucose being stored as fat. Moreover, the composition of a body part can change toward less muscle and more fat, so that a cross-section of the upper-arm for example, will have a greater area corresponding to fat and a smaller area corresponding to muscle. This is not muscle “turning into fat” however — it is simply a combination of muscle atrophy and increased fat storage in different tissues of the same body part. Another element of increased fatty deposits is that of diet, as most trainees will not significantly reduce their diet in order to compensate for the lack of exercise/activity.
______
Myth of lactate and muscle fatigue:
Certainly, repeated, high intensity contractions lead to muscle fatigue. Glycogenolysis and glycolysis can lead to lactic acidosis and disturbances to muscle and plasma pH. Furthermore, contractions also precipitate a variety of other disturbances to cell homeostasis including perturbations to energy charge and ion balances.
_
_
When you exercise, your body uses oxygen to break down glucose for energy. During intense exercise, there may not be enough oxygen available to complete the process, so a substance called lactate is made. Researchers once attributed fatigue to a build-up of lactic acid in muscles. However, this is no longer believed. Most athletes believe that lactate causes muscle fatigue by making the muscles too acidic to contract effectively. This is not true. While the muscles do become more acidic during exercise, lactate is not the cause. In any case, far from hastening fatigue, lactate accumulation in the muscles actually delays fatigue by mitigating the effects of a phenomenon known as depolarization. Each muscle contraction involves an action potential that activates voltage sensors, and so releases Ca2+ ions from the muscle fibre’s sarcoplasmic reticulum. The action potentials that cause this require also ion changes: Na influxes during the depolarization phase and K effluxes for the repolarization phase. Cl− ions also diffuse into the sarcoplasm to aid the repolarization phase. During intense muscle contraction, the ion pumps that maintain homeostasis of these ions are inactivated and this (with other ion related disruption) causes ionic disturbances. This causes cellular membrane depolarization. During intense exercise, your muscles lose power in the same way a battery does: by becoming depolarized. The accumulation of lactate in muscle tissue during intense exercise partly counteracts the effect of depolarization. Lactate does not cause post-exercise muscle soreness. The simplest proof of this is the fact that very little lactate is produced during highly prolonged, low-intensity exercise, and yet it is this very type of exercise that leaves the muscles sorest in the following days. Post-exercise muscle soreness is actually caused by simple mechanical damage to muscle fibers, free radical damage, and inflammation. Without lactate, you would not get fitter in response to training to the same degree you do with it. Lactate production during intense exercise stimulates a phenomenon called mitochondrial biogenesis after exercise. The mitochondria are little factories inside the muscle cells where aerobic metabolism occurs—that is, where oxygen is used to break down fats and glucose to yield energy. An increase in the concentration of mitochondria inside muscle cells is one of the major adaptations to training that improve endurance performance. And lactate makes it happen. This is one of the reasons high-intensity interval training is such a potent performance booster. We are aware that lactate produced during exercise can be “recycled” into glucose and used as fuel by the muscles, heart, and brain. But few are aware that lactate is also metabolized aerobically in the mitochondria as a direct fuel for muscle contractions. In fact, it has been estimated that roughly 75 percent of the lactate produced inside the muscle cells is used in this way, and only 25 percent leaks out into the bloodstream, where it can be measured through blood lactate testing. Some of the world’s best endurance athletes, such as Michael Phelps, appear to produce significantly less lactate during intense exercise than lesser athletes. This makes sense if you believe that lactate is a toxic waste product that causes fatigue and does not help exercise performance in any way. But it doesn’t make sense in the light of current knowledge about the effects of lactic acid. And it’s also very unlikely to be true. In all likelihood, the reason there is less lactate in the blood of Michael Phelps during intense exercise is not that their muscles produce less, but rather that they use more. If, in the average endurance athlete, 75 percent of lactate is burned in the mitochondria and only 25 percent escapes into the bloodstream, in come very special athletes, perhaps 85 percent of lactate is burned and only 15 percent escapes.
_______
_______
Muscles, Oxygen and Intensity of Exercise:
If you are going to be exercising for more than a couple of minutes, your body needs to get oxygen to the muscles or the muscles will stop working. Just how much oxygen your muscles will use depends on two processes: getting blood to the muscles and extracting oxygen from the blood into the muscle tissue. Your working muscles can take oxygen out of the blood three times as well as your resting muscles. Your body has several ways to increase the flow of oxygen-rich blood to working muscle:
•increased local blood flow to the working muscle
•diversion of blood flow from nonessential organs to the working muscle
•increased flow of blood from the heart (cardiac output)
•increased rate and depth of breathing
•increased unloading of oxygen from hemoglobin in working muscle
These mechanisms can increase the blood flow to your working muscle by almost five times. That means that the amount of oxygen available to the working muscle can be increased by almost 15 times!
_
Vigorous physical activity (such as exercise or hard labor) increases the body’s demand for oxygen. The first-line physiologic response to this demand is an increase in heart rate, breathing rate, and depth of breathing. Oxygen consumption (VO2) during exercise is best described by the Fick Equation: VO2 = Q X (a-v O2diff), which states that the amount of oxygen consumed is equal to cardiac output (Q) multiplied by the difference between arterial and venous oxygen concentrations. More simply put, oxygen consumption is dictated by the quantity of blood distributed by the heart as well as the working muscle’s ability to take up the oxygen within that blood; however, this is a bit of an oversimplification. Although cardiac output is thought to be the limiting factor of this relationship in healthy individuals, it is not the only determinant of VO2 max. That is, factors such as the ability of the lung to oxygenate the blood must also be considered. Various pathologies and anomalies cause conditions such as diffusion limitation, ventilation/perfusion mismatch, and pulmonary shunts that can limit oxygenation of the blood and therefore oxygen distribution. In addition, the oxygen carrying capacity of the blood is also an important determinant of the equation. Oxygen carrying capacity is often the target of exercise (ergogenic aids) aids used in endurance sports to increase the volume percentage of red blood cells (hematocrit), such as through blood doping or the use of erythropoietin (EPO). Furthermore, peripheral oxygen uptake is reliant on a rerouting of blood flow from relatively inactive viscera to the working skeletal muscles, and within the skeletal muscle, capillary to muscle fiber ratio influences oxygen extraction.
_
VO2 max (maximum oxygen uptake):
The maximum rate of oxygen consumption during the aerobic catabolism of pyruvic acid/fatty acid is called maximal oxygen uptake. VO2 max (also maximal oxygen consumption, maximal oxygen uptake, peak oxygen uptake or maximal aerobic capacity) is the maximum rate of oxygen consumption as measured during incremental exercise, most typically on a motorized treadmill. Maximal oxygen consumption reflects the aerobic physical fitness of the individual, and is an important determinant of their endurance capacity during prolonged, sub-maximal exercise. Maximal oxygen uptake (VO2 max) is widely accepted as the single best measure of cardiovascular fitness and maximal aerobic power. The name is derived from V – volume, O2 – oxygen, max – maximum. Maximal oxygen uptake is determined by sex (higher in males), age (highest at approximately age 20 y), and size (increases with body size). This rate in short-term studies is found to increase only 10% with the effect of training. However, that of a person who runs in marathons is 45% greater than that of an untrained person. This is believed to be partly genetically determined (e.g., stronger respiratory muscles, larger chest size in relation to body size) and partly due to long-term training. Highly trained athletes can have maximal oxygen uptakes that are twice that of average people, probably owing to a combination of genetics and training. As a result, highly trained athletes are capable of greater muscular activity without increasing their lactic acid production and have lower oxygen debts, which is why they do not become short of breath as readily as untrained individuals.
_
The usual VO2 measurements are in L/min; however, if the size of the individual needs to be accounted for, the measurements may be in mL/kg/min. One metabolic unit (MET) equals the VO2 at rest. The estimate of the value of one MET is 3.5 mL of oxygen per kg/min. Conversion of VO2 measurements may be obtained by dividing the value of the VO2 in mL of oxygen per kg/min by the value of one MET or 3.5. For example, a VO2 measurement of 35 mL of oxygen per kg/min is equivalent to an output of 10 METs. Absolute values of VO2 max are typically 40-60% higher in men than in women. The average untrained healthy male will have a VO2 max of approximately 35–40 mL/kg/min. The average untrained healthy female will score a VO2 max of approximately 27–31 mL/kg/min. In sports where endurance is an important component in performance, such as cycling, rowing, cross-country skiing, swimming and running, world-class athletes typically have high VO2 max. Elite male runners can consume up to 85 mL/kg/min, and female elite runners can consume about 77 mL/kg/min. In other words, while doing maximum effort exercise, an average person uses oxygen 10 times that of rest and highly trained athlete doing the same exercise uses oxygen half of that of average person as intensity of the same exercise will be lower in highly trained athlete. In other words, maximum effort exercise performed by highly trained athlete is of double intensity than maximum effort exercise performed by average man.
_
Training enhances the ability of the body, in particular the muscle cells, to better handle oxygen. Muscle must be able to use oxygen efficiently to keep anaerobic metabolism at a given level of effort to a minimum. Cardiac output is a major determinant of oxygen uptake. VO2max declines with age as the maximum HR declines. This is one of the major factors causing the approximately 7% decline with each decade of life after age 30 years. Muscle training and use of oxygen at the end organ, muscle, is the second factor that affects oxygen uptake. The arterial-venous oxygen difference comes about as a combination of arterial oxygen content, shunting of blood to muscles, and the muscle extraction of oxygen. Training results in a more efficient heart and an increase in the maximum stroke volume (SV). An increase in VO2 results in an ease in the stress of a given workload. When maximum SV is increased, the heart can work more efficiently at a given pulse rate. This lessens the necessity of an increased pulse at a given workload. Resting pulse is lower, as is the pulse at any given workload.
_
Components of exercise:
An exercise prescription generally includes the following specific recommendations:
• Type of exercise or activity (e.g., walking, swimming, cycling)
• Specific workloads (e.g., watts, walking speed)
• Duration and frequency of the activity or exercise session
• Intensity of exercise
• Precautions regarding certain orthopedic (or other) concerns or related comments
_
Aerobic activity causes a person’s heart to beat faster than usual.
Aerobic physical activity has three components:
•Intensity, or how hard a person works to do the activity. The intensities most often examined are moderate intensity (equivalent in effort to brisk walking) and vigorous intensity (equivalent in effort to running or jogging);
•Frequency, or how often a person does aerobic activity; and
•Duration, or how long a person does an activity in any one session.
Although these components make up a physical activity profile, research has shown that the total amount of physical activity (minutes of moderate–intensity physical activity, for example) is more important for achieving health benefits than is any one component (frequency, intensity, or duration).
_
Muscle-Strengthening Activity:
This kind of activity, which includes resistance training and lifting weights, causes the body’s muscles to work or hold against an applied force or weight. These activities often involve relatively heavy objects, such as weights, which are lifted multiple times to train various muscle groups. Muscle-strengthening activity can also be done by using elastic bands or body weight for resistance (climbing a tree or doing push-ups, for example).
Muscle-strengthening activity also has three components:
•Intensity, or how much weight or force is used relative to how much a person is able to lift;
•Frequency, or how often a person does muscle strengthening activity; and
•Repetitions, or how many times a person lifts a weight (analogous to duration for aerobic activity). The effects of muscle-strengthening activity are limited to the muscles doing the work. It’s important to work all the major muscle groups of the body: the legs, hips, back, abdomen, chest, shoulders, and arms.
_
Exercise intensity:
Intensity refers to the rate at which the activity is being performed or the magnitude of the effort required to perform an activity or exercise. Intensity is the rate of energy expenditure of exercise. It can be thought of “How hard a person works to do the activity”. The intensity of different forms of physical activity varies between people. The intensity of physical activity depends on an individual’s previous exercise experience and their relative level of fitness. Exercise intensity refers to how much energy is expended when exercising. Perceived intensity varies with each person. It has been found that intensity has an effect on what fuel the body uses and what kind of adaptations the body makes after exercise. Intensity is the amount of physical power (expressed as a percentage of the maximal oxygen consumption) that the body uses when performing an activity. For example, exercise intensity defines how hard the body has to work to walk a mile in 20 minutes. Heart Rate is typically used as a measure of exercise intensity. Heart rate can be an indicator of the challenge to the cardiovascular system that the exercise represents. The most precise measure of intensity is oxygen consumption (VO2). VO2 represents the overall metabolic challenge that an exercise imposes. There is a direct linear relationship between intensity of aerobic exercise and VO2. Our maximum intensity is a reflection of our maximal oxygen consumption (VO2 max). Such a measurement represents a cardiovascular fitness level. VO2 is measured in METs (mL/kg/min). One MET, which is equal to 3.5 ml/kg per minute, is considered to be the average resting energy expenditure of a typical human being. Intensity of exercise can be expressed as multiples of resting energy expenditure. An intensity of exercise equivalent to 6 METs means that the energy expenditure of the exercise is six times the resting energy expenditure. Some studies measure exercise intensity by having subjects perform exercise trials to determine peak power output, which may be measured in watts, heart rate, or (on a cycle) average cadence (cycling). This approach attempts to gauge overall workload.
_
The Metabolic Equivalent of Task (MET):
MET is the ratio of the work metabolic rate to the resting metabolic rate (RMR). One MET is defined as 1 kcal/kg/hour and is roughly equivalent to the energy cost of sitting quietly. A MET also is defined as oxygen uptake in ml/kg/min with one MET equal to the oxygen cost of sitting quietly, equivalent to 3.5 ml/kg/min. 1 MET is also defined as 58.2 W/m2 (18.4 Btu/h·ft2), which is equal to the rate of energy produced per unit surface area of an average person seated at rest. MET values of activities range from 0.9 (sleeping) to 23 (running at 22.5 km/h or a 4:17 mile pace). Although the RMR of any person may deviate from the reference value, MET can be thought of as an index of the intensity of activities: for example, an activity with a MET value of 2, such as walking at a slow pace (e.g., 3 km/h) would require twice the energy that an average person consumes at rest (e.g., sitting quietly). MET is used as a means of expressing the intensity and energy expenditure of activities in a way comparable among persons of different weight. Actual energy expenditure (e.g., in calories or joules) during an activity depends on the person’s body mass; therefore, the energy cost of the same activity will be different for persons of different weight. However, since the RMR is also dependent on body mass in a similar way, it is assumed that the ratio of this energy cost to the RMR of each person will remain more or less stable for the specific activity and thus independent of each person’s weight. The 1 MET reference value of 1 kcal·kg−1·h−1 is used by convention and refers to a typical metabolism at rest of an “average” individual. It must not be confused or misused as an approximation of Basal Metabolic Rate (BMR), which is the minimum metabolic rate obtained under specified conditions. This is illustrated by the fact that sleeping has a MET of 0.9, while an individual’s normal sleeping metabolism may be greater than the BMR.
_
MET-minutes:
For example, 1 MET is the rate of energy expenditure while at rest. A 4 MET activity expends 4 times the energy used by the body at rest. If a person does a 4 MET activity for 30 minutes, he or she has done 4 x 30 = 120 MET-minutes (or 2.0 MET-hours) of physical activity. A person could also achieve 120 MET-minutes by doing an 8 MET activity for 15 minutes.
_
MET-Minutes and Health Benefits:
A key finding of various studies is that the health benefits of physical activity depend mainly on total weekly energy expenditure due to physical activity. In scientific terms, this range is 500 to 1,000 MET-minutes per week. A range is necessary because the amount of physical activity necessary to produce health benefits cannot yet be identified with a high degree of precision; this amount varies somewhat by the health benefit. For example, activity of 500 MET-minutes a week results in a substantial reduction in the risk of premature death, but activity of more than 500 MET-minutes a week is necessary to achieve a substantial reduction in the risk of breast cancer. There is a dose-response relationship between physical activity and health benefits. A range of 500 to 1,000 MET-minutes of activity per week provides substantial benefit, and amounts of activity above this range have even more benefit. Amounts of activity below this range also have some benefit. The dose-response relationship continues even within the range of 500 to 1,000 MET-minutes, in that the health benefits of 1,000 MET-minutes per week are greater than those of 500 MET-minutes per week.
_
Two Methods of assessing Aerobic Intensity:
The intensity of aerobic physical activity can be defined in absolute or relative terms.
Absolute Intensity:
Absolute moderate-intensity or vigorous-intensity physical activity is necessary for substantial health benefits, and absolute aerobic intensity is defined in terms of METs as follows:
•Light-intensity activities are defined as 1.1 MET to 2.9 METs.
•Moderate-intensity activities are defined as 3.0 to 5.9 METs. Walking at 3.0 miles per hour requires 3.3 METs of energy expenditure and is therefore considered a moderate-intensity activity.
•Vigorous-intensity activities are defined as 6.0 METs or more. Running at 10 minutes per mile (6.0 mph) is a 10 MET activity and is therefore classified as vigorous intensity.
_
Figure above shows the movement continuum: illustrating different physical activity intensities. METs= metabolic equivalent tasks. SB= sedentary behavior.
_
Relative Intensity:
Relative intensity refers to the percent of aerobic power utilized during exercise and is expressed as percent of maximal heart rate or percent of VO2max. Moderate-intensity activities are those performed at a relative intensity of 40% to 60% of VO2max (or absolute intensity of 4 to 6 METs). Vigorous-intensity activities are those performed at a relative intensity of 60% to 80% of VO2max (or absolute intensity of 6 to 8 METs). For example, brisk walking at 3 miles/hr has an absolute intensity of 4 METs. In relative terms, this intensity is considered light for a 20-year-old healthy person but represents a vigorous intensity for an 80-year-old person. Another example, two individuals with different measures of VO2 max, running at 7 mph are running at the same absolute intensity (miles/hour) but a different relative intensity (% of VO2 max expended). The individual with the higher VO2 max is running at a lower intensity at this pace than the individual with the lower VO2 max is.
_
| Physical activity | MET |
| Light intensity activities: | < 3 |
| sleeping | 0.9 |
| watching television | 1.0 |
| writing, desk work, typing | 1.5 |
| walking, 1.7 mph (2.7 km/h), level ground, strolling, very slow | 2.3 |
| walking, 2.5 mph (4 km/h) | 2.9 |
| Moderate intensity activities: | 3 to 6 |
| bicycling, stationary, 50 watts, very light effort | 3.0 |
| walking 3.0 mph (4.8 km/h) | 3.3 |
| calisthenics, home exercise, light or moderate effort, general | 3.5 |
| walking 3.4 mph (5.5 km/h) | 3.6 |
| bicycling, <10 mph (16 km/h), leisure, to work or for pleasure | 4.0 |
| bicycling, stationary, 100 watts, light effort | 5.5 |
| sexual activity | 5.8 |
| Vigorous intensity activities: | > 6 |
| jogging, general | 7.0 |
| calisthenics (e.g. pushups, situps, pullups, jumping jacks), heavy, vigorous effort | 8.0 |
| running jogging, in place | 8.0 |
| rope jumping | 10.0 |
_
150 minutes (2 hours and 30 minutes) of moderate-intensity activity per week could be regarded as (roughly) equivalent to 500 MET-minutes per week. In fact, 3.3 METs for 150 minutes per week is equal to 500 MET-minutes per week. By recommending that adults do at least 150 minutes of moderate-intensity activity per week, adults will achieve 500 to 1,000 MET-minutes per week if the intensity is 3.3 METs or greater. As noted earlier, walking at 3.0 miles per hour is a 3.3 MET activity. Hence, it is appropriate to communicate to the public that a “brisk walk” is walking at 3.0 miles per hour or faster. By recommending at least 75 minutes (1 hour and 15 minutes) per week of vigorous-intensity activity, adults who choose to do vigorous-intensity activity will also generally achieve 500 to 1,000 MET-minutes per week. The lower limit of vigorous intensity activity (6.0 METs) is twice the lower limit of moderate-intensity activity (3.0 METs). So, 75 minutes of vigorous-intensity activity per week is roughly equivalent to 150 minutes of moderate-intensity activity per week. As the MET range for vigorous-intensity activity has no upper limit, highly fit people can even exceed 1,000 MET-minutes in 75 minutes by doing activities requiring 13.4 MET or more. It is not of concern that the vigorous-intensity guideline “misleads” people with a high degree of fitness into doing more activity than is really required to meet the guidelines. Highly fit people have already decided to do large amounts of physical activity, as this is the only way to achieve this degree of fitness. Because 150 minutes of moderate-intensity activity and 75 minutes of vigorous-intensity activity are the minimum amounts, the rule of thumb becomes that 1 minute of vigorous-intensity activity counts the same as 2 minutes of moderate-intensity activity.
__
Energy expenditure calculations:
Per-minute calculation: To calculate kilocalories per minute (kcal/min), multiply the METs times 3.5 times body weight in kilograms (kg) and divide by 200 (i.e., kcal/min = [MET X 3.5 X kg body weight]/200). For example, the energy (caloric) expenditure of a 70-kg individual at a prescribed 6-MET capacity with a weekly goal of 1000 kcl per week is calculated as (6 X 3.5 X 70 kg)/200, which equals 7.35 kcal/min (30.87 kJ/min). To convert kilocalories to kilojoules, note that 1 kcal = 4.2 kJ.
Per-week calculation: This determines the exercise duration per week. Using the numbers from the example above, divide 1000 kcal (4200 kJ) by 7.35 kcal/min (30.87 kJ/min), which equals 136 min/week or approximately 20-30 minutes, 6 d/wk.
_
Without using any calculator, you can classify intensity of exercise as:
•Light exercise
The exerciser is able to talk while exercising. Going for a walk is an example of light exercise.
•Moderate exercise
The exerciser feels slightly out of breath during the session. Moderate-intensity aerobic activity means you’re working hard enough to raise your heart rate and break a sweat. One way to tell if you’re working at a moderate intensity is if you can still talk but you can’t sing the words to a song. Examples could be walking briskly, cycling moderately, or walking up a hill.
•Vigorous exercise
The exerciser is panting during the activity. If your heart rate increases a lot and you are breathing so hard that it is difficult to carry on a conversation, you are probably doing vigorous-intensity activity. The exerciser feels his/her body is being pushed much nearer its limit, compared to the other two intensities. This could include running, cycling fast, and heavy weight training.
__
Heart rate as surrogate measure of energy expenditure and exercise intensity:
During moderate physical activity, there is a linear relationship between heart rate and oxygen consumption. This heart rate oxygen consumption relationship is subject to both intra- and inter-individual variability. Heart rate may be partially dissociated from energy expenditure by factors such as emotion, posture and environmental conditions. Heart rate monitoring, for estimating free-living energy expenditure, has been extensively validated using indirect calorimetry, doubly labelled water and wholeroom respirometry, and reported differences between measures range from -20% to +25%. In large groups of people, heart rate monitoring provides one of the most efficient and economical means of estimating energy expenditure. In addition, heart rate monitoring provides useful insights into the type of activity being undertaken over the measurement period. Other assessment methods, such as doubly labelled water, can only convey the total amount of physical activity measured, whereas heart rate monitoring provides physiological information about the type of activities being performed and describes the nature of day-to-day variability in energy expenditure. While whole-room respirometry and indirect calorimetry provide physiological information about the nature of the activity being performed, these tools are not only costly to maintain, but often take the participant out of his or her natural environment for the duration of the measurement period.
_
Heart Rate Goal:
Heart rate is the standard guide for determining aerobic exercise intensity. It is useful for people training at aerobic intensity, or people with certain cardiac risk factors who have been set a maximum heart rate by their doctor. You can determine your heart rate by counting your pulse, or by using a heart rate monitor. To feel your own pulse, press the first two fingers of one hand gently down on the inside of the wrist or under the jaw on the right or left side of the front of the neck. You should feel a faint pounding as blood passes through the artery. Each pounding is a beat.
_
There are different types of heart rates.
1. Resting heart rate. The average heart rate for a person at rest is 60 – 80 beats per minute. It is usually lower for people who are physically fit, and often rises as you get older. You can determine your resting heart rate by counting how many times your heart beats in one minute. The best time to do this is in the morning after a good night’s sleep before you get out of bed.
2. Maximum heart rate. To determine your own maximum heart rate per minute, subtract your age from 220. For example, if you are 45, you would calculate your maximum heart rate as follows: 220 – 45 = 175.
3. Target heart rate. Your target rate is 50 – 75% of your maximum heart rate. You should measure your pulse off and on while you exercise to make sure you stay within this range. After about 6 months of regular exercise, you may be able to increase your target heart rate to 85% (but only if you can comfortably do so).
Certain heart medications may lower your maximum and target heart rates. Always check with your doctor before starting an exercise program.
Note: Swimmers should use a heart rate target of 75% of the maximum and then subtract 12 beats per minute. The reason for this is that swimming will not raise the heart rate quite as much as other sports because of the so-called “diving reflex,” which causes the heart to slow down automatically when the body is immersed in water.
_
| Target Heart Rates for a One-minute Pulse Count | ||
| Age | Low | High |
| (50% max.) | (75% max.) | |
| 20 | 100 | 150 |
| 30 | 95 | 142 |
| 40 | 90 | 135 |
| 50 | 85 | 127 |
| 60 | 80 | 120 |
_
Intensity guide for aerobic exercise using heart rate:
When target heart rate is 60 to 80 % of maximum heart rate, it is moderate intensity exercise.
_______
_______
In a nutshell, I classify and summarize exercise in the following table:
| Elements | Light exercise | Moderate exercise (cardio) | Vigorous (intense) exercise |
| Oxygen used or not | Aerobic | Aerobic | Anaerobic plus aerobic |
| Fuel used | Fat and carbohydrate | Carbohydrate and fat | Predominantly carbohydrate |
| MET | 1.1 to 2.9 | 3 to 5.9 | 6 to 10 and even more |
| Oxygen consumption VO2 | Less than 40 % of VO2 max | 40 to 60 % of VO2 max | 60 to 85 % of VO2 max |
| Target heart rate | < 60 % of maximum heart rate | 60 to 80 % of maximum heart rate | 80 to 90 % of maximum heart rate aerobic glycolysis and > 90 % uses anaerobic glycolysis |
| Duration | At least > 10 minutes e.g. strolling | At least > 10 minutes e.g. brisk walking | < 2 minutes e.g. weight lifting, > 2 minutes e.g. running |
| How exerciser react | The exerciser is able to talk fluently while exercising | You feel slightly out of breath, sweating but can still talk | you are breathing so hard that it is difficult to carry on a conversation |
| Health benefits | Little benefits | Definite cardiovascular benefits with 150 minutes of exercise per week | Building muscles and strengthening bones in short duration and cardiovascular benefit with 75 minutes of exercise per week |
Maximum effort exercise is when exerciser makes so much efforts that he/she utilizes full VO2 max achieving maximum heart rate. Over-exercise is when person exercises for more than 2 hours continuously with the sole exception of highly trained athlete e.g. highly trained marathon runner
_
Exercise Capacity:
Exercise capacity is the maximum amount of physical exertion that a patient can sustain. Exercise capacity is best defined in terms of maximal effort tolerance. An accurate assessment of exercise capacity requires that maximal exertion is sufficiently prolonged to have a stable (or steady state) effect on the circulation and that the pattern of patient response is consistent when exertion is repeated. The function of several body systems, particularly the circulation and respiratory systems, is adequately tested only during exercise. Each system has reserve capacity far in excess of that needed to sustain normal, asymptomatic body functioning at rest and during modest activity. Many disease processes affecting the circulation or respiration cause progressive loss of physiologic function. Such diseases are likely to manifest themselves initially by a reduction in cardiac or pulmonary reserve. Since these reserve capacities are tested only during exercise, the early (and potentially remediable) stages of diseases of this sort may produce symptoms only with strenuous effort. By assessing the maximum capability of patients to perform exercise, the examining physician evaluates, at least in qualitative terms, the reserve capacity of each of the organ systems contributing to the exercise response. Impairment of exercise capacity should alert the physician to a potential need for more specific and precise studies of organ function. Exercise performance reflects a coordinated response of cardiovascular, pulmonary, and neural function along with the action of exercising muscles. Exercise induces graded increases in heart rate, arterial pressure, cardiac output, myocardial contractility, and rate and depth of respiration. Rapid, reversible shifts also occur in the distribution of blood flow and in blood composition. These changes are orchestrated by the central nervous system, which is responding to direct cortical input and to neural and humoral feedback from exercising muscles. Neural control of cardiovascular function is exerted, in part, through characteristic increases in sympathetic stimulation and reciprocal decreases in para-sympathetic stimulation. During steady effort, cardiovascular and pulmonary parameters begin to stabilize (after 1 to 2 minutes of rapid change) at levels appropriate for a specific intensity of exercise in a particular patient. These steady-state levels can be used to characterize patient performance.
_________
________
Functional capacity:
Functional capacity is defined as the ability of a cell, organ, system, or body to maintain homeostasis within their narrow limits of survival in response to a specified stress. If an external stress disrupts homeostasis beyond an organism’s functional capacity, life may not be sustained. Diminished ability to adapt to stressors increases the likelihood of death. Functional capacity is pliable; declining rapidly with extreme physical inactivity or more slowly with aging, while preventing inactivity can increase functional capacity (considered in specific detail in the aging section). Importantly, a direct relationship between functional capacity and survival is a cornerstone of general medicine theory. A major predictor of functional capacity is maximal aerobic capacity (VO2max), which while directly testing cardiovascular fitness and integrity also represents a combination of other physiologic components. For instance, VO2max also depends on pulmonary and muscle function, health status of other organ systems, nutritional status, medications, orthopedic limitations, and others. An aerobic functional capacity in patients under 4-metabolic equivalents (METs), a typical demand during normal daily activities, increases postoperative (time from admission to discharge from surgery) cardiac and long-term risks. In another study, patients were grouped by MET capacity in relationship to complication prevalence after they underwent angiographically verified coronary artery disease and subsequent open abdominal nonvascular surgery. Those from the group < 4 METs had cardiologic complications in 64% of cases, the 4–7 METs group had 29%, and the 7–10 METs group had 8%. These remarkable findings can be extrapolated to other stresses where the probability of complications, and even survival, is dependent upon the functional capacity needed to maintain homeostasis.
_______
_______
Biological effects of exercise:
There are number of biological effects that occur, from head to toe, when you exercise. This includes changes in your:
•Muscles, which use glucose and fatty acid to generate ATP for contraction and movement. To create more ATP, your body needs extra oxygen, so breathing increases and your heart starts pumping more blood to your muscles. Without sufficient oxygen, lactic acid will form instead. Tiny tears in your muscles make them grow bigger and stronger as they heal.
•Lungs. As your muscles call for more oxygen (as much as 15 times more oxygen than when you’re at rest), your breathing rate increases. Once the muscles surrounding your lungs cannot move any faster, you’ve reached what’s called your VO2 max—your maximum capacity of oxygen use. The higher your VO2 max, the fitter you are.
•Heart. As mentioned, your heart rate increases with physical activity to supply more oxygenated blood to your muscles. The fitter you are, the more efficiently your heart can do this, allowing you to work out longer and harder. As a positive side effect, this increased efficiency will also reduce your resting heart rate. Your blood pressure will also decrease as a result of new blood vessels forming.
•Brain. The increased blood flow also benefits your brain, allowing it to almost immediately function better. As a result, you tend to feel more focused after a workout. Furthermore, exercising regularly will promote the growth of new brain cells. In your hippocampus, these new brain cells help boost memory and learning. When you work out regularly, your brain gets used to this frequent surge of blood and adapts by turning certain genes on or off. Many of these changes boost brain cell function and protect from diseases such as Alzheimer’s, Parkinson’s or even stroke, and ward off age-related decline. A number of neurotransmitters are also triggered, such as endorphins, serotonin, dopamine, glutamate, and GABA. Some of these are well-known for their role in mood control. Exercise, in fact, is one of the most effective prevention and treatment strategies for depression.
•Joints and bones, as exercise can place as much as five or six times more than your body weight on them. Peak bone mass is achieved in adulthood and then begins a slow decline, but exercise can help you to maintain healthy bone mass as you get older. Weight-bearing exercise is actually one of the most effective remedies against osteoporosis, as your bones are very porous and soft, and as you get older your bones can easily become less dense and hence, more brittle — especially if you are inactive.
_
Routine physical activity is also associated with improved psychological well-being (e.g., through reduced stress, anxiety and depression. Psychological well-being is particularly important for the prevention and management of cardiovascular disease, but it also has important implications for the prevention and management of other chronic diseases such as diabetes, osteoporosis, hypertension, obesity, cancer and depression.
_
While evidence of the physical and mental benefits of exercise abounds, there exists no single, coherent theory that adequately explains why—despite many proposed explanations. One biological explanation asserts that exercise increases body temperature, adrenal and steroid activity, as well as the release of certain neurotransmitters such as endorphins. Another approach is psychosocial in origin and posits that exercise acts as a type of distraction, biofeedback, meditation, or psychological buffer and can result in an increased sense of self-efficacy, control, and mastery. Furthermore, some researchers have suggested that many of the derived psychological benefits may be due to expectancy effects; that is, “people may demonstrate improvement in psychological functioning simply because they are expecting self-enhancement”.
_
Changes in endothelial function may be a particularly important adaptation to routine physical activity. Endothelial dysfunction has been observed with aging, smoking and multiple chronic disease states, including coronary artery disease, congestive heart failure, stroke, type 2 diabetes, hypertension, hypercholesterolemia and obesity. Regular aerobic activity has been found to improve vascular function in adults independent of changes in other risk factors and has been said to result in a shear-stress–mediated improvement in endothelial function, which confers a health benefit to a number of disease states.
_
Although most research into the mechanisms of how physical activity and fitness improve health outcomes has dealt with the relation between cardiovascular disease and physical activity, researchers have also evaluated the primary mechanisms responsible for decreases in the risk and severity of individual disease states. In fact, despite the adaptations that are of global benefit for multiple disease states, physical activity also results in specific adaptations that affect individual disease states. For instance, in type 2 diabetes, adaptations that affect glucose homeostasis are of great importance. As reviewed by Ivy, a series of changes (independent of changes in body mass) occur as a result of regular physical activity, including increased glycogen synthase and hexokinase activity, increased GLUT-4 protein and mRNA expression, and improved muscle capillary density (resulting in improved glucose delivery to the muscle). A series of mechanisms may explain the 46% reduction in cancer rates observed with regular physical activity, including reductions in fat stores, increased energy expenditure offsetting a high-fat diet, activity-related changes in sex hormone levels, immune function, insulin and insulin-like growth factors, free-radical generation, and direct effects on the tumour.
