Dr Rajiv Desai
An Educational Blog
THE SLEEP
_
THE SLEEP
_
Prologue:
When I was working as a medical specialist in Saudi Arabia, my duty time was 7.30 am to 5 pm and additional calls at night. If I woke up at 2 am to treat a serious patient and finished work at 3 am, technically speaking I worked 1 hour extra. My Saudi boss used to say that I can come 1 hour late next day at 8.30 am as I worked previous night for 1 hour extra. It is stupid to say the least and cruel to say the most. The issue is not 1 hour night disturbance but you do not get good sleep after being woken up at midnight and your next day is spoiled due to day-time sleepiness. I am sure that medical professionals, police, military, fire brigade etc will agree with me. Even today, I am the only physician in the government hospital and therefore technically on call all nights 365 days. Even a midnight telephone call can disturb sleep. Will it affect my health and longevity? Is sleep not necessary for essential service provider? What is optimum sleep? To find answer to these questions, I decided to go into the details of sleep in humans.
_
Abbreviations and synonyms:
REM = rapid eye movement EEG = electroencephalogram
NREM = Non rapid eye movement EMG = electromyogram
Apnea = absence of breathing EOG = electrooculogram
Neuron = cell of brain PSG = polysomnogram
RAS = reticular activating system in brainstem
_
Sleep is a biological enigma. Why animals forgo eating and reproduction, while potentially increasing their risk of predation remains unknown. We spend about one-third of our lives sleeping, but exactly why we need sleep is the subject of much dispute. We spend more than 200,000 hours sleeping in a lifetime, the equivalent of more than 8,000 days. Yet research has only just begun to decode the mysteries behind what can go wrong. Sleep is an infant science in that it has not been long studied. Now, about 30 years after sleep research began, sleep researchers have uncovered relatively little knowledge of what sleep is about. However, they do occasionally unearth a gem or two of useful knowledge. Despite great progress in our understanding of the regulation and neurobiology of sleep, as well as the consequences of sleep loss on human performance, why the brain needs sleep still remains a mystery. Speculation has ranged from evolutionary theories – we need sleep to prevent us from wandering out of our caves in the dark – to theories has to do with the function of neural networks. Even today, there is no consensus about sleep among neuroscientists and sleep researchers.
_
Everybody agrees that sleep means sleeping of the brain. Obviously plants & trees do not have brain and so they do not sleep. On the other hand, animals & birds do have brains and so they sleep. Sleep is actively generated by the discharge of specific neurons in certain parts of the brain. Sleep is present throughout the animal kingdom. It has been identified in alligators, turtles, lizards, frogs, salamanders, bees, wasps, flies, dragon flies, grasshoppers, butterflies, scorpions and the primitive invertebrate sea hare. Barring occasional exception, not only do all mammals & birds sleep, but as a rule, they experience cyclical alternation between NREM and REM sleep.The question of the process and function of sleep thought the animal kingdom is truly fascinating. It’s obviously important: our bodies keep track of lost minutes of sleep and then try to make them up. The need for sleep can become irresistible even in the face of death, with many car accidents each year due to drowsy drivers. When completely deprived of sleep for too long, we sicken and die. We still don’t fully understand why sleep is so important – but we do know that it is a very active state.
_
Sleep statistics:
According to the National Sleep Foundation in the U.S., adults average 6.9 hours of sleep a night, even though many experts believe they need between 7 and 9 hours. Other studies found that most adults sleep 7 to 8 hours per night; although the timing, duration and internal structures of sleep vary among healthy individuals and as a function of age. About a third of adults in the U.S. may be getting less than seven hours of sleep per day, putting themselves at risk for serious health problems, according to two new CDC studies. It is estimated that 30 to 40% of children do not get sleep enough and over half of those over the age of 65 experience disturbed sleep. One in 10 people in the UK take medication to help them sleep, research has suggested. Analysis of the early data from Understanding Society based on 14,000 UK households found that overall best sleep was reported by people with higher levels of education and by married people. In some cultures, people have one consolidated sleep episode every night while in another culture people have a mid-afternoon nap and a shortened night sleep. Disturbed sleep is among the most frequent health complaints physicians encounter. More than 50 % population has experienced intermittent sleep disturbances which could be poor sleep at night or daytime sleepiness. However, at least 15 to 20 % of adults report chronic sleep disturbance or misalignment of circadian timing resulting in serious impediment of daytime functioning and contributes to medical problems and psychiatric conditions. More than 1,500 deaths a year are caused by drivers falling asleep at the wheel in the U.S.
_
Homo sapiens are not nocturnal animals; we don’t have good night vision and are not especially effective in darkness. Yet in an instant on the evolutionary time scale, Edison’s invention of the light bulb shifted our time-and-light environment in the nocturnal direction. At the snap of a switch, a whole range of nighttime activity opened up, and today we live in a 24-hour world that is always available for work or play. Consequently most of us now sleep less than people did a century ago, or even 50 years ago. Electric lighting and stress are the two chief culprits that have converted the natural process of sleep into a daily struggle for millions. A majority of the population inflict pain, misery and mental torture on themselves and their children by trying to regulate their sleep with alarm clocks, irrational shift-work patterns, sleeping pills, alcohol, caffeine etc.
_
Rest versus sleep:
Rest is a period of inactivity during which the faculties can restore expended nerve energy. When we create wastes faster than our body can eliminate them and deplete our energies faster than our faculties can restore them, a period of inactivity enables the body to catch up on its homework. Essentially, rest is the curtailment of energy expenditure and waste generation. This permits the body to redirect energies to cleansing and restoration. Physical and mental inactivity can be called rest. The cells of the body require rest but not necessarily sleep, but the brain and nervous system sleep. Cells require periodic rest so that they may cope with their eliminative and restorative functions. Many people are apt to confuse the words rest and sleep as being synonymous. Rest means cessation of activity. Sleep necessarily implies rest due to the immobilization of the body, but the condition of sleep exists only when consciousness has ceased. However, we should note that not all forms of unconsciousness are sleep. Coma, catalepsy and stupor must not be confused with sleep. There are many different kinds of rest. Some of them are as follows.
1) Physiological rest, during which the body and most of its faculties are inactive, as in sleep and in fasting.
2) Sensory rest, during which time the nervous system and brain are relaxed or not normally exerted, as in fasting, sleep and meditation. The eyes are closed in sleep and meditation, which curtails a great drain of energy.
3) Emotional rest, as in withdrawal from the affairs and excitants of daily life that draw upon our nerve energies.
4) Mental rest, as in avoiding those affairs that demand our attention and thoughts.
5) Relaxation as rest: To relax means to cease or decrease exertion. The word has broad connotations, and recreation or play might be called relaxation. Generally, relaxation means to let go of that which stresses the body and to undertake a course that does not tense or stress. Relaxation is a variant form of rest.
When you are sleeping, you are resting but when you are resting, you are not necessarily sleeping. I hope I made the distinction between rest and sleep clear.
_
Definition of sleep:
Sleep in humans is a naturally recurring state of rest characterized by partial or total loss of consciousness more easily reversible than stupor or coma, having a characteristic cycle of brain-wave activity that includes intervals of dreaming, relatively suspended sensory activity, inactivity of nearly all voluntary muscles with closure of eyes, a decreased ability to react to stimuli, and accompanied by an orderly sequence of electrical and chemical changes in the brain that affect the entire body and greatly alter the mind. Sleep is distinguished from other sleep-like states, for instance, stupor or coma because it is easily interrupted by external stimulation such as a loud noise. Wakefulness (consciousness) is maintained by firing of specific neurons of cerebral cortex of human brain under stimulation from neurons of the ascending reticular activating system (RAS) in the brainstem. During sleep, these specific wakefulness neurons of cerebral cortex are temporarily inhibited due to reduced firing of neurons of RAS.
_
EEG:
Scientists can record brain activity by attaching electrodes to the scalp and then connecting these electrodes to a machine called an electroencephalograph. The electroencephalogram (EEG) is the record of brain activity recorded with this machine. The wavy lines of the EEG are what most people know as “brain waves.” Our brains cycle through four main types of brain waves, referred to as delta, theta, alpha and beta. Each type of brain wave represents a different speed of oscillating electrical voltages in the brain. Beta waves are those associated with day to day wakefulness. These waves are the highest in frequency and lowest in amplitude, and also more desynchronous than other waves. That is, the waves are not very consistent in their pattern. This desynchrony makes sense given that day to day mental activity consists of many cognitive, sensory, and motor activities and experiences, and thus, when awake, we are mentally desynchronous as well. Beta waves are the fastest, cycles at 15 to 50 per second having amplitude of less than 50 microvolt. During periods of relaxation, while still awake, our brain waves become slower, increase in amplitude and become more synchronous. These types of waves are called alpha waves. Alpha waves operate at 8 to 12 cycles per second having amplitude of 50 microvolt. Such brain waves are often associated with states of relaxation and peacefulness. According to a new study, the alpha wave doesn’t disappear; it just goes undercover during sleep. Alpha wave activity decreases as people enter ever-deeper levels of sleep and increases as people cycle back into more shallow sleep stages. In study participants, the ups and downs of alpha wave activity were closely associated with how easily a person could be awoken by traffic noises, loud talking or other sounds that might be encountered in hospital or at home in a city. When alpha wave activity spiked just before a noise was played, volunteers woke up more easily than when alpha wave activity was low, the researchers found. Alpha wave activity may be the brain’s way of keeping people aware of their surroundings during sleep. Such awareness enables people to wake quickly in case of danger. Theta waves operate at 4 to 7 cycles per second having amplitude between 50 to 100 microvolt and are present in stage one when we’re in light sleep. Delta waves are the slowest having 0 to 4 cycles per second having amplitude 100 to 200 microvolt and are present in deep sleep. So one can see that as we progress from wakefulness to deep sleep, brain waves on EEG become slower, larger and synchronous.
_
EEG waves in sleep
_
Polysomnography (PSG):
PSG means recording of various parameters of a patient in sleep. Polysomnography is performed in a sleep laboratory while the patient sleeps, preferably at his or her usual sleeping time. Most sleep laboratories consist of two rooms; one with a bed for the subject, connected via a one-way window and by cables to the other, an instrument room where a technician monitors the sleeping subject (sometimes also by video). Recordings are made of electrical signals from the brain (electroencephalogram or EEG); from the eye (electrooculogram or EOG); and from the muscles (electromyogram or EMG). A polygraph is used to keep track (graph) of the several (poly) signals simultaneously. Other important bodily functions, like body temperature, breathing, heart rate, blood pressure, oxygen saturation in blood and even sex organ volume, can also be recorded. Sleep stages and other characteristics of sleep are commonly assessed by polysomnography in a specialized sleep laboratory. A single part of a polysomnogram is sometimes measured at home with portable equipment, for example oximetry, which records blood oxygen levels throughout the night. Polysomnography is not routinely used in the evaluation of patients with insomnia or circadian rhythm disorders, except as needed to rule out other disorders. It will usually be a definitive test for sleep apnea.
_
Sleep cycles & stages:
In mammals and birds, sleep is divided into two broad types: rapid eye movement (REM) and non-rapid eye movement (NREM) sleep and each of which recurs cyclically several times during a normal period of sleep. Each type has a distinct set of associated physiological, neurological, and psychological features. In the R&K sleep scoring manual, NREM sleep was divided into four stages, with slow-wave sleep comprising stages 3 and 4. In stage 3, delta waves made up less than 50% of the total wave patterns, while they made up more than 50% in stage 4. Furthermore, REM sleep was sometimes referred to as stage 5. This was reviewed by the American Academy of Sleep Medicine (AASM) which divides NREM into three stages: N1, N2, and N3, the last of which is also called delta sleep or slow-wave sleep (SWS). So N3 means stage 3 plus stage 4. Sleep proceeds in cycles of NREM and REM, the order normally being N1 to N2 to N3 to N2 to REM. The first REM sleep period usually occurs about 70 to 90 minutes after we fall asleep. There is a greater amount of deep sleep (stage N3) in the earlier sleep cycles, while the proportion of REM sleep increases in the later sleep cycles and just before natural awakening. So the cycles of stage N2 and REM sleep alternate with each other for the second half of the night. Sleep typically occurs in cycles that range from 90 to 120 minutes in length, with 4-5 cycles occurring during each night’s sleep and each sleep cycle comprise of 4 stages (N1 + N2 + N3 + REM). Each cycle begins with a relaxation phase, showing declines in brain wave (EEG) activation, muscle tone (EMG), eye movement (EOG), heart rate, breathing rate, and blood pressure, all of which typically reach a nadir after 45-60 minutes. This relaxation phase then gradually gives way to an activation phase, in which many of the brain and bodily functions resume the high levels of the awake state. In the face of this activation, sleep is maintained by the active suppression of sensory (input) signals and motor (output) commands. Over the course of the night the length and depth of the relaxation phase (which is called quiet, NREM or EEG slow-wave sleep) declines as the duration and intensity of the activation phase (called active, REM or EEG fast-wave sleep) increases. About 70-80% of an average sleep bout of 6.5-8.0 hours consists of NREM sleep, while 20-30% is REM. Each stage of sleep cycle has a distinct physiological function. If our REM sleep is disrupted one night, our bodies don’t follow the normal sleep cycle progression the next time we doze off. Instead, we often slip directly into REM sleep and go through extended periods of REM until we “catch up” on this stage of sleep.
_
PSG in wakefulness and sleep
_
NREM sleep:
According to the 2007 AASM standards, NREM consists of three stages. There is relatively little dreaming in NREM. During the deep states of NREM sleep, blood supply to the muscles is increased, energy is restored, tissue growth and repair occur, and important hormones are released for growth and development (growth hormone).
Stage N1 sleep is the stage of transition from wakefulness to deeper sleep. This is the lightest stage of sleep, and people may not always perceive they are asleep when in this stage. Stage N1 refers to the transition of the brain from alpha waves having a frequency of 8–12 Hz (common in the awake state) to theta waves having a frequency of 4–7 Hz. This stage is sometimes referred to as somnolence or drowsy sleep. Sudden twitches and hypnic jerks, also known as positive myoclonus, may be associated with the onset of sleep during N1. Some people may also experience hypnagogic hallucinations during this stage, which can be troublesome to them. During N1, the subject loses some muscle tone and most conscious awareness of the external environment.
Stage N2 is characterized by sleep spindles ranging from 11–16 Hz (most commonly 12–14 Hz) and K-complexes on EEG. During this stage, muscular activity as measured by EMG decreases, and conscious awareness of the external environment disappears. Stage N2 sleep is a true sleep state, and accounts for 40% to 50% of sleep time in adults.
Stage N3 sleep has been called deep sleep, delta sleep, or slow wave sleep (SWS). This stage accounts for about 20% of sleep in young adults. Stage N3 (deep or slow-wave sleep) is characterized by the presence of delta waves ranging from 0.5–2 Hz and having a peak-to-peak amplitude >75 microV. This is the stage in which parasomnias such as night terrors, nocturnal enuresis, sleepwalking, and somniloquy occur. Many illustrations and descriptions still show a stage 3 with 20 to 50% delta waves and a stage 4 with greater than 50% delta waves; these have been combined as stage N3.
_
REM sleep:
Infants spend about 50% of their sleep time in NREM and 50% in REM sleep. Adults spend about 20% of their sleep time in REM and 80% in NREM sleep. Elderly people spend less than 15% of their sleep time in REM sleep. Most dreaming occurs during REM sleep. During REM sleep, a person’s eyes move back and forth rapidly. Often when people in REM sleep wake up, they say that they were just dreaming. The EEG pattern during REM sleep is similar to the EEG pattern when people are awake. The criteria for REM sleep include rapid eye movements as well as a rapid low-voltage EEG. However, the muscle activity is very quiet during REM sleep. Muscles are inactive to prevent us from acting out our dreams. This also means that sleepwalkers are not in REM sleep and are not acting out their dreams. Most memorable dreaming occurs in this stage. During REM sleep, several physiological changes also take place. The heart rate and breathing quickens, the blood pressure rises, we can’t regulate our body temperature as well and our brain activity increases to the same level as when we are awake (beta). The rest of the body, however, is essentially paralyzed until we leave REM sleep. This paralysis is caused by the release of glycine an amino acid, from the brain stem onto the motor-neurons (neurons that conduct impulses outward from the brain or spinal cord to move muscles). Because REM sleep is the sleep stage at which most dreaming takes place, this paralysis could be nature’s way of making sure we don’t act out our dreams. Otherwise, if you’re sleeping next to someone who is dreaming about playing kickball, you might get kicked repeatedly while you sleep. At least in mammals, a descending muscular atonia is seen. Such paralysis may be necessary to protect organisms from self-damage through physically acting out scenes from the often-vivid dreams that occur during this stage. REM sleep is characterized by increased neuronal activity of the forebrain and midbrain, depressed muscle tone, dreaming, rapid eye movements, and vascular congestion of the sex organs.
_
PSG recording
_
EEG waves during sleep:
| Stage | Frequency (Hz) | Amplitude (micro Volts) | Waveform type |
| awake | 15-50 | <50 | beta rhythm |
| pre-sleep relaxation | 8-12 | 50 | alpha rhythm |
| 1 or N1 | 4-8 | 50-100 | theta |
| 2 or N2 | 4-15 | 50-150 | spindle waves |
| 3 or N3 | 2-4 | 100-150 | spindle waves, slow waves and delta waves 20 to 50 % |
| 4 or N3 | 0.5-2 | 100-200 | slow waves and delta waves > 50 % |
| REM | 15-30 | <50 | Similar to waking state |
Note: American Academy of Sleep Medicine (AASM) has combined stage 3 & 4 as N3.
_
Physiology of sleep:
There are billions of working cells in our brain called neurons and great variety in the kind of brain cells or neurons, with each group representing a specific cluster of functions. Neurons communicate with similar neurons by firing molecules from its nerve endings to the receiving nerve endings of the other neuron. The nerve endings of the firing part of the neuron are called axon terminals and the nerve endings of the receiving part of the neuron are called dendrites. The end of the axon terminals is called synapses. The synaptic cleft is the space where synapses and dendrites meet each other and where all the activity takes place. Each neuron is able to receive and fire molecules simultaneously. The molecules fired in the synaptic cleft are called neurotransmitters. The synapses are situated at the end of the axon terminals of the firing part of the neuron and work like “ball throwers.” The dendrites of the receiving part of the other neuron, work like “catcher’s mitts.” They use receptor-molecules, or receptors, to capture the “thrown” neurotransmitters. Once one neuron is firing neurotransmitters from its synapse to the receiving dendrite of the other neuron, it is critically important that the “mis-fired” neurotransmitter left over must be removed from the synaptic cleft. Any neurotransmitter which is not removed from the synaptic cleft prevents further neurotransmitters from getting through. Re-uptake, the process of removing neurotransmitters after firing or release, allow these neurotransmitter left over to be recycled for further use. Re-uptake is carried out by “transporter proteins” which bind to the mis-fired neurotransmitter and carry it across the plasma membrane back into the synapse of the firing neuron. There are about 50 neurotransmitters acting in a brain and more than 100,000 chemical reactions go on in your brain every second.
_
In the brain, serotonin is synthesized from the amino acid precursor “Tryptophan”. By enzymatic interaction, tryptophan converts into 5 hydroxy-tryptophan and eventually into serotonin (5 hydroxy-tryptamine). This neurotransmitter belongs to the group of serotonergic neurons which make the Serotonergic System in the brain. Levels of serotonin are highly concentrated in the Raphe nuclei of the reticular activating system (RAS) of Brainstem. From the Raphe Nuclei of the brainstem, serotonin pathways project through parts of the Limbic System (like the Thalamus and Hypothalamus) into the Forebrain. Serotonin plays an important role in sleep, appetite, memory, aggression, sexual behaviour, cardiovascular activity, respiratory activity, gastrointestinal motility, motor output, sensory and neuroendocrine function, but most important, perception. Serotonin is a modulator of both wakefulness and sleep. The effect of serotonin on wakefulness and sleep depends upon which neurons are firing, their projection sites and which postsynaptic receptors are present rather than the functional state of serotonergic system.
_
Cholinergic neurons fire the neurotransmitter “Acetylcholine.” There is a strong evidence to suggest that cholinergic neurons of the reticular activating system (RAS) in the brainstem control wakefulness under modulation of serotonergic system of RAS. Serotonergic activity gradually decreases as one becomes drowsy and enters slow-wave sleep. An overall slowing of serotonergic activity is observed during NREM sleep. This slowing of serotonergic system along with melatonin activates GABA (gamma amino-butyric acid) system in basal forebrain which suppresses activities of cerebral cortex to produce NREM sleep. During REM sleep, serotonergic activity falls completely silent. While during REM sleep the serotonergic neurons in the brainstem are “off” (silent), cholinergic neurons in the brainstem are “on” (firing)! Acetylcholine not only plays an important role in dreaming, but also in long-term memory processes. In the brainstem, the cholinergic “REM-on” neurons can only trigger REM sleep (and thus dreaming) when the serotonergic “REM-off” neurons are inactive. This happens because in the brainstem, the serotonergic neurons inhibit the cholinergic neurons whilst we are awake. When in brainstem the serotonergic neurons become inactive, only then, the cholinergic brainstem neurons will be able to get active, triggering the REM-dream sleep. Both the REM-on and the REM-off cells are localized in the brainstem. These brainstem mechanisms work as an “oscillator”, which controls the transitions from waking to sleeping and further controls the REM/non-REM cycle, which occurs 4 to 5 times during sleep.
_
The part of the brain most important in regulating sleep duration is the hypothalamus. Certain groups of hypothalamic neurons and adjacent groups of basal forebrain neurons produce the neurotransmitter GABA. Projections of these GABA neurons inhibit the firing of cells involved in wakefulness. Besides GABA neurons, several other groups of neurons have been shown to be inhibit the firing of cells involved in wakefulness including neurons containing histamine, norepinephrine, serotonin, hypocretin, and glutamate–and this inhibition promotes sleep. Hypocretin (also called orexin) was discovered in 1998, and its role in sleep and narcolepsy was identified in 2001.
_
The stress hormones “Cortisol” & “Adrenaline” (Epinephrine) in the brain and body are triggered by increased serotonergic activity. These released hormones, cortisol and adrenaline, are secreted from the “Adrenal Glands.” They give the human personality a boost and energy to work in wakeful state. So cortisol level is high when person wakes up.
_
What happens when the brain is awake?
The cholinergic cells of the ascending reticular activating system (RAS) of brainstem are active, so they facilitate sensory thalamus and inhibit the reticular nucleus. The inhibition of the reticular nucleus actually excites the sensory thalamus as well. As a result the thalamus lets all sensory information through, and cerebral cortex is highly active and desynchronized dealing with all the input. The adrenergic and dopaminergic neurons directly stimulate cerebral cortex under effect of cholinergic neurons of RAS being modulated by serotonergic system of RAS. So you need activities of both cholinergic and serotonergic neurons of RAS to remain awake. This is how our so called wakefulness (consciousness) is maintained by stimulation of cerebral cortex by RAS of brainstem.
_
What happens when the brain is asleep?