_
Muscle as a secretory organ: Myokine research:
Skeletal muscle is the largest organ in the body. Skeletal muscles are primarily characterized by their mechanical activity required for posture, movement, and breathing, which depends on muscle fiber contractions. However, skeletal muscle is not just a component in our locomotor system. Recent evidence has identified skeletal muscle as a secretory organ. New research on the endocrine functions of contracting muscles has shown that both aerobic and anaerobic exercise promote the secretion of myokines, with attendant benefits including growth of new tissue, tissue repair, and various anti-inflammatory functions, which in turn reduce the risk of developing various inflammatory diseases. Myokine secretion in turn is dependent on the amount of muscle contracted, and the duration and intensity of contraction. As such, both types of exercise produce endocrine benefits. It is suggested that cytokines and other peptides that are produced, expressed, and released by muscle fibers and exert either autocrine, paracrine, or endocrine effects should be classified as “myokines.” The muscle secretome consists of several hundred secreted peptides. This finding provides a conceptual basis and a whole new paradigm for understanding how muscles communicate with other organs such as adipose tissue, liver, pancreas, bones, and brain. In addition, several myokines exert their effects within the muscle itself. Many proteins produced by skeletal muscle are dependent upon contraction. Therefore, it is likely that myokines may contribute in the mediation of the health benefits of exercise. In a 2012 article regarding myokine research, Pedersen and Febbraio concluded that “physical inactivity and muscle disuse lead to loss of muscle mass and accumulation of visceral adipose tissue and consequently to the activation of a network of inflammatory pathways, which promote development of insulin resistance, atherosclerosis, neurodegeneration and tumour growth and, thereby, promote the development of a cluster of chronic diseases. By contrast, the finding that muscles produce and release myokines provides a molecular basis for understanding how physical activity could protect against premature mortality…. Physical inactivity or muscle disuse potentially leads to an altered or impaired myokine response and/or resistance to the effects of myokines, which explains why lack of physical activity increases the risk of a whole network of diseases, including cardiovascular diseases, T2DM (Type 2 Diabetes Mellitus), cancer and osteoporosis.
_
Physical activity and the endocannabinoid system: an overview: 2014:
Recognized as a “disease modifier”, physical activity (PA) is increasingly viewed as a more holistic, cost-saving method for prevention, treatment and management of human disease conditions. The traditional view that PA engages the monoaminergic and endorphinergic systems has been challenged by the discovery of the endocannabinoid system (ECS), composed of endogenous lipids, their target receptors, and metabolic enzymes. Indeed, direct and indirect evidence suggests that the ECS might mediate some of the PA-triggered effects throughout the body. Moreover, it is now emerging that PA itself is able to modulate ECS in different ways. ECS must be tightly regulated during PA, in order to maintain its beneficial effects on cognition, mood, and nociception, while avoiding impaired energy metabolism, oxidative stress, and inflammatory processes.
_
Exercise and antioxidants:
Antioxidants prevent health-promoting effects of physical exercise in humans: 2009 study:
Exercise, as well as weight loss, has been linked to activation of mitochondrial metabolism, and reduced mitochondrial metabolism has been functionally connected with type 2 diabetes. Mitochondria, however, are also the main source of reactive oxygen species (ROS), which are inevitable by-products of oxidative glucose metabolism. Muscle is also known to generate free radicals, especially during contraction and physical exercise. It has been suggested that ROS may mediate some health-promoting effects, at least in nonprimate model systems.
_
Mitohormesis links physical exercise and subsequent formation of reactive oxygen species to insulin sensitivity and antioxidant defense. Physical exercise exerts ameliorating effects on insulin resistance by increasing mitochondrial formation of reactive oxygen species in skeletal muscle to induce expression of PGC1α, PGC1β, and PPARγ as inducers of insulin sensitivity, as well as superoxide dismutases 1 and 2 and glutathione peroxidase 1, key enzymes of ROS defence. Notably, by blocking exercise-dependent formation of reactive oxygen species due to ingestion of antioxidant supplements, health promoting effects of physical exercise are abolished, and physical exercise fails to promote insulin sensitivity and antioxidant defense in the presence of vitamin C and vitamin E.
_
Antioxidants are widely used as supplements but whether they affect the health-promoting effects of exercise is unknown. Authors evaluated the effects of a combination of vitamin C (1000 mg/day) and vitamin E (400 IU/day) on insulin sensitivity as measured by glucose infusion rates (GIR) during a hyperinsulinemic, euglycemic clamp in previously untrained (n = 19) and pretrained (n = 20) healthy young men. Before and after a 4 week intervention of physical exercise, GIR was determined, and muscle biopsies for gene expression analyses as well as plasma samples were obtained to compare changes over baseline and potential influences of vitamins on exercise effects. Exercise increased parameters of insulin sensitivity (GIR and plasma adiponectin) only in the absence of antioxidants in both previously untrained (P < 0.001) and pretrained (P < 0.001) individuals. This was paralleled by increased expression of ROS-sensitive transcriptional regulators of insulin sensitivity and ROS defense capacity, peroxisome-proliferator-activated receptor gamma (PPARγ), and PPARγ coactivators PGC1α and PGC1β only in the absence of antioxidants (P < 0.001 for all). Molecular mediators of endogenous ROS defense (superoxide dismutases 1 and 2; glutathione peroxidase) were also induced by exercise, and this effect too was blocked by antioxidant supplementation. Consistent with the concept of mitohormesis, exercise-induced oxidative stress ameliorates insulin resistance and causes an adaptive response promoting endogenous antioxidant defense capacity. Supplementation with antioxidants may preclude these health-promoting effects of exercise in humans. If transient increases in oxidative stress are capable of counteracting insulin resistance in humans, it is possible that preventing the formation of ROS by, for example, antioxidants might actually increase, rather than decrease, the risk of type 2 diabetes. All larger intervention trials evaluating the diabetes-preventive potential of defined antioxidant supplements have been unable to find any positive effects of supplementation. Moreover, antioxidant use in type 2 diabetics has been linked to increased prevalence of hypertension and use of antioxidant supplements has recently been proposed to increase overall mortality in the general population. Taken together, these previously published findings tentatively suggest that fruits and vegetables may exert health-promoting effects despite their antioxidant content and possibly due to other bio-active compounds. However, it should be noted that the current study applied comparably high doses of oral antioxidants, which have been tested in healthy young men only.
_______
_______
Exercise and genes:
The relationship between exercise and genes is bilateral:
1. Genes affect exercise behaviour:
2. Exercise affects gene’s behaviour:
_
1. Genes affecting exercise behaviour:
Evidence suggests that our genes evolved to favor exercise. In other words, during prehistoric times, if a person couldn’t move quickly and wasn’t strong, that person died. Those who were fit survived to reproduce and pass on their “fitter” genes. Some researchers believe that with our current inactive lifestyle, these genes produce a number of bad effects, which can lead to many chronic illnesses.
_
How genes and environment interact vis-à-vis exercise:
The predisposition to engage in voluntary exercise is complex and simultaneously effected by genetic architecture, the environment, and gene-environment and gene-gene interactions. Both genetic architecture and the environment are comprised of multiple components with the relative influence of each varying.
_
A number of studies of both rodents and humans have demonstrated that individual differences in both ability and propensity for exercise (i.e., voluntary exercise) have some genetic basis. It has been well established that genetics plays an important role in regulation of voluntary activity levels and ability to respond to exercise training. Empirical support is rooted in the demonstration of heritability in humans, mice, and rats utilizing several different approaches. A study of 1022 pairs of twins estimated broad-sense heritability of total physical activity to be near 50%, and heritabilities of individual components of total activity (occupational, leisure time excluding sport, sport during leisure time) ranged from 40% to 65%. Additional human studies have estimated the heritability of physical activity to be anywhere between 18% and 92%, with variable environmental contributions. Perhaps the most convincing test of whether or not a trait, such as voluntary exercise behavior, exhibits significant narrow sense heritability is its response to direct selection. An ongoing artificial selection experiment for voluntary wheel running behavior in 4 replicate lines of mice resulted in a dramatic increases in activity. By generation 16, and continuing through generation 50 and beyond, the high-running (HR) lines had diverged significantly from the control lines with an approximate 3-fold increase in running on days 5 and 6 of a 6 day test. Narrow-sense heritability, representing the additive genetic component of phenotypic variation, was calculated to be 0.28. Given that exercise propensity has a heritable component and is an important component of positive health-related outcomes, investigations into the location or identity of specific genetic markers linked to exercise are becoming increasingly common.
_
2. Exercise affecting gene’s behaviour:
Epigenetic regulation on gene expression induced by physical exercise:
It is well established that physical exercise modulates the function of many physiological systems, such as the musculoskeletal, the cardiovascular and the nervous system, by inducing various adaptations to the increased mechanical load and/or metabolic stress of exercise. Many of these changes occur through epigenetic alterations to DNA, such as histone modifications, DNA methylations, expression of microRNAs and changes of the chromatin structure. All these epigenetic alterations may have clinical relevance, thus playing an important role in the prevention and confrontation of neurophysiological disorders, metabolic syndrome, cardiovascular diseases and cancer.
_
These epigenetic modifications are crucial for the activation of signalling cascades associated with genes that regulate metabolism and energy consumption in skeletal muscle. They also regulate numerous molecular pathways related to inflammatory processes. Moreover, some epigenetic modifications that possibly occur due to physical exercise can have a positive effect on restoring the genomic stability in cells with carcinogenesis potential, as well as on partially restoring age deregulated epigenetic patterns. Further insight into the epigenetic mechanisms involved in the aging process and their regulation by physical exercise might reveal ways in which exercise could be used as a preventive and/or complementary therapeutic strategy against age-related diseases. Furthermore, epigenetic alterations have a significant effect on the limbic system and especially on hippocampus, while the cardiovascular system is also affected by epigenetic changes caused by exercise, however, the evidence available for a clear association between them is not robust. It is suggested that exercise-related epigenetic changes could have an important role in preventing and/or confronting various disorders, such as metabolic or neurodegenerative diseases, that are either directly or indirectly associated with deregulation of normal epigenetic procedures and affect many people worldwide. Prof. Charlotte Ling and colleagues found that exercise brought about changes in 7,000 of the participants’ genes, i.e. 35% of their whole genetic makeup. They also noticed that fundamental genetic changes occurred which play a role in preventing obesity and type 2 diabetes. A profound understanding of human epigenetic procedures during physical exercise could explain, in a more global and integrated approach, the possible cross talking between cascades which are involved in the regulation of human physiological systems. In this context, exercise remains an essential factor for promoting important biological adaptations that have profound implications for public health.
______
______
Exercise and evolution:
Our ancestors were physically active not because they enjoyed exercise but because they needed to exercise. Early humans’ lifestyle demanded engagement in many energy-burning behaviors. The style of hunt-gathering life was composed of numerous physical activities (running to capture wounded prey, transporting children, building shelters) and social activities (visits to neighboring camps, dances as part of religious ceremonies or for recreation). As a response to this active lifestyle, an increase in aerobic and physical capacity allowed access to new food resources, influencing the development of brain components and consequently cognitive improvement in human. Bramble and Lieberman (2004) argue that our genus, Homo, evolved from more ape-like human ancestors, Australopithecus, 2 million or more years ago because natural selection favored the survival of australopithecines that could run and, over time, favored the perpetuation of human anatomical features that made long-distance running possible. Primate species with short toes are possibly best runners than those with longer toes, indicating an evolutionary adaptation to humans as good runners (Rolian et al., 2009). Another study shows that the gluteus maximus, muscle is also an adaptation to long-distance running, together with long legs and big buttocks in comparison with other primates. The reorganization of leg muscle anatomy in response to selective pressures on the environment over time was important to human pelvis development and bipedalism in order to increase the payoffs of foraging (Lieberman et al., 2006). Other researchers disagree with the notion that evolutionary selection pressure make us do exercise. According to them, there was never any evolutionary selection pressure to make us like exercise. Neanderthal or Homo erectus had to go long distances every day in order to survive. Not exercising was never an option, so there was never any selection pressure to make people like exercise. On the contrary, there was probably selection to help people avoid needless exercise when they could. Some hunter-gatherers had diets of about 2,200 calories a day. When your energy intake is that low, you can’t afford to go for a jog just for fun. According to them, evolution selected for traits that made us do no exercise and relax. When you walk into a train station and there is a staircase and an escalator, your brain always tells you to take the escalator. It’s not in your best interest, but it’s probably a very deeply rooted evolutionary instinct. Nowadays due to lack of daily physical activity and overeating, this trait has become maladaptive. That is why we have to make conscious effort to exercise through some form of socially acceptable coercion.
_
Exercise and evolution of brain:
The human brain is approximately three times larger than expected for our body size, due to increases in several brain components, including the frontal lobe, temporal lobe and cerebellum. This major increase in both absolute brain size and brain size relative to body mass occurred during the early evolution of the genus Homo, becoming especially pronounced during the evolution of Homo erectus. Because brain size changes in human evolution are often interpreted in the context of cognition, previous hypotheses for increased brain size in hominins have focused on greater social complexity or enhanced ecological demands on cognition. However, at the same time as brain size began to increase in the human lineage, aerobic activity levels appear to have changed dramatically. The hunting and gathering lifestyle adopted by human ancestors around 2 million years ago required a large increase in aerobic activity. High levels of physical activity altered the shape of the human body, enabling access to new food resources (e.g. animal protein) in a changing environment. Recent experimental work provides strong evidence that both acute bouts of exercise and long-term exercise training increase the size of brain components and improve cognitive performance in humans and other taxa. However, to date, researchers have not explored the possibility that the increases in aerobic capacity and physical activity that occurred during human evolution directly influenced the human brain. Researchers hypothesize that proximate mechanisms linking physical activity and neurobiology in living species may help to explain changes in brain size and cognitive function during human evolution. They review evidence that selection acting on endurance increased baseline neurotrophin and growth factor signalling (compounds responsible for both brain growth and for metabolic regulation during exercise) in some mammals, which in turn led to increased overall brain growth and development. This hypothesis suggests that a significant portion of human neurobiology evolved due to selection acting on features unrelated to cognitive performance.
________
_______
Exercise and health:
Health effects and benefits of exercise:
The landmark work by Morris and co-workers changed modern views of the relationship between physical activity, fitness, and health and inspired a new era in which the association between physical activity and human health, disease, and mortality was scrutinized scientifically. For more than half a century, a plethora of evidence has accumulated from large, long-term epidemiological studies that support a strong, inverse, and independent association between physical activity, health, and cardiovascular and overall mortality in apparently healthy individuals, and in patients with documented cardiovascular disease. The exercise-related health benefits are related in part to favorable modulations in both the traditional and novel cardiovascular risk factors that have been observed with increased physical activity patterns or structured exercise programs. The evidence for the health benefits of physical activity in adults is overwhelming. Being physically active plays an essential role in ensuring health and well-being, and there is a large body of research investigating the benefits of exercise. Physical activity benefits many parts of the body – the heart, skeletal muscles, bones, blood (for example, cholesterol levels), the immune system and the nervous system – and can reduce many of the risk factors for non –communicable diseases NCDs. Regular physical activity reduces the risk of chronic diseases such as coronary artery disease, diabetes, and obesity. Regular physical activity also helps improve mental health, and there might be a dose-response relationship between mental health and the level and intensity of activity.
_
Health benefits of exercise are divided in two groups:
Physical health benefits
Mental health benefits
_
Physical Health Benefits of Exercise:
1. Weight loss and weight control
2. Increased muscle strength and muscle mass (which helps burn calories and fat)
3. Increased energy
4. Improved flexibility and movement
5. Lower risk of some types of cancer (Exercising at least 4 hours per week has been shown to lower risk of breast cancer by 37%!)
6. Reduced risk of Diabetes 2 and metabolic syndrome
7. Improved immune system, for overall better health
8. Increased “good” cholesterol to keep blood flowing smoothly
9. Lower risk of a heart attack and stroke
10. Helps smokers quit with higher success rates
11. Strength training & weight-bearing exercise (like walking, jogging, etc), promotes stronger bones (which is particularly helpful for women entering menopause, when bone density is lost)
12. In short, Exercise can increase your life expectancy by an average of 7 years! (One study in New England Journal of Medicine showed that asymptomatic women who weren’t fit had twice the risk of death than those who were fit!)
_
Mental Health Benefits of Exercise:
Countless research studies show that exercise has incredible benefits not just for physical health, but for all areas of health, including mental, emotional, intellectual, and yes, even social well-being.
1. Regular aerobic exercise increases levels of seratonin and dopamine in the brain, which is linked with improved mood
2. Aerobic exercise increases endorphins in the brain, improving mood and energy
3. Exercise enhances the mind’s ability to withstand daily hassles and stressors and to regulate itself
4. Research shows exercise can alleviate symptoms of Pre-Menstrual Syndrome and Depression in women
5. Regular exercise has been shown equal to antidepressant use in treating Major Depressive Disorder
6. Exercise is associated with deeper relaxation and better quality of sleep (which protects the brain and increases energy)
7. Strength training has been shown to decrease tension and worry in the body and mind
8. Studies show exercise reduces/treats and may prevent anxiety and panic attacks
9. Exercise increases mental clarity and efficiency
10. Improves cognitive functioning in middle age and beyond
11. Exercise is associated with better thinking, learning, and judgment
12. It can help you tap into intuition and creativity
13. Exercise increases assertiveness and enthusiasm for life
14. Group or partner exercise increases social activity and decreases feelings of loneliness and isolation
15. Those who exercise regularly tend to have a better body-image
16. Regular exercise is associated with higher self-esteem
17. Overall, exercise is one of the best ways to improve happiness and life satisfaction
_____
Evidence for Health Benefits associated with Regular Physical Activity:
Children and Adolescents:
Strong evidence-
•Improved cardiorespiratory and muscular fitness
•Improved bone health
•Improved cardiovascular and metabolic health biomarkers
•Favorable body composition
Moderate evidence-
•Reduced symptoms of depression
Adults and Older Adults:
Strong evidence-
•Lower risk of early death
•Lower risk of coronary heart disease
•Lower risk of stroke
•Lower risk of high blood pressure
•Lower risk of adverse blood lipid profile
•Lower risk of type 2 diabetes
•Lower risk of metabolic syndrome
•Lower risk of colon cancer
•Lower risk of breast cancer
•Prevention of weight gain
•Weight loss, particularly when combined with reduced calorie intake
•Improved cardiorespiratory and muscular fitness
•Prevention of falls
•Reduced depression
•Better cognitive function (for older adults)
Moderate to strong evidence-
•Better functional health (for older adults)
•Reduced abdominal obesity
Moderate evidence-
•Lower risk of hip fracture
•Lower risk of lung cancer
•Lower risk of endometrial cancer
•Weight maintenance after weight loss
•Increased bone density
•Improved sleep quality
Note: The evidence of health benefits of physical activity are rated as strong, moderate, or weak. To do so, the number, and quality of studies available are considered, as well as consistency of findings across studies that addressed each outcome.
_____
There is incontrovertible evidence that regular physical activity contributes to the primary and secondary prevention of several chronic diseases and is associated with a reduced risk of premature death. There appears to be a graded linear relation between the volume of physical activity and health status, such that the most physically active people are at the lowest risk. However, the greatest improvements in health status are seen when people who are least fit become physically active. Physical exercise is important for maintaining physical fitness and can contribute positively to maintaining a healthy weight, building and maintaining healthy bone density, muscle strength, and joint mobility, promoting physiological well-being, reducing surgical risks, and strengthening the immune system. Developing research has demonstrated that many of the benefits of exercise are mediated through the role of skeletal muscle as an endocrine organ. That is, contracting muscles release multiple substances known as myokines which promote the growth of new tissue, tissue repair, and multiple anti-inflammatory functions, which in turn reduce the risk of developing various inflammatory diseases. Exercise reduces levels of cortisol which causes many health problems, both physical and mental. Conversely, exercise increases levels of saliva nitrite, which can be converted to the nitric oxide, thereby, increasing intensity and training load. Saliva testing for nitric oxide serves as a marker for training status. Endurance exercise before meals lowers blood glucose more than the same exercise after meals. According to the World Health Organization, lack of physical activity contributes to approximately 17% of heart disease and diabetes, 12% of falls in the elderly, and 10% of breast cancer and colon cancer. There is evidence that vigorous exercise (60–85% of VO2 Max) induces a greater degree of physiological cardiac hypertrophy than moderate exercise (40 to 60% of VO2 Max), but it is unknown whether this has any effects on overall morbidity and/or mortality. Both aerobic and anaerobic exercise work to increase the mechanical efficiency of the heart by increasing cardiac volume (aerobic exercise), or myocardial thickness (strength training). Ventricular hypertrophy, the thickening of the ventricular walls, is generally beneficial and healthy if it occurs in response to exercise. Not everyone benefits equally from exercise. There is tremendous variation in individual response to training; where most people will see a moderate increase in endurance from aerobic exercise, some individuals will as much as double their oxygen uptake, while others can never augment endurance. However, muscle hypertrophy from resistance training is primarily determined by diet and testosterone. This genetic variation in improvement from training is one of the key physiological differences between elite athletes and the larger population. Studies have shown that exercising in middle age leads to better physical ability later in life.
______
Exercise and mortality:
_
_
Physical inactivity has been identified as the fourth leading risk factor for global mortality (6% of deaths globally). This follows high blood pressure (13%), tobacco use (9%) and high blood glucose (6%). Overweight and obesity are responsible for 5% of global mortality. Levels of physical inactivity are rising in many countries with major implications for the general health of people worldwide and for the prevalence of NCDs such as cardiovascular disease, diabetes and cancer and their risk factors such as raised blood pressure, raised blood sugar and overweight. Physical inactivity is estimated as being the principal cause for approximately 21–25% of breast and colon cancer burden, 27% of diabetes and approximately 30% of ischaemic heart disease burden. In addition, NCDs now account for nearly half of the overall global burden of disease. It is estimated currently that of every 10 deaths, 6 are attributable to noncommunicable conditions.
_
_
Because of the many benefits for health of physical activity, recent analysis has suggested that reaching the recommended minimum level of physical activity compared with no activity was found to lead to a reduction in all-cause mortality of 19 per cent – and this rises to 24 per cent if an hour a day is spent in physical activity. In addition, there is a 31 per cent lower risk for all-cause mortality in active individuals. This demonstrates a positive dose-response – in other words, that the benefits of physical activity increase as the amount and intensity of the activity increases. Guidelines on physical activity and health from major health organizations have generally recommended exercise intensities in the range of 3 to 6 METs and an overall energy expenditure of at least 1000 kcal/wk (the equivalent of walking for roughly 30 minutes per day). This is based on a 20% to 40% reduction in mortality associated with increased physical activity patterns among middle-aged subjects followed for periods ranging between 5 and 15 years. Similar to fitness levels, health outcome benefits from physical activity appear to be most dramatic at the lowest end of the activity spectrum and reach a plateau among the most highly active individuals (>3500 kcal/wk).
_
The figure below shows exercise reduced relative risk of death:
_
NIH study finds leisure-time physical activity extends life expectancy as much as 4.5 years:
Leisure-time physical activity is associated with longer life expectancy, even at relatively low levels of activity and regardless of body weight, according to a study by a team of researchers led by the National Cancer Institute (NCI), part of the National Institutes of Health. The study, which found that people who engaged in leisure-time physical activity had life expectancy gains of as much as 4.5 years. In order to determine the number of years of life gained from leisure-time physical activity in adulthood, which translates directly to an increase in life expectancy, researchers examined data on more than 650,000 adults. These people, mostly age 40 and older, took part in one of six population-based studies that were designed to evaluate various aspects of cancer risk. The researchers also examined how life expectancy changed with the combination of both activity and obesity. Obesity was associated with a shorter life expectancy, but physical activity helped to mitigate some of the harm. People who were obese and inactive had a life expectancy that was between five to seven years shorter (depending on their level of obesity) than people who were normal weight and moderately active. According to data, a middle-aged person who gets the recommended 150 minutes per week of moderate exercise — defined as the level of brisk walking — can expect a 1-to-7 return: seven extra minutes of life gained for each minute spent exercising.
_
Another study shows that life expectancy gains from physical activity:
_
Elderly people who exercise ‘live five years longer’: 2015:
Regular exercise in old age has as powerful an effect on life expectancy as giving up smoking, researchers say. The analysis of 5,700 elderly men in Norway showed those doing three hours of exercise a week lived around five years longer than the sedentary. The authors, writing in the British Journal of Sports Medicine, called for campaigns to encourage fitness in older people.
_
MZ twin-activity comparisons show high mortality component:
Table below is presented to show the mortality outcome in MZ twins discordant for physical activity in a large cohort of Swedish twins. The higher physically active MZ had a 36%–66% lower mortality than their inactive MZ pair.
_
Tendency for dose-response between higher physical activity level and lower mortality in Swedish monozygotic twins:
| Sex | Physical activity level | All-cause mortality | Cardiovascular mortality | ||
| Hazard ratio | 95% confidence intervals | Hazard ratio | 95% confidence intervals | ||
| Men | Low | 1 | 1 | ||
| Moderate | 0.84 | 0.72, 0.98 | 0.86 | 0.68, 1.08 | |
| High | 0.64 | 0.50, 0.83 | 0.55 | 0.36, 085 | |
| Women | Low | 1 | 1 | ||
| Moderate | 0.82 | 0.70, 0.96 | 0.85 | 0.64, 1.13 | |
| High | 0.75 | 0.50, 1.14 | 0.34 | 0.1,0.95 | |
________
Various studies and reviews regarding impact of exercise on health:
In many studies covering a wide range of issues, researchers have focused on exercise, as well as on the more broadly defined concept of physical activity. Exercise is a form of physical activity that is planned, structured, repetitive, and performed with the goal of improving health or fitness. So, although all exercise is physical activity, not all physical activity is exercise. Studies have examined the role of physical activity in many groups—men and women, children, teens, adults, older adults, people with disabilities, and women during pregnancy and the postpartum period. These studies have focused on the role that physical activity plays in many health outcomes, including:
•Premature (early) death;
•Diseases such as coronary heart disease, stroke, some cancers, type 2 diabetes, osteoporosis, and depression;
•Risk factors for disease, such as high blood pressure and high blood cholesterol;
•Physical fitness, such as aerobic capacity, and muscle strength and endurance
•Functional capacity (the ability to engage in activities needed for daily living);
•Mental health, such as depression and cognitive function; and
•Injuries or sudden heart attacks.
These studies have also prompted questions as to what type and how much physical activity is needed for various health benefits.
_
Major Research Findings of various studies on the health benefits of Physical Activity:
•Regular physical activity reduces the risk of many adverse health outcomes.
•Some physical activity is better than none.
•For most health outcomes, additional benefits occur as the amount of physical activity increases through higher intensity, greater frequency, and/or longer duration.
•Most health benefits occur with at least 150 minutes a week of moderate-intensity physical activity, such as brisk walking. Additional benefits occur with more physical activity.
•Both aerobic (endurance) and muscle-strengthening (resistance) physical activity are beneficial.
•Health benefits occur for children and adolescents, young and middle-aged adults, older adults, and those in every studied racial and ethnic group.
•The health benefits of physical activity occur for people with disabilities.
•The benefits of physical activity far outweigh the possibility of adverse outcomes.
_
Overview of Evidence for improvement in health due to exercise:
| Condition | Evidence for improvement, and scale of improvement with physical activity |
| Short term improvements | Many papers report global improvements in health across a range of conditions. Physical activity helps to manage over 20 chronic conditions, including coronary heart disease, stroke, type 2 diabetes, cancer, obesity, mental health problems and musculoskeletal conditions. |
| COPD | Physical activity improves cardiorespiratory health. Furthermore, in COPD, exercise training reduces dyspnoea symptoms and increases ability for exertion. |
| Heart disease and/ or Heart failure and/or Angina | All studies show clear improvements in cardiovascular health with moderate exercise. There are similar beneficial effects for sufferers of angina. Overall, exercise reduces cardiac mortality by 31%. |
| Hypertension (high blood pressure) | Hypertension is very common with 30% of adults having this diagnosis. Hypertension is responsible for 50% of strokes and 50% of Ischaemic heart disease. Most people with hypertension are on long-term medication. Randomised controlled trials show a clear lowering of blood pressure with aerobic training. The scale of the reduction has been quantified: 31% of patients on average experience a drop of at least 10 mmHg with regular physical activity. |
| Cholesterol | Across several studies, exercise led to a reduction in LDL by an average of 1 to 2mmol/l and an increase in “good” High Density Lipoprotein (HDL). |
| Obesity | Exercise only has a moderate effect in reducing obesity. Aerobic physical activity has a consistent effect on achieving weight maintenance. Exercise also changes the distribution of fat, by reducing the less healthy visceral [abdominal] fat – for some individuals the body weight may stay the same as muscle is built up but the reduction in visceral fat is highly beneficial for health. |
| Depression | There has been a wealth of evidence on the effect of exercise in the treatment of depression, most showing positive outcome. An updated Cochrane review evaluated 30 trials of physical activity as a treatment for depression, showing overall ‘moderate’ improvement. |
| Peripheral vascular disease | Exercise leads to a moderate improvement in peripheral vascular disease. Improvements are seen in both pain-free walking time and distance in several studies. |
| Diabetes | Exercise has a statistically and clinically significant beneficial effect on glycemic control and the metabolic state. Exercise works as a treatment modality in both type 1 and type 2 diabetes. |
| Osteoarthritis Joints / Low back pain / osteoporosis | Osteoarthritis is sometimes thought to be related to “wear and tear” yet physical activity improves symptoms of osteoarthritis by 22-83% and does not lead to worsening of this condition. It has benefits in reducing pain (by 25-52%), improving function, improving quality of life and mental health. Others have commented on exercise being weakly effective in osteoarthritis and leading to moderate improvement in low back pain. Exercise increases muscle strength and coordination. |
| Chronic pain | Exercise leads to improvement in pain conditions by 25 -52%. |
| Fibromyalgia and fatigue | Aerobic exercise improves physical function and well-being in fibromyalgia. It can also reduce the symptom of fatigue seen in different conditions. |
| Cancer | There are few studies looking at exercise as a treatment for cancer, and effects would be expected to vary by type of cancer. In prostate cancer, a 57% lower rate of cancer progression was found with exercise. Exercise helps with side-effects of treatment, improves mood, fatigue and stamina and probably prolongs life. |
| Dementia | Physical exercise improves cognitive function and consistently reverses brain atrophy. A significant relationship between physical activity training and improved cognition was obtained for both normal adults and patients with early signs of Alzheimer’s disease, in which memory or cognitive ability was mildly impaired. Some studies lament the paucity of case-control studies for exercise in people with established dementia, but all show “strong indications of benefits” in well-being, quality of life, improved balance and strength with reduced falls and more prolonged independence. |
It should be noted that these effects occur at low levels of activity – 30 minutes, 5 times per week. The largest health gains occur in people moving from inactive to moderately inactive and from moderately inactive to moderately active. The effects work by different mechanisms. In patients with multiple co-morbidities, physical activity can improve several conditions in different ways. The benefits of physical activity work independently from those of weight change. Increasing ‘fitness’ works in a different way to reducing ‘fatness’ so even people who are overweight can improve their metabolic health by exercising, even if they don’t necessarily lose weight.
_
Classification of physical activities vis-à-vis health benefits:
As you can see in the table above, substantial health benefits are rendered if medium level of physical activity is performed i.e. 150 to 300 minutes of moderate intensity exercise per week.
_
Long-term health benefits of physical activity – a systematic review of longitudinal studies: 2013:
The purpose of this review is to summarize existing evidence for the long-term (>5 years) relationship between physical activity and weight gain, obesity, coronary heart disease, type 2 diabetes mellitus, Alzheimer’s disease and dementia. Fifteen longitudinal studies with at least 5-year follow up times and a total of 288,724 subjects (>500 participants in each study), aged between 18 and 85 years, were identified using digital databases. Only studies published in English, about healthy adults at baseline, intentional physical activity and the listed NCDs were included. The results of these studies show that physical activity appears to have a positive long-term influence on all selected diseases.
_
Intensity vs. duration of exercise:
The independent effects of exercise type, volume, and intensity on the risk for coronary heart disease (CHD) have been assessed in a large cohort of men (n=44 452) enrolled in the Health Professionals’ Follow-up Study. Walking pace (intensity) and exercise duration were both inversely related to the risk of CHD independent of walking volume. However, the much stronger association between exercise intensity and risk suggests that exercise intensity has a more significant effect on the incidence of CHD than duration. This was also the first study to provide evidence for the efficacy of resistance training on CHD risk. The reduction in CHD risk achieved by participation in resistance training was similar to that provided by brisk walking and rowing but was approximately half of that provided by running. Similarly, in the Women’s Health Study, exercise intensity (walking pace) and duration of walking were both inversely and independently related to the risk of coronary events. Women who walked 1 to 3 hours per week had between 30% and 50% reductions in CHD events compared with women who did no walking. However, for the same exercise volume achieved by either higher exercise intensity or longer duration, the risk reduction was substantially greater for exercise duration. In contrast to the findings reported in the Health Professionals’ Follow-up Study of men, this suggests that exercise duration is more effective in lowering the risk for coronary events than exercise intensity. However, the inextricable complexity of the interactions between gender, exercise intensity, duration, and frequency cannot be resolved by epidemiological studies. Most importantly, and despite possible differences attributable to gender and exercise stimulus, the salient finding of these and other reports is that moderate activity such as walking has a considerable impact on CHD events, and walking or similar activities a few hours per week should be recommended to all adults, as suggested in various guidelines.
________
Exercise and diseases:
Regular physical activity using large muscle groups, such as walking, running, or swimming, produces cardiovascular adaptations that increase exercise capacity, endurance, and skeletal muscle strength. Habitual physical activity also prevents the development of coronary artery disease (CAD) and reduces symptoms in patients with established cardiovascular disease. There is also evidence that exercise reduces the risk of other chronic diseases, including type 2 diabetes, osteoporosis, obesity, depression, and cancer of the breast and colon. This American Heart Association (AHA) Scientific Statement for health professionals summarizes the evidence for the benefits of physical activity in the prevention and treatment of cardiovascular disease, provides suggestions to healthcare professionals for implementing physical activity programs for their patients, and identifies areas for future investigation. This statement focuses on aerobic physical activity and does not directly evaluate resistance exercises, such as weight lifting, because most of the research linking physical activity and cardiovascular disease has evaluated aerobic activity. Whenever possible, the writing group has cited summary articles or meta-analyses to support conclusions and recommendations. This evidence supports the recommendation from the Center for Disease Control and Prevention (CDC) and the American College of Sports Medicine (ACSM) that individuals should engage in 30 minutes or more of moderate-intensity physical activity on most (preferably all) days of the week.
_
Benefits of Exercise:
Almost all patients benefit from physical activity, but some require risk stratification. Increasing physical activity is effective in the treatment and prevention of chronic disease and improving overall health and well -being.
Research has found that people who do regular physical activity have:
•up to a 35% lower risk of coronary heart disease and stroke
•up to a 50% lower risk of type 2 diabetes
•up to a 50% lower risk of colon cancer
•up to a 20% lower risk of breast cancer
•a 30% lower risk of early death
•up to an 83% lower risk of osteoarthritis
•up to a 68% lower risk of hip fracture
•a 30% lower risk of falls (among older adults)
•up to a 30% lower risk of depression
•up to a 30% lower risk of dementia
•up to a 50 % lower risk of high blood pressure
_______
How does physical activity and fitness lead to improved health outcomes?
Several biological mechanisms may be responsible for the reduction in the risk of chronic disease and premature death associated with routine physical activity. For instance, routine physical activity has been shown to improve body composition (e.g., through reduced abdominal adiposity and improved weight control), enhance lipid lipoprotein profiles (e.g., through reduced triglyceride levels, increased high-density lipoprotein [HDL] cholesterol levels and decreased low-density lipoprotein [LDL]-to-HDL ratios), improve glucose homeostasis and insulin sensitivity, reduce blood pressure, improve autonomic tone, reduce systemic inflammation; decrease blood coagulation, improve coronary blood flow, augment cardiac function and enhance endothelial function. Chronic inflammation, as indicated by elevated circulating levels of inflammatory mediators such as C-reactive protein, has been shown to be strongly associated with most of the chronic diseases whose prevention has benefited from exercise. Recent RCTs have shown that exercise training may cause marked reductions in C-reactive protein levels. Each of these factors may explain directly or indirectly the reduced incidence of chronic disease and premature death among people who engage in routine physical activity.