Now the cholinergic cells of the RAS is quiet, so sensory thalamus is not particularly sensitive. In addition, the reticular nucleus is freed from inhibition, so it can inhibit the sensory thalamus. The net effect is that thalamus is very insensitive to sensory stimuli, the gate is closed, and the cortex can rest. An interesting property of the thalamic neurons is that when hyperpolarized, they have slow intrinsic waves of activity, similar to the pacemaker of the heart. This activity may be the source of the slow synchronous pattern of the sleeping EEG. It also may function to keep the cortex in shape, ensuring that even when you are asleep the cortical neurons are active. The slowing of serotonergic system along with release of melatonin leads to activation of GABA system in basal forebrain to produce NREM. The GABA system also stimulates anterior pituitary to produce growth hormone. Dreaming occurs during REM sleep when the ascending cholinergic system again turns on and stimulates cerebral cortex simulating wakefulness with eye movements & vivid dreams. However, person is not conscious despite active cholinergic system bombardment of cortex during REM sleep due to inactivity of serotonergic system of RAS which keep consciousness suppressed.
| AWAKE | ASLEEP |
| Cholinergic system active in RAS
Modulatory effects of serotonergic system Release of catecholamine and cortisol |
Cholinergic system inactive except in REM Serotonergic system inactive in RAS GABA system active in basal forebrain neurons for NREM No release of catecholamine and cortisol |
| sensory thalamus facilitated | sensory thalamus inhibited |
| reticular nucleus inhibited | reticular nucleus active |
| thalamocortical neurons active | thalamocortical neurons in slow rhythm |
| EEG desynchronous | EEG synchronous |
So these two states, wakefulness and sleep are merely the endpoints of a single continuum. Sleep, in particular deep sleep, has an inhibiting influence on the hypothalamic-pituitary-adrenal (HPA) axis, whereas activation of the HPA axis or administration of glucocorticoids can lead to arousal and sleeplessness. Insomnia, the most common sleep disorder, is associated with a 24-hour increase of corticotropin and cortisol secretion, consistent with a disorder of central nervous system hyperarousal. Sleepiness and fatigue are very prevalent in the general population, and recent studies have demonstrated that the proinflammatory cytokines interleukin-6 (IL-6) or tumor necrosis factor (TNF-alfa) are elevated in disorders associated with excessive daytime sleepiness, such as sleep apnea, narcolepsy, and idiopathic hypersomnia. Sleep deprivation leads to sleepiness and daytime hypersecretion of IL-6. Combined, these findings suggest that the HPA axis stimulates arousal whereas IL-6 and TNF-alfa are possible mediators of excessive daytime sleepiness in humans. Dextroamphetamine which enhance catecholamine and dopaminergic activity, increase sleep latency, decrease total sleep time, and greatly reduce REM sleep. The REM sleep reduction effect is due to increased wakefulness, in contrast to drugs which primarily alter noradrenergic or serotonergic activity, in which REM sleep reduction occurs regardless of changes in total sleep or wakefulness. Many antidepressants suppress REM sleep because, for REM sleep to occur, you need absent serotonergic activities in RAS but SSRI antidepressants increase serotonin level in RAS. Since sleep and wakefulness are influenced by different neurotransmitter signals in the brain, foods & medicines that change the balance of these signals affect whether we feel alert or drowsy and how well we sleep. Drugs such as diet pills and decongestants stimulate some parts of the brain and can cause insomnia, or an inability to sleep.
_
Sleep and smoking (nicotine):
Heavy smokers often sleep very lightly and have reduced amounts of REM sleep. Nicotine enhances attention and vigilance by directly stimulating cholinergic neurotransmission in the basal forebrain responsible for cortical arousal. Smokers also tend to wake up after 3 or 4 hours of sleep due to nicotine withdrawal.
_
Sleep and caffeine:
Caffeine, the most widely consumed psychoactive substance in the world, increases wakefulness by stimulating neurons (notably cholinergic) involved in the maintenance of arousal, by inhibiting neurons (notably GABA-nergic) involved in the promotion of sleep. Adenosine reception is important to sleep, and especially to deep sleep. Caffeine blocks adenosine reception so you feel alert. It injects adrenaline into the system to give you a boost. And it manipulates dopamine production to make you feel good. The half-life of caffeine in your body is about six hours. That means that if you consume a big cup of coffee with 200 mg of caffeine in it at 3:00 p.m., by 9:00 p.m. about 100 mg of that caffeine is still in your system. You may be able to fall asleep, but your body will probably miss out on the benefits of deep sleep. Sources of caffeine include coffee, chocolate, soft drinks, non-herbal teas, diet drugs, and some pain relievers.
_
Sleep and alcohol:
Many insomniacs take a drink of whiskey or wine before bedtime in order to reduce sleep latency. While alcohol does reduce sleep latency and help people fall into light sleep, it also robs them of REM and the deeper, more restorative stages of sleep. Instead, it keeps them in the lighter stages of sleep, from which they can be awakened easily. So alcoholism is associated with frequent awakenings and a decrease in subjective sleep quality associated with daytime fatigue. It is not known whether any impairment of sleep quality occurs when small amounts are used at bedtime. There’s a connection between obstructive sleep apnea and alcohol consumption. Drinkers can experience apnea if only for a night. Alcohol impairs breathing in sleep by relaxing the throat muscles and it affects the brain’s breathing center by masking the effect of low oxygen levels in the bloodstream, possibly damaging tissue. Even people who normally don’t snore do so if they have been drinking the night before. Snorers without apnea can exhibit apnea symptoms if they have been drinking.
_
Sleep timing and human biological clock:
Human biological clock
_
Sleep timing is controlled by the circadian clock, sleep-wake homeostasis, and in humans, within certain bounds, willed behavior. In humans, sleepiness occurs as the circadian element causes the release of the hormone melatonin and a gradual decrease in core body temperature. The timing is affected by one’s chronotype. It is the circadian rhythm that determines the ideal timing of a correctly structured and restorative sleep episode. Homeostatic sleep propensity (the need for sleep as a function of the amount of time elapsed since the last adequate sleep episode) must be balanced against the circadian element for satisfactory sleep. Along with corresponding messages from the circadian clock, this tells the body it needs to sleep. Sleep offset (awakening) is primarily determined by circadian rhythm. A person who regularly awakens at an early hour will generally not be able to sleep much later than his or her normal waking time, even if moderately sleep-deprived.
_
Circadian component:
Picture illustrating the influence of light and darkness on circadian rhythms and related physiology and behaviour through the suprachiasmatic nucleus in humans.
_
A circadian rhythm is an endogenously driven roughly 24-hour cycle in biochemical, physiological, or behavioural processes. Circadian rhythms have been widely observed, in plants, animals, fungi and cyanobacteria. The term “circadian” comes from the Latin circa, meaning “around”, and diem meaning “day”. Circadian rhythmicity is present in the sleeping and feeding patterns of animals, including human beings. There are also clear patterns of core body temperature, brain wave activity, hormone production, cell regeneration and other biological activities. The rhythm is linked to the light–dark cycle. The photoperiodism, the physiological reaction of organisms to the length of day or night, is vital to both plants and animals, and the circadian system plays a role in the measurement and interpretation of day length. The human biological clock for circadian cycle/rhythm is evolved to match light/dark cycle of day/night. Circadian rhythms are controlled by a master biological clock. The primary circadian “clock” in mammals is located in the suprachiasmatic nucleus (or nuclei) (SCN), a pair of distinct groups of cells located in the hypothalamus. The retina contains specialized ganglion cells which are directly photosensitive, and project directly to the SCN where they help in the entrainment of this master circadian clock. The SCN takes the information on the lengths of the day and night from the retina, interprets it, and passes it on to the pineal gland. In response, the pineal secretes the hormone melatonin. Secretion of melatonin peaks at night and ebbs during the day and its presence provides information about night-length. The circadian rhythms of humans can be entrained to slightly shorter and longer periods than the Earth’s 24 hours.
_
At the subcellular level of organization, circadian rhythms are generated by transcriptional and translational feedback loops involving multiple clock genes. The precise periodicity (or cycle length) of the biological clock is known to be genetically determined, and variation in clock genes is thought to be related to individual differences in natural wake and sleep times. Sleep duration is affected by the gene DEC2. Some people have a mutation of this gene; they sleep two hours less than normal. Researchers at the University of California, San Francisco discovered that people having this gene enables them to do well on 6 hours of sleep a night. But the gene is very rare, appearing in less than 3% of the population. For the other 97% of us, six hours doesn’t come close to cutting it.
_
The biological clock generates and maintains circadian rhythms in most physiological, biochemical, and behavioral variables including core body temperature, triacylglycerol, blood pressure, sleep-wakefulness, alertness and mental performance. It is also responsible for the synthesis and secretion of many hormones including growth hormone, cortisol, prolactin and melatonin. Absence of light stimulates melatonin which promotes sleep & stimulates growth hormone and reactivation of serotonergic system at the end of sleep stimulates cortisol and catecholamine on awakening. So no light means melatonin & growth hormone in sleep at night and light means cortisol and catecholamine in a day for human activities. For humans who rely on vision for activities, these day-hormones increase alertness and energy availability during the daylight hours, but animals (like rats) that rely more on smell than on vision are active at night and sleep in the daytime. However, in very hot climates humans may also shift their activity into the darker, cooler night and therefore need to have a siesta during the forbiddingly hot period of the early afternoon. A close interaction exists between the sleep-wake, melatonin, core temperature, blood pressure, immune and hormonal rhythms leading to optimization of the internal temporal order. The classic phase markers for measuring the timing of human circadian rhythm are: melatonin secretion by the pineal gland, core body temperature and plasma level of cortisol.
_
Melatonin:
Melatonin synthesis
_
Melatonin is related to the mechanism by which some amphibians and reptiles change the color of their skin and, indeed, it was in this connection the substance first was discovered. Melatonin is N-acetyl-5-methoxy-tryptamine, a derivative of the amino acid tryptophan, which also has other functions in the central nervous system. Tryptophan is converted into 5 hydroxy-tryptophan which is converted into serotonin (5 hydroxy-tryptamine) and serotonin is converted into melatonin in pineal gland. The production of melatonin by the pineal gland is stimulated by darkness and inhibited by light. Photosensitive cells in the retina detect light and directly signal the SCN, entraining its rhythm to the 24-hour cycle in nature. Fibers project from the SCN to the paraventricular nuclei (PVN), which relay the circadian signals to the spinal cord and out via the sympathetic system to superior cervical ganglia (SCG), and from there into the pineal gland. Thus, the pineal gland is similar to the adrenal medulla in the sense that it transduces signals from the sympathetic nervous system into a hormonal signal. It is principally blue light, around 460 to 480nm wavelength, which suppresses melatonin, increasingly with increased light intensity and length of exposure. Melatonin has been called the body’s own natural sleeping pill. It plays a key role in the sleep cycle by helping you fall asleep. Low melatonin levels can cause sleep-onset insomnia. Melatonin is stored in the pineal gland inside the brain. The pineal gland releases melatonin only during times when the level of light is low. Practically speaking, this means that melatonin is secreted only at night, while you are asleep. In the morning, when you open your eyes, the presence of light is a sign to your brain to shut down the melatonin production. The duration of melatonin secretion each day is directly proportional to the length of the night. Melatonin functions as synchronizer of the biological clock for circadian rhythm. Use of blue-blocking goggles the last hours before bedtime has also been advised for people who need to adjust to an earlier bedtime, as melatonin promotes sleepiness.
_
However, it appears that the sleep- promoting effects of melatonin are most apparent only if a person’s melatonin levels are low.This is the really important thing you should understand about melatonin: Melatonin is a sleep and body clock regulator, not a sleep initiator. Melatonin works with your biological clock by telling your brain when it is time to sleep. Melatonin does not increase your sleep drive or need for sleep. Melatonin is produced primarily in darkness and inhibited by light. The levels of your melatonin increase in the middle of the night and gradually fall as the night turns to morning, so exposure to light before bed can push your biological clock in the wrong direction, making melatonin ineffective. Melatonin treats Circadian Rhythm Disorders (where you sleep the right amount of minutes but your body clock is at the wrong time), jet lag, Shift Work Sleep Disorders and early morning awakenings — all things that deal with the timing of your need to sleep. Melatonin is not considered an effective treatment for insomnia.
_
Melatonin exerts hypnotic properties by numerous mechanisms:
1) Through its specific receptors
2) Reducing body heat and temperature
3) Through its acetylated metabolites
4) By acting on GABA receptors
5) By regulating the cycle of motor activity and rest.
_
Melatonin, which is secreted only in total darkness, also stimulates the nighttime release of another equally valuable hormone — growth hormone. Another great benefit of sleep is the nightly release of growth hormone. Growth hormone is vital for normal development of children, but it has wonderfully beneficial effects in adults as well: Growth hormone is released from your pituitary gland just as you enter the deep sleep part of your normal sleep cycle and does wonders.
1) Makes your bones stronger
2) Increases your muscle mass through the creation of new muscle cells
3) Promotes lipolysis, which helps you lose body fat
4) Increases protein synthesis and stimulates optimal maintenance of all internal organ
5) Supports your pancreas’ ability to make insulin
6) Stimulates your immune system.
All together, growth hormone makes you look and feel younger.
_
Your circadian rhythm evolved over hundreds of generations to align your physiology with your environment. Your body clock is “set” to sleep at night and stay awake during daylight hours, just like your ancestors did. Humans were absolutely designed to synchronize their sleep/wake patterns with sunlight. However, we developed the ability to bypass these normal rhythms with the invention of the electric light bulb about 100 years ago. With the help of the light bulb, many of us are violating this important sleep cycle. Very few people appreciate the importance of getting to bed early, ideally before 9 p.m., and then sleeping long enough to ensure a good night’s sleep.
_
Sleepiness comes back to us in cycles which are usually about one day long. In an average case, the maximum sleepiness comes in the middle of the night, reaches the minimum at awakening, and again increases slightly at siesta time in the afternoon. However, the circadian sleepiness is often shifted in phase as compared with your desired sleep time. Consequently, if your maximum sleepiness comes in the morning (e.g. jet lag), you may find it difficult to fall asleep late in the evening, even if you missed a lot of sleep on the preceding day. In other words, the optimum timing of your sleep should take into consideration your circadian rhythm. Circadian component correlates negatively with temperature, ACTH, cortisol, and catecholamines; and positively with melatonin and NREM propensity. By these means sleep is also tied to the rhythm of body temperature, such that sleep occurs as body temperature falls and waking occurs when body temperature is highest.
The figure above shows the time required to fall asleep during the day: after long sleep, normal sleep and a sleepless night.
_
Sleepiness is a basic physiological need state which can be likened to hunger or thirst. As with hunger or thirst, the deprivation of sleep induces sleepiness and sleep reverses this need state. The presence and intensity of sleepiness, like hunger or thirst, are inferred by how readily its onset occurs, how easily it is disrupted, and how long it endures. Normally, severe deprivation states do not routinely regulate eating, drinking, or sleeping. Other factors (i.e., taste, smell, time-of-day, social and other biological variables) modulate these behaviors much before severe deprivation states develop.
_
Homeostatic component:
Sleepiness increases with the length of time we stay awake. Homeostasis is the term that refers to maintaining equilibrium or balance in physiological and metabolic functions. The longer you stay awake, the more you learn, the more you think, the higher your tendency to fall asleep. On the other hand; caffeine, stress, exercise and other factors may temporarily reduce your sleepiness. The homeostatic mechanism prepares you for sleep after a long day of intellectual work. At the same time it prevents you from falling asleep in emergencies. Adenosine signals the brain when it needs sleep. Adenosine triphospate (ATP) releases energy to fuel reactions. With each burst of energy, ATP loses it triphospate molecule, and the adenosine binds to receptors. Rising levels of adenosine signal the brain it needs rest. When we are awake and active, we burn ATP, which breaks down to adenosine. Over time, adenosine levels build up, causing pressure for sleep. During sleep, many of the body’s cells are less active and hence burn less ATP, so adenosine levels fall again, setting the stage for wakefulness. The adenosine cycle explains the homeostatic drive for sleep—the longer we are awake, the greater our fatigue, and pressure to sleep builds up progressively. A drug like caffeine, however, partially blocks adenosine receptors, so the brain doesn’t perceive the actual adenosine level, and we don’t get tired. Adenosine-related homeostatic sleep propensity increases in proportion to mental effort and can be partially cleared by caffeine, stress, etc. Scientists think that the build-up of adenosine during wakefulness may promote the “drive to sleep.” As long as we are awake, adenosine accumulates and remains high. During sleep, the body has a chance to clear adenosine from the system, and, as a result, we feel more alert when we wake.
_
Only the superposition of these two components determines the optimum time for sleep. Most importantly, you should remember that even strong sleepiness resulting from the homeostatic component may not be sufficient to get good sleep if the timing goes against the sleep-high in the circadian component. High quality night sleep means combination of strong homeostatic sleepiness and strong circadian sleepiness. Strong homeostatic sleepiness means going to sleep not earlier than 15-19 hours after awakening from the previous night sleep and strong circadian sleepiness means going to sleep at a time of day when you usually experience a rapid increase in drowsiness. Not earlier and not later! Free running sleep is a sleep that comes naturally at the time when it is internally triggered by the combination of your homeostatic and circadian components. In other words, free running sleep occurs when you go to sleep only then when you are truly sleepy (independent of the relationship of this moment to the actual time of day). People with irregular sleep hours and highly stressful lives may simply be unable to locate the point of strong circadian sleepiness as this point may not exist!
| High circadian sleepiness | Low circadian sleepiness | |
| High homeostatic sleepiness | Peak of the night: You are very drowsy and fall into refreshing sleep with latency of less than five minutes | Insomnia: You are tossing and turning in bed. You are very tired but you cannot fall asleep. Your temperature, blood pressure and pulse are raised. Your thoughts are racing
Solution: Wait for the arrival of the circadian phase. Delay going to sleep by 3-6 hours |
| Low homeostatic sleepiness | Hypersomnia: You are drowsy throughout the day despite long sleep hours. Napping does not help. You show minimum energy levels. Your muscles are weak and atonic
Solution: Adjust your sleep phase to your circadian (e.g. try to go to sleep 3-6 hours later) |
Peak of the day: You are alert, energetic, and full of new ideas |
Optimizing the timing of brainwork with respect to the circadian cycle. The horizontal axis expresses the number of hours from awakening (note that the free running rhythm period is often longer than 24 hours). Homeostatic sleepiness can roughly be expressed as the ability to initiate sleep. Circadian sleepiness can roughly be expressed as the ability to maintain sleep. Optimum timing of brainwork requires both low homeostatic and circadian sleepiness. There are two quality alertness blocks during the day: first after the awakening and second after the siesta. Both are marked yellow in the graph. For best learning and best creative results use these yellow blocks. Caffeine can only be used to enhance alertness early in this optimum window (brown color). Later use will affect sleep (caffeine half-life is about six hours). Note that this data refer solely to free running sleep. If you use an alarm clock to regulate your sleep timing, these measurements may not apply! In addition, timing and the amplitude of changes differ between individuals.
_
A circadian pacemaker (clock) located in the suprachiasmatic nuclei (SCN), and a sleep homeostat located outside the SCN, are two major determinants of the timing of the human sleep-wake cycle and sleep structure. The oscillation of the sleep homeostat is strongly, and maybe exclusively, determined by the sleep-wake cycle. Light input to the circadian clock is mediated by circadian photoreception. The sleep-wake cycle is a major determinant of light input to the clock. The sleep-wake cycle is normally timed to occur at a specific phase relative to the external cycle of light-dark exposure. It is also timed at a specific phase relative to internal circadian rhythms, such as the pineal melatonin rhythm, the circadian sleep-wake propensity rhythm, and the rhythm of responsiveness of the circadian pacemaker to light. Variations in these internal and external phase relationships, such as those that occur in blindness, aging, morning & evening, and advanced & delayed sleep-phase syndrome, lead to sleep disruptions and complaints. Alterations in these processes and their interactions may lead to sleep and wakefulness occurring at abnormal clock times (altered external timing) and/or out of phase with endogenous circadian rhythms (altered internal timing).
_
Jet lag is a physiological condition which results from alterations to the body’s circadian rhythms while traveling across a number of time zones as on a jet plane. A time zone is a geographical region which has the same time everywhere within it. The world has 24 time zones, one for each hour in the day. Each zone runs from north to south in strips that are approximately 1,000 miles (1,600 kilometers) wide. As the earth rotates, dawn occurs at a set hour in one time zone, then an hour later in the time zone immediately to the west and so on through the 24-hour cycle. The cause of jet lag is the inability of the body of a traveler to immediately adjust to the time in a different zone. For instance, if you travel from California to New York, you “lose” 3 hours according to your body’s clock. You will feel tired when the alarm rings at 8 a.m. the next morning because, according to your body’s clock, it is still 5 a.m. As the body struggles to cope with the new schedule, temporary insomnia, fatigue, irritability, and an impaired ability to concentrate may set in. It usually takes several days for your body’s cycles to adjust to the new time.
_
Symptoms much like jet lag are common in people who work nights or who perform shift work. Attempts to sleep at inappropriate phases of the circadian cycle will usually result in shorter sleep episodes and more awakenings. Such attempts are frequent in workers on night shifts. The investigators compare the short-term effects of shift work to symptoms of jet lag, such as daytime sleepiness, disturbed sleep, gastrointestinal problems and blunted alertness. The difference is that travelers will eventually adapt to their environment, while shift workers live out of synch with their daily surroundings. And over time this may take a toll. Because these people’s work schedules are at odds with powerful sleep-regulating cues like sunlight, they often become uncontrollably drowsy during work, and they may suffer insomnia or other problems when they try to sleep. Shift workers have an increased risk of heart problems, digestive disturbances, and emotional and mental problems, all of which may be related to their sleeping problems. The number and severity of workplace accidents also tend to increase during the night shift. Major industrial accidents attributed partly to errors made by fatigued night-shift workers include the Exxon Valdez oil spill and the Three Mile Island & Chernobyl nuclear power plant accidents. One study also found that medical interns working on the night shift are twice as likely as others to misinterpret hospital test records, which could endanger their patients. A number of studies indicate shift workers face a higher risk of heart disease — possibly due to the metabolic effects of working and sleeping unusual hours. There is also a price for society. For one, sleep loss may make shift workers less productive. And accidents that stem from sleepiness, such as car accidents, exact a high cost. According to the researchers, “sleepiness-related accidents” cost the U.S. about $16 billion a year. Employers and individuals need to be aware of the major performance and alertness decrements associated with night activity and how to best manage and counteract them.
_
Many people with total blindness experience life-long sleeping problems because their retinas are unable to detect light. These people have a kind of permanent jet lag and periodic insomnia because their circadian rhythms follow their innate cycle rather than a 24-hour one. Daily supplements of melatonin may improve night-time sleep for such patients. However, since the high doses of melatonin found in most supplements can build up in the body, long-term use of this substance may create new problems.
_
Evolution and sleep:
Much has been learned about sleep from laboratory studies of non-human animals. For example, the diversity of sleep behaviour increases as the brain becomes more and more specialized during evolution. Below the level of the reptiles (who have clear-cut NREM sleep but not REM), it is difficult to distinguish sleep from simple inactivity. REM sleep first appears in birds and then only fleetingly, because while hatchlings have it in abundance, adults have little or none. REM sleep is first clearly and enduringly seen in mammals, suggesting a relationship to the two features which distinguish that class of animal: large, highly developed brains and the capacity for strong internal temperature control.
_
Anthropology of sleep:
Research suggests that sleep patterns vary significantly across cultures. The most striking differences are between societies that have plentiful sources of artificial light and ones that do not. The primary difference appears to be that pre-light cultures have more broken-up sleep patterns. For example, people might go to sleep far sooner after the sun sets, but then wake up several times throughout the night, punctuating their sleep with periods of wakefulness, perhaps lasting several hours. Plentiful artificial light has been available in the industrialized West since at least the mid-19th century, and sleep patterns have changed significantly everywhere that lighting has been introduced. In general, people sleep in a more concentrated burst through the night, going to sleep much later, although this is not always true. In almost all societies, sleeping partners are strongly regulated by social standards. For example, people might only sleep with their immediate family, extended family, spouses, their children, children of a certain age, children of specific gender, peers of a certain gender, friends, peers of equal social rank, or with no one at all. Sleep may be an actively social time, depending on the sleep groupings, with no constraints on noise or activity. People sleep in a variety of locations. Some sleep directly on the ground; others on a skin or blanket; others sleep on platforms or beds. Some sleep with blankets, some with pillows, some with simple headrests, and some with no head support. These choices are shaped by a variety of factors, such as climate, protection from intruders, housing type, technology, and the incidence of pests.
_
Alarm clock:
You may often notice that waking up with an alarm clock gives you a quick start into a day. You may then come to believe that using the alarm clock might help you keep alert later during the day. This is not the case. The alarm signal simply scares your brain into wakefulness disrupting the carefully planned system for memory consolidation. As a result, you get an immediate injection of adrenaline and your levels of ACTH and cortisol also increase. This is the same cortisol that peaks at awakening in natural sleeping rhythm that provides you with the fresh-mind impression. With passing time, this cheaply gained alertness will wear thin unless you continue abusing your physiology with more “remedies”. You may use more scare tactics for keeping yourself alert, abuse caffeine, or even get a more profound effect with cocaine. Alertness should be achieved via sufficient sleep, not despite the lack of sleep! Apart from your reduced ability to learn new things, all unnatural anti-drowsiness methods will produce a great deal of side effects that can be pretty damaging to your health in the long run.