_
Now let me discuss some important diseases vis-à-vis exercise:
______
Cancer:
Exercise improves quality of life in cancer patients as seen in the figure below:
_
The graphic below from the American Institute for Cancer Research visually depicts the importance of both daily physical activity and structured exercise (in relation to cancer indicators). Here, the green reflects structured exercise, while the yellow reflects daily physical activity.
This shows that even though structured moderate exercise volume remains same, reduced daily physical activity increases cancer risk.
_
A systematic review evaluated 45 studies that examined the relationship between physical activity and cancer survivorship. According to the study results “There was consistent evidence from 27 observational studies that physical activity is associated with reduced all-cause, breast cancer–specific, and colon cancer–specific mortality”.
_
Cancer cachexia:
Physical exercise is becoming a widely accepted non-pharmacological intervention for the prevention and attenuation of cancer cachexia. Cachexia is a multiorganic syndrome associated with cancer, characterized by inflammation, body weight loss (at least 5%) and muscle and adipose tissue wasting. The exercise-induced transcription coactivator peroxisome proliferator-activated receptor-γ coactivator 1α (PGC1α), which suppresses FOXO and NF-κB dependent transcription during atrophy induced by fasting or denervation, may be a key intermediate responsible for the beneficial antiatrophic effects of physical exercise on cancer cachexia. The exercise-induced isoform PGC1α4, which can repress myostatin and induce IGF1 and hypertrophy, is a potential drug target for treatment of cancer cachexia. Other factors, such as JUNB and SIRT1, that maintain skeletal muscle mass and promote hypertrophy are also induced with regular physical exercise.
_
How might physical activity affect cancer survivorship?
Research indicates that physical activity after a diagnosis of breast cancer may be beneficial in improving quality of life, reducing fatigue, and assisting with energy balance. Both reduced physical activity and the side effects of treatment have been linked to weight gain after a breast cancer diagnosis. One study found that women who exercised moderately (the equivalent of walking 3 to 5 hours per week at an average pace) after a diagnosis of breast cancer had improved survival rates compared with more sedentary women. The benefit was particularly pronounced in women with hormone responsive tumors. Another study found that a home-based physical activity program had a beneficial effect on the fitness and psychological well-being of previously sedentary women who had completed treatment for early-stage through stage II breast cancer. Increasing physical activity may influence insulin and leptin levels and influence breast cancer prognosis. Although there are several promising studies, it is too early to draw any strong conclusions regarding physical activity and breast cancer survival.
_
_
Two additional studies have suggested a protective association of physical activity after colon cancer diagnosis and survival. Researchers examined the relationship between levels of physical activity both before and after a diagnosis of colon cancer in two different observational studies. Whereas levels of pre-diagnosis physical activity were not related to survival, participants with higher levels of physical activity post-diagnosis were less likely to have a cancer recurrence and had increased survival. Although these studies suggest protective effects of physical activity, more research is needed to understand what levels of physical activity provide these benefits.
_______
Cardiovascular system:
The beneficial effect of exercise on the cardiovascular system is well documented. There is a direct relation between physical inactivity and cardiovascular mortality, and physical inactivity is an independent risk factor for the development of coronary artery disease. There is a dose-response relation between the amount of exercise performed from approximately 700 to 2000 kcal of energy expenditure per week and all-cause mortality and cardiovascular disease mortality in middle-aged and elderly populations. The greatest potential for reduced mortality is in the sedentary who become moderately active. Most beneficial effects of physical activity on cardiovascular disease mortality can be attained through moderate-intensity activity (40% to 60% of maximal oxygen uptake, depending on age). Persons who modify their behavior after myocardial infarction to include regular exercise have improved rates of survival. … Persons who remain sedentary have the highest risk for all-cause and cardiovascular disease mortality.
_
A sedentary lifestyle is one of the major risk factors for cardiovascular disease, as outlined by the AHA. Evidence from many scientific studies shows that reducing this risk factors decreases the chance of having a heart attack or experiencing another cardiac event, such as a stroke, and reduces the possibility of needing a coronary revascularization procedure (bypass surgery or coronary angioplasty). Regular exercise has a favorable effect on many of the established risk factors for cardiovascular disease. For example, exercise promotes weight reduction and can help reduce blood pressure. Exercise can reduce “bad” cholesterol levels in the blood (the low-density lipoprotein [LDL] level), as well as total cholesterol, and can raise the “good” cholesterol (the high-density lipoprotein level [HDL]). In diabetic patients, regular activity favorably affects the body’s ability to use insulin to control glucose levels in the blood. Although the effect of an exercise program on any single risk factor may generally be small, the effect of continued, moderate exercise on overall cardiovascular risk, when combined with other lifestyle modifications (such as proper nutrition, smoking cessation, and medication use), can be dramatic.
_
How much Exercise does it take to lower Cholesterol?
Exactly how much exercise is needed to lower cholesterol has been a matter of some debate. In general, most public health organizations recommend, at a minimum, 30 minutes per day of moderate to vigorous exercise, such as walking, jogging, biking, or gardening. But a 2002 study by researchers at Duke University Medical Center found that more intense exercise is actually better than moderate exercise for lowering cholesterol. In a study of overweight, sedentary people who did not change their diet, the researchers found that those who got moderate exercise (the equivalent of 12 miles of walking or jogging per week) did lower their LDL level somewhat. But the people who did more vigorous exercise (the equivalent of 20 miles of jogging a week) lowered it even more. The people who exercised vigorously also raised their levels of high-density lipoprotein (HDL) — the “good” kind of lipoprotein. According to Kraus’s findings, however, even though moderate exercise was not as effective in reducing LDL or increasing HDL, it did keep cholesterol levels from rising. The exercise volume for achieving significant HDL cholesterol changes is estimated at ≈1000 to 1500 kcal/wk. This parallels an earlier study in which a mean estimated weekly energy expenditure of 1245 kcal for individuals running ≈7 to 10 miles per week (average, 9 miles) and 1688 kcal for those running 11 to 14 miles per week (average, 12 miles) resulted in 7% and 11% increases in HDL cholesterol concentrations, respectively. Others have reported similar changes in HDL cholesterol among individuals running similar weekly distances for ≈9 to 12 months. It is likely that other modes of physical activity will invoke similar increases in HDL cholesterol concentrations as long as they meet or exceed the caloric expenditure of 1200 to 1600 kcal.
_
Epidemiological evidence of exercise benefits:
Studies have linked sedentary living with high rates of coronary heart disease mortality. One study found that San Francisco longshoremen who worked in jobs requiring high levels of energy expenditure had less risk of dying of heart disease than did longshoremen who performed sedentary jobs. This study showed that dockworkers and cargo handlers expended at least 1,000 kilocalories more per day than did clerks and foremen and that sedentary workers, during a 22-year observation, were about twice as likely to die from heart disease. The higher risk of death in the less active men was not due to other coronary heart disease risk factors, such as smoking, obesity, and high blood pressure; nor was it the result of less healthy men’s shifting to sedentary jobs. Another study followed the health status of approximately 17,000 male graduates of Harvard University for many years. All these men essentially had sedentary jobs, but they differed in the amount of leisure time they spent on physical activities. Men who expended at least 2,000 kilocalories per week on physical activity had only half the death rate from heart disease as did those men who expended less than 500 kilocalories per week. Not all of this energy was spent in exercise programs; some was expended during routine activities such as climbing stairs.
_
Primary prevention of cardiovascular disease:
Since the seminal work of Morris and colleagues in the 1950s and the early work of Paffenbarger and colleagues in the 1970s, there have been numerous long-term prospective follow-up studies (mainly involving men but more recently women also) that have assessed the relative risk of death from any cause and from specific diseases (e.g., cardiovascular disease) associated with physical inactivity. Both men and women who reported increased levels of physical activity and fitness were found to have reductions in relative risk (by about 20%–35%) of death. For example, in a study involving healthy middle-aged men and women followed up for 8 years, the lowest quintiles of physical fitness, as measured on an exercise treadmill, were associated with an increased risk of death from any cause compared with the top quintile for fitness. Recent investigations have revealed even greater reductions in the risk of death from any cause and from cardiovascular disease. For instance, being fit or active was associated with a greater than 50% reduction in risk. Furthermore, an increase in energy expenditure from physical activity of 1000 kcal (4200 kJ) per week or an increase in physical fitness of 1 MET (metabolic equivalent) was associated with a mortality benefit of about 20%. Physically inactive middle-aged women (engaging in less than 1 hour of exercise per week) experienced a 52% increase in all-cause mortality, a doubling of cardiovascular-related mortality and a 29% increase in cancer-related mortality compared with physically active women. These relative risks are similar to those for hypertension, hypercholesterolemia and obesity, and they approach those associated with moderate cigarette smoking. Moreover, it appears that people who are fit yet have other risk factors for cardiovascular disease may be at lower risk of premature death than people who are sedentary with no risk factors for cardiovascular disease. An increase in physical fitness will reduce the risk of premature death, and a decrease in physical fitness will increase the risk. The effect appears to be graded, such that even small improvements in physical fitness are associated with a significant reduction in risk. A recent systematic review of the literature regarding primary prevention in women revealed that there was a graded inverse relation between physical activity and the risk of cardiovascular-related death, with the most active women having a relative risk of 0.67 (95% CI 0.52 to 0.85) compared with the least active group. These protective effects were seen with as little as 1 hour of walking per week. In summary, observational studies provide compelling evidence that regular physical activity and a high fitness level are associated with a reduced risk of premature death from any cause and from cardiovascular disease in particular among asymptomatic men and women. Furthermore, a dose– response relation appears to exist, such that people who have the highest levels of physical activity and fitness are at lowest risk of premature death.
__
30 minute of Exercise per day not enough to prevent Heart failure: a 2015 study:
In the latest study, Jarett Berry, associate professor of medicine and clinical sciences at University of Texas Southwestern Medical Center, and his colleagues studied how exercise can affect risk of heart failure. They report in the journal Circulation on how much physical activity is needed to effectively lower risk of the condition. Berry and his team analyzed responses from 12 large studies involving 370,460 people who were asked about their exercise habits and followed on average for 13 years. Berry found that those who were the most physically active showed a 30% lower risk of having heart failure than those who exercise the least. These people got more activity than what the government currently recommends, which is 150 minutes of moderate physical activity each week. The people who exercise that much also lowered their risk of heart failure, but not by as much: a 15% to 22% drop. In fact, people who doubled the recommended level of activity lowered their risk of heart failure by 19% while those who quadrupled the amount of exercise reduced their risk by 35%. So higher dose of exercise is not a waste of time in preventing heart failure. Berry stresses that while the people who exercised more clearly derived more benefit from the activity, any amount of exercise is still helpful. Compared to people who were not active at all, those who followed the recommended 150 minutes of activity a week lowered their risk of heart failure by 10%. The findings do suggest, however, that exercise advice to lower heart failure may be different from recommendations for reducing heart attacks and stroke. That may be because the two categories of heart problems are caused by different factors. The study alone won’t be enough to change the recommendations for heart failure patients, and Berry notes that it highlights a possible connection between exercise and heart failure.
_
Secondary prevention of cardiovascular disease:
The benefits of physical activity and fitness extend to patients with established cardiovascular disease. This is important because, for a long time, rest and physical inactivity had been recommended for patients with heart disease. Unlike studies of primary prevention, many studies of secondary prevention are RCTs. Several systematic reviews have clearly shown the importance of engaging in regular exercise to attenuate or reverse the disease process in patients with cardiovascular disease. For instance, a systematic review and meta-analysis of 48 clinical trials revealed that, compared with usual care, cardiac rehabilitation significantly reduced the incidence of premature death from any cause and from cardiovascular disease in particular. An energy expenditure of about 1600 kcal (6720 kJ) per week has been found to be effective in halting the progression of coronary artery disease, and an energy expenditure of about 2200 kcal (9240 kJ) per week has been shown to be associated with plaque reduction in patients with heart disease. Low-intensity exercise training (e.g., exercise at less than 45% of maximum aerobic power) has also been associated with an improvement in health status among patients with cardiovascular disease. However, the minimum training intensity recommended for patients with heart disease is generally 45% of heart rate reserve. In summary, regular physical activity is clearly effective in the secondary prevention of cardiovascular disease and is effective in attenuating the risk of premature death among men and women.
_
Effects of Exercise on Heart Failure:
Activity restriction was recommended for heart failure (HF) patients until the late 1970s and 1980s, when it was recognized that exercise capacity in patients with left ventricular dysfunction could not be predicted by such parameters as intracardiac filling pressures and left ventricular ejection fraction. Numerous trials have demonstrated that both exercise testing and training of patients with HF appear to be safe. Exercise training benefits HF in several ways. The mean increase in peak VO2 in 15 randomized controlled trials of exercise training that included 426 HF patients was 20.5%. The frequency, duration, and intensity varied among the trials, but all showed an increase in the average peak VO2 between 12% and 31%. In addition to improving exercise capacity, exercise training in HF patients has been shown to improve cardiac output at maximal workloads, improve mitochondrial size and density, increase skeletal muscle oxidative enzymes, reduce endothelial dysfunction, and decrease circulating catecholamines. Exercise training has also been shown to improve quality of life in both men and women with moderate, chronic HF. Whether these physiological adaptations will ultimately reduce mortality and morbidity is yet to be determined by a large prospective trial, although there is at least one small trial which showed a reduction in hospitalizations and improved 1-year survival.
________
Hypertension:
The high prevalence of hypertension (estimated to be one third of the adult population) is due in part to lifestyle factors. Positive lifestyle modifications, including weight loss and increased physical activity, contribute significantly to BP control. Significant reductions in BP after aerobic exercise programs of mild to moderate intensity have been a consistent finding of many well-controlled studies. At least 44 randomized controlled trials including 2674 participants have studied the effect of exercise training on resting blood pressure. The average reduction in systolic and diastolic blood pressure was 3.4 and 2.4 mm Hg, respectively. Baseline blood pressure was an important determinant of the exercise effect. Average systolic and diastolic blood pressures decreased 2.6 and 1.8 mm Hg in normotensive subjects and 7.4 and 5.8 mm Hg in hypertensive subjects, respectively, suggesting that exercise may serve as the only therapy required in some mildly hypertensive subjects. There was no relationship between the weekly training frequency, time per session, or intensity of exercise training and the magnitude of the blood pressure reduction, which suggests that the dose-response curve for exercise and blood pressure is flat. Consequently, increased physical activity is now strongly recommended as part of the lifestyle modifications as an adjunct to pharmacological therapy proposed by the Seventh Report of the Joint National Committee on Prevention, Detection, Evaluation, and Treatment of High Blood Pressure and recent European Society of Hypertension/European Society of Cardiology guidelines.
_
Resistance Exercise and Hypertension:
Strength training as a way to lower BP was traditionally discouraged by physicians and other health professionals largely because excessive elevations in BP have been noted during high-resistance weight-lifting exercises. However, resistance training has been widely recommended in recent years for the elderly, in cardiac rehabilitation programs, and for the public because it is associated with numerous health benefits, including reducing the risk of falls by reversing or attenuating the age-related decline in bone mineral density, muscle mass, and power. Information available on the effects of strength training on resting BP is limited and conflicting. The conclusion of a recent meta-analysis was that the average systolic BP reduction as a result of resistance training was ≈3 mm Hg. This is substantially less than that reported for endurance exercise. Consequently, the recommendation of the American College of Sports Medicine is for resistance training to serve as an adjunct to an aerobic-based exercise program for BP reduction. Despite the limited favorable changes in BP, strength training is associated with numerous other health benefits, and in accordance with recommendations from the American Heart Association and the American College of Sports Medicine, resistance exercise should be implemented as part of a complete exercise program.
_
If you have high blood pressure, your doctor or nurse may suggest that you try to become more active to lower it. However, you may be worried that regular exercise will increase your blood pressure to dangerous levels. It is true that physical activity (exercise) will cause your blood pressure to rise for a short time. However, when you stop the activity, your blood pressure should soon return to normal. The quicker it does this, the fitter you are likely to be. Most people with high blood pressure should be able to increase their physical activity levels quite safely. However, if your blood pressure is relatively high, your doctor or nurse may prefer to lower it with medicines before starting you on an exercise programme. If your blood pressure is very high, you should not start any new activity without consulting your doctor. Everyone, especially people with high blood pressure, should breathe as normally as possible through each exercise. Holding your breath increases blood pressure. The table below gives a general idea of what levels you need to be concerned about, but bear in mind that every person is different, and your doctor or nurse may decide differently.
| Blood pressure level | General ability to be more active |
| Below 90/60 | You may have low blood pressure, speak to your doctor or nurse before starting any new exercise |
| 90/60-140/90 | It is safe to be more active, and it will help to keep your blood pressure in this ideal blood pressure range |
| 140/90 – 179/99 | It should be safe to start increasing your physical activity to help lower your high blood pressure |
| 180/100 – 199/109 | Speak to your doctor or nurse before starting any new exercise |
| 200/110 or above | Do not start any new activity – speak to your doctor or nurse |
To be safe, it is always a good idea to get advice from your doctor or nurse before you start any new physical activity. In moderately severe and severe hypertension (diastolic blood pressure values in excess of 105mm Hg), sporting activities and endurance training are contraindicated till blood pressure is controlled by drugs.
_____
Management of Hypertension in Actively Exercising Patients:
In general, rises in systolic blood pressure to over 200mm Hg during exercise with a workload of 100W are regarded as pathological. Excessive exercise blood pressure values are to be expected in principle in all hypertensives. However, there are so far no generally accepted criteria for diagnosis of isolated systolic exercise hypertension (with normal values of resting blood pressure). The incidence of isolated systolic exercise hypertension is estimated to be about 10% of a selected population. In patients with excessive rises in blood pressure during exercise who want to engage actively in sport, general measures (reduction of obesity, restriction of alcohol and salt intake) and endurance training should be recommended initially. For endurance training, sporting activities that involve dynamic exercise are to be recommended (walking, running, mountain hiking, cycling, swimming, cross-country skiing). Activities involving isometric exercise (rowing, diving, tennis) and sport of a competitive nature are not suitable.
____
Effects of Exercise on Stroke:
Physical activity lowers stroke risk. All stroke survivors should have a medical evaluation before starting an exercise program. The effects of exercise on stroke are less established than those on heart disease, but most studies show benefits.
______
Diabetes mellitus:
For improving blood sugar control, the American Diabetes Association recommends at least 150 minutes per week of moderate-intensity aerobic physical activity (50 – 70% of maximum heart rate) or at least 90 minutes per week of vigorous aerobic exercise (more than 70% of maximum heart rate). Exercise at least 3 days a week, and do not go more than 2 consecutive days without physical activity. Strength training, which increases muscle and reduces fat, is also helpful for people with diabetes who are able to do this type of exercise. The American Diabetes Association recommends performing resistance exercise three times a week. Build up to three sets of 8 – 10 repetitions using weight that you cannot lift more than 8 – 10 times without developing fatigue. Be sure that your strength training targets all of the major muscle groups.
_
Evidence of exercise benefit in diabetes:
A review of 9 trials examining the effect of exercise training in 337 patients with type II diabetes reported an average reduction ofnA1c of 0.5% to 1%. These findings may underestimate the absolute decrease in A1C because of concomitant reductions in diabetic medications. Evidence from large cohort studies demonstrates that physical activity in general provides a highly effective way to delay or avert the development of diabetes mellitus. In addition, physical activity has been shown to reduce the risk of mortality in diabetics. The incidence of type 2 diabetes mellitus was inversely related to leisure time physical activity among men in the Harvard Alumni Study and in US male physicians. Likewise, in the Nurses’ Health Study60 (n=70), the relative risk for developing diabetes mellitus in women was inversely related to the level of fitness as well as exercise volume and intensity in a dose-response fashion. Equivalent energy expenditures from different activities and intensities conferred similar health benefits. These epidemiological findings are supported by 2 interventional studies. In the Finnish Diabetes Prevention Study, 522 middle-aged, overweight men and women were randomized to either an intervention group or a control group. The intervention group was counselled to follow a healthy diet, reduce weight, and increase physical activity. At the end of 3.2 years of follow-up, the cumulative incidence of diabetes mellitus was 11% for the intervention group and 23% for the control group. The overall risk for diabetes mellitus was reduced by 58% in the intervention group. The Diabetes Prevention Program Research Group Study provided strong evidence that lifestyle modifications, including diet and exercise, were more effective in reducing the incidence of diabetes than treatment with metformin. Compared with the control group, the incidence of diabetes mellitus was 58% lower in the lifestyle-intervention group encouraged to exercise 150 min/wk and 31% in the metformin group. The incidence of diabetes mellitus was 39% lower in the lifestyle-intervention group than in the metformin group. To prevent 1 case of diabetes mellitus, the investigators calculated that 6.9 persons would have to participate in the lifestyle-intervention group and 13.9 would have to receive metformin. Finally, lifestyle intervention resulted in more participants maintaining normal blood glucose values over a period of 3 years compared with the metformin or placebo group. Evidence also suggests that the all-cause mortality risk in physically unfit or sedentary diabetics is >2 times higher compared with physically fit men and women diabetics regardless of body weight. Because blacks have a 2- to 6-fold higher risk for developing diabetes mellitus and approximately double the diabetes mellitus death rate compared with whites, the relationship between exercise capacity and all-cause mortality in black and white diabetic individuals was assessed in the Veterans Exercise Testing Study. The findings support the concept that exercise capacity is a strong predictor of mortality in black and white men with type 2 diabetes mellitus. The age-adjusted reduction was graded and more pronounced in whites than in blacks; each 1-MET increase in exercise capacity yielded 14% and a 19% lower risk for blacks and whites, respectively Similarly, the risks were 34% and 46% lower for moderately and highly fit blacks versus blacks in the low-fitness category, respectively. For whites, the comparable reductions were 43% and 67%, respectively.
_
Physical activity activates has acute and chronic effects on glucose, lipid and protein metabolism. In type 1 diabetic subjects, the lack of the physiological inhibition of insulin secretion during exercise results in a potential risk of hypoglycemia. On the other hand, exercise-induced activation of counterregulatory hormones might trigger an acute metabolic derangement in severe insulin-deficient subjects. Thus, diabetic patients, before starting exercise sessions, must be carefully educated about the consequences of physical activity on their blood glucose and the appropriate modifications of diet and insulin therapy. Long-term effects of regular exercise are particularly advantageous for type 2 diabetic patients. Regular aerobic exercise reduces of visceral fat mass and body weight without decreasing lean body mass, ameliorates insulin sensitivity, glucose and blood pressure control, lipid profile and reduces the cardiovascular risk. For these reasons, regular aerobic physical activity must be considered an essential component of the cure of type 2 diabetes mellitus. In this regard, individual behavioral strategies have been documented to be effective in motivating sedentary type 2 diabetic subjects to the adoption and the maintenance of regular physical activity.
_
The rulebook of physically active insulin-treated diabetic subjects:
1. Inject regular insulin or fast-acting insulin analogues into abdominal subcutaneous region
2. Cut regular insulin or fast-acting insulin dosage by 10-40% before the exercise, dependent on duration and intensity of the session
3. Plan to exercise 3-4 hours after the injection of regular insulin or 2 hours after the injection of fast-acting insulin analogue
4. Before starting the exercise session, check your blood glucose
5. Before starting, ingest 20-60 g of simple carbohydrates if your blood glucose is less than 120 mg%
6. Before starting, delay the exercise session if your blood glucose is less than 80 mg%
7. Before starting, delay the exercise session if your blood glucose is greater than 250 mg%; you can exercise only if your blood or urinary ketones are negative
8. During exercise of moderate (60-75% maximal heart rate) or higher intensity supplement with 20-60 g of simple carbohydrates, every 30 minutes
9. Check your blood glucose after 30 minutes of exercise
10. After exercise, cut your usual pre-meal regular insulin or fast-acting insulin dosage by 10-30%
_
Exercises to avoid when you have Diabetes:
Regular physical activity is an important part of a healthy lifestyle when you have diabetes. It is good for your cardiovascular system and can help control blood glucose levels. However, there are times when you need to be careful about exercising with diabetes. If you have certain diabetes complications, there are exercises that you should avoid. The following complications may affect your exercise routine:
1. Proliferative diabetic retinopathy (PDR)—Patients with diabetes and active PDR should avoid activities that involve strenuous lifting; harsh, high-impact activities; or placing the head in an inverted position for extended periods of time.
2. Diabetic peripheral neuropathy— Diabetic peripheral neuropathy may result in loss of sensation and position awareness of your feet. Repetitive exercise on insensitive feet can lead to ulceration and fractures.
3. Advanced kidney disease— Individuals with diabetes and advanced kidney disease can engage in moderate intensity activities, but should avoid strenuous activity.
4. High blood glucose levels— Individuals with type 1 diabetes should avoid exercise if fasting blood glucose is higher than 250 mg/dl and ketones are present. Caution should be used if glucose levels are higher than 300 and no ketones are present. Individuals with type 2 diabetes should avoid exercise if blood glucose is higher than 400 mg/dl. Monitoring blood glucose before, after and possibly during physical activity is necessary to keep blood glucose within an appropriate range.
Always consult with an exercise or health care professional before beginning any fitness program.
_______
Immune system:
Epidemiological evidence suggests that moderate exercise has a beneficial effect on the human immune system; an effect which is modelled in a J curve. Moderate exercise has been associated with a 29% decreased incidence of upper respiratory tract infections (URTI), but studies of marathon runners found that their prolonged high-intensity exercise was associated with an increased risk of infection occurrence. Regular moderate exercise is associated with a reduced incidence of infection compared with a completely sedentary state. However, prolonged bouts of strenuous exercise cause a temporary depression of various aspects of immune function (e.g., neutrophil respiratory burst, lymphocyte proliferation, monocyte antigen presentation) that usually lasts ∼3–24 h after exercise, depending on the intensity and duration of the exercise bout. Postexercise immune function dysfunction is most pronounced when the exercise is continuous, prolonged (>1.5 h), of moderate to high intensity (55–75% maximum O2 uptake), and performed without food intake. Periods of intensified training (overreaching) lasting 1 wk or more may result in longer lasting immune dysfunction. Although elite athletes are not clinically immune deficient, it is possible that the combined effects of small changes in several immune parameters may compromise resistance to common minor illnesses, such as upper respiratory tract infection. However, this may be a small price to pay as the anti-inflammatory effects of exercise mediated through cytokines and/or downregulation of toll-like receptor expression are likely mediators of many of the long-term health benefits of regular exercise.
_
The figure above shows possible mechanisms by which exercise increases susceptibility to infection but reduces inflammation and risk of developing chronic disease. TLR, Toll-like receptor; TH1, T helper 1; IL-1ra, IL-1 receptor antagonist. The encircled minus sign represents an inhibitory action of IL-6 on TNF production.
______
Inflammation:
Acute exercise induces a transient inflammatory response, including heightened CRP concentration. This is most likely due to joint and muscle inflammation after vigorous activity. However, regular, sustained exercise has been shown to suppress inflammation. This has been observed by studying inflammatory markers and physical activity patterns cross-sectionally and also by measuring CRP before and after periods of training. Among runners studied before and after 9 months of training in preparation for a marathon, mean CRP decreased by 31%. A strong and independent association between higher physical activity patterns and level of CRP was also observed in 3638 middle-aged or older healthy men. Those who engaged in physical activity ≥5 times per week had 37% lower CRP levels than those who performed activity roughly once a week or less. In a more generalized follow-up from the National Health and Nutrition Examination Survey III, CRP levels from 13748 adults were analyzed; the most active subjects had CRP levels nearly 50% lower than those of sedentary subjects. CRP levels have shown similar improvements in response to 3 months of cardiac rehabilitation. Some reports suggest that CRP and other inflammatory markers are lower only among subjects who engage in relatively vigorous activities (jogging and aerobic classes) compared with those participating in less demanding activities. However, others have reported markedly reduced CRP levels among those engaging in both larger and smaller volumes of physical activity compared with those who are sedentary. Biomarkers of inflammation such as C-reactive protein, which are associated with chronic diseases, are reduced in active individuals relative to sedentary individuals, and the positive effects of exercise may be due to its anti-inflammatory effects.
_
It is widely recognized that atherosclerosis is largely an inflammatory process. The “response to injury” hypothesis as a cause of atherosclerosis suggests that damage to the arterial endothelium initiated by a pathogen leads to immune responses that interact with metabolic risk factors to propagate an arterial lesion, eventually progressing to an atherosclerotic plaque. Circulating immune cells are recruited to the inflamed vessel by interacting with adhesion molecules and other proteins associated with the body’s immune response. Inflammation particularly occurs in areas where plaque is unstable. It is thought that as many as 70% of myocardial infarctions occur in areas of “vulnerable plaque.” A number of blood markers have been identified that are associated with inflammation, most notably white blood cell count, C-reactive protein (CRP), homocysteine, fibrinogen, and other proteins involved in the immune response. The most widely studied inflammatory blood marker is CRP. In a recent follow-up study, elevated levels of CRP were associated with a higher risk of myocardial infarction, stroke, and mortality in both healthy individuals and patients with existing cardiovascular disease. The relationship between CRP and cardiovascular risk has consistently been shown to be independent of traditional risk factors such as smoking, hypertension, and lipid disorders. Others observed that CRP added markedly to the prognostic power of traditional risk factors and had twice the predictive value for cardiovascular events as low-density lipoprotein and HDL cholesterol. In the Physicians’ Health Study, the highest risk quartile for CRP was associated with a nearly 3-fold risk of sudden cardiac death compared with subjects in the lowest quartile for CRP. In addition, several recent studies have shown that higher CRP levels and other inflammatory markers are associated with risk factors that define the metabolic syndrome (abnormal blood glucose, obesity, low HDL cholesterol, high triglycerides, hypertension). In individuals with heart disease, exercise interventions lower blood levels of fibrinogen and C-reactive protein, an important cardiovascular risk marker. The depression in the immune system following acute bouts of exercise may be one of the mechanisms for this anti-inflammatory effect.
_____
Thrombosis:
Thrombosis plays a significant role in the pathogenesis of acute myocardial infarction, unstable angina, and sudden cardiac death, and therefore this issue has long been the topic of studies in the context of acute and chronic exercise. A number of hemostatic changes occur with exercise that involves blood platelets, coagulation factors, and fibrinolysis. Thrombin, a protein that has multiple catalyzing effects that promote clotting, activates platelets and other proteins in the “coagulation cascade,” leading to enhanced fibrin generation and clot formation. Both acute and chronic exercise regimens influence these markers of blood homeostasis. Because acute exercise is thought to increase platelet aggregation, concerns have been raised regarding exercise as a potential trigger for thrombosis-related cardiac events. However, such events are rare during exercise, and the precise role of the coagulation cascade in triggering cardiac events with acute exercise is unclear. For example, acute exercise increases some clotting factors (particularly factor VIII and von Willebrand factor), and this has been associated with a reduction in clotting time, but it is unclear whether this leads to significant thrombin generation and/or fibrin formation. Many of these changes disappear quickly during recovery from exercise, although other factors may take as long as 48 hours to return to baseline levels. There is considerable interindividual variability in the response to acute exercise, and these responses are dependent on exercise intensity, suppressed by β-blockade, enhanced by catecholamine responses, and more pronounced among patients with coronary artery disease. In contrast to acute exercise, both higher physical activity patterns and structured exercise programs have an inhibitory effect on thrombogenic factors and enhance blood fibrinolytic potential. These changes have been demonstrated in both healthy subjects and patients with cardiovascular disease and occur across a broad range of factors involved in the coagulation cascade. For example, platelet aggregation has been shown to be reduced after a low to moderate period of exercise training in overweight, hypertensive men and other high-risk groups. Although cross-sectional studies have consistently shown that plasma fibrinogen is lower among more active subjects, controlled training studies on the effects of fibrinogen have been mixed. Nevertheless, the findings of most studies suggest that regular exercise has a significant impact on the coagulation cascade and may be a factor underlying the reduction in cardiovascular risk among physically active individuals.
________
Osteoporosis, fractures and falls:
Exercise is very important for slowing the progression of osteoporosis, and extremely important for reducing the risk of falling, which causes fractures. Falls are one of the leading causes of death in people over the age of 65. Exercise helps build balance and flexibility, which reduces the risk of falling.
_
Primary prevention:
Weight-bearing exercise, especially resistance exercise, appears to have the greatest effects on bone mineral density. In one review, several cross-sectional reports revealed that people who did resistance training had increased bone mineral density compared with those who did not do such training. Furthermore, athletes who engaged in high-impact sports tended to have increased bone mineral density compared with athletes who engaged in low-impact sports. Numerous longitudinal studies have examined the effects of exercise training on bone health in children, adolescents, and young, middle-aged and older adults. There is compelling evidence that routine physical activity, especially weight-bearing and impact exercise, prevents bone loss associated with aging. In a meta-analysis of RCTs, exercise training programs were found to prevent or reverse almost 1% of bone loss per year in the lumbar spine and femoral neck in both pre-and postmenopausal women. Exercise training appears to significantly reduce the risk and number of falls. The risk and incidence of fractures is also reduced among active people. Among 3262 healthy men (mean age 44 years) followed for 21 years, intense physical activity at baseline was associated with a reduced incidence of hip fracture (hazard ratio 0.38, 95% CI 0.16 to 0.91). This observation supports findings from an earlier investigation in which fracture rates were lower among people who performed more weight-bearing activities than among sedentary people. In summary, routine physical activity appears to be important in preventing loss of bone mineral density and osteoporosis, particularly in postmenopausal women. The benefits clearly outweigh the potential risks, particularly in older people.
_
Secondary prevention:
Preliminary evidence from an RCT indicates that exercise training is effective in improving bone density in older women (75–85 years of age) with low bone mineral density. In this 6-month RCT, 98 women were randomly assigned to participate in resistance training (n = 32), agility training (n = 34) or stretching (sham exercise, n = 32). Agility training resulted in a significant increase in cortical bone density by 0.5% (standard error of the mean [SEM] 0.2%) at the tibial shaft, and resistance training resulted in a significant increase in cortical bone density by 1.4% (SEM 0.6%) at the radial shaft; the stretching group experienced losses in cortical bone density. Furthermore, a study involving early postmenopausal osteopenic women revealed that a 2-year intensive training program was effective in attenuating the rate of bone loss. In summary, preliminary evidence indicates that regular physical activity is an effective secondary preventive strategy for the maintenance of bone health and the fight against osteoporosis.
_
Efficacy of physical exercise in preventing falls in older adults with cognitive impairment: A systematic review and meta-analysis: 2015:
Seven randomized controlled trials involving 781 participants were included, 4 of which examined solely older people with cognitive impairment. Subgroup data on persons with cognitive impairment were obtained from the other 3 trials that targeted older populations in general. The meta-analysis showed that physical exercise had a significant effect in preventing falls in older adults with cognitive impairment, with a pooled estimate of rate ratio of 0.68 (95% confidence interval 0.51-0.91). The present analysis suggests that physical exercise has a positive effect on preventing falls in older adults with cognitive impairment. Further studies will be required to determine the modality and frequency of exercise that are optimal for the prevention of falls in this population.