_
Optimum sleep in humans:
Human ‘sleep need’ can vary by age and among individuals, and sleep is considered to be adequate when an individual wakes up feeling rested, refreshed and when there is no daytime sleepiness or dysfunction. Children need more sleep per day in order to develop and function properly: up to 18 hours for newborn babies, with a declining rate as a child ages. A newborn baby spends almost 9 hours a day in REM sleep. By the age of five or so, only slightly over two hours is spent in REM. The physiological signature of aging is reduced and fragmented sleep, often involving an inability to fall asleep quickly, getting up throughout the night, and early morning awakenings.
_
The optimal amount of sleep is not a meaningful concept unless the timing of that sleep is seen in relation to an individual’s circadian rhythms. A person’s major sleep episode is relatively inefficient and inadequate when it occurs at the “wrong” time of day; one should be asleep at least six hours before the lowest body temperature. The timing is correct when the following two circadian markers occur after the middle of the sleep episode and before awakening.
1) Maximum concentration of the hormone melatonin
2) Minimum core body temperature.
_
Sleep from infancy to adulthood
| Age and condition | Average amount of sleep per day |
| Newborn | up to 18 hours |
| 1–12 months | 14–18 hours |
| 1–3 years | 12–15 hours |
| 3–5 years | 11–13 hours |
| 5–12 years | 9–11 hours |
| Adolescents | 9–10 hours |
| Adults, including elderly | 7–8 hours |
| Pregnant women | 8(+) hours |
_
Individuals also show marked differences in sleep behaviour. Most of us lie between two extreme ends of a bell-shaped curve of sleep length and efficiency. At one end are the short-sleepers, who need as few as 3-5 hours, and at the other are long-sleepers, who need 8-11 hours to feel rested and refreshed by sleep. Short-sleepers tend to be energetic, active, and productive, while long-sleepers tend to be lethargic, sedentary, and reflective. Society, with its interest in tight schedules and productivity, is kind to short-sleepers but merciless to long-sleepers. Long-sleepers are ill-advised to seek professions like medical profession which greatly curtail sleep.
_
Many mammals sleep for a large proportion of each 24-hour period when they are very young. However, killer whales and some dolphins do not sleep during the first month of life. Such differences may be explained by the ability of land-mammal newborns to be easily protected by parents while sleeping, while marine animals must, even while very young, be more continuously vigilant for predators. The duration of sleep among species is, in general, inversely related to animal size and directly related to basal metabolic rate. Rats with a very high basal metabolic rate (BMR) sleep for up to 14 hours a day, whereas elephants and giraffes with lower BMR sleep only 3–4 hours per day. Herbivores, who require a long waking period to gather and consume their diet, typically sleep less each day than similarly sized carnivores, who might well consume several days’ supply of meat in a sitting. Horses and other herbivorous ungulates can sleep while standing, but must necessarily lie down for REM sleep (which causes muscular atony) for short periods. Giraffes, for example, only need to lie down for REM sleep for a few minutes at a time.
_
Variability of sleep duration, sleep timing and sleep posture in birds & animals:
Total Daily Sleep Time (in hours)
Giraffe 1.9
Roe deer 3.09
Asiatic elephant 3.1
Pilot whale 5.3
Human 8.0
Baboon 9.4
Domestic cat 12.5
Laboratory rat 13.0
Lion 13.5
Bats 19.9
Humans sleep in night, wake in the day (diurnal).
Mice sleep in day, wake at night (nocturnal).
Cows sleep with eyes open.
Horses sleep standing.
Bats sleep upside down.
Seals/ Hippos sleep underwater (part of the time).
Dolphins/porpoises sleep with one half of the brain at a time to allow breathing while swimming/sleeping.
Ducks/pigeons sleep with one half of the brain while keeping one eye on predators.
Migratory birds sleep while flying across the ocean.
Various theories were proposed for variability of sleep time & posture in animals depending on whether animal is prey or predator, whether animal size is large or small but none of them were consistently logical. There is also variability of REM and NREM sleep among animals & birds.
_
Why sleep exists?
It has been pointed out that, if sleep was not essential, one would expect to find
1) Animal species that do not sleep at all
2) Animals that do not need recovery sleep when they stay awake longer than usual
3) Animals that suffer no serious consequences as a result of lack of sleep
No animals with viable functioning brain have been found to date that satisfy any of these criteria. In fact some varieties of shark, such as great whites and hammerheads, must remain in motion at all times to move oxygenated water over their gills, they still “sleep” by deactivating one cerebral hemisphere at a time ( making sleep half a brain at a time).
_
Although scientists are still trying to learn exactly why people need sleep, animal studies show that sleep is necessary for survival. For example, while rats normally live for two to three years, those deprived of REM sleep survive only about 5 weeks on average, and rats deprived of all sleep stages live for only about 3 weeks.
_
By unfolding the mystery of sleep through science, sleep researchers have discovered that:
1) You can die from sleep deprivation, just like you can die from being deprived of food.
2) A single night of sleeping only four to six hours can impact your ability to think clearly the next day.
3) Good sleepers and poor sleepers experience about the same number of daily minor stressful events, but good sleepers are less disturbed by them. Poor sleepers experience both their minor and major life events as being more negative than do those who sleep well.
4) Sleep deprivation can cause changes in your brain activity similar to those experienced by people with psychiatric disorders.
5) Sleep deprivation puts your body into a pre-diabetic state, and makes you feel hungry, even if you’ve already eaten.
6) Interrupted sleep can significantly weaken your immune system
7) Tumors grow two to three times faster in laboratory animals with severe sleep dysfunctions.
_
Various theories have been put forward for the existence of sleep:
1) Inactivity Theory:
One of the earliest theories of sleep, sometimes called the adaptive or evolutionary theory, suggests that inactivity at night is an adaptation that served a survival function by keeping organisms out of harm’s way at times when they would be particularly vulnerable. The theory suggests that animals that were able to stay still and quiet during these periods of vulnerability had an advantage over other animals that remained active. These animals did not have accidents during activities in the dark, for example, and were not killed by predators. Through natural selection, this behavioral strategy presumably evolved to become what we now recognize as sleep. A simple counter-argument to this theory is that it is always safer to remain conscious in order to be able to react to an emergency (even if lying still in the dark at night). Thus, there does not seem to be any advantage of being unconscious and asleep if safety is paramount.
_
2) Energy conservation:
Research has shown that energy metabolism is significantly reduced during sleep (by as much as 10 percent in humans and even more in other species). For example, both body temperature and caloric demand decrease during sleep, as compared to wakefulness. However, energy conservation may not be the purpose of sleep because a sedentary nonsleeping animal is more likely to survive predators, while still preserving energy. Another example is of hibernating animals waking up from hibernation go into rebound sleep because of lack of sleep during the hibernation period. They are definitely well-rested and are conserving energy during hibernation, but still need sleep for something else.
_
3) Restoration:
The arguments which support restorative function of sleep include
A) Wound healing has been shown to be affected by sleep.
B) It has been suggested that mammalian species which invest in longer sleep times are investing in the immune system, as species with the longer sleep times have higher white blood cell counts.
C) It has been shown that sleep – more specifically, slow-wave sleep (SWS) – does affect growth hormone levels in adult men. During eight hours’ sleep, researchers found that the men with a high percentage of SWS (average 24%) also had high growth hormone secretion, while subjects with a low percentage of SWS (average 9%) had low growth hormone secretion.
D) The metabolic phase during sleep is anabolic; anabolic hormones such as growth hormones (as mentioned above) are secreted preferentially during sleep.
_
4) Brain plasticity theory, memory and learning:
One of the most recent and compelling explanations for why we sleep is based on findings that sleep is correlated to changes in the structure and organization of the brain. This phenomenon, known as brain plasticity, is not entirely understood, but its connection to sleep has several critical implications. It is becoming clear, for example, that sleep plays a critical role in brain development in infants and young children. Sleep in early life does play crucial role in brain development. A recent study found direct evidence that sleep and sleep loss modify experience-dependent changes in synaptic plasticity & synaptic circuits in brain, and neuronal connections are remodeled during sleep. The main reason why infants sleep as much as three times the amount of sleep in human adults is the need for the development of brain. Various studies have shown that REM sleep functions as a protective state during early Central Nervous System (CNS) development and prevent apoptosis (programmed cell death) of brain cells in infants. Studies investigating the effects of deprivation of active sleep have shown that deprivation early in life can result in behavioral problems, permanent sleep disruption, decreased brain mass, and an abnormal amount of neuronal cell death. A link between sleep and brain plasticity is becoming clear in adults as well. This is seen in the effect that sleep and sleep deprivation have on people’s ability to learn and perform a variety of tasks.
_
Memory is the cognitive process whereby past experiences, learning and recognition are recalled. Memory “formation” is a product of brain plasticity, the structural changes within synapses that create associations between stimuli. Synaptic plasticity can be described as the changing in strength between two related neurons. Regional brain measurements in neo-natal REM sleep deprived rats displayed a significant size reduction in areas such as the cerebral cortex and the brain stem. The rats were deprived during critical periods after birth and thus anatomical size reduction is observed. Generally, declarative memories are enhanced by slow-wave sleep (NREM), while non-declarative memories are enhanced by REM sleep. Declarative memory is the memory for conscious events. A landmark study allowed 18 women and 22 men to sleep only 26 minutes per night over a four-day period. Subjects were given initial cognitive tests while well-rested, and then were tested again twice a day during the four days of sleep deprivation. On the final test, the average working memory span of the sleep-deprived group had dropped by 38% in comparison to the control group. Also, various studies have suggested that there is a correlation between sleep and the complex functions of memory. Sleep researchers have pointed out that an essential part of memory and learning consists of nerve cell dendrites’ sending of information to the cell body to be organized into new neuronal connections. This process demands that no external information is presented to these dendrites, and it is suggested that this may be why it is during sleep that memories and knowledge are solidified and organized. The latest research suggests that while you are asleep, your brain is busily processing the day’s information. It combs through recently formed memories, stabilizing, copying, filing, and making them more useful for the next day. A night of sleep can make memories resistant to interference from other information and allow you to recall them more effectively. It also lets your brain sift through newly formed memories, possibly even identifying what is worth keeping and what to let go of.
_
Why different age groups and different people of the same age group have different sleep duration?
A newborn baby may sleep 16 hours; whereas a person aged 50 might sleep only six hours. Why? The sleep time depends on two factors, the amount of the data that needs to be transferred to the long-term memory, and the speed of the data transfer from the temporary memory to the long-term memory. It is obvious that the database in the long-term memory of a newborn baby is just starting to establish. He/she has to file almost every memory, both declarative and procedural, from the temporary memory to long-term memory. Since the procedural memory (skill to control body movement) is very crucial to the newborn, they spend about 50% of their sleep time in the REM stage. In contrast to this, adults have significant less information that needs to be transferred to the long-term memory since a huge database has already been created. It is also reasonable to assume that adults with a mature brain should have a higher processing and data transfer rate from the temporary memory to long-term memory. In fact this data processing/filing rate could well be different in each person. This would explain variations in required sleep times, why some people always need to sleep longer than others. This would also explain why geniuses sleep less than average humans because their data processing & transfer rate is higher than average humans. This would also explain the fact that the cognitive hallmark of aging is a progressive decrease in the ability to acquire and retain new facts because there is a disturbed mechanism of synaptic plasticity due to neuronal dysfunction in elderly. Additionally, elderly have sub-optimal blood supply to brain due to atherosclerosis of blood vessels. No wonder, elderly leaders have lesser grasping power than younger leaders. I have always believed that nobody should occupy the highest office (President, Prime minister, Supreme Court judge etc) above the age of 65 years and above discussion amply prove my point.
_
Researchers found that the children had more trouble with their schoolwork and more difficulty paying attention when they stayed up late each night and their Grades suffer when kids lose valuable Sleep Time. Also, studying nights before an exam may be sufficient for passing the exam, yet it will leave few useful traces in long-term memory. The exam on its own replaces knowledge as the main purpose of studying! Also, just as we do not have much capacity to survive without drinking due to our poor water storage ability; similarly we cannot sleep in advance in preparation for a double all-nighter before an exam or important deadline. A survey of university students in Utah has found that students who habitually go to bed late and sleep late the next day have lower grade point averages (GPAs) than students with early-to-bed and early-to-rise sleeping habits. So ‘Early to Bed – Early to Rise’ improves brain function.