_______
Asthma and chronic obstructive pulmonary disease (COPD):
_
Effects of Exercise on Asthma
Exercise-Induced Asthma (EIA):
Exercise-induced asthma occurs when exercise triggers coughing, wheezing, or shortness of breath. It occurs most often in children and young adults and during intense exercise in cold dry air. EIA is triggered only by exercise. Unlike allergic asthma, there is no long-term increase in airway activity. People who have only EIA do not need long-term maintenance therapy. The warm-up and cool-down periods, which are important for any exercise regimen, may help reduce EIA events. EIA is not a reason to exclude people from physically demanding occupations. The preferred term for this condition is exercise-induced bronchoconstriction (EIB); exercise does not cause asthma, but is frequently an asthma trigger. If you have EIB, you may have problems breathing within five to 20 minutes after exercise. Symptoms of EIB are similar to those of chronic asthma, but the timing of the symptoms is closely linked with physical activity. People with EIB are typically very sensitive to both low temperatures and dry air. Air is usually warmed and humidified by the nose, but during demanding activity people breathe more through their mouths. This allows cold, dry air to reach your lower airways and your lungs without passing through your nose, triggering asthma symptoms. Air pollutants, high pollen levels and viral respiratory infections may also be triggers. Other causes of symptoms while exercising include being out of shape, poorly controlled nasal allergies or vocal cord issues.
_
Exercise is a common trigger of asthma, particularly in children. The mechanism is linked to hyperventilation, which results in increased osmolality in airway lining fluid and triggers mast cell mediator release, resulting in bronchoconstriction. Exercise-induced asthma (EIA) typically begins after exercise has ended, and recovers spontaneously within about 30 minutes. EIA is worse in cold, dry climates than in hot, humid conditions. It is, therefore, more common in sports such as cross-country running in cold weather, overland skiing, and ice hockey than in swimming. It may be prevented by prior administration of beta 2-agonists and antileukotrienes, but is best prevented by regular treatment with inhaled corticosteroids, which reduce the population of surface mast cells required for this response.
_
The following are some suggestions for reducing the impact of EIA:
•For those with chronic asthma, follow the health care provider’s instructions for using long-term control medications, particularly inhaled corticosteroids, when prescribed.
•Warm-up and cool-down periods are important.
•Patients with EIA might do better with activities that involve short bursts of exercise (tennis, football), rather than with exercises involving long-duration regular pacing (cycling, soccer, and distance running). In winter, indoor exercise is best. Swimming is particularly desirable because of the humidity.
•When exercising in cold air, breathing through a scarf or through the nose helps warm up the airways.
_
Managing EIA/EIB:
People with EIB are still able to exercise – and should exercise regularly. But you need to be sure that you are doing the right kind and right amount of exercise. To prevent asthma flare-ups, your doctor may prescribe that you take an inhaled short-acting medication prior to exercise. These medications are effective in preventing EIB symptoms in 80 to 90% of patients. Drinking water, warming up and cooling down as part of your exercise routine can also help minimize EIB
_
Is it good for people with asthma to exercise?
Yes. Even though physical exercise is a common trigger of asthma symptoms, it is just as important for people with asthma to exercise as for anyone else. Keep in mind that it takes time to get in shape and you lose fitness quickly when you stop exercising regularly. With the right medication, most people with asthma will be able to do some kind of physical exercise, many will feel no restrictions, and some will only react to exercise in combination with other triggers.
_
How can I avoid exercise-induced asthma?
The best way to avoid exercise-induced asthma is to make sure that your asthma is properly controlled and, if necessary, that you take extra medication before exercising. A good warm-up also reduces the risk of exercise-induced asthma. Anti-inflammatory treatment, preferably with inhaled corticosteroids, taken regularly will prevent exercise-induced asthma in many people. However, some people still need to take an airway opener (bronchodilator) before exercise. Many people with asthma should have daily treatment with both inhaled corticosteroids and a long acting bronchodilator. Combination medications are now available in many countries. Particular types of exercise, such as running and jogging, are more likely to expose the airways to large volumes of dry air and trigger asthma, while less vigorous activities, like swimming and yoga, are less likely to cause these symptoms.
_
What types of Exercise are best for people with Asthma?
Activities that involve short, intermittent periods of exertion, such as volleyball, gymnastics, baseball, and wrestling, are generally well tolerated by people with symptoms of asthma. Activities that involve long periods of exertion, such as soccer, distance running, basketball, and field hockey, may be less well tolerated. Also, cold-weather sports, such as ice hockey, cross-country skiing, and ice-skating, may pose challenges. However, many people with asthma are able to participate fully in these activities. Swimming, which is a strong endurance sport, is generally well tolerated by many people with asthma because it is usually performed while breathing warm, moist air. It is also an excellent activity for maintaining physical fitness. Other beneficial activities for people with asthma include both outdoor and indoor biking, aerobics, walking, and running on a treadmill.
_
Study finds that Daily Exercise relieves Asthma symptoms: 2015:
Physical activity has been shown to offer various health benefits for patients with asthma, especially in children. However, there is still limited data on the nature of the association between physical activity and asthma control in adults. Results from a recent study published in the BMJ Open Respiratory Research, a team of researchers found that asthma patients who engaged in optimal levels of physical activity on a regular basis were nearly two-and-a-half times more likely to have good control of their symptoms compared to those who didn’t exercise. Just 30 minutes a day of walking, riding a bike, doing yoga — anything active, really — can result in significant reduction of asthma symptoms. Patients with asthma have been discouraged from engaging in physical exercise as it is thought to trigger shortness of breath and asthma attacks. However, simple protective measures can be taken to prevent the discomforts that physical activity can cause. The issue of exercise-induced bronchospasm is real — but if you use your reliever medication before you exercise, and then take the time to cool down afterwards, you should be okay.
______
Effects of Exercise on COPD:
Walking is the best exercise for people with emphysema. Patients should try to walk three to four times daily for 5 – 15 minutes each time. Devices that assist ventilation may reduce breathlessness that occurs during exercise. Exercising and strengthening the muscles in the arms and legs helps some patients improve their endurance and reduce breathlessness Inspiratory muscle training involves exercises and devices that make inhaling (breathing in) more difficult, in order to strengthen breathing muscles. Yoga or martial arts exercises, such as tai chi, which emphasize breathing techniques and balanced movements, may be particularly beneficial for patients with emphysema. A study found that for COPD, incremental aerobic resistance physical exercises are better than constant load physical exercises at an intensity range from 90% to 50 % of VO2 max, with a frequency of two or four days a week, the session is from 30 to 60 minutes during a period of treatment from eight to twelve weeks. Exercise training induces several symptomatic and functional adaptations resulting in an increased aerobic capacity.
______
Exercise and testosterone:
If you’re a man with low testosterone, exercise may help. Doctors and fitness professionals still have a lot to learn about exercise and its effects on testosterone. Several factors besides your workout are involved. But one thing is clear: You need to make exercise a habit in order to get the benefits. After exercise, testosterone levels rise — but not for long. It’s not yet clear what health effects, if any, these temporary boosts may have. Of course, exercise has many other well-known health perks. For men who have low testosterone, exercise alone probably won’t raise their levels enough to make a difference in how they feel but for men whose testosterone level is on the borderline between normal and low, it’s going to have a much more potent effect.
_
Exercise improves sex life:
Studies show exercise leads to a higher quality sex life. It soups up your sex life. Sex and exercise go hand-in-hand. In a study of women between 45 and 55 years old, those who exercised, including brisk walking, reported not only greater sexual desire, but better sexual satisfaction, too. You are also likely to feel more fit and be more fit, which in turn will benefit your interest in and ability to carry out sexual activity. Your emotional resilience will also be greater if you exercise, which also benefits your relationship health. Regular exercise boosts circulation, and primes the brain for sexual satisfaction. It gets your blood flow pumping, which not only creates rosy cheeks, but also improves arousal. Physical fitness can increase blood flow, which in theory can make sex more pleasurable since sexual arousal for both men and women involves increased blood flow to the genital area. Lubrication, genital sensation, and the tingle of sexual excitement are all fuelled by good blood flow. In order to have an erection, the penis must swell with blood. Blocked arteries, high blood pressure and other cardiovascular issues can interfere with that process. Exercise keeps the heart and arteries healthy, reducing the risk of erectile dysfunction. Researchers looked at men over the age of 50 and found that those who were physically active reported better erections and a 30% lower risk of impotence than men who were inactive. During exercise, endorphins bathe the brain, washing away tension and ushering in positive, empowering thoughts. In addition, exercise increases testosterone (essential for libido), by adding muscle mass, and this can take your libido to new heights and mentally (as well as the physical) improve our body image, making us more confident in the bedroom. Exercise strengthens pelvic floor muscles so that both men and women get better and intense orgasm. Not only can exercise improve your sex life, but sex can actually double as exercise. An energetic session can scorch calories and give you a full-body workout, especially if you incorporate plenty of positions and foreplay. Sex itself is a physical activity and burns calories and increases fitness. Many factors influence how many calories are spent during sex, but most reports seem to indicate about 85 for a half hour to hour session. Besides sex can also increase self-esteem, cardio-vascular health, emotional intimacy, improves sleeping, and increase immunity!
______
______
Exercise and obesity:
Obesity and overweight are considered to be leading risk factors for a number of chronic health conditions, including diabetes mellitus, hypertension, CHD, and premature mortality. Obesity not only increases CHD risk directly but also enhances it indirectly through its adverse effects on several established risk factors, including insulin resistance and hypertension. Although the causes of obesity are complex, physical inactivity is considered to be an important causal factor. For example, in a representative sample of American adults, the relative risk of obesity among individuals physically active in leisure time (≥5 bouts of physical activity per week) was ≈50% lower than among those who were physically inactive. Although such an association does not demonstrate cause and effect, this and similar reports strongly suggest that a relationship exists between physical activity levels and obesity, in which comparatively sedentary individuals are more likely to be obese compared with those who are physically active.
_
Despite relatively modest weight reductions associated with structured programs of physical activity, findings from large epidemiological studies support the concept that a reduced risk of cardiovascular disease and all-cause mortality occurs among more active individuals regardless of weight loss. In a large follow-up from the ACLS (n=25 714), higher fitness levels were associated with lower risk of mortality in normal-weight, overweight, and obese men. Compared with other risk factors (total cholesterol, hypertension, and smoking), having a low fitness level carried similarly heightened risks in each weight category for both cardiovascular and all-cause mortality. In a subsequent study from the ACLS among older subjects (>60 years), higher waist circumference was associated with higher mortality, but this association was not significant after adjustment for fitness. Fitness strongly predicted mortality independent of measures of body dimensions. These investigators suggested that it is as important for clinicians to assess the fitness status of an overweight or obese patient as it is to evaluate BP, inquire about smoking habits, and measure fasting plasma glucose and lipid levels. As mentioned above, modest weight reductions have been associated with structured programs of physical activity. Because of the high prevalence of overweight and obesity among patients referred for cardiac rehabilitation (estimated to be >80%), there has been recent interest in high-calorie-expenditure exercise. A recent trial demonstrated that patients randomized to an intensive counselling and exercise program designed to achieve an energy expenditure of 3000 to 3500 kcal/wk experienced double the weight loss of those in the standard cardiac rehabilitation group (8.2±4 versus 3.7±5 kg), a greater reduction in waist circumference, reduced insulin resistance, improved blood lipids, and lower prevalence of the metabolic syndrome (59% versus 31%).
_
The following are some suggestions and observations on exercise and weight loss:
•The treadmill burns the most calories of standard aerobic machines. Exercise sessions as short as 10 minutes, which are done frequently (about four times a day), may be the most successful program for obese people.
•The more strenuous the exercise, the longer the body continues to burn calories before returning to its resting level. This state of fast calorie burning can last for as little as a few minutes after light exercise, to as long as several hours after prolonged or heavy exercise.
•Resistance (strength) training is excellent for reducing fat and building muscles. It should be performed two or three times a week.
•Fidgeting may be very helpful in keeping pounds off. Regular exercise is certainly the best course, but for people who must sit for hours at work, frequently shifting positions while sitting may have some benefit.
•It is important to realize that as people slim down, they burn fewer calories per mile of walking or jogging. The rate of weight loss slows down, sometimes discouragingly so, after an initial dramatic head start using diet and exercise combinations. People should be aware of this trend and keep adding to their daily exercise routine.
•Changes in fat and muscle distribution may differ between men and women as they exercise. Men tend to lose abdominal fat (which lowers their risk for heart disease faster than reducing general body fat). In women, aerobic and strength training are more likely to result in fat loss in the arms and trunk. However, they do not gain muscle tissue in those areas.
Because obesity is one of the risk factors for heart disease, anyone who is overweight must discuss their exercise program with a physician before starting.
_
How much am I burning?
This chart shows the estimated number of calories burned while doing various exercises for one hour. Specific calorie expenditures vary widely depending on the exercise, intensity level and individual characteristics such as weight.
| Activity (1-hour duration) | Weight of person and calories burned | ||
| 160 pounds (73 kilograms) | 200 pounds (91 kilograms) | 240 pounds (109 kilograms) | |
| Aerobics, high impact | 533 | 664 | 796 |
| Aerobics, low impact | 365 | 455 | 545 |
| Aerobics, water | 402 | 501 | 600 |
| Backpacking | 511 | 637 | 763 |
| Basketball game | 584 | 728 | 872 |
| Bicycling, < 10 mph, leisure | 292 | 364 | 436 |
| Bowling | 219 | 273 | 327 |
| Canoeing | 256 | 319 | 382 |
| Dancing, ballroom | 219 | 273 | 327 |
| Elliptical trainer, moderate effort | 365 | 455 | 545 |
| Football, touch or flag | 584 | 728 | 872 |
| Golfing, carrying clubs | 314 | 391 | 469 |
| Hiking | 438 | 546 | 654 |
| Ice skating | 511 | 637 | 763 |
| Racquetball | 511 | 637 | 763 |
| Resistance (weight) training | 365 | 455 | 545 |
| Rollerblading | 548 | 683 | 818 |
| Rope jumping | 861 | 1,074 | 1,286 |
| Rowing, stationary | 438 | 546 | 654 |
| Running, 5 mph | 606 | 755 | 905 |
| Running, 8 mph | 861 | 1,074 | 1,286 |
| Skiing, cross-country | 496 | 619 | 741 |
| Skiing, downhill | 314 | 391 | 469 |
| Skiing, water | 438 | 546 | 654 |
| Softball or baseball | 365 | 455 | 545 |
| Stair treadmill | 657 | 819 | 981 |
| Swimming laps, light or moderate | 423 | 528 | 632 |
| Swimming laps, vigorous | 715 | 892 | 1,068 |
| Tae kwon do | 752 | 937 | 1,123 |
| Tai chi | 219 | 273 | 327 |
| Tennis, singles | 584 | 728 | 872 |
| Volleyball | 292 | 364 | 436 |
| Walking, 2 mph | 204 | 255 | 305 |
| Walking, 3.5 mph | 314 | 391 | 469 |
| Yoga, hatha | 183 | 228 | 273 |
| Yoga, power | 292 | 364 | 436 |
__
Although vigorous exercise is good for weight loss, moderate aerobic exercise burning 3500 Kcal per week confers survival benefit:
One recent study found that in overweight sedentary subjects, moderate exercise was more efficient at helping them burn body fat – including a reduction that was far greater than what could be explained by the caloric expenditure – while intense exercise induced a “compensatory” response that hampered fat loss. Another study examined weekly caloric expenditure via aerobic exercise in a group of former athletes and non-athletes and plotted it against mortality, cardiovascular disease, and hypertension. Those who exercised moderately lived the longest and were healthiest. In a study on the exercise habits of college alumni and their impact on mortality, researchers found that up to 3,500 calories expended per week conferred a survival benefit, but at calorie expenditures greater than that, mortality began to tick upwards. And in a pair of recent studies, researchers found that moderate exercise – jogging up to 20 miles a week at an 11 minute mile pace – offered the most protection against early mortality. Running more than 20 miles a week, or running at a 7 minute mile pace, offered fewer mortality benefits. In the second paper, Danish scientists found that people who spent one to two and a half hours jogging at a “slow or average pace” lived longer than those who didn’t run at all or who ran at a faster pace. James O’Keefe, a cardiologist and presenter at the Ancestral Health Symposium, was quoted as saying that “after about 45 to 60 minutes a day, you reach a point of diminishing returns.” It’s pretty clear that once exercise gets to be “too much,” the benefits are reduced, or even reversed, and it becomes a chronic stressor that reduces overall wellness.
_
What’s better for Weight Loss: Diet or Exercise?
A new study in the International Journal of Epidemiology shows that it might be more about what you eat, putting truth to the idiom “abs are made in the kitchen, not the gym.” In 2013, researchers from Loyola University began looking into the relative power of diet and exercise as they relate to moving the scale. They thought they’d discover that exercise would prove to be a crucial component for weight loss. Two years later, though, the science shows that the largest driver behind obesity is not how sedentary people are but instead how poor their diet is. Physical activity is crucially important for improving overall health and fitness levels, but there is limited evidence to suggest that it can blunt the surge in obesity. Why? The more you work out, the more your appetite increases. Of course, this new Loyola study isn’t the first to come to this conclusion. Research has consistently shown for years now that exercise doesn’t necessarily lead to weight loss. In a meta-analysis published in the Journal of the Academy of Nutrition and Dietetics last year, for example, researchers found that people only lost noticeable weight if they combined exercise and calorie restriction. Plus, research shows that dieters who exercise are better able to maintain weight loss and are also able to lose fat while keeping valuable muscle. You just need to make sure you’re logging your gym time and your food intake. Researchers challenge conventional wisdom further by arguing that those who want to avoid excess weight gain should adopt a diet that is high in fat but low on both sugar and carbohydrates. Athletes and others about to do exercise should ditch high-carbohydrate intake regimes and instead eat more fat, they say, because “fat, including ketone bodies, appears to be the ideal fuel for most exercise. It is abundant, does not need replacement or supplementation during exercise, and can fuel the forms of exercise in which most participate.” Catherine Collins, of the British Dietetic Association, said the doctors had downplayed the metabolic and physical health benefits of undertaking even moderately intense exercise and had used “incomplete evidence” to make their case. Professor Susan Jebb, professor of diet and population health at Oxford University, who also chairs the food network of the government’s Responsibility Deal, said: “The authors fail to note that weight loss programmes which combine diet and physical activity are the most successful route to weight loss in both the short (three to six months) and medium term (12 months)”.
_______
Belly fat:
The myth of targeted fat reduction:
Spot reduction is a myth that exercise and training a particular body part will preferentially shed the fat on that part; for example, that doing sit-ups is the most direct way to reduce subcutaneous belly fat. This is false: one cannot reduce fat from one area of the body to the exclusion of others. Most of the energy derived from fat gets to the muscle through the bloodstream and reduces stored fat in the entire body, from the last place where fat was deposited. Sit-ups may improve the size and shape of abdominal muscles but will not specifically target belly fat for loss. Such exercise might help reduce overall body fat and shrink the size of fat cells. There is a very slight increase in the fat burnt at the area being exercised (e.g. abs) compared with the rest of the body, due to the extra blood flow at this area.
_
Reduce belly fat:
An extra storage of fat in the belly could bring about different health conditions. There are two kinds of belly fat: visceral and subcutaneous. If the amount of fat in the belly area is large, there is greater risk of developing joint problems, sleep apnea, colorectal cancer, high blood pressure, diabetes, breast cancer, and heart disease. If you’re looking to shrink and tone your belly, there’s a better way to do it than trying to do crunches. In fact, research has shown that doing abdominal exercises alone—even when performed five days a week for six weeks—has no effect at all on subcutaneous fat stores and abdominal circumference. Jennifer Cohen suggests using strategies that burn up cortisol instead. Cortisol is a hormone in your body that depletes lean muscle and holds on to fat in the abdominal region. One of the most important ways to help this process is to reduce stress in your life, because stress causes cortisol levels to spike. Cohen also delves into a number of other strategies that help reduce your cortisol levels, such as the following.
1. Getting enough sleep
2. Reducing or eliminating refined sugars from your diet
3. Slowing down your breathing
4. Doing short bursts of exercise (high-intensity interval training)
5. Supplementing with vitamin C
6. Eating fats―the good kinds such as the omega 3’s found in salmon, avocados and walnuts
_
Once you’ve addressed your diet, exercise can truly begin to work its magic on your physique, and help boost fat loss even further. The trick to achieve flat abs is to incorporate the correct types of exercises. High-intensity interval exercises are at the core. This short intense training protocol improves muscle energy utilization and expenditure due to its positive effects on increasing muscle mass and improving muscle fiber quality. Muscle tissue burns three to five times more energy than fat tissues, so as you gain muscle, your metabolic rate increases, which allows you to burn more calories, even when you’re sleeping. Further, several studies have confirmed that exercising in shorter bursts with rest periods in between burns more fat than exercising continuously for an entire session. In fact, you can actually lose more weight by reducing the amount of time you spend on exercise, because when doing high-intensity interval training you only need 20 minutes, two to three times a week.
_
Exercises that target your Abs:
While ab workouts specifically may not help you reduce body fat, they still provide important benefits and should not be overlooked. Your abdominals are part of your body’s 29 core muscles, which are located mostly in your back, abdomen and pelvis. This group of muscles provides the foundation for movement throughout your entire body, and strengthening them can help protect and support your back, make your spine and body less prone to injury and help you gain greater balance and stability. When you build your ab muscles, it’s like developing an internal corset that holds your gut in. By doing so, you help stabilize your spine, vertebrae and discs, which in turn can significantly reduce back pain and make it easier for you to lift heavy items, twist and turn and perform the movements required for a full life. Having a strong abdominal wall is very important for optimal body movement and gets increasingly more important with advancing age. A strong abdominal wall is also what will produce that six-pack look once you’ve lost sufficient amounts of subcutaneous fat. However, conventional crunches and sit-ups are not the most effective when it comes to creating flat, well-defined abs. In order to effectively train your core muscles, you must incorporate a variety of stabilization, functional and traditional exercises. A study by Petrofsky (2007) actually put this to the test by researching how much muscle activity is generated by different abdominal exercises. The simple, traditional abdominal floor crunch was found to produce and recruit the least amount of muscle activity when subjects were attached to an electromyography (EMG) machine! That’s not to say that you should never perform a traditional abdominal crunch; but this particular exercise should be done as part of a varied core-strengthening routine. This may include:
•Traditional exercises, such as a standard crunch with rotation or a standing rotation with a light hand weight.
•Functional exercises, including work on a stability ball.
•Stabilizing exercises, such as lying on the floor and pulling your belly back toward your spine and holding that position while breathing deeply
•Extension exercises, such as lying on your stomach with arms extended above your head. Then raising both arms and both legs, at the same time, off the floor. (Hold for a count of 5, or 5 breaths, and slowly return to the floor.)
_
How to reduce stomach size after delivery?
Reducing the tummy after delivery can be quite difficult as the stomach of a woman continues to bulge even after child birth. Carrying the weight of the child causes a stretching of the stomach, and it does not go back automatically to the original shape. Some of the tips to reduce fat after delivery include performing some mild exercises after enough rest has been taken post-delivery. A simple routine of walking for around 20 minutes each day can be helpful. It is also essential that you choose the right foods as part of your diet for belly fat reduction. You should include wheat bread, nuts, lean meats, fresh fruits, and leafy vegetables to your meals. It is also important that your diet is healthy as the baby will feed on what you eat. Physical exercise is the best way to reduce tummy after a C-section. However, you should avoid any exercise that is too vigorous as physical stress can have an impact in the natural recovery process. After consulting a doctor, you can also perform some aerobic exercises to decrease stomach fat. These exercises include dancing, swimming, and cycling. However, it is important that you first consult a doctor before performing these exercises. You could also try some crunches and Pilates.
_________
_________
Exercise and brain:
Introduction:
The relationship between exercise and your brain is the most important one for increasing brain power. When we’re young, we lose approximately 2% of our brain volume as brain cells die. Once we reach age 60, brain cell loss accelerates to 2% loss every two years. And for people with Alzheimer’s, cell loss is double that. Unfortunately, it is the hippocampus, the seat of our memory, which loses the most cells. Exercise has been shown to reverse this process of brain atrophy in the hippocampus. One studied showed this could be accomplished simply by walking regularly. Exercise encourages the growth of new brain cells just like it makes our muscles grow. Some neuroscientists believe that exercise might do more to improve your brain than thinking does. Exercise increases circulation which increases the supply of oxygen and glucose to your brain. This particularly benefits the hippocampus and thus improves memory, concentration, and focus. It also benefits the prefrontal cortex where planning and reasoning occur. By improving circulation, you are also reducing your chances of dementia that is caused by heart disease. Exercise also improves blood sugar control which lowers the risk for diabetes. There is a correlation between diabetes and the risk of Alzheimer’s. Exercise increases endorphin release which in turn makes you feel happier and more relaxed, while reducing your risk of developing problems with anxiety or depression. Surprisingly, it’s been found that those who regularly exercise moderately have better cognitive functions than people who regularly exercise strenuously! Strenuous exercise draws glucose and oxygen away from your brain and into your muscles. Vigorous exercise also increases free radical production. Because your brain uses a lot of oxygen, it is very susceptible to free radical damage.
_
There are several possibilities for why exercise is beneficial for the brain.
•increasing the blood and oxygen flow to the brain;
•increasing growth factors that help neurogenesis and promote synaptic plasticity — possibly improving short and long term memory;
•increasing chemicals in the brain that help cognition, such as dopamine, glutamate, norepinephrine, and serotonin.
Physical activity is thought to have other beneficial effects related to cognition as it increases levels of nerve growth factors, which support the survival and growth of a number of neuronal cells.
_
Neurobiology of exercise:
The neurobiological effects of physical exercise are numerous and involve a wide range of interrelated neuropsychological changes. A large body of research in humans has demonstrated that consistent aerobic exercise (e.g., 30 minutes every day) induces persistent beneficial behavioral and neural plasticity as well as healthy alterations in gene expression in the brain; some of these long-term effects include: increased neuron growth, increased neurological activity (c-Fos and BDNF signalling), improved stress coping, enhanced cognitive control over behavior, improved declarative and working memory, and structural and functional improvements in brain structures and pathways associated with cognitive control and memory. The effects of exercise on cognition have important implications for improving academic performance in children and college students, improving adult productivity, preserving cognitive function in old age, preventing or treating certain neurological disorders, and improving overall quality of life.
_
Neuroplasticity and neurogenesis:
Neuroplasticity is essentially the ability of neurons in the brain to adapt over time, and most often occurs in response to repeated exposure to stimuli; whereas neurogenesis is the postnatal (after-birth) growth of new neurons, a beneficial form of neuroplasticity. Aerobic exercise promotes neurogenesis by increasing the production of neurotrophic factors (compounds which promote the growth or survival of neurons), such as brain-derived neurotrophic factor (BDNF), insulin-like growth factor 1 (IGF-1), and vascular endothelial growth factor (VEGF). Consistent aerobic exercise over a period of several months induces marked clinically significant improvements in executive function (i.e., the “cognitive control” of behavior) and increased gray matter volume in multiple brain regions, particularly those which give rise to cognitive control. The brain structures that show the greatest improvements in gray matter volume in response to aerobic exercise are the prefrontal cortex and hippocampus; moderate improvements seen in the anterior cingulate cortex, parietal cortex, cerebellum, caudate nucleus, and nucleus accumbens. The prefrontal cortex, caudate nucleus, and anterior cingulate cortex are among the most significant brain structures in the dopamine and norepinephrine systems that give rise to cognitive control. Exercise-induced neurogenesis (i.e., the increases in gray matter volume) in the hippocampus is associated with measurable improvements in spatial memory. Higher physical fitness scores (measured by VO2 max) are associated with better executive function, faster processing speed, and greater volume of the hippocampus, caudate nucleus, and nucleus accumbens. Long-term aerobic exercise is also associated with persistent beneficial epigenetic changes that result in improved stress coping, improved cognitive function, and increased neuronal activity (c-Fos and BDNF signalling).
_
If you start exercising, your brain recognizes this as a moment of stress. As your heart pressure increases, the brain thinks you are either fighting the enemy or fleeing from it. To protect yourself and your brain from stress, you release a protein called BDNF (Brain-Derived Neurotrophic Factor). This BDNF has a protective and also reparative element to your memory neurons and acts as a reset switch. That’s why we often feel so at ease and like things are clear after exercising. Simultaneously, your brain releases endorphins, another stress-related chemical. The endorphins minimize the physical pain and discomfort associated with exercise. They’re also responsible for the feeling of euphoria that many people report when exercising regularly. The researchers also discovered that exercise does not affect the brains of all people in exactly the same way. Some people, about 30 percent of people of European Caucasian descent, have a BDNF gene variant that hinders post-exercise BDNF production. The people with this BDNF variant did not improve their memory scores, even when exercising regularly, as significantly as those without this variant. Still, the research clearly suggests that—with individual variations as to the degree—regular exercise will cumulatively enhance your memory and other brain functions.
_
Regular exercise has been shown to counter the shrinking of the hippocampus and memory impairment that naturally occurs in late adulthood. Sedentary adults over age 55 show a 1–2% decline in hippocampal volume annually. A neuroimaging study with a sample of 120 adults revealed that participating in regular aerobic exercise increased the volume of the left hippocampus by 2.12% and the right hippocampus by 1.97% over a one-year period. Subjects in the low intensity stretching group who had higher fitness levels at baseline showed less hippocampal volume loss, providing evidence for exercise being protective against age-related cognitive decline. In general, individuals that exercise more over a given period have greater hippocampal volumes and better memory function.
_
Epigenetic effects of exercise on brain:
Figure above shows proposed model for the effect of exercise on molecular, neuroplastic and cognitive patterns through epigenetics. IGF-1: Insulinlike growth factor-1; VEGF: Vascular endothelial growth factor; BDNF: Brain-derived neurotrophic factor.
______
Exercise, cognition and dementia:
_
How exercise improves cognition:
Figure above provides a schematic illustration of some of the important factors which both help to influence whether (and the extent to which) individuals participate in cardiovascular fitness training as well as the potential mechanisms of improved fitness and the influence of these mechanisms on cognition. The factors included in the illustration are derived from animal research, human epidemiological studies, and human randomized clinical trials.
_
Physical activity has been shown to be neuroprotective in many neurodegenerative and neuromuscular diseases. Evidence suggests that it reduces the risk of developing dementia. The Caerphilly Heart Disease Study followed 2,375 male subjects over 30 years and examined the association between regular physical exercise and dementia. The study found that men who exercised regularly had a 59% reduction in dementia when compared to the men who didn’t exercise. In addition, a 2008 review of cognitive enrichment therapies (strategies to slow or reverse cognitive decline) concluded that “physical activity, and aerobic exercise in particular, enhances older adults’ cognitive function”. In mice, exercise improves cognitive functioning via improvement of spatial learning, and enhancement of synaptic plasticity and neurogenesis. In a 2009 study, scientists made two groups of mice swim a water maze, and then in a separate trial subjected them to an unpleasant stimulus to see how quickly they would learn to move away from it. Then, over the next four weeks they allowed one group of mice to run inside their rodent wheels, an activity most mice enjoy, while they forced the other group to work harder on mini-treadmills at a speed and duration controlled by the scientists. They then tested both groups again to track their learning skills and memory. Both groups of mice improved their performances in the water maze from the earlier trial. But only the extra-worked treadmill runners were better in the avoidance task, a skill that, according to neuroscientists, demands a more complicated cognitive response. The mice who were forced to run on the treadmills showed evidence of molecular changes in several portions of their brains when viewed under a microscope, while the voluntary wheel-runners had changes in only one area. According to an author of the study, “our results support the notion that different forms of exercise induce neuroplasticity changes in different brain regions.” Furthermore, anecdotal evidence suggests that frequent exercise may reverse alcohol-induced brain damage. There is also some evidence that physical activity may help to slow the progression of Alzheimer’s and reduce its risk through a number of mechanisms such as promoting vascular health by lowering blood pressure and reducing other risk factors that lead to the disease. Research so far in this area is showing promising results – but further studies need to be done. Epidemiological studies suggest that exercise reduces the risk of Parkinson’s disease, and regular physical activity is shown to improve the quality of life in Parkinson’s disease patients and reduce their neurological symptoms. However, there is limited evidence on the exact cognitive processes and, again, further studies need to be done.
_
Walking slows cognitive decline: 2010 study:
Walking may slow cognitive decline in adults with mild cognitive impairment (MCI) and Alzheimer’s disease, as well as in healthy adults, according to a study presented today at the annual meeting of the Radiological Society of North America.
_
Figure above compares the beneficial effects of physical activity on the brains of healthy aging individuals (n = 299) to the positive relationships between exercise and brain structure in cognitively impaired persons with either mild cognitive impairment or Alzheimer’s (n = 127). In both normal aging and cognitive impairment, physical activity preserves volume in brain areas that are important for memory, learning, and attention. These structures include the prefrontal cortex and temporal cortex. The top row of images shows these relationships in a 3-D rendering of the brain while the bottom row shows the prefrontal cortex findings in side view cutaway images of the brain..
_
Exercise makes you smarter:
University of South Carolina experts found regular treadmill sessions create more mitochondria – structures in the cells that produce the body’s energy – in the brain. This energy boost helped the brain to work faster and more efficiently, effectively keeping it younger, researchers said. In the short term this could reduce mental fatigue and sharpen your thinking in between gym sessions. And building up a large reservoir of mitochondria in the brain could also create a ‘buffer’ against age-related brain diseases such as Alzheimer’s.
_
Exercise improves balance and coordination: 2015 study on twins:
Physical activity can increase grey matter in the brain, increasing the size of areas that contribute to balance and coordination. The changes in the brain may have health implications in the long-term, such as reducing the risk of falling. It could also reduce the risk of being immobile in older age. Authors recruited 10 pairs of identical twins, who were all men aged 32 to 36 years. Focusing on twins, who have the same DNA, would allow researchers to see how their environment affects their bodies. In each pair of twins, one brother had exercised more over the past three years than the other, though they reported they carried out similar levels of exercise earlier in their lives. The twins had MRI scans of their brains so researchers could see whether physical activity had any impact on the size of their brains, and specific regions. Exercise didn’t seem to affect the size of the brain as a whole. But there was a connection between more activity and more brain volume in areas related to movement. The twins who exercised more did a better job of controlling their blood sugar, which reduces the risk of diabetes, a finding which is already well-known. The study was published in the journal Medicine & Science in Sports & Exercise.
_
Physical exercise can keep your brain young: 2015:
In an investigation of more established men between ages 64-75 years, the specialists found that the fitter men performed preferable rationally over the less fit men, by utilizing parts of their brains as a part of the same route as in their childhood. In other words, fit older people are more likely to use their brains the way they did when they were young, compared to older people seeing a decline in this area. This change is known as HAROLD (hemispheric asymmetry reduction in older adults), and reflects adaptations of the brain necessary to make up for reduced brain capacity and efficiency caused by age-related structural and physiological decline. When we’re young, we use the left side of the brain more than the right and older adults tend to have both sides of their PFC active without having a difference between right and left regions.
_
The bottom line is more exercise on a daily basis may very well lead to a younger better performing brain. The secret to a younger brain may be in exercising your body. There has been evidence which supports the theory that adults who are fitter are able to better maintain this white matter than adults who are not as fit.
_
The effects of exercise on cognitive function in children and young adults:
Unfortunately, there have been far fewer studies involving young people. However, one study, reported at the 2001 Society for Neuroscience conference, found that following a 12 week regimen of jogging for 30 minutes two to three times a week, young adults significantly improved their performance on a number of cognitive tests. The scores fell again if participants stopped their running routine. The researchers suggested that increased oxygen flow to the brain might have been behind the improvement in mental sharpness. Oxygen intake did rise with the joggers’ test scores. Supplemental oxygen administration has been found to significantly improve memory formation in healthy young adults, as well as improving reaction time. A new analysis of 19 studies involving 586 kids, teens, and young adults that was published in the British Medical Journal found that short 10 to 40 minutes bursts of exercise led to an immediate boost in concentration and mental focus, likely by improving blood flow to the brain. These results provide further evidence that doing about 20 minutes of exercise just before taking a test or giving a speech can improve performance. Public health experts have long complained about the cutting of gym and recess time at school to make time for more academics, which could actually be having the opposite effect of impeding kids’ learning. Preliminary results from a series of studies undertaken with elementary school children do indicate a strong relationship between academic achievement and fitness scores. One study found that physically fit children identified visual stimuli faster. Brain activation patterns provided evidence that the fit children allocated more cognitive resources towards the task, as well as processing information faster.
_
Physical activity and academic performance in school-age children:
Recently, owing to the increasing importance placed on standardized testing, many schools in the United States have reduced or eliminated physical education (PE) requirements, in an effort to increase students’ academic performance. However, no empirical evidence exists to suggest that the elimination of non-academic programmes (such as PE) is related to higher academic achievement. In fact, empirical evidence suggests otherwise. Aerobic fitness has a small but positive relation to academic achievement, whereas body mass index (BMI) has a negative relation. Recent studies have indicated that achievement in standardized tests of mathematics and reading was positively related to physical fitness scores, measured using the progressive aerobic cardiovascular endurance run (PACER) test (a 20 metre shuttle run that increases in difficulty and is considered a field test of aerobic capacity), in school-age children. This relationship was selective to aerobic fitness, as muscle strength and flexibility fitness were unrelated to academic achievement. Similarly, beneficial relationships have been observed between physical activity and other measures of academic performance, such as academic grades in the classroom. Relevant neural networks have been identified for component processes that might be involved in mathematics and reading performance. Research that examined the functional neuroanatomy of reading comprehension revealed an activation of the prefrontal cortex (PFC) and parietal/posterior cingulate cortex (PCC). Likewise, mathematical calculations and numerical magnitude processing have been linked to bilateral regions of the intraparietal sulcus in children and adults. However, children also recruit the right dorsolateral prefrontal cortex. Given that both mathematics and reading elicit activation in the frontoparietal network, there is a sound basis for examining these structures in relation to academic performance. As fitness has also been related to the frontoparietal network, it would follow that children might derive benefits in school performance from increased participation in physical activity. Finally, a few studies have indicated that physical activity is unrelated to academic performance. For example, a study that relied on the self-reported teacher perception of students’ physical activity did not find a relation with academic performance. However, another study reported that pupils who engaged in vigorous physical activity performed better in school than those that performed moderate or no physical activity. Sallis et al. observed a trend for improved achievement test scores following physical activity, but the relationship might have been blunted because the school district examined was one with historically high test scores. Collectively these data indicate that, at the very least, time spent in physical activity programmes does not hinder academic performance, and it might indeed improve performance. Given the positive health benefits that are derived from physical activity, these studies support PE as an important component of children’s health and wellbeing.
_
Exercise and Children’s Intelligence, Cognition, and Academic Achievement:
Summary of findings of Prospective and Experimental Studies performed to assess the Chronic Effects of Exercise on Children’s Intelligence, Cognition, and Academic Achievement:
| Author(s) | n | Sample | Design | Exercise intervention | Duration | Tests | Results |
| Exercise and children’s intelligence | |||||||
| Corder (1966) | 8 | 12–16 years, MR | R | Balance and coordination | 20 days | WISC | Inconclusive |
| Brown (1967) | 40 | 12 years, MR | R | Strength training | 6 weeks | Stanford–Binet | Improvement |
| Ismail (1967) | 142 | 10–12 years | R | Enhanced school PE | Academic year | Vineland Otis | Improvement No effect |
| Exercise and cognition | |||||||
| Tuckman and Hinkle (1986) | 154 | 9–12 years | R | Aerobic running | 12 weeks | Perceptual-motor | No effect |
| Hinkle et al. (1993) | 42 | 13–14 years | R | Aerobic running | 8 weeks | Creativity | Improvement |
| Zervas et al. (1991) | 26 | 11–14 years | R | Aerobic exercise | 6 months | Design matching | Inconclusive |
| Davis et al. (2007) | 30 | 8–10 years | R | Aerobic exercise | 10–15 weeks | CAS: executive Non-executive | Improvement No effect |
| Exercise and academic achievement | |||||||
| Ismail (1967) | 142 | 10–12 years | R | Enhanced school PE | Academic year | SAAT | Improvement |
| Shephard et al. (1984) | 546 | First–sixth grade | NR | Enhanced school PE | Academic year | Class grades | Inconclusive |
| Dwyer et al. (1983) | ~500 | Fifth grade | NR | Aerobic exercise | Academic year | ACER GAP |
No effect No effect |
| Sallis et al. (1999) | 759 | K-fifth grade | NR | Enhanced school PE | Academic year | MAT | Inconclusive |
| Coe et al. (2006) | 214 | Sixth grade | R | Enhanced school PE | 4 months | TN | No effect |
n number of participants, MR mental retardation, R Random assignment, NR Non-random assignment, WISC Wechsler Intelligence Scale for Children, CAS Cognitive Assessment System, SAAT Stanford Academic Achievement Test, ACER Arithmetic Test Form C, GAP Reading Comprehension Test, MAT Metropolitan Achievement Test, TN Terra Nova Test
_
Similar to adults, exercise facilitates children’s executive function (i.e., processes required to select, organize, and properly initiate goal-directed actions). Exercise may prove to be a simple, yet important, method of enhancing those aspects of children’s mental functioning central to cognitive development.
_
This study shows that physically active students have higher brain activities:
_
Regular participation in physical activity and higher levels of physical fitness have been linked to improved academic performance and brain functions, such as attention and memory. These brain functions are the foundation for learning. Long-term studies have demonstrated that increases in physical activity, resulting from greater time spent in physical education, were related to improved academic performance. Even single sessions of physical activity have been associated with better scores on academic tests, improved concentration, and more efficient transfers of information from short- to long-term memory. Children participating in physical activity are better able to stay focused and remain on task in the classroom, thus enhancing the learning experience.
_
The medical journal Pediatrics published research that found kids who took part in a regular physical activity program showed important enhancement of cognitive performance and brain function. The findings, according to University of Illinois professor Charles Hillman and colleagues, “demonstrate a causal effect of a physical program on executive control, and provide support for physical activity for improving childhood cognition and brain health.” Physical activity is clearly a high-yield investment for all kids, but especially those attentive or hyperactive. The improvements in this case came in executive control, which consists of inhibition (resisting distraction, maintaining focus), working memory, and cognitive flexibility (switching between tasks). The images below show the brain activity in the group of kids who did the program as opposed to the group that didn’t. It’s the kind of difference that’s so dramatic it’s a little unsettling. The study only lasted nine months, but when you’re only seven years old, nine months is a long time to be sitting in class with a blue head.
_
Electrophysiological plots representing brain processing capacity and mental workload (P3 amplitude) during cognitive tasks that require executive control in children in the experiment and control groups. Red represents the greatest amplitude, and blue the lowest.
_
Acute aerobic exercise increases cortical activity during working memory: a functional MRI study in female college students: 2014:
There is increasing evidence that acute aerobic exercise is associated with improved cognitive function. However, neural correlates of its cognitive plasticity remain largely unknown. The present study examined the effect of a session of acute aerobic exercise on working memory task-evoked brain activity as well as task performance. Specifically, acute exercise induced increased brain activation in the right middle prefrontal gyrus, the right lingual gyrus, and the left fusiform gyrus as well as deactivations in the anterior cingulate cortexes, the left inferior frontal gyrus, and the right paracentral lobule. Despite the lack of an effect on behavioral measures, significant changes after acute exercise with activation of the prefrontal and occipital cortexes and deactivation of the anterior cingulate cortexes and left frontal hemisphere reflect the improvement of executive control processes, indicating that acute exercise could benefit working memory at a macro-neural level. In addition to its effects on reversing recent obesity and disease trends, these results provide substantial evidence highlighting the importance of promoting physical activity across the lifespan to prevent or reverse cognitive and neural decline.
_
Brain activation maps during the performance of the N-back task in the exercise session and the control session. Red areas indicate greater activation during the N-back condition relative to the resting condition.
_______
Mental health:
The evidence on the mental health benefits of physical activity is less well documented than for the physical effects – as the editors of the journal Mental Health and Physical Activity put it, in the journal’s inaugural editorial: ‘So many research questions come to mind in this field that have barely been considered.’ However, the body of evidence is growing fast, with many studies and clinical trials having shown specific benefits including: improved mood, reducing symptoms of stress, anger and depression, alleviating anxiety and slowing cognitive decline. One of the ways exercise promotes mental health is by normalizing insulin resistance and boosting natural “feel good” hormones and neurotransmitters associated with mood control, including endorphins, serotonin, dopamine, glutamate, and GABA. Much research has focused on adults, but there is evidence that among adolescents increased leisure-time physical activity (i.e. outside structured school programmes) is significantly associated with fewer depressive symptoms over a two-year period.
_
Exercise and mental stress:
_
_
Exercise is a form of physical stress. Can physical stress relieve mental stress? Alexander Pope thought so: “Strength of mind is exercise, not rest.” Plato agreed: “Exercise would cure a guilty conscience.” The “stress hormone”, cortisol, is a glucocorticoid that binds to glucocorticoid receptors. Psychological stress induces the release of cortisol from the adrenal gland by activating the hypothalamic–pituitary–adrenal axis (HPA axis). Short-term increases in cortisol levels are associated with adaptive cognitive improvements, such as enhanced inhibitory control; however, excessively high exposure or prolonged exposure to high levels of cortisol causes impairments in cognitive control and has neurotoxic effects in the human brain. For example, chronic psychological stress decreases BDNF expression which has detrimental effects on hippocampal volume and can lead to depression. As a physical stressor, aerobic exercise stimulates cortisol secretion in an intensity-dependent manner; however, it does not result in long-term increases in cortisol production since this exercise-induced effect on cortisol is a response to transient negative energy balance. Individuals who have recently exercised exhibit improvements in stress coping behaviors. Aerobic exercise increases physical fitness and lowers neuroendocrine (i.e., HPA axis) reactivity and therefore reduces the biological response to psychological stress in humans (e.g., reduced cortisol release and attenuated heart rate response). Exercise also reverses stress-induced decreases in BDNF expression and signalling in the brain, thereby acting as a buffer against stress-related diseases like depression. Exercise also promotes production of neurohormones like norepinephrine that are associated with improved cognitive function, elevated mood and learning. And that can improve thinking dulled by stressful events. Exercise forces the body’s physiological systems — all of which are involved in the stress response — to communicate much more closely than usual: The cardiovascular system communicates with the renal system, which communicates with the muscular system. And all of these are controlled by the central and sympathetic nervous systems, which also must communicate with each other. This workout of the body’s communication system may be the true value of exercise; the more sedentary we get, the less efficient our bodies in responding to stress.
_
Does Aerobic Exercise reduce Stress Responses?
Physical exercise has become increasingly popular as a leisure-time activity, in part due to its potential health benefits. In particular, physical activity has been shown to decrease the risk of cardiovascular disease. The cardioprotective effects of exercise may be due to a reduction in cardiac risk factors, such as obesity, hyperlipidemia, and hypertension. In addition, exercise may reduce cardiovascular risk by attenuating cardiovascular and neuroendocrine responses to psychosocial Stressors. It has been shown that improved aerobic fitness is associated with altered cardiovascular and sympathoadrenal functioning. Specifically, decreased heart rate at rest and during exercise, as well as decreased plasma concentrations of epinephrine and norepinephrine during exercise, result from aerobic training. It is believed that these cardiovascular and hormonal changes are related to decreased sympathetic activity and increased vagal tone following aerobic training. In addition to altering physiologic activity at rest and during physical work (i.e., exercise), it is hypothesized that exercise also may modulate cardiovascular responses to psychological stress.
_
Social exercise and stress relief:
Does exercising with another enhance the Stress-Reducing benefits of Exercise? A 2001 study:
This study sought to determine if the stress-reducing benefits of exercise are improved by exercising with others rather than alone. Results suggest that exercise with someone may be calming but more tiring due to a potential increased competition or workload.
________
Depression:
Physical exercise, particularly aerobic exercise, has pronounced long-term antidepressant effects and can produce euphoria in the short-term. Numerous systematic reviews suggest that regular aerobic exercise (at sufficient intensity and duration) has comparable antidepressant efficacy to standard pharmaceutical antidepressants in treating depression. Consequently, current medical evidence supports the use of aerobic exercise as a treatment for depression. The biomolecular basis for exercise-induced antidepressant effects is believed to be a result of increased neurotrophic factor signalling, particularly brain-derived neurotrophic factor. Continuous exercise can produce short-term euphoria, colloquially known as a “runner’s high” in distance running or a “rower’s high” in crew, through the increased biosynthesis of at least three euphoriant neurochemicals: anandamide (an endocannabinoid), β-endorphin (an endogenous opioid), and phenethylamine (a trace amine and amphetamine analogue).
___
Exercise for depression: Cochrane review 2013:
The 2013 Cochrane Collaboration review on physical exercise for depression noted that, based upon limited evidence, it is more effective than a control intervention and comparable to psychological or antidepressant drug therapies. Three subsequent 2014 systematic reviews that included the Cochrane review in their analysis concluded with similar findings: one indicated that that physical exercise is effective as an adjunct treatment (i.e., treatments that are used together) with antidepressant medication; the other two indicated that physical exercise has marked antidepressant effects and recommended the inclusion of physical activity as an adjunct treatment for mild–moderate depression and mental illness in general. One review asserted that evidence from clinical trials supports the efficacy of physical exercise as a treatment for depression over 2–4 months.
What does the evidence from the review tell us?
Exercise is moderately more effective than no therapy for reducing symptoms of depression.
Exercise is no more effective than antidepressants for reducing symptoms of depression, although this conclusion is based on a small number of studies.
Exercise is no more effective than psychological therapies for reducing symptoms of depression, although this conclusion is based on small number of studies.
The reviewers also note that when only high-quality studies were included, the difference between exercise and no therapy is less conclusive.
Attendance rates for exercise treatments ranged from 50% to 100%.
The evidence about whether exercise for depression improves quality of life is inconclusive.
_
Exercise and Anxiety:
Anxiety is “distress or uneasiness of mind caused by fear of danger or misfortune.” It is a stage of apprehension. The results of over 30 published papers substantiate an indisputable link with exercise (acute and chronic) and the reduction of anxiety. Most of the research on exercise and anxiety has been of an aerobic nature. The few studies with resistance training and flexibility have actually shown a slight increase in anxiety, but more research in this area is warranted. In regards to the actual aerobic exercise prescription, there appears to be much debate as to whether low-intensity (40-50% maximum heart rate [MHR]), moderate intensity (50-60% MHR), or high intensity (70-75% MHR) is most beneficial. The best compromise from the research suggests that exercise intensity be set at an adjustable level agreed upon by the individual in consultation with a physician (or health practitioner). It appears that even short bursts of 5 minutes of aerobic exercise will stimulate antianxiety effects. The research also indicates that those individuals training for periods of 10 to 15 weeks will receive the greatest beneficial effects.
_
Exercise and Mood State:
It appears that aerobic and anaerobic exercise can positively help effect different mood states including tension, fatigue, anger and vigor in normal and clinical populations. Mood state is affected by psychosocial, psychophysiological, and pharmacological factors that make explaining the exercise-induced mechanism quite difficult.
_
Exercise and Self Esteem:
As with the other psychological health variables, exercise has a positive connection in improving self-esteem. This link also appears to be mightier with those who have lower self-esteem. At this time, it appears that aerobic exercise may have a more pronounced effect, perhaps because there is so little research available with resistance training exercise and self-esteem. However, self-esteem is quite complex and studies suggest that certain subcomponents exist such as perceived sport competence, physical condition, attractive body, and strength, which may differ within a person. In other words, a person may highly value their physical condition and yet have a negative evaluation of their body.
_
Sleep:
A 2010 review of published scientific research suggested that exercise generally improves sleep for most people, and helps sleep disorders such as insomnia. The optimum time to exercise may be 4 to 8 hours before bedtime, though exercise at any time of day is beneficial, with the possible exception of heavy exercise taken shortly before bedtime, which may disturb sleep. There is, in any case, insufficient evidence to draw detailed conclusions about the relationship between exercise and sleep. According to a 2005 study, exercise is the most recommended alternative to sleeping pills for resolving insomnia. Sleeping pills are more costly than to make time for a daily routine of staying fit, and may have dangerous side effects in the long run. Exercise can be a healthy, safe and inexpensive way to achieve more and better sleep.
_
Learning:
Exercise increases the level of brain chemicals called growth factors, which help make new brain cells and establish new connections between brain cells to help us learn. Interestingly, complicated activities, like playing tennis or taking a dance class, provide the biggest brain boost. You’re challenging your brain even more when you have to think about coordination. Like muscles, you have to stress your brain cells to get them to grow. Complicated activities also improve our capacity to learn by enhancing our attention and concentration skills, according to German researchers who found that high school students scored better on high-attention tasks after doing 10 minutes of a complicated fitness routine compared to 10 minutes of regular activity. (Those who hadn’t exercised at all scored the worst.)
____
Creativity:
Exercise can also boost your creativity, and help you come up with new solutions to problems. For example, researchers at Stanford University found that walking can increase creativity up to 60 percent. Even a casual stroll around your office can be helpful. According to the authors: “Four experiments demonstrate that walking boosts creative ideation in real time and shortly after… Walking opens up the free flow of ideas, and it is a simple and robust solution to the goals of increasing creativity and increasing physical activity.”
____
Exercise and intelligence:
No study has ever demonstrated the impairment of intellectual performances from increases in physical activity. However, the bulk of studies show that physical activity does not increase basic intelligence, but may improve academic performance. Studies of children with mental retardation that looked at the role of physical activity in improving intelligence showed that there was no gain in intelligence scores and no improvement in academic performances. However, an improved body image was observed in children with mental handicaps when they participated in regular physical activity. A 2009 Swedish study found that – on average – young men who moved in their percentile ranking for cardiovascular fitness also moved in their percentile ranking for intelligence. In other words, changes in intelligence from age 15 to age 18 seem to track changes in fitness. A likely biological mechanism behind the observed effect relates to the impact of physical exercise on the brains plasticity (the brain’s ability to adapt new situations and environments), and one of the physiological mediators for this mechanism may be the simple fact of improved blood circulation among those who exercise more.
__
Regular exercise has many psychological and emotional benefits, too. It can help you:
•Gain confidence. Meeting exercise goals or challenges, even small ones, can boost your self-confidence. Getting in shape can also make you feel better about your appearance.
•Take your mind off worries. Exercise is a distraction that can get you away from the cycle of negative thoughts that feed anxiety and depression.
•Get more social interaction. Exercise and physical activity may give you the chance to meet or socialize with others. Just exchanging a friendly smile or greeting as you walk around your neighborhood can help your mood.
•Cope in a healthy way. Doing something positive to manage anxiety or depression is a healthy coping strategy. Trying to feel better by drinking alcohol, dwelling on how badly you feel, or hoping anxiety or depression will go away on its own can lead to worsening symptoms.
_
Exercise as ADHD Medication:
Physical movement improves mental focus, memory, and cognitive flexibility; new research shows just how critical it is to academic performance. Mental exercises to build (or rebuild) attention span have shown promise recently as adjuncts or alternatives to amphetamines in addressing symptoms common to Attention Deficit Hyperactivity Disorder (ADHD). Building cognitive control, to be better able to focus on just one thing, or single-task, might involve regular practice with a specialized video game that reinforces “top-down” cognitive modulation, as was the case in a popular paper in Nature.
_
Exercise and autism:
One of the most effective treatments for autistic people is exercise. Studies show that vigorous or strenuous exercise is associated with decreases in stereotypic (self-stimulatory) behaviors, hyperactivity, aggression, self-injury, and destructiveness. Vigorous exercise means a 20-minute or longer aerobic workout, 3 to 4 days a week; mild exercise has little effect on behavior. Many autistic children gain weight if they have an inactive life-style, and weight gain brings another set of problems. In general, exercise is important for both physical and mental health. A number of studies have shown that vigorous exercise is one of the best treatments for depression. Exercise can reduce stress and anxiety as well as improve sleep, reaction time, and memory. Since stereotypic behaviors interfere with teaching, an exercise program might improve the student’s attention in the classroom. Since exercise is inexpensive, safe, and healthful, it makes sense to try an exercise program to reduce behavior problems rather than to use more expensive and possibly harmful treatments, such as drugs.
_
Exercise and substance use disorder:
Epidemiological studies reveal that individuals who report risky substance use are generally less likely to meet physical activity guidelines (with the exception of certain population segments, such as adolescents and athletes). A growing body of evidence suggests that individuals with substance use disorders (SUDs) are interested in exercising and that they may derive benefits from regular exercise, in terms of both general health/fitness and SUD recovery. Numerous theoretical and practical reasons support exercise-based treatments for SUDs, including psychological, behavioral, neurobiological, nearly universal safety profile, and overall positive health effects. Similar to other natural rewards and addictive drugs, consistent aerobic exercise increases gene expression of the gene transcription factor that causes and maintains addiction, ΔFosB, in the nucleus accumbens; however, exercise also increases c-Fos expression as well, thereby opposing the long-term accumulation of ΔFosB. Clinical and preclinical evidence indicate that consistent aerobic exercise, especially endurance exercise (e.g., marathon running), actually prevents the development of certain drug addictions and is an effective adjunct treatment for drug addiction, and for psychostimulant addiction in particular. Consistent aerobic exercise magnitude-dependently (i.e., by duration and intensity) reduces drug addiction risk, which appears to occur through the reversal of drug induced addiction-related neuroplasticity. In particular, aerobic exercise decreases psychostimulant self-administration, reduces the reinstatement (i.e., relapse) of drug-seeking, and induces opposite effects on striatal dopamine receptor D2 (DRD2) signalling (increased DRD2 density) to those induced by pathological stimulant use (decreased DRD2 density). Consequently, consistent aerobic exercise leads to better treatment outcomes when used as an adjunct treatment for addiction.
______
Juvenile delinquency:
According to the majority of scientific studies, juvenile delinquency among athletic groups is less than that in the nonathletic population. There are some theories, proposed as an explanation. These theories include the following:
•the surplus energy theory (excess energy needs to be spent, and activity allows subjects to ‘blow off steam’);
•the stimulus-seeking theory (the excitement and thrills resulting from physical activity satisfy the increased need for stimulation); and
•the boredom theory (sport provides an alternative to occupy a time void, and by participating in physical activities, the child is too tired and too occupied to have energy left for delinquent behaviour).
Positive family interactions as a result of exercise may also be a contributing factor in explaining the reduced incidence of delinquency among physically active children and youth.
_
Character development:
Athletic competition does not appear to promote character development; instead, there are some studies that suggest that individuals with athletic experience have poorer attitudes toward fair play. Socially desirable behaviours such as friendliness, generosity and cooperation are inconsistent with physical activities that emphasize winning. However, physical activity may have the potential for personal growth in qualities including persistence, deeper self-reliance, commitment and motivation, and may increase resourcefulness. This is probably truer for noncompetitive physical activities than team competition.
_
Exercise may not help brain: a contrary study of 2015:
Exercise can help the heart, lower the risk of diabetes, keep blood pressure in check and help you maintain a healthy weight. But researchers say you shouldn’t expect it to keep your brain alert. In a study published in JAMA, Dr. Kaycee Sink, director of the memory assessment clinic at Wake Forest Baptist Medical Center and her colleagues come to the somewhat surprising conclusion that exercise doesn’t help elderly to maintain their brain function. Previous studies that found people who were more active documented less decline in mental abilities over time. And the theory behind the relationship made sense — physical activity can improve circulation and keep brain neurons nourished and fed with the nutrients they need to keep working properly. But when Sink and her team put the idea to the test with a group of 1,635 elderly, sedentary people aged 70 to 89 years, they found that exercise didn’t provide the benefits they expected for most people. The participants were randomly assigned to either a moderately vigorous exercise regimen of walking or a health education program that was interactive but didn’t involve as much physical activity. After two years, the scores on a battery of cognitive function tests for the two groups were about the same. The relationship held even after the researchers adjusted for the potential effects of other factors that could contribute to cognitive abilities. The idea that exercise doesn’t help the brain “flies in the face of conventional wisdom,” says Sink. Because the volunteers in the study were older, Sink says that the exercise may not have started early enough or lasted long enough for it to have significant effects on the brain. “We certainly can’t rule out that exercise is something that needs to start earlier,” she says. “Lifelong healthy habits are probably important.” And, she says, there are other health benefits of exercise beyond the brain. “Even though we couldn’t prove that exercising is better for the brain than attending education classes, exercise is still good for the body in m any ways,” she says. “So I would say to continue to exercise and stay physically active, but also try to stay cognitively and socially active as well.”
_____
_____
Exercise and aging:
Does Exercise slow the Aging Process?
Dating a cell’s age is tricky, because its biological and chronological ages rarely match. A cell could be relatively young in terms of how long it has existed but function slowly or erratically, as if elderly. Today, many scientists have begun determining a cell’s biological age — meaning how well it functions and not how old it literally is — by measuring the length of its telomeres. Telomeres are tiny caps found on the end of DNA strands, like plastic aglets on shoelaces. They are believed to protect the DNA from damage during cell division and replication. As a cell ages, its telomeres naturally shorten and fray. But the process can be accelerated by obesity, smoking, insomnia, diabetes and other aspects of health and lifestyle. In those cases, the affected cells age prematurely. However, recent science suggests that exercise may slow the fraying of telomeres. Past studies have found, for instance, that master athletes typically have longer telomeres than sedentary people of the same age, as do older women who frequently walk or engage in other fairly moderate exercise. But those studies were relatively narrow, focusing mostly on elderly people who ran or walked. It remained unclear whether people of different ages who engaged in a variety of exercises would likewise show effects on their telomeres. So in the new study, which was published in Medicine & Science in Sports & Exercise, researchers from the University of Mississippi and University of California, San Francisco, decided to look more broadly at the interactions of exercise and telomeres among a wide swath of Americans? To do so, they turned to the immense trove of data generated by the ongoing National Health and Nutrition Examination Survey, for which tens of thousands of adults answer questions annually about their health, including their exercise habits, and complete an in-person health exam, providing a blood sample. In recent years, those blood samples have been tested for, among other markers of health, telomere length in the participants’ white blood cells. The researchers gathered the data for about 6,500 of the participants, ranging in age from 20 to 84, and then categorized them into four groups, based on how they had responded to questions about exercise. Those questions in this survey tended to be broad, asking people only if, at any time during the past month, they had engaged in weight training, moderate exercise like walking, more vigorous exercise like running, or have walked or ridden a bike to work or school. If a participant answered yes to any of those four questions, he or she earned a point from the researchers. So, someone who reported walking received a point. If he also ran, he earned another, and so on, for a maximum of four points. The researchers then compared those tallies to each person’s telomere length. And there were clear associations. For every point someone gained from any type of exercise, his or her risks of having unusually short telomeres declined significantly. Specifically, someone who participated in a single activity, earning them a 1, was about 3 percent less likely to have very short telomeres than someone who didn’t exercise at all. That risk declined more substantially if someone exercised more. People who reported two types of exercise were 24 percent less likely to have short telomeres; three types of exercise were 29 percent less likely; and those who had participated in all four types of activities were 59 percent less likely to have very short telomeres. Interestingly, these associations were strongest among people between the ages of 40 and 65, the researchers found, suggesting that middle age may be a key time to begin or maintain an exercise program if you wish to keep telomeres from shrinking. However this study is purely associational, so cannot show whether exercise actually causes changes in telomere length, only that people who exercise have longer telomeres. Perhaps most important, the results don’t tell us whether longer telomeres translate into better health.
_____
_____
Non-health benefits of exercise:
Social Benefits
•boost self-confidence and help prevent depression
•Regular exercise can even help with the treatment of depression and anxiety
•As muscle definition is improved and body fat reduced, this can help to make you feel better about your appearance
_
Economic Benefits
•Perform better at work as you have a greater mental and physical ability
•Motivation improved leads to increased productively and efficiency
•Annual costs of physical inactivity in England to be in the region of £8.2 billion; costs of obesity alone being a further £2.5 billion.
•Sickness absence costs employers a minimum of £18 billion each year in England, which roughly equates to 16% of salary costs.
_
Exercise reduces absenteeism:
By improving your overall health, exercise can help you ward off both acute and chronic illness. You’ll get fewer colds, be less prone to the flu, and avoid the accidents or surgical interventions that can force you to take prolonged absences. In a tough economy, you need every edge you can get, and by showing up for work every day, you’ll maintain that edge over your absentee-prone non-exercising co-workers.
_
Exercise reduces exertion at work:
High physical exertion during work is a risk factor for musculoskeletal pain and long-term sickness absence. Physical exertion reflects the balance between physical work demands and physical capacity of the individual. Thus, increasing the physical capacity through physical exercise may decrease physical exertion during work. A 2014 study found that physical exercise performed at the workplace appears more effective than home-based exercise in reducing physical exertion during daily work tasks in healthcare workers.
_
The Cost of “Unfitness”:
Studies show that a lack of fitness in North American society has a severely negative economic impact. And in the United States, more than half of the $623 billion spent on health care annually went to treat preventable conditions – with at least one-quarter of the total cost reflecting adverse personal life-styles. Translated into dollars and time, the significance of inactivity, or being unfit, is staggering. According to the comprehensive California study on Economic Costs of Physical Inactivity, Obesity and Overweight (2005), the incremental cost to the employer of a physically inactive worker is $2,400/year; and $3,270 for an obese worker.
| Risk Factor Population | Incremental Incidence | Cost/Employee/Year* |
| Inactive | 50% | $2,400 |
| Obese** | 17.5% | $3,270 |
| Overweight | 35% | $515 |
*Cost: Medical 50% / Productivity 50%
**Rate of obesity is growing at 4.5% per Year
_
Exercise and happiness:
The graph above shows that the more frequent your workouts, the happier you’ll be, according to Jawbone data. The happiest people exercise six or seven days per week.
_
Exercise builds self-esteem and improves body image:
You don’t need to radically change your body shape to get a confidence surge from exercise. Studies suggest that simply seeing fitness improvements, like running a faster mile or lifting more weight than before, can improve your self-esteem and body image.
_
Does physical exercise affect demand for hospital services? Evidence from Canadian panel data: 2011:
Recent epidemiological literature shows that regular physical activity is effective in preventing several chronic diseases, and is associated with a reduced risk of premature death. The results show that physical exercise decreases the demand for hospital services, and its marginal effect decreases as physical activity increases.
_______
_______
Lack of exercise (physical inactivity):
Worldwide there has been a large shift towards less physically demanding work. This has been accompanied by increasing use of mechanized transportation, a greater prevalence of labor saving technology in the home, and less active recreational pursuits. Globally, around 31% of adults aged 15 and over were insufficiently active in 2008 (men 28% and women 34%). Approximately 3.2 million deaths each year are attributable to insufficient physical activity. In 2008, prevalence of insufficient physical activity was highest in the WHO Region of the Americas and the Eastern Mediterranean Region. In both these regions, almost 50% of women were insufficiently active, while the prevalence for men was 40% in the Americas and 36% in Eastern Mediterranean. The South East Asian Region showed the lowest percentages (15% for men and 19% for women). In all WHO Regions, men were more active than women, with the biggest difference in prevalence between the two sexes in Eastern Mediterranean. This was also the case in nearly every country. Globally, 81% of adolescents aged 11-17 years were insufficiently physically active in 2010. Adolescent girls were less active than adolescent boys, with 84% vs. 78% not meeting WHO recommendations. Some experts refer to sitting as “the new smoking” because of its negative effects on overall health. These exercise trends are contributing to the rising rates of chronic diseases including: obesity, heart disease, stroke and high cholesterol. Active transport (walking, bicycling, etc.) has been found to be inversely related to obesity in Europe, North America, and Australia. Thus exercise has been associated with a decrease in mortality.
_
Causes of lack of exercise:
_
_
Common reasons why we don’t exercise:
1. I don’t have enough time to exercise.
2. Exercise is too difficult and painful.
3. I’m too tired to exercise.
4. I’m too old to start exercising, I’m too fat, my health isn’t good enough.
5. I’m not athletic.
6. Exercise is boring.
7. I can never stick with an exercise routine long enough to reap the benefits.
_
One of the causes most prevalent in the developing world is urbanization. As more of the population moves to cities, population over-crowding, increased poverty, increased levels of crime, high-density traffic, low air quality and lack of parks, sidewalks and recreational sports facilities leads to a less active lifestyle. Physical inactivity is increasing or high among many groups in the population including: young people, women, and the elderly. A 2005 population study in south Brazil showed physical inactivity during leisure time to be more prevalent among females and those living with a partner; with a positive correlation associated with age and number of cigarettes smoked, and a negative correlation (decreased levels of physical inactivity) associated with years of formal education, body mass index, and increasing socioeconomic status. Studies in children and adults have found an association between the number of hours of television watched and the prevalence of obesity. A 2008 meta-analysis found that 63 of 73 studies (86%) showed an increased rate of childhood obesity with increased media exposure, and rates increasing proportionally to time spent watching television. Another cause in the case of children is that physical activity in activities from self-propelled transport, to school physical education, and organized sports is declining in many countries. . Barriers to physical activity include perceived lack of time, lack of resources, family obligations and embarrassment. For many, pain, injury and disability encourage sedentary behavior. A lack of energy, motivation and confidence are among the top reasons adults cite for not adopting a more physically active lifestyle.
_
Exercise varies between different socio-economic groups:
There have been some studies into why patterns of physical activity vary between different socioeconomic groups – and there are certainly intuitive reasons why this may be so, even where strong empirical evidence is lacking. For example, the streets in poorer neighbourhoods are often less safe for walking or cycling because of traffic and a perceived fear of crime. The infrastructure for active living may also not be in place in such areas: one study in the United States found that ‘moving from a community with a 1% poverty rate to a 10% poverty rate is associated with a decreased prevalence of bike paths from 57% to 9% respectively – as the area got poorer, the availability of bike paths fell dramatically. In addition, access both to attractive, safe green space and to commercial resources for structured physical activity such as gyms may be more limited in some more deprived areas.
_
Contributors to Sedentary Behavior:
The physical and social environments in which we live are changing in ways that reduce the demand for physical activity. Common behaviors that contribute to inactivity include TV viewing, computer use and electronic gaming. People of all ages are spending more time interacting with technology: the Internet, video games, cell phones and MP3 players. Drive-through windows, elevators, escalators and automation have made our lives more efficient, but less active.