_
After a week of stressful combat and lack of sleep, soldiers perform worse than if they were drunk or sedated, according to a study. The findings raise questions of tired soldiers’, such as those in Iraq and their ability to determine whether a potential target is an enemy, civilian or ally, as growing number of civilians and friendly forces have mistakenly been killed.
_
Researchers have found that the circadian system is crucial to learning and memory. Biologists have shown that a functioning circadian system is critical to hamsters’ ability to remember what they have learned. Without it, in fact, they can’t remember anything. Hamsters whose circadian system was disabled consistently failed to remember their environment, unlike hamsters with normally functioning circadian systems. Your circadian clock controls your daily cycle of sleep and wakefulness by alternately inhibiting and exciting different parts of your brain through regulation of the release of certain neurotransmitters. If your internal clock isn’t functioning properly, it causes the release of too much GABA, the brain inhibiting neurotransmitter. According to the results of the Stanford study, an excess of GABA inhibits the brain in a way that leads to short term memory problems and the inability to retain new information. Regardless of your age, the best way to keep your circadian clock functioning properly is to make sure you’re getting the necessary amount of high quality sleep, during those hours when your body expects to be sleeping. A good night’s sleep is an essential requirement for being healthy, regardless of your age.
_
A study reported in the journal Current Biology showed that Sleep Spindles seen on EEG during stage N2 of NREM sleep is linked to learning. These electrical impulses help to shift fact-based memories from the brain’s hippocampus—which has limited storage space—to the prefrontal cortex’s “hard drive,” thus freeing up the hippocampus to take in fresh data. The more sleep spindles the sleeper produced, the more refreshed they were for learning. So sleep is necessary for learning! Without sleep we reduce the retention of facts we have learned the previous day. By cutting down on sleep we learn less, we develop less, we are less bright, we make worse decisions, we accomplish less, we are less productive, we are more prone to errors, and we undermine our true intellectual potential! Sleep not only enhances performance, learning and memory but also improves the creative ability to uncover novel connections among seemingly unrelated ideas. Sleep assists the brain in flagging unrelated ideas and memories, forging connections among them that increase the odds that a creative idea or insight will surface. After sleep, people are 33 percent more likely to infer connections among distantly related ideas. So good sleep promotes creativity.
_
Lack of sleep encourages you to make bad decisions. A study revealed that Brain Scans showed lack of sleep increased activity in parts of the brain that deal with ‘positive outcomes’, but reduced activity in regions that handle negative results. Sleep deprivation encourages the sleepless to concentrate on ‘positive outcomes’ in any situation. The researchers concluded that lack of sleep “appears to create an optimism bias; for example, participants behave as if positive consequences are more likely (or more valuable) and as if negative consequences are less likely (or less harmful).” It could explain why traders and late-night gamblers make reckless decisions. It also explains high frequency of accidents by drivers who are sleep deprived.
_
Sleep deprivation and health:
_
Sleep deprivation occurs when an individual fails to get enough sleep. The amount of sleep that a person needs varies from one person to another, but on average most adults need about seven to eight hours of sleep each night to feel well rested and alert next day. About one in five adults fail to get enough sleep. Sleep deprivation can be either acute or chronic.
_
Common causes of sleep deprivation include stress, high sugar high fat diet, Caffeine (coffee, tea, chocolate, cola and energy drinks), alcohol, drugs, smoking, travel, overwork, uncomfortable sleep environment (pillow, mattress, bed, light, noise, temperature, sleeping partner, pets etc) and coexisting illness. Stress is the number one cause of short-term sleeping difficulties, according to sleep experts. Drinking alcohol or beverages containing caffeine in the afternoon or evening, exercising close to bedtime, following an irregular morning and nighttime schedule, and working or doing other mentally intense activities right before or after getting into bed can disrupt sleep. Shift work forces you to try to sleep when activities around you – and your own “biological rhythms” – signal you to be awake. Traveling also disrupts sleep, especially jet lag and traveling across several time zones. This can upset your biological or “circadian” rhythms. If you have to lie beside someone who has different sleep preferences, snores, can’t fall or stay asleep, or has other sleep difficulties, it often becomes your problem too! A number of physical problems can interfere with your ability to fall or stay asleep. For example, arthritis and other conditions that cause pain, backache, or discomfort can make it difficult to sleep well. Certain medications such as decongestants, steroids and some medicines for high blood pressure, asthma, or depression can cause sleeping difficulties as a side effect. Groups that are at particular risk for sleep deprivation include night shift workers, physicians (average sleep = 6.5 hours a day; residents = 5 hours a day), truck drivers, parents and teenagers.
_
Sleep deprivation has two consequences that never fail to occur. The first one is intrusion of sleep into wakefulness. When wakefulness is enforced, sleep pressure increases and sleep cannot be avoided, irrespective of stimulation. The second is performance deterioration, especially cognitive impairment.
_
Sleep deprivation is not insomnia. It is not actually clear that insomniacs “lose sleep,” particularly when it is primary. Sleep deprivation and insomnia are two different concepts. I will give example. Suppose, I woke up at night to treat a heart patient and lost 2 hours of sleep. Then it is a sleep deprivation and not insomnia. Suppose, I went to sleep but could not get sleep due to stress of financial debt, it becomes insomnia resulting in sleep deprivation. Suppose, I went to sleep but got up in the morning with perceived inadequate sleep even though I might have got adequate sleep, then it is primary insomnia but no sleep deprivation. People with insomnia commonly complain that they are very light sleepers and are always aware of their surroundings. Although many insomniacs get a full night of sleep, they report that their sleep is not restful. But sleep laboratory tests often don’t show any abnormalities. So insomnia may or may not lead to sleep deprivation and sleep deprivation does not necessarily mean insomnia. Insomnia is discussed in sleep disorders (vide infra).
_
Say you decide to go on a fast, and so you effectively starve yourself for a week. At the end of seven days, how would you be feeling? You’d probably be hungry, perhaps a little weak, and almost certainly somewhat thinner. But basically you’d be fine. Now let’s say you deprive yourself of sleep for a week. Not so good. After several days, you’d be almost completely unable to function. That’s why Amnesty International lists sleep deprivation as a form of torture. Also, sleep loss of four hours is equivalent to being drunk with alcohol as far as cognitive performance is concerned.
_
Sleep appears necessary for our nervous systems to work properly. Too little sleep leaves us drowsy and unable to concentrate the next day. It also leads to impaired memory and physical performance and reduced ability to carry out math calculations. If sleep deprivation continues, hallucinations and mood swings may develop. Some experts believe sleep gives neurons utilized by us while we are awake, a chance to shut down and repair themselves. Without sleep, neurons may become so depleted in energy or so polluted with byproducts of normal cellular activities that they begin to malfunction. It adversely affects the brain and cognitive function. Complete absence of sleep over long periods is impossible for humans to achieve and brief microsleeps cannot be avoided.
_
Microsleep:
A microsleep is an episode of sleep which may last for a fraction of a second or up to thirty seconds. People who experience microsleeps usually remain unaware of them, instead believing themselves to have been awake the whole time, or to have temporarily lost focus. EEG-monitored microsleeps have shown a 3–14 second episode during which 4–7 Hz (theta) activity replaced the waking 8–13 Hz (alpha) background rhythm. Microsleeping can occur at any time, typically without significant warning. Often, it is the result of sleep deprivation, mental fatigue, depression, sleep apnea, hypoxia, narcolepsy, or hypersomnia. Microsleeps (or microsleep episodes) become extremely dangerous when occurring during situations which demand constant alertness, such as driving a motor vehicle or working with heavy machinery.
_
Sleep debt:
Sleep debt is the difference between the amount of sleep you need and the hours you actually get. Every time you sacrifice on sleep, you add to the debt. Eventually, the debt will have to be repaid. It won’t go away on its own. If you lose an hour of sleep, you must make up that extra hour somewhere down the line in order to bring your “account” back into balance. Sleep debt is the effect of not getting enough rest and sleep; a large debt causes mental, emotional and physical fatigue. Sleep debt results in diminished abilities to perform high-level cognitive functions. Neurophysiological and functional imaging studies have demonstrated that frontal regions of the brain are particularly responsive to homeostatic sleep pressure. Many of us try to repay our sleep debt by sleeping in on the weekends. But as it turns out, bouncing back from chronic lack of sleep isn’t that easy. One or two solid nights of sleep aren’t enough to pay off a long-term debt. If you lost 10 hours of sleep, pay the debt back in nightly one or two-hour installments. To prevent sleep debt, make sleep a priority. Instead of cutting back on sleep in order to tackle the rest of your daily tasks, put sleep at the top of your to-do list.
_
Signs of sleep deprivation:
1) Experts say that if you feel drowsy during the day, even during boring activities, you haven’t had enough sleep. Also, sleep deprivation gives you a hard time getting out of bed in the morning, feel sluggish in the afternoon and get sleepy in meetings, lectures, or warm rooms.
2) If you routinely fall asleep within 5 minutes of lying down, you probably have severe sleep deprivation, possibly even a sleep disorder.
3) Microsleeps, or very brief episodes of sleep in an otherwise awake person, are another mark of sleep deprivation. In many cases, people are not aware that they are experiencing microsleeps.
4) The National Sleep Foundation says that if you have trouble keeping your eyes focused, if you can’t stop yawning, or if you can’t remember driving the last few miles, you are probably too drowsy to drive safely.
5) Need an alarm clock in order to wake up on time.
6) Fall asleep while watching TV or relaxing in the evening.
7) Feel the need to sleep in on weekends.
_
Generally sleep deprivation may result in
1) Aching muscles and increased risk of fibromyalgia
2) Confusion, memory lapses or loss, irritability, hand tremors, hallucinations, headache
3) Reduced performance & ability, increased car accidents and occupational accidents
4) Lack of concentration causing impaired learning
5) Depression
6) blood pressure
7) Increased stress hormone levels
8) Increased risk of diabetes
9) Obesity
10) Temper tantrums in children
11) Yawning
12) Symptoms similar to: Attention-deficit hyperactivity disorder (ADHD) and Psychosis
13) Impaired immune function
14) Increased risk of cancer.
15) Increased inflammation. Chronic or systemic inflammation can cause a variety of diseases and conditions.
_
Sleep is the most undervalued contributor to optimal health and performance. Many people have no idea that getting enough sleep is essential for helping them stick to a diet, making their workouts more productive, or boosting their immune system in general. A good night’s sleep is one of the absolute essential requirements for being healthy. You can have a perfect diet, have no stress, and be physically fit, but if you aren’t sleeping well you will simply not be healthy. Eight out of ten people said that they would sleep more if they knew it would improve their health and memory. In terms of prevention, various studies indicate that consistently sleeping around seven hours per night is optimal for health, and a sustained reduction may predispose to ill health. Furthermore, sleep difficulties are closely associated with psychiatric disorders such as depression, alcoholism, and bipolar disorder. Sleeping too little or too much increases your chances of dying from all causes by up to 15 percent.
_
A prospective study of sleep duration and mortality risk in women was conducted at Division of Sleep Medicine, Department of Medicine, Brigham and Women’s Hospital, Boston. It is commonly believed that 8 hours of sleep per night is optimal for good health. However, recent studies suggest the risk of death is lower in those sleeping 7 hours. Researchers prospectively examined the association between sleep duration and mortality in women to better understand the effect of sleep duration on health. During the 14 years of this study (1986-2000), 5409 deaths occurred in the 82,969 women who responded to the initial questionnaire. Mortality risk was lowest among nurses reporting 7 hours of sleep per night. After adjusting for age, smoking, alcohol, exercise, depression, snoring, obesity, and history of cancer and cardiovascular disease, sleeping less than 6 hours or more than 7 hours remained associated with an increased risk of death. The relative mortality risk for sleeping 5 hours or less was 1.15, for 6 hours 1.01, for 7 hours 1.0, for 8 hours 1.12, and for 9 or more hours 1.42. These results confirm previous findings that mortality risk in women is lowest among those sleeping 6 to 7 hours. New research analyzed data from 16 separate studies and found that people who habitually slept for less than six hours a night were 12 percent more likely to experience premature death.