______
Effects of lack of exercise:
______
How to increase physical activity?
Both, society in general and individuals can take action to increase physical activity.
_
Policies to increase physical activity aim to ensure that:
•in cooperation with relevant sectors physical activity is promoted through activities of daily living;
•walking, cycling and other forms of active transportation are accessible and safe for all;
•labour and workplace policies encourage physical activity;
•schools have safe spaces and facilities for students to spend their free time actively;
•quality physical education supports children to develop behaviour patterns that will keep them physically active throughout their lives; and
•sports and recreation facilities provide opportunities for everyone to do sports.
Policies and plans to address physical inactivity have been developed in about 80% of WHO Member States, though these were operational in only 56% of the countries in 2013. National and local authorities are also adopting policies in a range of sectors to promote and facilitate physical activity.
_
WHO response:
The “Global Strategy on Diet, Physical Activity and Health”, adopted by the World Health Assembly in 2004, describes the actions needed to increase physical activity worldwide. The Strategy urges stakeholders to take action at global, regional and local levels to increase physical activity. The “Global Recommendations on Physical Activity for Health”, published by WHO in 2010, focus on primary prevention of NCDs through physical activity. It proposes different policy options to reach the recommended levels of physical activity globally, such as:
•the development and implementation of national guidelines for health-enhancing physical activity;
•the integration of physical activity within other related policy sectors, in order to secure that policies and action plans are coherent and complementary;
•the use of mass media to raise awareness of the benefits of being physically active;
•the surveillance and monitoring of actions to promote physical activity.
• Global recommendations: physical activity for health
In 2013, the World Health Assembly agreed on a set of global voluntary targets which include a 25% reduction of premature mortality from NCDs and a 10% decrease in insufficient physical activity by 2025. The “Global Action Plan for the Prevention and Control of Noncommunicable Diseases 2013-2020” guides Member States, WHO and other UN Agencies on how to effectively achieve these targets. A sector specific toolkit is under development by WHO to assist Member States implement actions and achieve the targets. WHO has established several partnerships to help support Member States in their efforts to promote physical activity – these include the United Nations Educational, Scientific and Cultural Organization (UNESCO) and United Nations Sport for Development and Peace (UNOSPD) and a Memo of Understanding with the International Olympic Committee (IOC).
________
Public health measures to increase physical activity:
Multiple component community-wide campaigns are a popular approach to increasing the population’s level of physical activity. A Cochrane review of public health measures included 267 studies from a total of 33 countries in both high (n=25) and low/middle income countries (n=8). Many of the studies were of poor quality, although four studies were judged as trustworthy. Partnerships with local governments and non-government agencies were a popular feature, along with mass-media strategies. When the reviewers looked across all the studies, it was noticed that there was little reporting of benefit (including within the trustworthy studies). Environmental approaches appear promising: Signs that encourage the use of stairs, as well as community campaigns, may increase exercise levels. The city of Bogotá, Colombia, for example, blocks off 113 kilometers (70 mi) of roads on Sundays and holidays to make it easier for its citizens to get exercise. These pedestrian zones are part of an effort to combat chronic diseases, including obesity.
_
Active living:
Role of exercise is a way of life that integrates physical activity into your everyday routines, such as walking to the store or biking to work. Active living brings together urban planners, architects, transportation engineers, public health professionals, activists and other professionals to build places that encourage active living and physical activity. One example includes efforts to build sidewalks, crosswalks, pedestrian crossing signals and other ways for children to walk safely to and from school, as seen in the Safe Routes to School program. Recreational opportunities (parks, fitness centres etc.) close to the home or workplace, walking trails and bike lanes for transportation also encourage a more active lifestyle. Active living is a combination of physical activity and recreation activities aimed at the general public to encourage a healthier lifestyle.
_
Myth: Physical activity is needed only in industrialised countries. Developing countries have other problems.
Fact: Physical inactivity is now identified as the fourth leading risk factor for global mortality. Physical inactivity is also an independent risk factor for non-communicable diseases which caused more than 35 million deaths in 2005. Importantly, 80% of deaths from common NCDs occur in low- and middle-income countries. Therefore, non-communicable diseases associated with physical inactivity are a significant public health problem in most countries around the world. Levels of inactivity are high in virtually all developed and developing countries. In developed countries more than half of adults are insufficiently active. In rapidly growing large cities of the developing world, physical inactivity is an even greater problem. Urbanisation has resulted in several environmental factors which discourage participation in physical activity particularly in the transport and occupational domains. In rural areas of developing countries, sedentary pastimes (e.g. watching television) are also becoming increasingly popular.
______
Exercise pill:
Exercising is one of the tried and tested methods for weight loss, but recently, scientists are reportedly developing an exercise pill that can supposedly give humans almost the same benefits of physical exercise. With this new exercise pill, a lot of people would surely be interested to use it, especially those who do not want to get all sweaty and slave all over a treadmill, push-up bar or whatever workout contraption they might be already using. Having an exercise pill offering benefits of physical exercise without any physical effort seems to be too good to be true, but exercise pill is a reality and is actually a serious scientific goal and researchers have already published a major breakthrough. Although the said exercise pill is not yet in production, the major breakthrough refers to the fact that the researchers have finally discovered and created a blueprint of the molecular reactions to exercise. Scientists have discovered that physical exercise cause around 1,000 molecular changes in skeletal muscles and according to Dr. Nolan Hoffman, one of the authors of the study and research associate at Sydney’s School of Molecular Bioscience, the main goal of their research is to identify the most important changes in the body so that it can be replicated through drugs. “We’ve created an exercise blueprint that lays the foundation for future treatments, and the end goal is to mimic the effects of exercise,” Dr. Hoffman says. “It’s long been thought that there were many signals elicited by exercise, but we were the first to create this map and we now know the complexity,” he added. As of now, the researchers are working on identifying the most significant biological changes because the blueprint is said to be incredibly complicated. Further, the results are still under analysis because no drug exists that could safely replicate the effects of physical exercise. Despite the science behind it, Ismael Laher, a professor at the University of British Columbia and co-author of a second study about the subject, noted that the exercise pill, if ever one is created, should not be considered as a magical drug that can completely replace the benefits of being physically active. In other words, it will not be as effective as actual physical exercise paired with a healthy diet. But, for those who cannot engage in traditional exercise routines such as stroke victims and amputees, this type of pill could help them remain physically fit. Exercise requires your heart rate to go up, blood to flow faster, and you cannot do that with an exercise pill…but in particular groups, it’s the next best thing. At first glance, this can seem like the greatest idea ever, but critics would say just the opposite: This could be a gateway to promoting the worst possible attitude people could have about exercise. An ‘exercise pill’ would be a perversion of science and a prescription for the promotion of unhealthy lifestyles.
________
________
Harms of exercise:
_
Most people believe that all exercises are good, safe and effective. The truth is that some common exercises aren’t safe at all (especially for people who have muscle, joint, and health problems). Certain exercises require a bit more know-how than the average person possesses. And other exercises are downright wastes of your time. What you should do—or avoid—depends on your goals, fitness level, health history, workout schedule, and other personal issues. An article like this can’t replace your own efforts to identify your goals and needs. That requires you to do some research on your own, talk to your medical professional about any pain or physical limitations you have, and learn how to exercise with proper form and technique.
What makes an exercise risky? Here are a few red flags to look out for:
Any unusual or “unnatural” movement pattern in the exercise
Any movement that causes pain or discomfort in any way
Any movement that enhances muscular imbalances that are already present
Any movement that requires joint flexibility that is above and beyond your range of motion
Any exercise with risks of injury that outweigh the potential benefit of the exercise itself
_
Costly fitness mistakes that could harm your body:
1. Forgetting the basics:
Eating, breathing and stretching are three basics that work together to keep you safe before, during and after your workout. Large meals are best avoided before a workout – better to snack on fresh fruit, energy bars or yoghurt. Remember to drink water before, during and after your workout Warming up means warming up your muscles, ready for a workout – as opposed to relaxing them, such as by massage. The wrong kind of stretching can include stretching from the waist, which can put unnecessary strain on your back. It’s better to put your foot on an elevated surface, and then lean over to stretch the hamstrings. Yoga is also good for all-over stretching.
2. Right routine, wrong time:
Sometimes, do basic exercises such as lunges feel wrong for you?
A basic pre-exercise assessment from a fitness professional will determine your current fitness level, your bio-mechanical efficiency and your exercise needs. You’ll get a schedule of the best exercises for you and great results from your workout.
3. Ignoring your pain:
Pain is an important warning sign, not an indication that you’re doing well. Enthusiasm can lead you to do too much, too soon, particularly when you start a new workout or fitness class. Pain protects us from potential serious injuries, so take heed when it happens in your workout – and stop.
4. Repetition:
Doing the same exercise over and over again might make you very good at that one thing – but it can also lead to overuse injury. That could mean you end up with problems with muscle imbalance or weakness, and even alignment problems. Varying your exercise training routine is the answer.
5. Poor technique:
Don’t hold on to the treadmill, whether you’re walking or running. That poor technique affects your natural posture – and can lead to some bad muscle strain. A skilled fitness professional will show you the right technique and make exercise fun as well as correct.
6. Too much weight:
Short, intense workouts are designed to get fast results, especially in building strength and power. However, incorrect lifting of heavy weights will hurt you, while incorrect jumping technique can lead to serious injury to knees or Achilles tendons. Improper coaching and overtraining can multiply the problem. If you decide to do these extreme workouts, then choose a professional fitness trainer who can make sure you’re doing it correctly, and keeping safe from injury.
7. Aim to be well rounded:
Doing any exercise to exhaustion levels is unnecessary, and may even be dangerous. A well-rounded exercise routine should include various components, including strength, low-level aerobics, and interval training. Aim for an exercise programme that will accomplish your fitness goals without unnecessary fatigue.
8. Forgetting to stop:
This idea might seem counter to all the hard work you’re putting into your healthy workout, but do remember to take a rest – at least one day a week. Your body needs time to recover. Respect your body and what it can do.
_
Risks of Exercise:
As can be seen from the foregoing discussion, regular participation in an exercise program can provide several benefits. Yet exercise is similar to other medical or health interventions in that there are also potential costs associated with the activity. These costs range from minor inconveniences, such as time taken up by exercise, to more serious complications, including injury and even sudden death.
_
Exercise and injury:
Overall, available information suggests that physical activity in the range recommended by recent public health guidelines, such as the CDC/ACSM guideline, has quite an acceptable risk-to-benefit ratio. The most common risk of physical activity in adults is musculoskeletal injury. The incidence of injury can be as high as 55% in 8 weeks among women undergoing US Army basic training. In contrast, injuries are rare in research studies of supervised exercise training among older adults when individuals at high risk of injury are excluded. In a cohort study of community adults aged 20 to 85 years with above-average activity levels, 25% reported a musculoskeletal injury over 1 year, and one third of injured adults stopped exercising. The best available studies on injury rates suggest that about 25 to 30 percent of adult runners will become injured over the course of a year, if injury is defined as an incident that causes an individual to stop exercising for at least one week. If only more serious injuries, such as those for which the individual seeks medical care, are considered, injury rates are much lower, perhaps in the range of 1 percent per year. Several factors affecting injury risk are modifiable and offer opportunities for risk management. Risk of injury increases with obesity, volume of exercise, and participation in vigorous exercise such as competitive sports, whereas higher fitness, supervision, stretching exercises, protective equipment such as bike helmets, and well-designed environments protect against injury. The general principle that the volume of physical activity should be increased gradually over time is widely regarded as critical for reducing injury risk. Walking, the most popular activity and the standard example of a moderate-intensity activity, is a low-risk activity. One study reported that increasing the duration of walking did not result in any increase in injury risk. In some situations, regular physical activity actually reduces injury risk, as indicated by a recent consensus statement that physical activity is recommended to reduce the risk of fall injuries in older adults. While one set of joints and muscles may have the tolerance to withstand multiple marathons, another body may be damaged by 20 minutes of light jogging. This must be determined by each individual.
_
Take these steps to prevent injury:
•If you’re not active at all or have a health problem, start your program with short sessions (5 to 10 minutes) of physical activity and build up to your goal. (Be sure to ask a doctor before you start if you have a health problem.)
•Use safety equipment such as a helmet for bike riding or supportive shoes for walking or jogging.
•Start every workout with a warm-up. If you plan to walk at a brisk pace, start by walking at an easy pace for 5 to 10 minutes. When you’re done working out, do the same thing until your heart rate returns to normal.
•Drink plenty of fluids when you are physically active, even if you are not thirsty.
•Use sunscreen when you are outside.
•Always bend forward from the hips, not the waist. If you keep your back straight, you’re probably bending the right way. If your back “humps,” that’s probably wrong.
•Stop your activity if you feel very out of breath, dizzy, nauseous, or have pain. If you feel tightness or pain in your chest or you feel faint or have trouble breathing, stop the activity right away and talk to your doctor.
Exercise should not hurt or make you feel really tired. You might feel some soreness, a little discomfort, or a bit weary. But you should not feel pain. In fact, in many ways, being active will probably make you feel better.
_
Exercise and sudden death:
Vigorous physical activity acutely increases the risk of sudden cardiac death and myocardial infarction among individuals with both diagnosed and occult heart disease. A variety of congenital and acquired conditions such as hypertrophic cardiomyopathy, coronary artery anomalies, aortic stenosis, and cardiomyopathies are associated with sudden death during vigorous activity in children and young adults. Recommendations for athletic screening and participation for these conditions have been presented in the AHA Statement on Cardiovascular Preparticipation Screening of Competitive Athletes. During exercise, there is a transient increase in the risk of having a cardiac-related complication (for example, a heart attack or serious heart rhythm disorder). However, this risk is extremely small. For adults without existing heart disease, the risk of a cardiac event or complication ranges between 1 in 400000–800000 hours of exercise. For patients with existing heart disease, an event can occur an average of once in 62000 hours. Among high school and college athletes, an estimated 1 death per year occurs during or within an hour after athletic activity for every 133333 male and 769230 female participants. Importantly, the risk of a cardiac event is significantly lower among regular exercisers. Evidence suggests that a sedentary person’s risk is nearly 50 times higher than the risk for a person who exercises about 5 times per week. Stated simply, individuals who exercise regularly are much less likely to experience a problem during exercise. Moreover, contrary to popular view, the majority of heart attacks (approximately 90%) occur in the resting state, not during physical activity. Exercise is therefore considered to be extremely safe. Nevertheless, it is a good idea to be aware of the warning signs or symptoms that may indicate a problem: chest discomfort (pain or pressure in the chest, jaw, or neck, possibly radiating into the shoulder, arm, or back), unusual shortness of breath, dizziness or light-headedness, and heart rhythm abnormalities (sensations of heart beat skipping, palpitations, or thumping). If one of these symptoms occurs, medical attention should be sought immediately. High dose anabolic steroids and products containing ephedra have been associated with cases of stroke, heart attack, and even death.
_
Although the absolute incidence of sudden death associated with exercise is quite low, exercise does acutely increase the rate of sudden death compared with more leisurely activities. Exercise also transiently increases the risk of acute myocardial infarction. Approximately 5% to 10% of myocardial infarctions are associated with vigorous physical activity. The relative risk of both exercise-related myocardial infarction and sudden death is greatest in individuals who are the least physically active and who were performing unaccustomed vigorous physical activity. Sedentary adults should avoid isolated bouts of unaccustomed vigorous physical activity and should follow the standard recommendation to increase physical activity levels gradually over time. The possible value of this strategy is supported by the observation that the risk of exercise-related cardiac events is greatest in the least active individuals. Because atherosclerotic CAD is the most frequent cause of exercise-related events, the incidence of such events is higher among patients with known atherosclerotic coronary disease. Among participants in cardiac rehabilitation programs, the average incidence of cardiac arrest, nonfatal myocardial infarction, and death is 1 for every 117000, 220000, and 750000 patient-hours of participation, respectively. The low ratio of cardiac arrest to death is due to the availability of acute medical care.
_____
Dehydration and Exercise: a dangerous combination:
Do you want to make the most of your workouts? Drinking plenty of water is a necessity for both performance and safety during exercise. On a basic level, even slight dehydration can cause decreased physical and mental capability, which can reduce the benefits of your workout. Yes, drinking too little water can make you feel thirsty, but it can also cause dizziness, light-headedness, lack of energy, and muscle cramping. Severe dehydration can lead to heat exhaustion, heat stroke, seizures, and even death. Exercise creates an increase in body temperature, which is cooled by sweating. If your body isn’t properly hydrated, it is not able to properly cool itself. Exercising outside in extreme heat? Even more dangerous without enough fluid intake! Fluids help with muscle contraction and blood flow – two things necessary for your body to receive the full benefits of physical activity. Even physical activity such as swimming requires proper hydration, even if you do not feel hot or thirsty. If you are working out, chances are your body will need a bit more fluid than daily requirement. The best way to ensure proper hydration is to drink plenty of fluids not only during the workout, but also before and after any physical exercise. Drinking a few glasses of water several hours before exercise allows your body to absorb the fluid and prepare itself for the upcoming stress. Drinking water during exercise helps maintain a safe body temperature, and drinking water after helps your muscles recover. If you will be working out for more than an hour, you may want to drink fluids that replace electrolytes (i.e. sports drinks). What is the easiest way to check for dehydration? Check the color of your urine! A darker color can mean that you aren’t getting enough water, whereas a light yellow to clear urine usually means that you are properly hydrated. Another way to tell of you are depleting your fluid levels during exercise is to weigh before and after your workout. If your weight is less after, then you need to increase your fluid intake. Exercise is a critical component of excellent overall health, and water is a necessary fuel for your body during exercise. Water also has other benefits beyond merely hydration, such as making it easier to maintain a healthy weight, helping digestion, and can even contribute to clearer skin. So grab your water bottle and drink to your health!
_
Exercise produces heat. Prevention of overheating occurs by transfer of heat to the skin by vasodilation of the cutaneous circulation, and by the cooling effect of evaporation of sweat. Exercise causes body fluid losses from moisture in exhaled air as well as from sweating. Although sweat rates are highest under conditions of high-intensity exercise in heat and high humidity, total fluid losses can be appreciable in very prolonged events, whatever the conditions. Sweat rates of 2 to 3 litres/hour can be expected during short periods of hard exercise in the heat, and an excess of 1.5-2 litres/hour during endurance events. Even in cooler conditions losses are appreciable. During a football game on a cool day (10 deg. C), players can lose up to two litres of sweat, and runners are estimated to lose around 1.2 litres/hour at 6 minute/mile pace on a cool, dry day (double this amount on a hot, humid day). Additionally, fluid is lost via moisture in exhaled air. Except in extreme circumstances, blood Na levels are maintained during exercise. Sweat is mainly composed of water, and Na losses in sweat represent a small fraction of total body content and are readily replaced afterwards by normal food. Unless fluid losses are replaced by drinks, sweating causes progressive depletion of circulating blood volume, commonly called dehydration and a thickening of blood (increased viscosity). This places a strain on the cardiovascular system, with a rise in heart rate in order to maintain adequate blood flow to exercising muscles and vital organs. As blood volume depletes, blood flow to the skin is reduced. As a result, sweating decreases and heat dissipation from the skin is impaired, causing body core temperature to rise, potentially leading to heat stress, collapse and even death. Even low levels of dehydration have physiological consequences. A loss of 2% bodyweight (just 1kg for a 50kg person) causes an increase in perceived effort and is claimed to reduce performance by 10-20%. A fluid loss exceeding 3-5% bodyweight reduces aerobic exercise performance noticeably and impairs reaction time, judgement, concentration and decision making – vital elements in all sports, from pole-vaulting to football. A particular issue for boxers is that dehydration increases risk of brain injury.
_
Exercise-induced nausea:
Exercise-induced nausea is a feeling of sickness or vomiting which can occur shortly after exercise has stopped as well as during exercise itself. It may be a symptom of either over-exertion during exercise, or from too abruptly ending an exercise session. People engaged in high-intensity exercise such as aerobics and bicycling have reported suffering from exercise-induced nausea. Lack of hydration during exercise is a well-known cause of headache and nausea during exercise. Exercising at a heavy rate causes blood flow to be taken away from the stomach, causing nausea. Another possible cause of exercise induced nausea is overhydration. Drinking too much water before, during, and/or after extreme exercise (such as a marathon) can cause nausea, diarrhea, confusion, and muscle tremors. Excessive water consumption reduces or dilutes electrolyte levels in the body causing hyponatremia.
____
Frostbite in cold weather:
Precautions are also necessary in cold weather. When exercising in winter, dress in layers, including gloves and socks, which create insulated air pockets that trap heat. In cold weather, wear shoes with less ventilation than those worn in the summer. Fingers, toes, ears, and nose are most susceptible to frostbite. Frostbite progresses from stinging or aching to numbness. Fingers and toes may become white. Soaking the hands and feet in warm water can help, but only once there is no risk of refreezing, since a second bout of frostbite after thawing can quicken tissue damage.
_
Exercise can break up families:
In 2010, The Wall Street Journal published the article “A Workout Ate My Marriage”, describing how couples become increasingly conflicted as a spouse becomes obsessed with a particular exercise goal, such as extreme weight loss or an Ironman triathlon – to the detriment of time spent with family. Often, since the exercise goal can be justified as “noble”, it is difficult for a spouse or family member to negotiate with the over-exerciser to spend more time with family. If your goals require you to exercise “excessively”, then at least attempt to include family in exercise. Join a gym with free childcare so you and the spouse can exercise together, get a jogging stroller and bicycle trailer, and train indoors with the kids at home so a spouse can go enjoy free time.
_
Exercise is associated with body perception disorders:
Body dysmorphic disorder is a psychological disorder in which you are excessively concerned about a perceived defect in your physical features, such as your arm or leg muscles being too small or your waistline not being thin enough. This can result in heavy, often socially isolated exercise to “repair the defect”. Typically, this type of activity can begin in adolescence or early adulthood, but can stay with you your entire life as you strive to achieve or maintain the “perfect body”. You may turn to bodybuilding, marathoning, cycling or any other activity which uses the same muscles over and over again to try to hammer away at your perceived defects, even when it comes to the detriment of your joints or health. If you don’t have the time to exercise and address what you perceive to be a significant body issue, this can result in depression, social anxiety, and even social phobia, or complete avoidance of being in public, especially where your body might be exposed. Often, you might justify your behavior by believing that you are a serious athlete who can never work too hard or too long at your sport, and this can often lead to excessive and addictive exercise in an attempt to control or lose weight, or sometimes to gain muscle or “sculpt” a body part.
_
Stopping regular exercise suddenly can also create a change in mood. Feelings of depression and agitation can occur when withdrawal from the natural endorphins produced by exercise occurs. Exercise should be controlled by each body’s inherent limitations.
_
Exercise intolerance:
Exercise intolerance is a condition of inability or decreased ability to perform physical exercise at the expected level or duration of someone with a specific physical condition. It also includes experiences of unusually severe post-exercise pain, fatigue, nausea, vomiting or other negative effects. Exercise intolerance is not a disease or syndrome in and of itself, but a primary symptom of chronic diastolic heart failure. In most cases, the specific reason that exercise is not tolerated is of considerable significance when trying to isolate the cause down to a specific disease. Dysfunctions involving the pulmonary, cardiovascular or neuromuscular systems have been frequently found to be associated with exercise intolerance, with behavioural causes also playing a part in it.
_________
________
Over-exercise (excessive exercise/ overtraining):
Overtraining means the intensity or volume of training exceeds the body’s capacity to recover between bouts. Working out more than two hours a day may be a sign of excessive exercise. Limit vigorous exercise to 30- to 50-minute sessions per day to avoid stressing your cardiovascular system. One hour sessions are enough for weight training; going beyond that can bring on catabolism, which can cause muscle breakdown. Runners should keep it to no more than 10 to 15 miles per week to protect their hearts.
_
Exercise is a stressor and the stresses of exercise have a catabolic effect on the body – contractile proteins within muscles are consumed for energy, carbohydrates and fats are similarly consumed and connective tissues are stressed and can form micro-tears. However, given adequate nutrition and sufficient rest to avoid overtraining, the body’s reaction to this stimulus is to adapt and replete tissues at a higher level than that existing before exercising. The results are all the training effects of regular exercise: increased muscular strength, endurance, bone density, and connective tissue toughness. Too much exercise can be harmful. The body parts exercised need at least a day of rest, which is why some health experts say one should exercise every other day or 3 times a week. Without proper rest, the chance of stroke or other circulation problems increases, and muscle tissue may develop slowly. It has also been noted by the medical field that expectant mothers should never exercise two days consecutively. Inappropriate exercise can do more harm than good, with the definition of “inappropriate” varying according to the individual. For many activities, especially running, there are significant injuries that occur with poorly regimented exercise schedules. In extreme instances, over-exercising induces serious performance loss. Unaccustomed overexertion of muscles leads to rhabdomyolysis (damage to muscle) most often seen in new army recruits. One sign of Overtraining Syndrome (OTS) is suppressed immune function, with an increased incidence of upper respiratory tract infection (URTI). An increased incidence of URTIs is also associated with high volume/intensity training, as well as with excessive exercise (EE), such as in a marathon.
_
Seven Signs you may be overdoing it:
The article by personal trainer Jennipher Walters addresses signs of overtraining that are commonly overlooked or misdiagnosed. The following seven symptoms may signal that you need to cut back a bit and allow your body to recover between sessions:
1. Exercise leaves you exhausted instead of energized.
2. You get sick easily (or it takes forever to get over a cold)
3. You have the blues
4. You’re unable to sleep or you can’t seem to get enough sleep
5. You have ”heavy” legs
6. You have a short fuse
7. You’re regularly sore for days at a time
_
Overtraining:
It is important to note the difference between overtraining and over-reaching; over-reaching is when an athlete is undergoing hard training but with adequate recovery, overtraining however, is when an athlete is undergoing hard training without the adequate recovery. Overtraining can lead to exercise addiction which can lead to negative physiological and psychological effects.
_
Some Effects of Excessive Exercise:
•You are prone to injuries- When you exercise excessively your body is prone to injuries. Your body needs rest too. If you exercise a lot, then it leads to strained ligaments and tendons. This put your bones at the risk of fractures. Too much exercise can also harm your body tissues. So you need to exercise only so much, which your body can support.
•Muscle Mass- You tend to lose muscle mass and your body becomes nutrition deficient. You curb your body’s need of nutrition by excessive exercise and diet.
•Weakened Immune System- When you exercise a lot your body’s immune system weakens. You get more prone to viruses and colds. Exercise affects your body and leaves it exhausted. Your body pains and your weakened immune system are not efficient enough to kill bacteria or other illness.
•Cessation of Menstrual Cycle- Studies show that female athletes who face rigorous training experience Amenorrhea and if it persists for long, then it is difficult to cure. Other factors like changes in diet, excessive weight loss and stress can also cause amenorrhea.
•Eating Disorders- People who are exercise addicts and just have weight loss in mind, are prone to eating disorders. So, such people may face eating disorders like bulimia and anorexia can be caused due to exercise addiction.
•Sleeping Disorders- You face this problem because your body feels very tired, lethargic and drained out. Everything seems heightened and your body pains because of excessive exercise.
_
Excessive exercise and heart damage:
Exercisers who train chronically to compete in marathons, triathlons, and other long-distance events may be hurting their heart health. Chronic extreme endurance efforts, like marathons, ultra-marathons, and long-distance triathlons, can cause cardiovascular damage over time. Healthier exercise patterns involve not such extreme duration or intensity. Researchers found that running at moderate speeds was linked with a lower risk of death from any cause compared to no running. More intense running didn’t yield additional benefit. Evidence about the ill effects of chronic training for extreme endurance events is accumulating. An evolving body of data indicates that chronic training for, and participation in, extreme endurance events ”can cause dilation and stretching of the heart’s chambers, especially the atria and right ventricle”. The pumping ability of the right ventricle can be reduced. Blood indicators (biomarkers) that reflect damage to the heart muscle can increase. These changes usually return to normal within about a week. However, if the training is chronic, it may lead to scarring, enlargement, and stiffening of the heart. There is a risk, too, of developing abnormal heart rhythms such as atrial fibrillation. In a 2012 study in the European Heart Journal researchers compared 102 healthy male runners, aged 50 to 72, to 102 men who did not run. Each runner had done at least five marathons in the last three years. About 12% of the marathon runners had heart scarring. It was three times more common in them than in the comparison group. During a two-year follow-up, the marathoners were more likely to have a heart attack or other heart or stroke-related problem. Additionally, long-term excessive sustained exercise may be associated with coronary artery calcification, diastolic dysfunction, and large-artery wall stiffening. A 2011 German study revealed a very high incidence of carotid and peripheral atherosclerosis among male marathon runners. An autopsy released after the recent death of legendary long-distance runner Micah True found he had cardiomyopathy. In the condition, the heart becomes enlarged, thick, or rigid.
_
Scientific studies showing heart damage due to excessive exercise:
1. A 2006 study screened 60 non-elite participants of the 2004 and 2005 Boston Marathons, using echocardiography and serum biomarkers. Researchers found decreased right ventricular systolic function in the runners, caused by an increase in inflammation and a decrease in blood flow.
2. A 2010 study presented by the American College of Cardiology showed that endurance runners have more calcified plaque in their arteries (which also increases stroke and dementia risk) than those who are not endurance athletes.
3. According to a study presented at the Canadian Cardiovascular Congress 2010 in Montreal, regular exercise reduces cardiovascular risk by a factor of two or three, but the extended vigorous exercise performed during a marathon raises your cardiac risk seven-fold!
4. In a 2011 study published in the Journal of Applied Physiology, researchers recruited a group of extremely fit older men, all members of the 100 Marathon club (having completed a minimum of 100 marathons). Half of the men showed heart muscle scarring as a result of their endurance running—specifically, the half who had trained the longest and hardest. If running marathons provided cardiovascular benefit, this group would have had the healthiest hearts!
5. A 2011 rat study published in the journal Circulation was designed to mimic the strenuous daily exercise load of serious marathoners over the course of 10 years. All the rats had normal, healthy hearts at the outset of the study, but by the end, most of them had developed “diffuse scarring and some structural changes, similar to the changes seen in the human endurance athletes.
_
Excessive exercise causes oxidative stress:
Endurance exercise can increase oxygen utilization to over 10 to 20 times the resting state, and all this extra oxygen consumption then increases production of free radicals, which are produced as the oxygen is used to convert energy into ATP for muscle contractions. Oxidative stress from free radicals damages cellular proteins, membranes and genes and leads to a state of chronic, systemic inflammation. Chronic inflammation is implicated in diseases such as cancer, heart disease, strokes, Alzheimer’s, Parkinson’s and premature aging; the same diseases exercise is supposed to prevent.
_
Excessive exercise causes hormonal imbalance:
The adrenal glands are two thumb-sized glands sitting atop your kidneys. They produce hormones like norepinephrine, cortisol and DHEA, which allow your body to respond and make adjustments to physical or emotional stress. If the intensity and frequency of the stress becomes too great, then the adrenal glands can begin to become exhausted, and the hormones that they produce can become depleted, resulting in serious imbalances that can cause issue like estrogen dominance in women or testosterone deficiencies in men. The end result is a tired, chronically fatigued individual who has disrupted sleep, low libido, worn-out looking eyes, a set and stressed jawline, and a “skinny fat” body look no matter how much exercise they do.
_______
_______
Exercise addiction:
The upcoming Diagnostic and Statistical Manual of Mental Disorders (DSM-5) include behavioral addictions. Although gambling will be the only designated behavioral addiction, this new diagnostic nomenclature will no doubt lead to increased research into all forms of excessive behavior, such as exercise, that have been considered to be addictive. This research will require a clear description of exercise addiction as distinct from a healthy habit. As with other behavioral addictions, it will also be necessary to distinguish exercise addiction from compulsions and impulse control disorders. An understanding of common co-occurring disorders will also be important to the extent that they mask exercise addiction and/or complicate treatment.
_
Defining Exercise Addiction:
What distinguishes the everyday gym enthusiast from someone addicted to exercise?
Would we consider an elite athlete training for the Olympics as having an exercise addiction?
Hausenblas and Downs identify exercise addiction based on the following criteria:
•Tolerance: increasing the amount of exercise in order to feel the desired effect, be it a” buzz” or sense of accomplishment;
•Withdrawal: in the absence of exercise the person experiences negative effects such as anxiety, irritability, restlessness, and sleep problems;
•Lack of control: unsuccessful at attempts to reduce exercise level or cease exercising for a certain period of time;
•Intention effects: unable to stick to one’s intended routine as evidenced by exceeding the amount of time devoted to exercise or consistently going beyond the intended amount;
•Time: a great deal of time is spent preparing for, engaging in, and recovering from exercise;
•Reduction in other activities: as a direct result of exercise social, occupational, and/or recreational activities occur less often or are stopped;
•Continuance: continuing to exercise despite knowing that this activity is creating or exacerbating physical, psychological, and/or interpersonal problems.
Although others have defined exercise addiction using different models, the above definition is most closely aligned with the DSM-5 criteria for behavioral addiction which will be modelled after those for substance dependence. Based on a review of a wide range of studies on exercise addiction, Sussman, Lisha, and Griffiths estimate the prevalence in the general population to be close to 3%. Among certain groups such as ultra-marathon runners and sport science students the figure is even higher. According to Lejoyeux, Avril, Richoux, Embouazza, and Navoli, 42% of the members at a Parisian fitness club met criteria for exercise addiction.
_
Five indicators of exercise addiction are:
1. An increase in exercise that may be labelled as detrimental, or becomes harmful.
2. A dependence on exercise in daily life to achieve a sense of euphoria; exercise may be increased as tolerance of the euphoric state increases.
3. Not participating in physical activity will cause dysfunction in one’s daily life.
4.Withdrawal symptoms following exercise deprivation including anxiety, restlessness, depression, guilt, tension, discomfort, loss of appetite, sleeplessness, and headaches.
5. High dependence on exercise causing individuals to exercise through trauma and medical conditions.
_
There is a fine line between a healthy habit and an addictive obsession. The phrase ‘healthy obsession’ is really an oxymoron, since obsession is arguably a pathological disease state of the mind, therefore not healthy. Definitions for obsession range from compelling motivation to compulsive preoccupation. However you want to label it, obsession relates to an altered state of consciousness in which the need or compulsion to do a certain act overpowers all else, becoming a priority over all other needs and obligations in a person’s life. When exercise becomes the obsession, the risk of dependence is lurking nearby. You may have heard of the so called, ‘runner’s high,’ which presents as a euphoria from the natural opioid-like chemicals, endorphins, released in the brain during exercise. Another theory proposed to explain the euphoric mechanism has to do with catecholamine release, which directly controls mood, attention, movement, and the body’s endocrine/cardiovascular responses to stress. Key differences between healthy and addictive levels of exercise include the presence of withdrawal symptoms when exercise is stopped as well as the addictive properties exercise may have leading to a dependence on exercise.
_
According to Modolo et al., compulsive athletes report four components of addiction:
1) feeling euphoria,
2) the need to increase the dose of exercise to obtain feelings of well-being (tolerance),
3) difficulties in the performance of professional or social activities (rearrangement of priorities) and
4) symptoms of the absence or need, including depression, irritability, and anxiety, when unable to engage in the activity (withdrawal).
This 2011 study also found a direct relationship between the intensity of exercise and the severity of withdrawal symptoms. The time spent preparing for, engaging in, and recovering from workouts and the continuance despite exacerbating physical, psychological, and/or interpersonal problems are two more signs that a healthy habit has turned into a neurotic addiction. More negative characteristics include low self-esteem, the use of exercise as management or manipulation of psychological states, increasing body dissatisfaction, and chronic vulnerability to overtraining injuries. The physical manifestations of exercise dependence have been most documented in distance runners; persistent soft tissue injuries (sprains and strains), stress fractures, pressure sores, gastrointestinal blood loss and iron-deficiency anemia just name a few. From a genetic standpoint, asymmetry in the brain has been correlated to negative emotions. One study in particular found a relationship between frontal lobe brain asymmetry and exercise addiction, implying that exercise directly activates and alters the part of the frontal lobe responsible for affect and mood, thereby improving negative emotions. There are often feelings of guilt associated with the absence of or inability to exercise for even one day, and dieting to improve performance is common. It should be noted that there is a strong risk and link between eating disorders and excessive exercise, since it is often the primary means of weight loss. It is important to distinguish one from the other, usually by analyzing the motive for exercise and other associated symptoms that may point toward the diagnosis of an eating disorder.
_
Causes of exercise addiction:
Exercise addiction is thought to be related to the euphoric feelings resulting from the rapid release of endorphins that occurs during intense bouts of exercise. Although the evidence is not conclusive, there is a high correlation between exercise addiction and endorphins. Endorphins work by activating opiate receptors in the brain causing pain relief and are also correlated with causing euphoric feelings. The decrease of pain and increase in euphoric feelings creates a positive feedback loop associated with exercise which is thought to be a cause of addiction. This feedback loop also helps to explain why intensity of exercise increases over time with exercise addiction. For individuals who exercise more frequently the effects of endorphins are decreased. A person with an exercise addiction will need to increase the frequency, intensity, and/or time of exercising to reach the desired euphoric feelings. Biological studies show that in rodents, exercise such as wheel running activates the dopamine reward system and thus contributing to stress reduction. Further evidence suggests that running is associated with endorphins and cannabinoids thus explaining the “runners high” or euphoric feelings that may lead to exercise addiction. Genetic studies suggest that genes which control preference for drugs also control the preference for naturally rewarding behaviors such as exercise. Psychological studies also explain exercise addiction in terms of reward, habituation, social support, stress-relief, avoidance of withdrawal and reduction of anxiety.
_
Treatment of exercise addiction:
Treatment for exercise addictions and activity disorders is often similar to that for men and women with eating disorders, especially if they coexist. Depending on the other issues at hand, it may require an inpatient treatment program and medical attention. Therapists and counsellors can work on the person on his or her underlying issues and help with the achieving of peace of mind and body. When it comes to treating this addiction, abstinence from exercise may not be the required goal. Because exercise in moderation is considered a healthy habit, a typical treatment goal will be to return to moderate exercise. In some cases, a new form of exercise may be recommended; the runner becomes a swimmer. In other cases the person may continue to do the same form of exercise in a more controlled or moderate manner. Whether moderating the original exercise behavior or replacing one activity with another, clinicians can use the attributes of the four phases of addiction as a way to help patients distinguish problematic or addictive exercise from moderate or recreational exercise.
______
_____
Now let me discuss few ground breaking studies:
__
Lack of exercise is a global pandemic, according to The Lancet: 2012:
According to a recent study published in The Lancet, lack of exercise has become a global pandemic, causing nearly a tenth of all deaths worldwide. What is most alarming about the study is that lack of exercise is killing roughly the same number of humans as smoking. The new research covered 122 nations representing 89% of the world’s population. About 5.3 million of the 57 million deaths worldwide in 2008 could be attributed to inactivity, the new report estimates, largely due to four major diseases: heart disease, Type 2 diabetes, breast cancer and colon cancer. The study finds that if physical inactivity could be reduced by just 10%, it could avert some 533,000 deaths a year; if reduced by 25%, 1.3 million deaths could be prevented. Say we got everyone off the couch and eliminated inactivity altogether: the life expectancy of the world’s population would rise by about 0.68 years (more, if you discount those who were already active), comparable to the effect of doing away with smoking or obesity. Though nearly 3 out of 4 countries that are members of the World Health Organization have national plans to tackle inactivity, only 42% of those plans are funded and operational, another Lancet study found.
______
Lack of Exercise more deadly than Obesity: a 2015 study:
Being sedentary may be twice as deadly as being obese, a new study suggests. However, even a little exercise — a brisk 20-minute walk each day, for example — is enough to reduce the risk of an early death by as much as 30 percent. Efforts to encourage small increases in physical activity in inactive individuals likely have significant health benefits. The risk reduction was seen in normal weight, overweight and obese people. Authors estimated that eradicating physical inactivity in the population would reduce the number of deaths twice as much as if obesity was eradicated. The message from this study is clear and simple — for any given body weight, going from inactive to active can substantially reduce the risk of premature death. For the study, researchers collected data from 334,000 men and women. Over an average of 12 years of follow-up, they measured height, weight, waist circumference and self-reported levels of physical activity. They found that a moderate amount of physical activity, compared with no activity, was the key to lowering the chances of premature death. The researchers estimated that exercise that burns between 90 and 110 calories a day could reduce the risk of an early death by between 16 percent and 30 percent. The effect of moderate exercise was greatest among normal weight people, but even overweight and obese people saw a benefit. Using the most recent data on deaths in Europe, the team estimated that 337,000 of the 9.2 million deaths of European men and women were linked to obesity. However, twice that number of deaths could be connected to lack of exercise. Aerobic exercise ignites the body’s immune system, improves mental function, boosts energy, strengthens muscles and bones, and reduces the risk for chronic diseases such as heart disease, cancer and diabetes.
________
_______
Sitting or Standing? Makes Zero difference without Exercise: 2015 study:
Researchers at the University of Exeter and University College London studied 16 years’ worth of health data from 5,132 people. The results showed that the total amount of time spent sitting (including sitting at work, at home, during leisure time) was not linked with the risk of all-cause mortality. Researchers also tracked time spent walking daily and on physical activity. Their findings suggest that reducing sitting time might not be quite as important for mortality risk as previously publicized and that encouraging people to be more active should still be a public health priority. 450 participants died during the course of the study, but the researchers found that overall sitting time didn’t correlate with a higher incidence of death, even after they controlled for age, gender, diet, general health and socio-economic status. They stressed on the importance of physical activity more than avoiding sitting for long periods. Spending long hours sitting is painted as an extremely unhealthy habit that is associated with a number of diseases. An expert statement released in the British Journal of Sports Medicine recommended Americans stand, move and take breaks for two hours out of an eight-hour work day. So are standing desks a solution? No, according to this study. New findings now suggest that sitting is not detrimental to one’s health if one indulges in physical exercise. It’s the sedentary lifestyle itself that kills, not the nice comfy chair. This also means that it’s pretty pointless for us to be standing at our desks at work since we’ll still be at equal risk of dying anyway.
_
Contrary study: prolonged sitting wipes out health benefits of recommended exercise:
Active couch potato effects:
An active couch potato refers to someone who is inactive for the majority of the day, but regularly makes sure to get in 30 minutes of moderate intensity exercise on most days. In a 2012 study published in the International Journal of Behavioral Nutrition and Physical Activity, researchers reported that people spent an average of 64 hours a week sitting, 28 hours standing, and 11 hours milling about (nonexercise walking), whether or not they exercised the recommended 150 minutes a week. That’s more than nine hours a day of sitting, no matter how active they otherwise were. Unless you have a job that keeps you moving, most of your nonrunning time is likely spent sitting. And that would make you an “active couch potato”—a term coined by Australian researcher Genevieve Healy, Ph.D., of the University of Queensland to describe exercisers who sit most of their day. If they aren’t careful, she says, active couch potatoes face the same health risks as their completely inactive counterparts. Up until very recently, if you exercised for 30 minutes or more a day, you were considered physically active. Now a consistent body of emerging research suggests it is entirely possible to meet current physical activity guidelines while still being incredibly sedentary, and that sitting increases your risk of death and disease, even if you are getting plenty of physical activity. Perhaps most potentially disconcerting about the health risks of sitting is that exercise does not appear to be enough to counteract its negative effects.
_
Your body is designed to move. Sitting for an extended period of time causes your body to shut down at the metabolic level. When your muscles, especially certain leg muscles, are immobile, your circulation slows. So you use less of your blood sugar and you burn less fat, which increases your risk of heart disease and diabetes. Indeed, a study of 3,757 women found that for every two hours they sat in a given work day, their risk for developing diabetes went up seven percent, which means their risk is 56 percent higher on days they sit for eight hours. And a study published in the American Journal of Epidemiology reports that a man who sits more than six hours a day has an 18 percent increased risk of dying from heart disease and a 7.8 percent increased chance of dying from diabetes compared with someone who sits for three hours or less a day. Although running does much good for you, if you spend the rest of your waking hours sitting, those health benefits depreciate. In a 12-year study of more than 17,000 Canadians, researchers found that the more time people spent sitting, the earlier they died—regardless of age, body weight, or how much they exercised. Adding to the mounting evidence, researchers recently discovered that a key gene (called lipid phosphate phosphatase-1 or LPP1) that helps prevent blood clotting and inflammation to keep your cardiovascular system healthy is significantly suppressed when you sit for a few hours. The shocker was that LPP1 was not impacted by exercise if the muscles were inactive most of the days. Heart disease and diabetes aren’t the only health hazards active couch potatoes face. The American Institute for Cancer Research now links prolonged sitting with increased risk of both breast and colon cancers. Sitting time is emerging as a strong candidate for being a cancer risk factor in its own right. Emerging evidence suggests that the longer you sit, the higher your risk. It also seems that exercising won’t compensate for too much sitting. Interrupting your sedentary time as often as possible and making frequent posture changes is important.
_
The Importance of Non-Exercise Movement:
If you think about it, why do we exercise? We exercise because we’re trying to replicate what our ancestors did. They moved around to a far greater degree than we do today, largely because they did not have the major technology we do today to easily obtain our food and shelter. Our ancestors didn’t have to exercise per se because they rarely sat down. They moved all day long, and research shows this is absolutely key for health. In fact, studies show that engaging in consistent exercise does not counteract the adverse cardiovascular and metabolic effects of prolonged sitting. So non-exercise movement is now recognized as being a foundational piece for optimal health — even more so than exercising for an hour a few times a week. Ideally, you’d do them both, but if you’re currently sedentary, start by sitting less.
_______
_______
Are exercise recommendations too much?
That looming 150-minute figure seems like nobody has time for that. This is the problem with our exercise recommendations, argues a new analysis published in The BMJ. They’re just set far too high to motivate the people who need them the most. That’s the argument of Philipe de Souto Barreto, a researcher at University Hospital of Toulouse in France and author of the new paper. “Getting inactive people to do a little bit of physical activity, even if they don’t meet the recommendations, might provide greater population health gains,” he writes. It’s not that the recommendations are off for optimal health. 150 minutes of moderate physical activity each week, which the World Health Organization sets as its target, is a great goal that’s been shown to reduce risk for all kinds of diseases and death, Barreto says. But other data shows that gentler goals can also provide important health benefits. One study of more than 250,000 older adults found that getting less than an hour of moderate physical activity each week was linked to a 15% drop in death. Barreto also cites a review of 254 articles looking at the link between exercise and disease reduction, which found that the relationship between the two is dose-dependent. In other words, it’s not an all or nothing affair: even minor shifts can help people who don’t get enough exercise. Another analysis of studies found that when people walk just 74 minutes a week, they have a 19% reduced risk of death, compared to the most sedentary people. Achieving target physical activity recommendations should remain as a goal but not the core public health message surrounding physical activity,” Barreto writes.
_______
_______
My logic:
The figure above shows that only regular exercise with daily life physical activity (Non-Exercise Movement) confers health benefits.
_______
_______
Not everyone benefits equally from exercise:
It does seem clear that older adults benefit more from exercise than younger people, as far as cognitive function is concerned. It also seems that older women, especially those on hormone-replacement therapy, receive greater cognitive benefits from exercise than men. Generalisations aside, it is as well to remember the findings of a very recent study showing that, while most people benefit (physically) from exercise, the degree of benefit is hugely variable between individuals, and some people don’t benefit at all! People mature at different rates, and there seems to be a genetic component to coordination, strength, speed, and one’s response to exercise. Nonetheless, everyone should strive to be as fit as they possibly can, given their strengths and limitations.
_
Conventional wisdom has it that anyone who really wants to become fit can do so. Just walk or ride a bicycle, swim or run. Speed and endurance will improve and what was once hard will become easy. Lift weights, work with a trainer in a gym, and muscles will grow larger and stronger. But when a few intrepid scientists began asking if those beliefs were true, they found that fitness, like weight loss, has genetic underpinnings, making it inherently much easier for some to get fit than it is for others.
_
Three examples prove the role of genes in exercise benefits and physical fitness:
Example 1:
A measurement of a training response is the increase in the amount of oxygen people use when they try to push themselves hard. The more oxygen taken in, the more that enters the blood and is delivered to muscles and so the more intensely the person can exercise, running faster for example. The average increase after training was 400 milliliters of oxygen. But some people had no increase and in some the increase was more than double the average. The range was zero milliliters to 1,000 milliliters. The standard deviation was 200, meaning that two-thirds of the people increased their oxygen consumption by 200 to 600 milliliters of oxygen. These are huge differences, but within families, you have aggregation. Children tend to respond the way their parents do. Siblings tend to respond like each other. The heritability of responsiveness to exercise training was at least as great as it is for body weight, blood pressure and cholesterol.
Example 2:
The study, with Dr. Eric Hoffman, a geneticist at the Children’s National Medical Center in Washington and others, involves 700 men and 700 women who had not previously lifted weights and who agreed to train in a laboratory. They are trying to build the biceps and triceps muscles of one arm only. The other arm serves as a control while the researchers look for genetic variants that can explain their responses to training. Although muscle strength and size seem to go together, Dr. Hoffman says they are independent — some people can gain muscle size but not much strength; others can gain strength but not much size. Some gain both. Others gain neither.
Example 3:
Dr. Claude Bouchard, who now directs the Pennington Biomedical Research Center at Louisiana State University, did the studies with pairs of identical twins, finding that if one twin responded well to training, so did the other; if one did not respond, neither did the other.
_
Some exercise physiologists and sports trainers had assumed that people who said they exercised but never increased their fitness were cheating, either dissembling about the amount of exercise they did or deceiving themselves about how hard they worked when they exercised. But it was not true. Now, having garnered convincing evidence that genes determine a person’s abilities at athletic training, scientists are conducting large and rigorous studies to track down the particular genes, and genetic variants, involved. The studies do not address the effects of exercise on overall health, whether it helps ward off heart disease or brings longer life, but they are intent on determining the answers to certain health-related questions. For instance, the new research may help find better ways of preventing old people from falling because their muscles are weak. Is there a way of deciding who needs extra help in maintaining muscle strength or is there an ideal way of augmenting strength in people who are genetically predisposed to be weak? Can an understanding of the genetic variants that control how large and how strong muscles grow lead to better treatments? But the research is detecting measures of athletic fitness and, as a consequence, the studies raise ethical questions. Should people be told if they have a gene that will prevent them from ever getting aerobically fit? Should coaches be able to do genetic testing of athletes to learn who is most likely to improve, and who has the genes to be a future star?
________
________
Exercise as medicine:
Did you know that exercise is one of the safest, most effective ways to prevent and treat chronic diseases such as heart disease?
This common-sense advice was again confirmed in a meta-review conducted by researchers at Harvard University and Stanford University, which compared the effectiveness of exercise versus drug interventions on mortality outcomes for four common conditions:
•Diabetes
•Coronary heart disease
•Heart failure
•Stroke
After reviewing 305 randomized controlled trials, which included nearly 339,300 people, they found “no statistically detectable differences” between physical activity and medications for prediabetes and heart disease. Exercise was also found to be more effective than drugs after you’ve had a stroke. The only time drugs beat exercise was for the recovery from heart failure, in which case diuretic medicines produced a better outcome.
The drugs assessed in the studies included:
•Statins and beta blockers for coronary heart disease
•Diuretics and beta blockers for heart failure
•Anticoagulants and antiplatelets for stroke
_
The featured review is a potent reminder of the power of simple lifestyle changes, as well as the shortcomings of the drug paradigm. If you’re interested in living a longer, healthier life, nothing will beat proper diet and exercise. Exercise is in fact so potent, the researchers suggested that drug companies ought to be required to include it for comparison when conducting clinical trials for new drugs! The analysis adds to evidence showing the benefit of non-medical approaches to disease through behavior and lifestyle changes. In cases where drug options provide only modest benefit, patients deserve to understand the relative impact that physical activity might have on their condition. Exercise interventions should therefore be considered as a viable alternative to, or, alongside, drug therapy.
_
Exercise prescription:
Exercise prescription commonly refers to the specific plan of fitness-related activities that are designed for a specified purpose, which is often developed by a fitness or rehabilitation specialist for the client or patient. Due to the specific and unique needs and interests of the client/patient, the goal of exercise prescription should be focus on motivation and customization, thus making achieving goals more likely to become successful. In the United Kingdom there is a scheme called “Exercise on prescription” in which doctors are able to prescribe exercise to those with conditions that benefit from it, such as asthma, depression or obesity. The initiative particularly aimed to lower the rate of heart disease. Researchers in New Zealand have also discussed the benefits of exercise referral by medical practitioners there. In New Zealand it is known as a green prescription, while in the United States a similar initiative is known as Exercise is Medicine.
_
The thinking in today’s society is that exercise is a tool to cure. If physical activity is considered normal and necessary for good health, the notion that physical inactivity is a cause of chronic diseases will be easy to support. Healthcare professionals play an important role in promoting physical activity and weight management. Primary care starts with primary prevention. General practitioners have access to a large proportion of patients with co-morbidities, obesity and sedentary lifestyles and are a respected source of advice. Prescribing exercise as prevention should be a responsibility of primary care providers.
_
Physical therapy:
Physical therapy or physiotherapy (often abbreviated to PT) is a physical medicine and rehabilitation specialty that remediates impairments and promotes mobility, function, and quality of life through examination, diagnosis, prognosis, and physical intervention (therapy using mechanical force and movements). It is carried out by physical therapists (known as physiotherapists in most countries). PT management commonly includes prescription of or assistance with specific exercises, manual therapy and manipulation, mechanical devices such as traction, education, physical agents which includes heat, cold, electricity, sound waves, radiation, rays, prescription of assistive devices, prostheses, orthoses and other interventions.
________
_______
Role of family physicians in promoting physical activity in society:
Among the many reasons for low levels of activity among population is the missed opportunity for family physicians to influence their patients’ exercise behaviour. Although family physicians are well positioned to counsel patients about exercise, studies show that rates of such counselling remain low. When it comes to things that get in the way of physicians providing exercise advice to their patients, the usual suspects come into play—lack of time, lack of financial reimbursement, and lack of training. One of the best predictors of whether a physician provides exercise counselling to patients, however, is the physician’s own level of physical activity. One of the earliest studies to show this was the US Women Physicians’ Health Study, which determined that women doctors who complied with the ACSM-AHA physical activity recommendations were much more likely to counsel patients to exercise and to be trained in such counselling. Subsequent further work by Frank and colleagues has shown clearly that “active doctors prescribe activity.” These researchers have also indicated that talking to your patients about your own exercise habits can make your advice more credible and can help motivate them to become more active. Doctors are unique in being trusted, often seeing people at their most vulnerable and interacting with many of those suffering the worst health, in particular those with the most to gain from small improvements in health. Since such a large proportion of the population are inactive or moderately inactive, even small differences in lifestyle may make a big difference to health in the population and encourage behaviour change. Rates of exercise counselling by doctors remain low; only 34% of US adults report exercise counselling at their last medical visit. In view of this gap, one of the US health objectives is increasing the proportion of patients appropriately counselled about health behaviours, including exercise.
_____
What should doctors be saying to their patients?
The message is simple:
All adults should do physical activity at a minimum amount of 5-times-a-week, for 30 minutes each time. The sessions can be broken into 10- or 15-minute blocks. The activity should have moderate intensity – enough to get a little out of breath, and/or to feel your heart rate increase, and/or to feel a little sweaty. For children, a minimum of one hour exercise is expected, five times a week.
_______
_______
The moral of the story:
_
1. We would expect captive elephants to live at least as long, if not longer, than those in the wild because they are better cared for, but that is not the case. A study found that captive elephants in Zoo lived for 16-18 years while wild for 56 years. This is because wild elephants can roam over 300 to 2000 miles per day. Regular exercise is important to avoid illness and encourage normal behaviour patterns in most pet animals. If physical inactivity reduces life span of elephant by third, what about humans?
_
2. Physical activity means voluntary movement of large skeletal muscles requiring energy more than resting energy expenditure, often done to sustain daily living or recreation, and often provide health benefits. Activities that involve small skeletal muscles (e.g. writing) are not classified as physical activity as they hardly provide any health benefit. Exercise is a subcategory of physical activity that is planned, structured, repetitive, and purposeful, usually performed at free time with the goal to improve or maintain physical fitness. A “workout” is a term that refers to the period of time spent exercising — the exercise event. That makes “working out” the same thing as “exercise.” Physical inactivity means physical activity levels less than that required for optimal health and prevention of premature death.
_
3. Physical fitness is a measure of the body’s ability to function efficiently and effectively in work and leisure activities without undue fatigue, resist diseases from sedentary lifestyles, and to meet emergency situations. In other words, physical fitness enables us to perform moderate-to-vigorous levels of physical activity without undue fatigue.
_
4. Our ancestors had to go long distances every day in order to survive. Not exercising was never an option. So there was evolutionary selection pressure to avoid needless exercise to save energy. For example, when you walk into a train station and there is a staircase and an escalator, your brain always tells you to take the escalator due to very deeply rooted evolutionary instinct. Nowadays due physical inactivity and overeating, this trait has become maladaptive. That is why we have to make conscious effort to exercise through some form of socially acceptable coercion.
_
5. Aerobic exercise means large skeletal muscles performing exercise utilize oxygen to generate energy for exercise so that all glucose/fatty acid is aerobically turned into energy and muscle cells can contract repeatedly without fatigue. Cardio is aerobic exercise performed at moderate levels of intensity for extended periods of time. Intensity is the rate of energy expenditure of exercise correlating with the efforts to perform exercise. This moderate intensity can vary from 60 to 80% of maximum heart rate, 40 to 60 % of VO2 max and 3 to 5.9 MET. For cardiovascular health benefits, at least 30 minutes of moderate intensity aerobic exercise should be performed on most days per week. Aerobic exercise of fewer than 2 days per week, at less than 40 % of VO2 max, and for less than 10 min duration is generally not sufficient to confer cardiovascular health benefit. Anaerobic exercise does not utilize oxygen to generate energy for exercise and generate lactate from anaerobic glycolysis. The muscles are exercised at high intensity for short durations. Resistance training not only builds muscle and bone density, it reduces body fat and even improves your cardiovascular health. Simply put, aerobic exercise is a low to moderate intensity activity sustained for a long duration, while anaerobic is a high intensity exercise done for a short duration. In reality, the more intensely we exercise, the greater the need for anaerobic energy production. Consequently, it is best to view the terms aerobic and anaerobic as transitions in metabolism, where the proportion between aerobic and anaerobic metabolism changes depending on exercise intensity. All aerobic exercises like running, cycling and rowing, effectively become anaerobic when performed in excess of 90% maximum heart rate. In almost all conditions, anaerobic exercise is accompanied by aerobic exercises because the less efficient anaerobic metabolism must supplement the aerobic system due to energy demands that exceed the aerobic system’s capacity.
_
6. Maximum effort exercise is when exerciser makes so much efforts that he/she utilizes full VO2 max achieving maximum heart rate (i.e. 220 minus age). Over-exercise (excessive exercise) is when person exercises for more than 2 hours continuously, the only exception being highly trained athlete e.g. highly trained marathon runner.
_
7. Metabolic Equivalent of Task (MET) is the ratio of the work metabolic rate to the resting metabolic rate. One MET is 1 kcal/kg/hour (0.0166 kcal/kg/min) energy expenditure utilizing 3.5 ml/kg/min oxygen; equivalent to the energy cost and the oxygen use of sitting quietly. MET values of activities range from 0.9 (sleeping) to 2 (walking at a slow pace 3 km/h) to 3.3 (brisk walking at 3 miles/hr) to over 6 (running).
_
8. VO2 max is the maximum rate of oxygen consumption during the aerobic catabolism of glucose/fatty acid measured during incremental exercise, most typically on a motorized treadmill. Maximal oxygen uptake (VO2 max) is widely accepted as the single best measure of cardiovascular fitness and maximal aerobic power. Absolute values of VO2 max are typically 40-60% higher in men than in women. The average untrained healthy male will have a VO2 max of approximately 35 – 40 mL/kg/min. Highly trained male athletes can consume up to 85 mL/kg/min.
_
9. While doing maximum effort exercise, an average person uses oxygen 10 times that of rest and highly trained athlete doing the same exercise uses oxygen half of that of average person as intensity of the same exercise will be lower in highly trained athlete. In other words, maximum effort exercise performed by highly trained athlete is of double intensity than maximum effort exercise performed by average man.
_
10. Over half of the world population are physically inactive, that is, not performing the minimum recommended 30 minutes of moderate-intensity activity on at least 5 days of the week. Screen time is the time spent watching television, computers, video games and smartphones making you inactive and taking away your time for exercise.
_
11. About 50% of people who start an exercise program will drop out during the first 6 months due to low levels of motivation & self-efficacy, time-shortage, low familiarity with exercise, poor social & cultural support, and the belief that exercise will not bring any benefit.
_
12. You don’t have to be athletic to exercise. A perfect example is brisk walking.
_
13. No one is too young or too old to exercise.
_
14. Household work cannot be counted as exercise as people who say they exercise by doing housework are overestimating the intensity or the duration of the activity.
_
15. Health benefits of physical activity depend mainly on total weekly energy expenditure due to physical activity rather than any one component (frequency, intensity, or duration). The minimum optimal “volume” (frequency, duration and intensity of exercise) of exercise that confers health benefits is exercise that uses energy worth 500 to 1,000 MET-minutes per week. Most experts and professionals advocate a minimum volume of exercise that expends 1000 kcal (4200 kJ) per week for health benefits. For a 70 kg individual, 1000 kcal per week comes to 860 MET-minutes. The target could be lower for elderly. However, it is not all or none phenomenon as relationship between exercise and disease reduction is dose dependent, and even micro-workout of 7 minutes is helpful. Some exercise is better than none; more exercise is better than some; and exercise in greater variety is better than uniform exercise. The combination of aerobic exercise with resistance training and flexibility exercises would render greater health benefits and better quality of life. The largest health gains occur in people moving from inactivity to activity.
_
16. Although exercise affects gene’s behaviour by epigenetic alteration resulting in preventing and/or confronting various disorders, such as metabolic or neurodegenerative diseases, obesity, diabetes mellitus, cardiovascular disease and cancer; it is your genes that determine how you respond to exercise in getting exercise benefits and fitness. Therefore not everyone benefits equally from exercise.
_
17. Aerobic exercise improves cardio-respiratory system by improving their efficiency and capacity. Skeletal muscles contractions improve muscle mass; with resultant pull over bones and weight bearing improve bone density. Exercise improves insulin sensitivity, reduces obesity, reduces LDL and reduces blood pressure & heart rate. Although acute exercise increases heart rate & blood pressure transiently due to stimulation of sympathetic nervous system, chronic regular aerobic exercises leads to aerobic conditioning (training) which decreases heart rate at rest and during exercise, and also decreases blood pressure due to improved stroke volume, reduced peripheral resistance, decreased sympathetic activity and increased vagal tone.
_
18. Exercise improves blood flow to brain, promotes neuronal growth and triggers neurotransmitters such as endorphins, norepinephrine, serotonin, dopamine, glutamate, and GABA. Routine physical activity is also associated with improved psychological well-being through reduced stress, anxiety and depression. Exercise can be a healthy, safe and inexpensive way to achieve more and better sleep. Exercise acts as a type of distraction, biofeedback, meditation, or psychological buffer and can result in an increased sense of self-efficacy, control, and mastery.
_
19. Exercise in elderly reduces risk of cardiovascular disease, osteoarthritis, osteoporosis, hypertension, diabetes and falls. It also improves cognition, maintains their independence and contributes to the management of depression and anxiety. Taken together, these benefits can significantly improve quality and quantity of life in elderly populations. When elderly cannot do the recommended amounts of physical activity due to health conditions, they should be as physically active as their abilities and conditions allow.
_
20. Physically active children are better off cognitively, emotionally and socially. For school going children, time spent in physical activity programmes does not hinder academic performance, and it may indeed improve academic performance.
_
21. People who exercise regularly yet have other risk factors for cardiovascular disease may be at lower risk of premature death than people who are sedentary with no risk factors for cardiovascular disease.
_
22. For a long time, rest and physical inactivity had been recommended for patients with heart failure. Numerous trials have now demonstrated that moderate exercise in patients with heart failure appear to be safe; and in fact improves cardiac output at maximal workloads, improves mitochondrial size and density in cardiac muscle, reduces endothelial dysfunction, and decreases circulating catecholamine.
_
23. Although moderate aerobic exercise is now strongly recommended as part of the lifestyle modifications as an adjunct to pharmacological therapy for treatment of hypertension, people with moderate to severe hypertension must reduce blood pressure by pharmacological therapy before starting exercise regimen.
_
24. Exercise with diet control is better than metformin to prevent diabetes mellitus. Also in diabetics, exercise reduces A1c level by 0.5 to 1 % and reduces mortality risk.
_
25. Largest driver behind obesity is not how sedentary people are but how unhealthy their diet is (i.e. fast food plus junk food), and people only lose noticeable weight if they combine exercise and calorie restriction. In my view, to reduce weight in obese individual, dietary restriction contribute 80 % and exercise contribute 20 %; although exercise does reduce risk of cardiovascular disease and all-cause mortality among more active individuals regardless of weight loss. Being sedentary may be twice as deadly as being obese. In other words, physically fit obese individual exercising regularly is healthier than a sedentary normal weight individual.
_
26. To reduce belly fat, first you have to address your diet, and then do exercise to reduce weight, and then do exercise that target your abdominal muscles.
_
27. Walking and swimming are two activities that are considered safe throughout pregnancy. Moderate exercise during pregnancy decreases risk of pre-eclampsia and gestational diabetes in mother. However, vigorous exercise in pregnancy is associated with miscarriage and small birth weight babies.
_
28. Exercise confers economic benefits by reducing absenteeism, increasing productively & efficiency at work, and reducing health expenditures of many non-communicable diseases (NCD). Lack of fitness in the society has a severe negative economic impact.
_
29. Physical inactivity has been identified as the fourth leading risk factor for global mortality and this risk may decrease by 19 % with as little as 30 minutes of moderate-intensity physical activity per day five days a week in people who are physically inactive. Recommended moderate exercise extends life expectancy to as much as 4 to 5 years. A middle-aged person who gets the recommended 150 minutes per week of moderate exercise can expect a 1-to-7 return: seven extra minutes of life gained for each minute spent exercising.
_
30. The global epidemic of physical inactivity is labelled as ‘the new smoking’ because lack of exercise is killing roughly the same number of humans as smoking. About 5.3 million of the 57 million deaths worldwide in 2008 could be attributed to inactivity while more than 5 million of deaths are the result of direct tobacco use.
_
31. Inactive individual may have a maximal aerobic power of only six times their resting metabolic rate while person who exercises regularly will have a maximal aerobic power 10 to 12 times resting. A person cannot work throughout the day at much more than about 20 percent of maximal capacity without becoming chronically fatigued. An inactive person who has a maximal aerobic power of six times resting can comfortably sustain a work level of only about 1.2 times resting throughout the day (6 × 0.20 = 1.2). This low capability for sustained energy expenditure can support only a very sedentary existence. So inactiveness leads to sedentary life style and not vice versa. On the other hand, person who exercises regularly can comfortably sustain a work level of about 2.4 times resting throughout the day (12 × 0.20 = 2.4) and thereby leads active life easily. In other words, whether to lead sedentary or active life depends on your voluntary exercise behaviour, and not on your job, lack of time, socioeconomic factor or culture.
_
32. Family physicians are well positioned to counsel patients about exercise; studies show that rates of such counselling remain low due to lack of time, lack of financial reimbursement, lack of training, and more importantly lack of exercise by physicians themselves. Active doctors prescribe activity. Inactive doctors do not prescribe activity. Similarly, those doctors who smoke tobacco or drink alcohol are unlikely counsel their patients to quit smoking or drinking.
_
33. Exercise is equivalent to medicine in prevention and treatment of non-communicable diseases and exercise ought to be included for comparison when conducting clinical trials for new drugs. Exercise prescription should be given by doctors to prescribe exercise to those with conditions that benefit from it such as diabetes, hypertension, obesity, coronary artery disease, heart failure, stroke, osteoporosis, pulmonary diseases, cancer, dementia, depression and elderly.
_
34. Active couch potato refers to someone who is inactive (sitting) for the majority of the day, but regularly makes sure to get in 30 minutes of moderate intensity exercise on most days. Prolonged sitting increases risk of heart disease, diabetes and some cancers despite getting recommended daily exercise. Exercising won’t compensate for too much sitting. You have to interrupt sitting by walking out of your chair frequently. Remember, regular exercise with daily life physical activity (Non-Exercise Movement) confers health benefits. Regular exercise with sitting whole day does not confer health benefits.
_
35. Once exercise becomes too much, the benefits are reduced, or even reversed, and it becomes a chronic stressor that reduces overall wellness. Those who exercised moderately lives the longest and are the healthiest compared to inactive (no exercise) or hyperactive (too much exercise).
_
36. Walking is free, simple, enjoyable, low impact (does not put stress on the joints), weight-bearing (it can improve bone density) and already a part of everyday life. Nearly everyone can do it, no matter their age or physical condition. It requires no equipment. All you need to do is correct your technique, walk faster (about 100 steps per minute i.e. 3 miles per hr) and for longer time. This is brisk walking, 3.3 MET moderate intensity aerobic exercise, and 150 minutes of brisk walking per week is 500 MET-minute exercise conferring significant cardiovascular benefits. A brisk 20-minute walk each day is enough to reduce the risk of an early death by as much as 30 percent. Walking gives more health benefits than running provided energy expenditure of both are same (walk longer than you’d have to run); and walking stresses joints & cartilages of legs considerably less than running. Running at moderate speeds is linked with a lower risk of death from any cause compared to no running. However more intense running didn’t yield additional benefit. In fact chronic extreme running efforts like marathons, ultra-marathons, and long-distance triathlons do cause cardiovascular damage over time. My exercise prescription to everybody is brisk walking at least 150 minutes per week.
________
Dr. Rajiv Desai. MD.