_
Sleep deprivation and Brain:
Sleep deprivation can adversely affect the brain and cognitive function. A study revealed using MRI scans, that lack of sleep causes the brain to become incapable of putting an emotional event into the proper perspective and incapable of making a controlled, suitable response to the event. Sleep deprivation may have been the underlying cause of the overdose deaths of celebrities Heath Ledger, Anna Nicole Smith and Michael Jackson. A noted 2002 University of California animal study indicated that non-rapid eye movement sleep (NREM) is necessary for turning off neurotransmitters and allowing their receptors to “rest” and regain sensitivity which allows monoamines (norepinephrine, serotonin and histamine) to be effective at naturally-produced levels. This leads to improved regulation of mood and increased learning ability. The study also found that REM (rapid eye movement) sleep deprivation may alleviate clinical depression because it mimics selective serotonin reuptake inhibitors (SSRIs). This is because the natural decrease in monoamines during REM is not allowed to occur, which causes the concentration of neurotransmitters in the brain that are depleted in clinically depressed persons to increase. Sleep outside of the REM phase may allow enzymes to repair brain cell damage caused by free radicals. High metabolic activity while awake damages the enzymes themselves preventing efficient repair. Animal studies suggest that sleep deprivation increases stress hormones, which may reduce new cell production in adult brains. Lack of sleep may cause the brain to stop producing new cells. A study on rats showed that lack of sleep caused a stress hormone to affect the hippocampus, a brain region involved in forming memories. Rats that were deprived of sleep for 72 hours had higher levels of the stress hormone cortisol and as a result produced significantly fewer new brain cells in a region of the hippocampus. When cortisol levels were kept at a constant level, the hippocampus produced a normal amount of new cells. After the animals were restored to normal sleep patterns, it took two weeks for nerve cell production levels to normalize. Researchers concluded that sleep deprivation increases dopamine in the striatum part of the brain involved in motivation & reward and in the thalamus involved in alertness. Following sleep deprivation, the rise in dopamine, the researchers say, may promote wakefulness to compensate for sleep loss. However, the concurrent decline in cognitive performance, which is associated with the dopamine increases, suggests that the adaptation is not sufficient to overcome the cognitive deterioration induced by sleep deprivation and may even contribute to it.
_
Chronic sleep deprivation produces increase in certain hormones (cortisol, catecholamine) & chemicals in the body which increase the risk of developing heart disease and strokes, and other conditions like high blood pressure & cholesterol, diabetes and obesity. The University of Warwick studied 470,000 people in 8 countries and found that sleeping less than 6 hours per night makes you more susceptible to heart disease by 48 % and more susceptible to strokes by 15 %. Sleeping less than 5 hours a day including naps, more than doubles risk of heart attacks and strokes. Likewise, shift workers run a much higher risk of heart attack as compared to people whose waking and sleeping hours are more normal. Having to change shifts frequently and having to sleep during daylight hours are quite damaging — possibly even deadly.
_
At the American Diabetes Association’s annual meeting in June 2001, it reported that people who regularly do not get enough sleep can become less sensitive to insulin. This increases their risk for diabetes and high blood pressure – both serious threats to the brain. The chronic sleep loss may not only hasten the onset but could also increase the severity of age-related ailments such as diabetes, hypertension, obesity, and memory loss. Good sleep helps prevent diabetes mellitus and metabolic syndrome. In one clinical experiment, healthy young men were restricted to just four hours of sleep for six nights and then allowed to recover for six nights. During the sleep-debt period thyroid function went down, while cortisol levels and sympathetic activity went up. But the most important finding in the study was that glucose tolerance tanked during the temporary sleep debt. So chronic sleep-loss could be expected to contribute to the onset of diabetes. And indeed, when a group of men were followed from roughly 1988 through 2004, those who got only five and six hours of sleep per night were twice as likely to develop diabetes. Another study found that poor sleep was associated with a 44 percent increase in the odds of having pre-diabetes among 210 volunteers averaging 46 years of age. Metabolic syndrome is not only the precursor to diabetes, but also to high blood pressure, cardiovascular disease, and other life-threatening diseases. Sleep is a valuable means to combat these problems as well.
_
Not having enough sleep disrupts the balance of two key hormones, ghrelin and leptin, which control the appetite. When it comes to dieting, leptin and ghrelin are the two hormones that regulate appetite, and are adversely affected by sleep deprivation. Ghrelin, which is produced in the stomach, signals to the brain when it’s time to eat. Leptin, on the other hand, is secreted by fat tissue and has the reverse effect, signaling when you are full. Chronic lack of sleep increases ghrelin, making you feel hungry when you don’t really need to eat, and decreases leptin, urging you to keep eating although you’ve already gotten all the calories you need. This leads to obesity and insulin resistance.
_
Melatonin, which is secreted by the pineal gland in the brain and plays an important role in the body’s sleep cycle, is thought to influence the secretion of estrogen, which in turn influences breast cancer risk. Melatonin fights abnormal cell growth, especially in breast cancer and colon cancer. Since melatonin is released at night, less sleep means less melatonin. Thus, a reduced cancer-fighting ability. People who have normal sleep patterns get less cancer. For every hour a woman sleeps less than the recommended seven to eight hours per night, the chances of her getting breast cancer go up by six percent. Tumors grew two to three times faster in laboratory animals with severe circadian rhythm dysfunction. And working the night shift robbed nurses of a normal dose of melatonin, a powerful anti-oxidant known to protect DNA. The research suggests a correlation between decreased melatonin, elevated estrogen, and the observed higher incidence of breast cancer among night shift nurses. High blood levels of the hormone melatonin may explain why blind women have significantly lowered risks for breast cancer compared with sighted women. The investigators found that totally blind women had a 36% lower risk of breast cancer compared with sighted women. This supports the theory that increased nighttime exposure to artificial light reduces melatonin levels, altering estrogen secretion rates and upping risks for breast cancer. Hence women should sleep well in total darkness to reduce risk of breast cancer.
_
The dangers of sleep deprivation are apparent on the road; the American Academy of Sleep Medicine reports that one in every five serious motor vehicle injuries is related to driver fatigue. According to the NHSA, falling asleep while driving is responsible for at least 100,000 crashes, 71,000 injuries and 1,550 deaths each year in the United States. Modern adolescents are habitually nocturnal creatures. They have a habitual tendency to stay up late — 11 p.m. or later — and to awaken late in the morning. But there’s one problem with this arrangement: School! Classes usually begin between 7 and 8 a.m. As a result, only one-fourth of adolescents get the recommended 8.5 to 9.25 hours of sleep each night. Twenty-six percent get 6.5 hours or less each school night. Lack of sleep often translates into poor school performance, negative moods (anger, sadness, etc.), increased use of stimulants and increased risk of unintentional injuries and death. One study found that young drivers age 25 or younger (peak age was 20) cause more than one-half of fall-asleep car crashes.
_
A study found that 14 surgeons in training who got less than 3 hours of sleep after working a 17-hour shift made significantly more errors when performing laparoscopic surgery, a minimally invasive procedure, due in part to lack of concentration and coordination. The surgeons were not operating on real patients, but were using a “virtual reality” surgery system. The surgeons also took longer to perform certain tasks associated with the surgery. A potential risk for compromising patient safety exists with the current system where doctors may need to perform surgery after a sleepless night. Hospitals should ensure that a sufficient number of doctors are available to share workloads and stop the common practice of allowing physicians to work after a night during which they are “on call,” or available for emergencies.
_
It is vital to understand when you regularly shift your sleep patterns because of a job like police, fire or medical profession, then you are simply sacrificing your longevity, and if you engage in this shifted sleep period for many years you can easily knock ten or more years off your lifespan. How many people know that doctors are sacrificing 10 years of longevity by getting disturbed at night to attend medical emergencies? How many patients are grateful to doctors for sacrificing 10 years of longevity?
_
Does stress cause poor sleep, or does poor sleep cause stress? Answer: YES.
Stress leads to activation of the hypothalamic-pituitary-adrenal (HPA) axis and activated HPA axis increases arousal and causes sleeplessness. Stress causes poor sleep. And research shows that insomniacs do have elevated cortisol in the middle of the night, when cortisol should be at its lowest. Conversely, poor sleep also causes stress. But more recently, researchers have discovered that good quality sleep the night before a stressful event can protect you from negative health consequences. Even though you will still encounter stressful events in your life, good quality sleep gives you better brain chemistry to deal with those events. Sleeping well can protect you from stress induced depression … and a variety of other Mood Disorders. Serotonin is an important brain neurotransmitter. Altered serotonin activity has been associated with a host of problems such as aggressive and angry behaviors, clinical depression, obsessive-compulsive disorder, migraine, irritable bowel syndrome, tinnitus, fibromyalgia, bipolar disorder, and anxiety disorders. In a study reported in Journal of Sleep Research, stress plus sleep deprivation caused serotonin receptors in the brain to become less sensitive, while stress following sleep had no such negative effect. It is not known how sleep provided this beneficial influence on brain chemistry.
_
Experiments on mice have shown that throwing off their ancient circadian rhythms by artificially altering the length of their days has a substantial impact on their bodies and brains. Researchers put mice through 10 weeks in 20-hour light-dark cycles, instead of their natural 24-hour circadian cycle. After six weeks, the disrupted mice got fatter, showed less mental flexibility and were more impulsive than mice kept on their natural schedule. The researchers found changes in metabolic hormones, and loss of dendritic length and decreased complexity of neurons in the prelimbic prefrontal cortex, a brain region important in executive function and emotional control. Since the circadian system “drives” the rhythms of biological activity at the cellular level, disruptions tend to cascade outward throughout your entire body, which explains why the health effects of sleep deprivation and sleep disruption are so numerous. This suggests that the modern, round-the-clock lifestyle, made possible by electric lighting, could disrupt metabolism and interfere with learning in ways that are only just beginning to be understood.
_
So in a nutshell, what are the health benefits of sleep?
1) Sleep keeps your heart healthy
2) Sleep may prevent cancer
3) Sleep reduces stress
4) Sleep reduces inflammation
5) Sleep makes you more alert
6) Sleep bolsters your memory
7) Sleep may help you lose weight
8) Naps make you smarter
9) Sleep may reduce your risk for depression
10) Sleep helps the body make repairs
_
What is the impact of sleep on other coexisting diseases?
Sleep and sleep-related problems play a role in a large number of human disorders and affect almost every field of medicine. For example, problems like stroke and asthma attacks tend to occur more frequently during the night and early morning, perhaps due to changes in hormones, heart rate, and other characteristics associated with sleep. Sleep also affects some kinds of epilepsy in complex ways. REM sleep seems to help prevent seizures that begin in one part of the brain from spreading to other brain regions, while deep sleep may promote the spread of these seizures. Sleep deprivation also triggers seizures in people with some types of epilepsy. Sleep is in fact such a crucial aspect of health that it can have an adverse impact on some very serious diseases such as Parkinson‘s disease (PD), Alzheimer‘s disease (AD), Multiple sclerosis (MS), Gastrointestinal tract disorders, Kidney disease and Behavioral problems in children.
_
Neurons that control sleep interact closely with the immune system. As anyone who has had the flu knows, infectious diseases tend to make us feel sleepy. This probably happens because cytokines, chemicals our immune systems produce while fighting an infection, are powerful sleep-inducing chemicals. Sleep may help the body conserve energy and other resources that the immune system needs to mount an attack.
_
Sleeping problems occur in almost all people with mental disorders, including those with depression and schizophrenia. People with depression, for example, often awaken in the early hours of the morning and find themselves unable to get back to sleep. The amount of sleep a person gets also strongly influences the symptoms of mental disorders. Sleep deprivation is an effective therapy for people with certain types of depression, while it can actually cause depression in other people. Extreme sleep deprivation can lead to a seemingly psychotic state of paranoia and hallucinations in otherwise healthy people and disrupted sleep can trigger episodes of mania (agitation and hyperactivity) in people with manic depression.