November 19, 2015
________
Postscript:
I am surprized to know that so many studies found exercise improving brain power by improving cognition & memory resulting in improved academic performance in children and college students, and preserving cognitive function in old age. Only one study of 2015 found that exercise may not help brain. When I look at my own life, I hardly exercised since childhood. Yet my cognition, memory, academic performance and creativity are above average. There are many examples of people with both interest in exercise and exceptional intelligence, but little if any evidence of a causal relationship in those cases. For example, Albert Einstein frequently commented that a large number of his theories were conceived while riding his bicycle. Outstanding intellectual achievement seems to be a result of different kinds of factors in different people. It doesn’t appear that holding all other things equal and exercising heavily would lead someone to gain exceptional intellectual ability. Top athletes do possess the ability to process and react to complex and rapidly changing visual cues but that is not cognition. Physical exercise improving physical health is logical, physical exercise increasing brain volume in areas related to movement is plausible, but physical exercise improving intellectual ability is weird. In my view, most claims regarding exercise and the brain concern the neuroprotective effect of exercise rather than cognitive enhancement per se.
_
Footnote 1:
If you’re interested in living a longer, healthier life, nothing will beat proper diet, moderate exercise, maintaining ideal body weight, with no tobacco and no alcohol. Not a difficult task but believe me, very few can do it.
_______
Footnote 2:
Advice to common man regarding exercise:
Take time to warm up and stay hydrated. You need to be sweating a bit and get short of breath. Keep it up for 15-20 minutes a day and you’re done! Never exercise when you are tired. Exercise without rest does not work. You should not be fatigued and/or dehydrated before exercise, during exercise and after exercise.
________


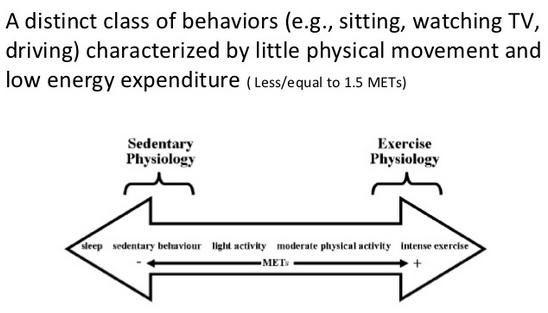
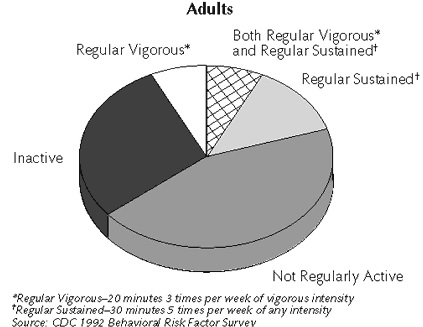


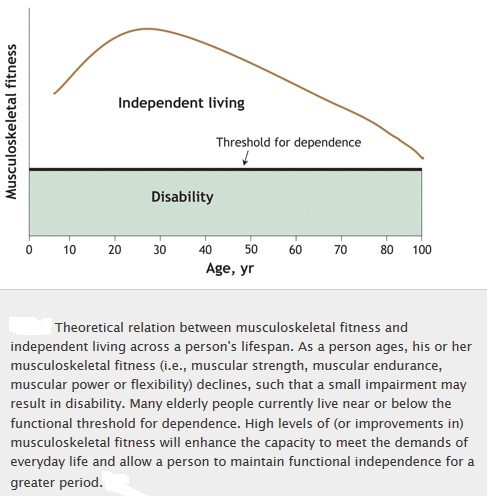
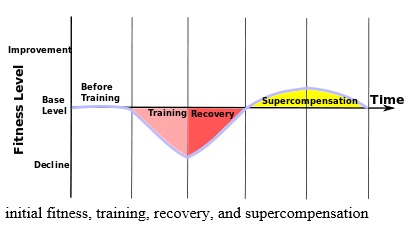
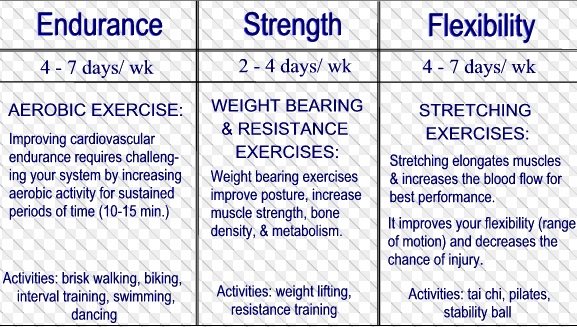
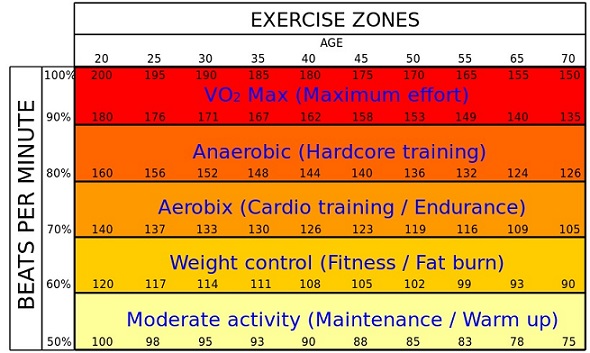
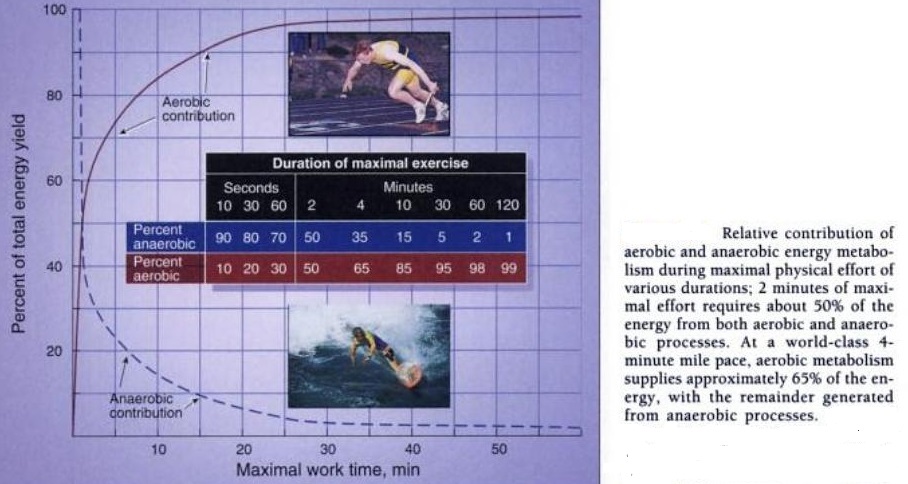
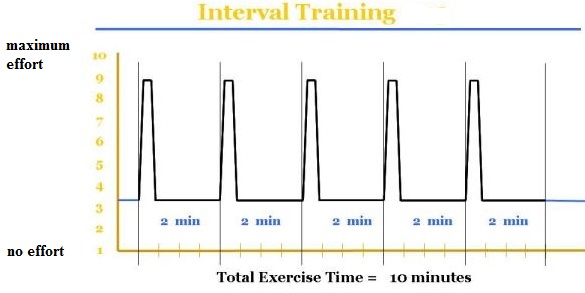

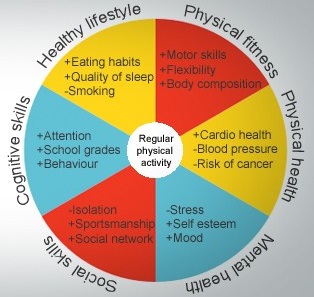
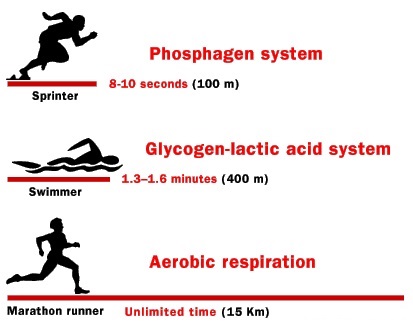
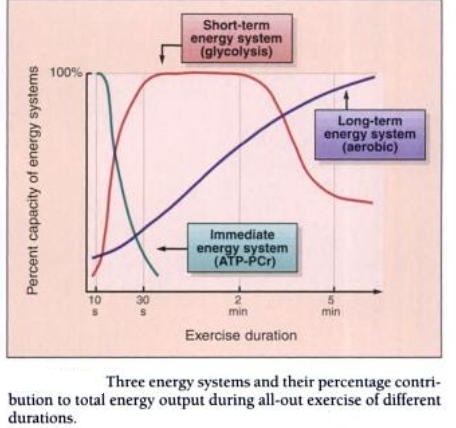
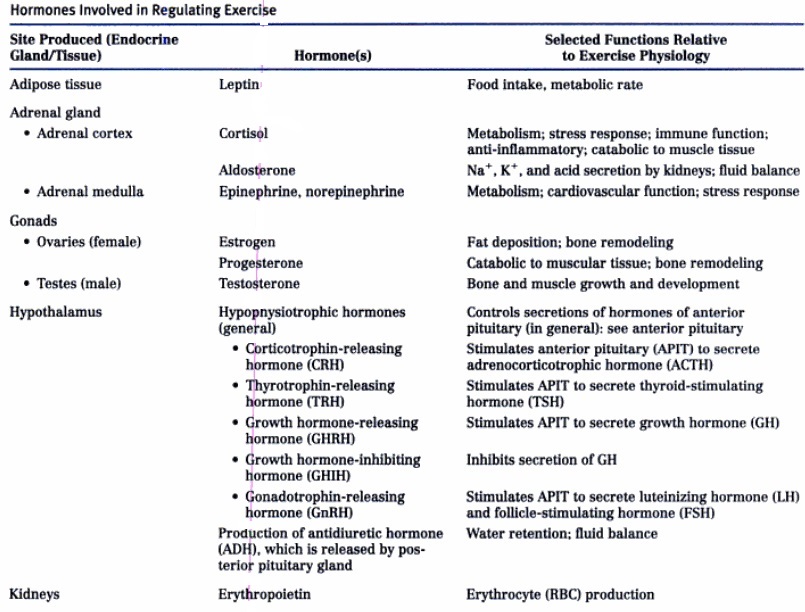

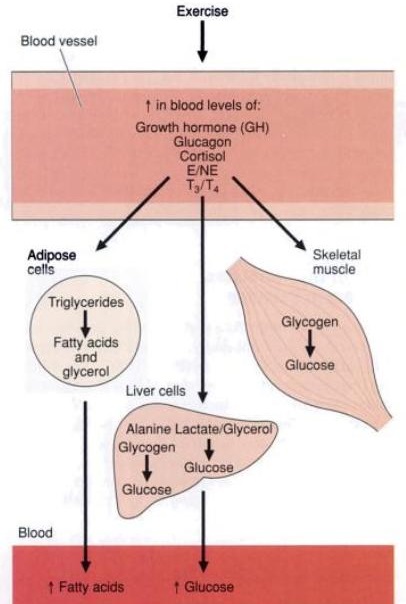
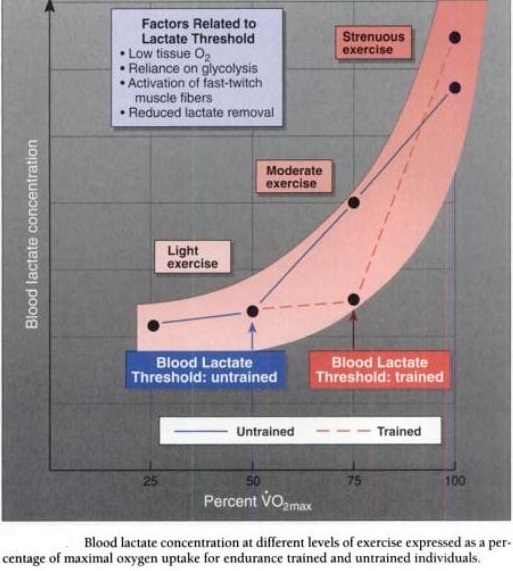
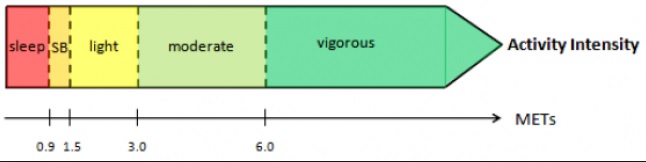
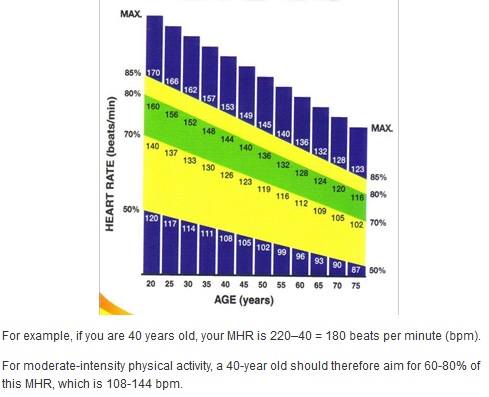
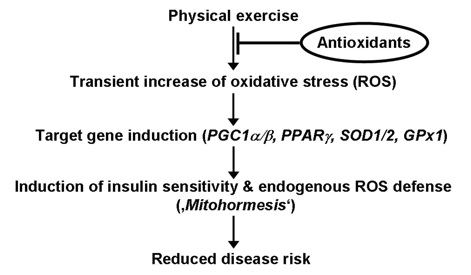
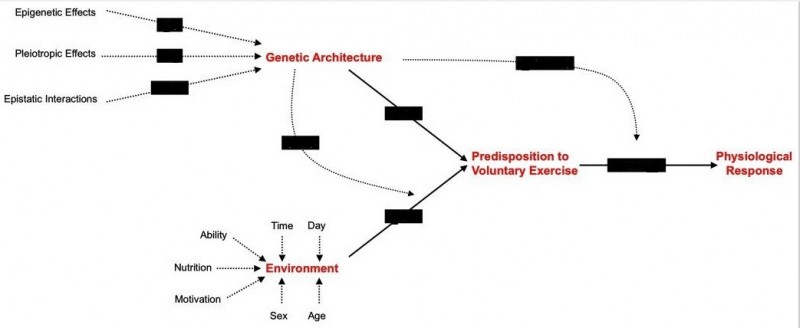
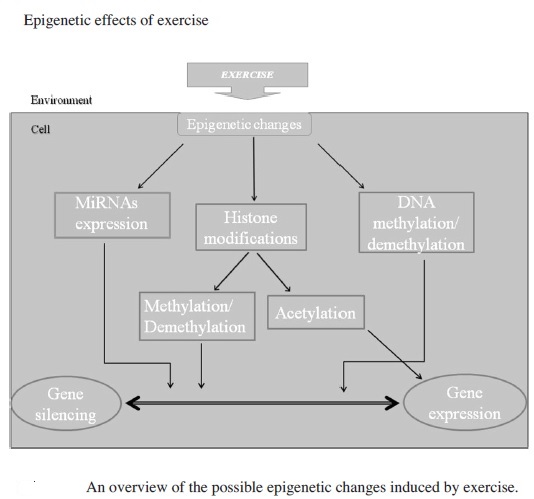
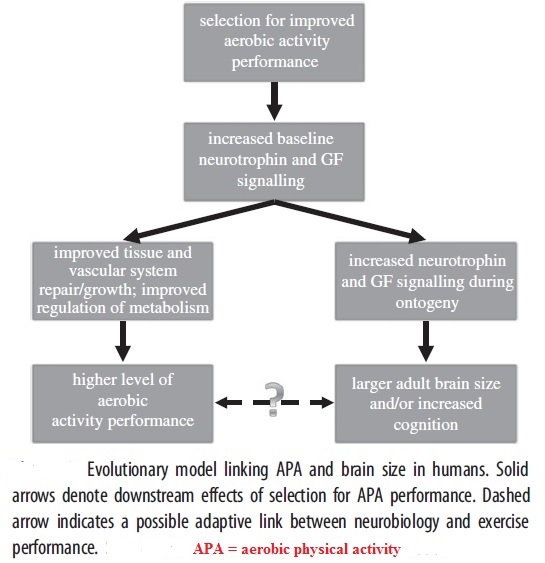
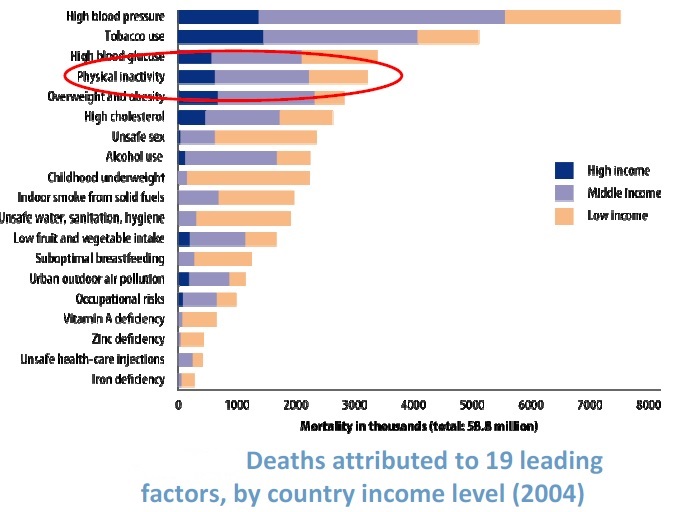
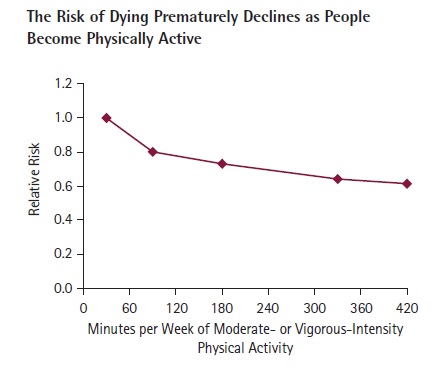
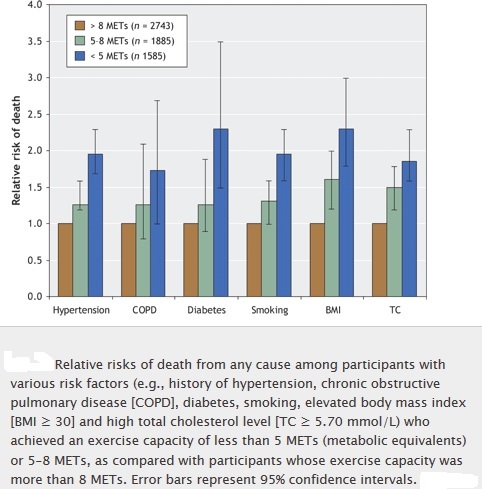
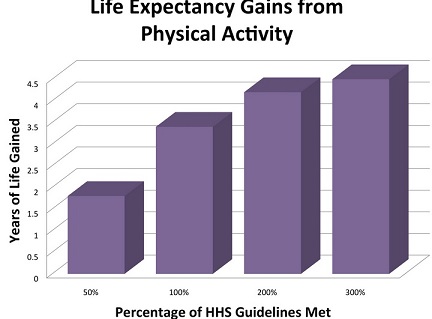
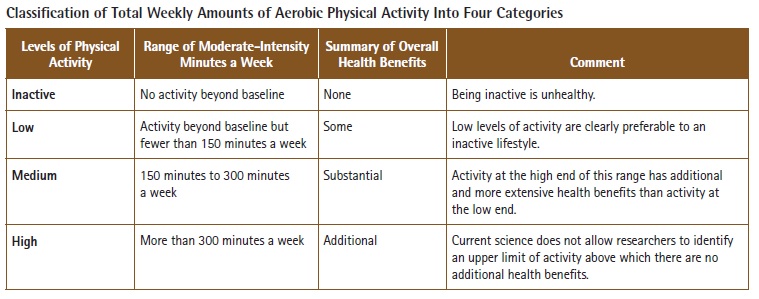
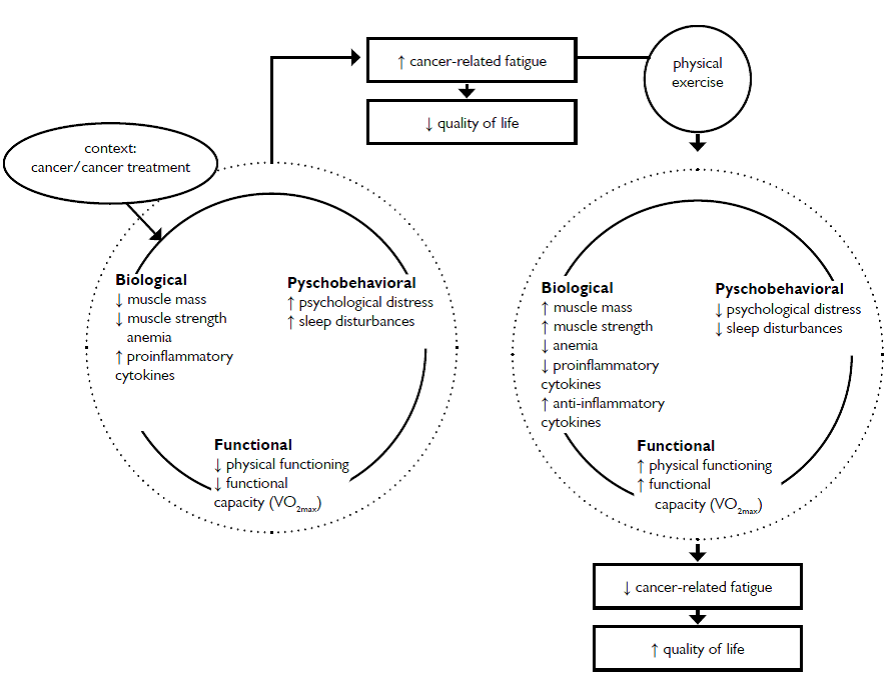
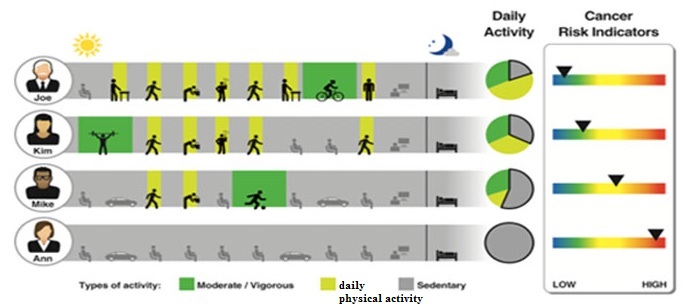

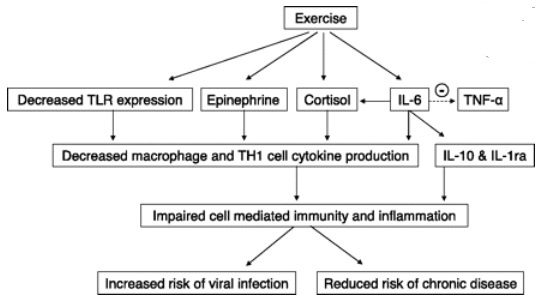
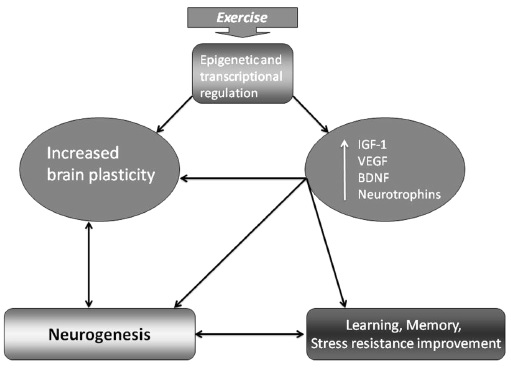
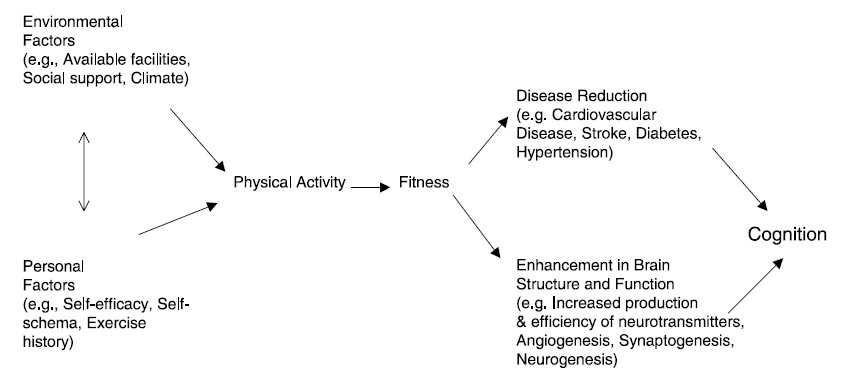
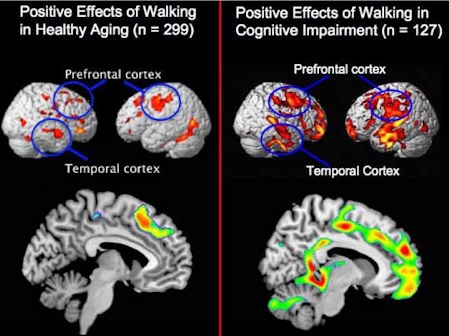
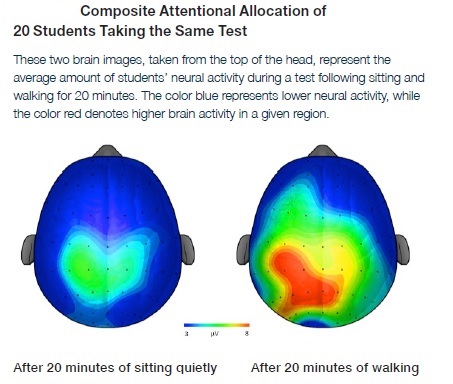
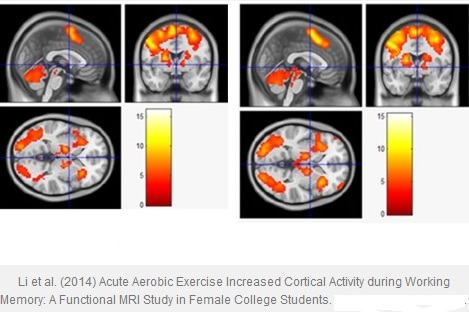
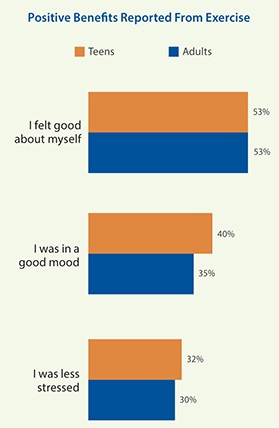
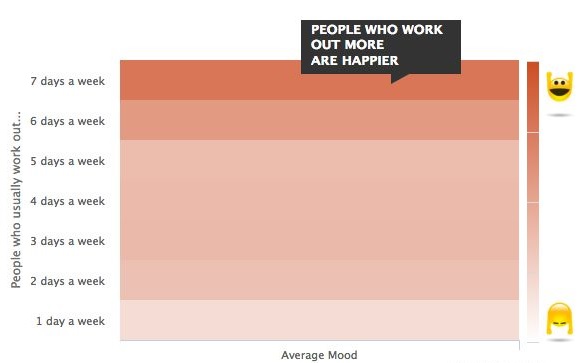
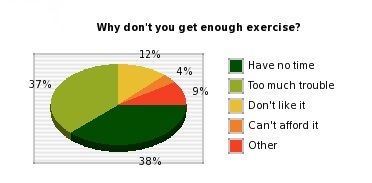
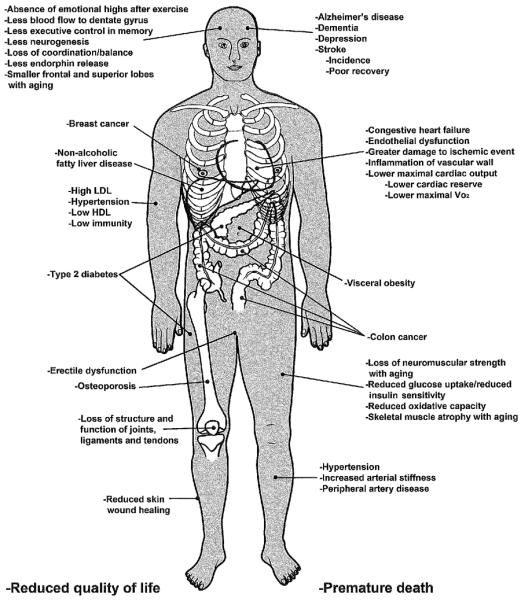

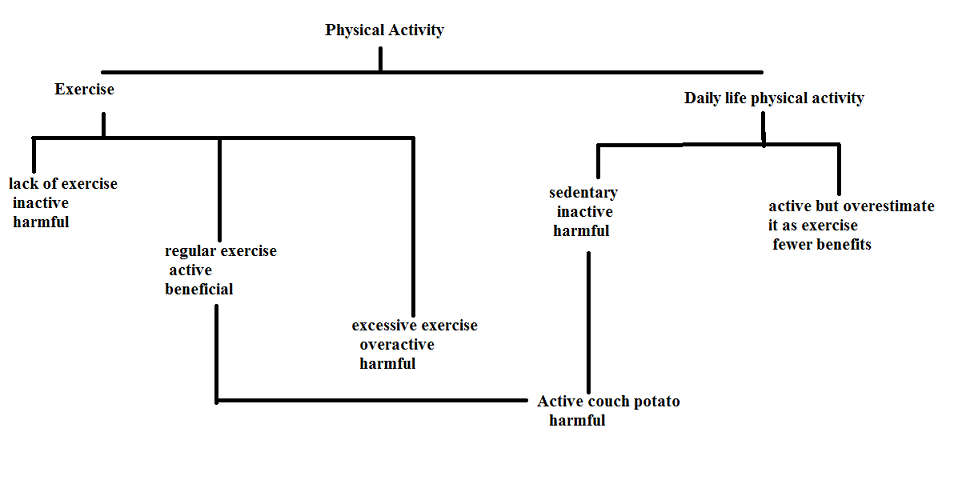
I am actually thankful to the owner of this website who has shared this wonderful post at here.|
It is perfect time to make some plans for the long run and it is time to be happy. I have read this post and if I may I desire to suggest you few interesting issues or tips. Maybe you could write next articles referring to this article. I desire to read more issues approximately it!|
Wow, great blog post.Really looking forward to read more. Want more.
This info is worth everyone’s attention. Where can I find out more?|
You don’t have to be superhuman to be remarkable. Let Amazingness assist you do extra, feel better, as well as get ahead.
You do not need to be superhuman to be outstanding. Let Amazingness aid you do a lot more, really feel better, as well as prosper.
You sound like me! Wow!
Excellent write-up. I definitely appreciate this website.
Keep writing!
I’m really enjoying the design and layout of your blog.It’s a very easy on the eyes which makes it much more pleasant for me to come here and visit more often.
Your style is so unique in comparison to other folks I’ve read stufffrom. Thank you for posting when you’ve got the opportunity, Guess I will justbookmark this web site.
This design is spectacular! You certainly know how to keep a reader amused. Between your wit and your videos, I was almost moved to start my own blog (well, almost…HaHa!) Excellent job.
Hi there friends, how is everything, and what you
wish for to say about this paragraph, in my
view its genuinely remarkable in support of me.
Quality posts is the key to interest the users to pay a quick visit the
website, that’s what this website is providing.
I like the valuable info you provide in your articles. I’ll bookmark your
blog and check again here frequently. I am quite certain I will learn a lot of new stuff
right here! Good luck for the next!
I simply want to say I am just all new to blogging and site-building and absolutely savored this web blog. Very likely I’m planning to bookmark your blog . You definitely come with remarkable well written articles. Thanks a bunch for sharing with us your web-site.
Excellent way of telling, and fastidious paragraph to obtain facts regarding my presentation topic, which
i am going to convey in academy.
It’s enormous that you are getting ideas from this paragraph as well
as from our dialogue made at this time.
Hi there colleagues, its wonderful piece of writing on the topic of teachingand fully explained,
keep it up all the time.
It’s an remarkable paragraph in favor of all the internet people; they will take
benefit from it I am sure.
Im obliged for the blog article.Really thank you! Awesome.
Asking questions are really pleasant thing if you are not understanding anything fully, except this piece
of writing presents good understanding yet.
I have been exploring for a bit for any high quality articles or weblog posts in this sort of area .
Exploring in Yahoo I finally stumbled upon this website.
Studying this information So i am glad to exhibit that I have an incredibly just right uncanny feeling
I found out just what I needed. I most for sure will make
sure to don?t overlook this web site and give
it a glance regularly.
the time to read or take a look at the material or internet sites we have linked to below the
thanks for sharing
Fantastic article.Really looking forward to read more. Great.
Im thankful for the article. Much obliged.
I really like and appreciate your post.
A big thank you for your article post.Really looking forward to read more. Will read on…
Im thankful for the blog post. Really Great.
I value the blog.Thanks Again. Great.
Great, thanks for sharing this blog.Really thank you! Cool.
I am really impressed with your writing skills and also
with the layout on your blog. Is this a paid theme or did you modify it yourself?
Anyway keep up the excellent quality writing, it is rare to see a great blog like this one today.
I do not even know how I ended up here, but I thought this post was great.
I don’t know who you are but definitely you’re going to a famous blogger if you aren’t already 😉 Cheers!
Useful info. Lucky me I discovered your site by chance, and I’m stunned why this accident did not happened earlier! I bookmarked it.|
I have been absent for some time, but now I remember why I used to love this web site. Thanks, I will try and check back more frequently. How frequently you update your site?
Awesome write-up. I’m a normal visitor of your site and appreciate you taking the time to maintain the excellent site. I will be a frequent visitor for a really long time.
Valuable information. Fortunate me I discovered your web site accidentally, and I’m shocked why this accident didn’t came about earlier! I bookmarked it.
Some truly excellent info , Sword lily I observed this. “The outer conditions of a person’s life will always be found to reflect their inner beliefs.” by James Allen.
I’ve recently started a site, the info you provide on this web site has helped me greatly. Thank you for all of your time & work. “Her grandmother, as she gets older, is not fading but rather becoming more concentrated.” by Paulette Bates Alden.
What a data of un-ambiguity and preserveness of precious familiarity regarding
unpredicted feelings.
I hardly leave responses, however i did a few searching and wound up here EXERCISE – Dr Rajiv Desai.
And I do have a few questions for you if it’s allright. Could it be just me or does
it look as if like some of the remarks look like left by brain dead
individuals? 😛 And, if you are posting on other
social sites, I would like to follow everything new you have to post.
Would you list of all of your communal pages like
your Facebook page, twitter feed, or linkedin profile?
You could certainly see your skills in the work you write.
The sector hopes for even more passionate writers like you who aren’t afraid to mention how they believe.
All the time go after your heart.
Hello there! I could have sworn I’ve been to this blog before but after
reading through some of the post I realized it’s new to me.
Anyhow, I’m definitely glad I found it and I’ll be bookmarking and checking back frequently!
Pretty! This has been an extremely wonderful article.
Many thanks for supplying this info.
What’s up every one, here every one is sharing these kinds of experience, so it’s pleasant to read this weblog, and I used to pay a
quick visit this blog all the time.
Your mode of explaining the whole thing in this article is really fastidious,
every one be able to without difficulty understand it, Thanks a lot.