_
Sleeping problems are common in many other disorders as well, including Alzheimer’s disease, stroke, cancer, and head injury. These sleeping problems may arise from changes in the brain regions and neurotransmitters that control sleep, or from the drugs used to control symptoms of other disorders. In patients who are hospitalized or who receive round-the-clock care, treatment schedules or hospital routines also may disrupt sleep. The old joke about a patient being awakened by a nurse so he could take a sleeping pill contains a grain of truth. Once sleeping problems develop, they can add to a person’s impairment and cause confusion, frustration, or depression. Patients who are unable to sleep also notice pain more and may increase their requests for pain medication. Better management of sleeping problems in people who have other disorders could improve these patients’ health and quality of life.
_
Sleep disorder:
A sleep disorder (somnipathy) is a medical disorder of the sleep patterns of a person. Sleep disorders are disruptions of the sleep cycle or the quality of sleep. An estimated 40 million Americans and millions of others worldwide suffer from some type of sleep disruption or disorder, and these numbers are rapidly increasing. Some sleep disorders are serious enough to interfere with normal physical, mental and emotional functioning. When a person suffers from difficulty in falling asleep and/or maintaining sleep, it is often referred to as Insomnia. In addition, sleep disorders may also cause sufferers to sleep excessively, a condition known as Hypersomnia.
_
INTERNATIONAL CLASSIFICATION OF SLEEP DISORDERS (ICSD):
The International Classification of Sleep Disorders (ICSD) was produced by the American Academy of Sleep Medicine (AASM) in association with the European Sleep Research Society, the Japanese Society of Sleep Research, and the Latin American Sleep Society.
The ICSD consists of four categories.
The first category comprises the dyssomnias i.e., the disorders of initiating and maintaining sleep and the disorders of excessive sleepiness.
The second category, the parasomnias, comprises the disorders of arousal, partial arousal, or sleep stage transition, which do not cause a primary complaint of insomnia or excessive sleepiness.
The third category, sleep disorders associated with mental, neurologic, or other medical disorders, comprises disorders with a prominent sleep complaint that is felt to be secondary to another condition.
The fourth category, proposed sleep disorders, includes those disorders for which there is insufficient information available to confirm their acceptance as definitive sleep disorders.
_
Classification Outline
_
1. Dyssomnias:
A. Intrinsic Sleep Disorders
1. Psychophysiologic Insomnia
2. Sleep State Misperception
3. Idiopathic Insomnia
4. Narcolepsy
5. Recurrent Hypersomnia
6. Idiopathic Hypersomnia
7. Post-traumatic Hypersomnia
8. Obstructive Sleep Apnea Syndrome
9. Central Sleep Apnea Syndrome
10. Central Alveolar Hypoventilation Syndrome
11. Periodic Limb Movement Disorder
12. Restless Legs Syndrome
13. Intrinsic Sleep Disorder NOS
B. Extrinsic Sleep Disorders
1. Inadequate Sleep Hygiene
2. Environmental Sleep Disorder
3. Altitude Insomnia
4. Adjustment Sleep Disorder
5. Insufficient Sleep Syndrome
6. Limit-setting Sleep Disorder
7. Sleep-onset Association Disorder
8. Food Allergy Insomnia
9. Nocturnal Eating (Drinking) Syndrome
10. Hypnotic-Dependent Sleep Disorder
11. Stimulant-Dependent Sleep Disorder
12. Alcohol-Dependent Sleep Disorder
13. Toxin-Induced Sleep Disorder
14. Extrinsic Sleep Disorder NOS
C. Circadian-Rhythm Sleep Disorders
1. Time Zone Change (Jet Lag) Syndrome
2. Shift Work Sleep Disorder
3. Irregular Sleep-Wake Pattern
4. Delayed Sleep-Phase Syndrome
5. Advanced Sleep-phase Syndrome
6. Non-24-Hour Sleep-Wake Disorder
7. Circadian Rhythm Sleep Disorder NOS
_
2. Parasomnias:
A. Arousal Disorders
1. Confusional Arousals
2. Sleepwalking
3. Sleep Terrors
B. Sleep-Wake Transition Disorders
1. Rhythmic movement Disorder
2. Sleep Starts
3. Sleep Talking
4. Nocturnal Leg Cramps
C. Parasomnias Usually Associated with REM Sleep
1. Nightmares
2. Sleep Paralysis
3. Impaired Sleep-Related Penile Erections
4. Sleep-Related Painful Erections
5. REM Sleep-Related Sinus Arrest
6. REM Sleep Behavior Disorder
D. Other Parasomnias
1. Sleep Bruxism
2. Sleep Enuresis
3. Sleep-Related Abnormal Swallowing Syndrome
4. Nocturnal Paroxysmal Dystonia
5. Sudden Unexplained Nocturnal Death Syndrome
6. Primary Snoring
7. Infant Sleep Apnea
8. Congenital Central Hypoventilation Syndrome
9. Sudden Infant Death Syndrome
10. Benign Neonatal Sleep Myoclonus
11. Other Parasomnia NOS
_
3. Sleep Disorders Associated with Mental, Neurologic, or Other Medical Disorders:
A. Associated with Mental Disorders
1. Psychoses
2. Mood Disorders
3. Anxiety Disorders
4. Panic Disorders
5. Alcoholism
B. Associated with Neurologic Disorders
1. Cerebral Degenerative Disorders
2. Dementia
3. Parkinsonism
4. Fatal Familial Insomnia
5. Sleep-Related Epilepsy
6. Electrical Status Epilepticus of Sleep
7. Sleep-Related Headaches
C. Associated with Other Medical Disorders
1. Sleeping Sickness
2. Nocturnal Cardiac Ischemia
3. Chronic Obstructive Pulmonary Disease
4. Sleep-Related Asthma
5. Sleep-Related Gastroesophageal Reflux
6. Peptic Ulcer Disease
7. Fibromyalgia
_
4. Proposed Sleep Disorders:
1. Short Sleeper
2. Long Sleeper
3. Subwakefulness Syndrome
4. Fragmentary Myoclonus
5. Sleep Hyperhidrosis
6. Menstrual-Associated Sleep Disorder
7. Pregnancy-Associated Sleep Disorder
8. Terrifying Hypnagogic Hallucinations
9. Sleep-Related Neurogenic Tachypnea
10. Sleep-Related Laryngospasm
11. Sleep Choking Syndrome
_
Sleep medicine:
Sleep Medicine is now a recognized subspecialty within internal medicine, family medicine, pediatrics, otolaryngology, psychiatry and neurology. The sleep specialist has demonstrated expertise in the diagnosis and management of clinical conditions that occur during sleep, that disturb sleep, or that are affected by disturbances in the wake-sleep cycle. This specialist is skilled in the analysis and interpretation of comprehensive polysomnography and well-versed in emerging research and management of a sleep laboratory.
_
Sleep tests:
Sleep disorders can be diagnosed with various sleep tests including polysomnography (PSG), multiple sleep latency test (MSLT) and Epworth sleepiness scale. PSG is already discussed (vide supra). The multiple sleep latency test (MSLT) is designed to measure daytime sleepiness. The test is based upon the fact that the sleepier an individual is, the faster he or she will fall asleep. In this test, the patient is given four to five opportunities to nap in a quiet, dark room, usually at two hour intervals during the day. Body functions such as EEG and muscle tone are measured as in polysomnography. The time period needed from wakefulness to sleep onset is measured to determine the “sleep latency.” This is repeated during each of the naps, and an average time for sleep latency across all the naps is calculated. Usually a sleep latency of 5 minutes or less is signifies severe daytime sleepiness. The Epworth sleepiness scale is a questionnaire that is given to patients, often as part of an office visit to a health care practitioner. The test asks individuals to rate how likely they would be to fall asleep in a number of situations (such as a passenger in a car, sitting quietly after lunch, etc.).
_
It is beyond scope of this article to discuss all sleep disorders but I will discuss few prominent one.
_
Insomnia:
Insomnia is defined as the inability to get the amount of sleep you as an individual need to wake up feeling rested. Insomnia is the perception of poor-quality sleep, including the inability to fall asleep and/or stay asleep. Because people differ in their need for sleep, there are no fixed criteria that define insomnia. Insomnia is very common and occurs in 30% to 50% of the general population. Approximately 10% of the population may suffer from chronic (long-standing) insomnia persisting for more than one month. Insomnia can be a disorder in its own right, but often it is a symptom of some other disease or condition. Half of all those who have experienced insomnia blame the problem on stress and worry. Sometimes insomnia is caused by pain, digestive problems or a sleep disorder. Insomnia may also signal depression or anxiety. Often times, insomnia exacerbates the underlying condition by leaving the patient fatigued and less able to cope and think clearly. Some medications can lead to insomnia, including those taken for: colds and allergies, high blood pressure, heart disease, thyroid disease, birth control, asthma, pain medications and depression (especially SSRI antidepressants). Some common sleep disorders such as restless legs syndrome and sleep apnea can also lead to insomnia. Left untreated, insomnia is linked to increased illness or morbidity. There is a wealth of research indicating that people with insomnia have poorer overall health, more work absenteeism, and a higher incidence of depression.
_
Cognitive behavioral therapy techniques are usually the first ones recommended because they are effective for a wide variety of causes of insomnia. This approach involves a combination of techniques such as stimulus control instructions, sleep restriction therapy, and addressing the cognitive aspects of sleep problems such as the tendency to worry about insomnia and misconceptions about sleep. There are circadian rhythm treatments such as exposure to bright light or the ingestion of melatonin, which reset the body clock to allow you to sleep better at night and function during the day. For some people, the cause of insomnia is a mood disorder or problems in living, and they may find it helpful to seek psychotherapy where they can talk about these issues. There are psychiatric drugs that are effective in treating mood disorders and anxiety disorders.
_
Sleeping pills:
Medications can be effective in many cases. Sleeping pills vary in how fast they act and the duration of their action. Therefore, choosing the right medication, the dose and timing its administration will depend on the characteristics of the sleep problem. Many tranquilizers actually decrease deeper stages of sleep that are required for the restoration and fresh feeling in the morning. Americans spend nearly $5 billion a year for sleep medications that are only marginally effective. An analysis of sleeping pill studies financed by the National Institutes of Health found that newer sleeping pills like zolpidem, eszopiclone and zaleplon reduced the average time to go to sleep by just under 13 minutes compared with fake pills. Meanwhile, people who took the sleeping pills increased their total sleep time by just over 11 minutes compared with those who took fake pills. As for older sleeping medications like benzodiazepine derivative, people who took the drugs fell asleep 10 minutes faster and slept 32 minutes longer than those taking a placebo. Yet, the participants believed they had slept longer, about 52 extra minutes with the older drugs and 32 minutes with the newer drugs. People may believe they sleep longer than they really do when they take sleeping pills because of a condition called anterograde amnesia, which causes trouble with forming memories. When people wake up after taking sleeping pills, they may, in fact, simply forget that they had been unable to sleep. Is it worth nearly $5 billion (the amount Americans spend on sleeping pills) to sleep for 11 minutes longer a night? On the top of it, sleeping pills are addicting, promote weight gain, increase risk of vehicular accident by continued drowsiness during the day, reduce short-term memory and worsen breathing difficulties. However, if you decide to try sleeping pills, keep in mind the following guidelines.
1) Only take a sleeping pill when you will have enough time to get a full night of sleep (7 to 8 hours).
2) Never drink alcohol near the time when you take a sleeping pill.
3) Never drive a car or operate machinery after taking a sleeping pill.
4) Carefully read the package insert that comes with your medication.
My personal experience with sleeping pill alprazolam 0.5 mg suggests that it works wonder when used occasionally. Many times it has happened that I could not get natural sleep for few days due to hyperactivity of mind due to unnecessary excessive thoughts and I took this tablet and I got adequate sleep with refreshed feeling in the day time but I used to take it may be once in a month. So everybody does need sleeping pill occasionally but you should have strong will power not to get addicted to it.
_
Restless leg syndrome:
Restless legs syndrome (RLS), a familial disorder causing unpleasant crawling, prickling, or tingling sensations in the legs & feet and an urge to move them for relief, is emerging as one of the most common sleep disorders, especially among older people. This disorder leads to constant leg movement during the day and insomnia at night. RLS is a neurologic sensorimotor disorder that is characterized by an overwhelming urge to move the legs when they are at rest. RLS affects approximately 10% of adults in the U.S. RLS runs in families and may have a genetic component. The autopsy studies reported that cells from the portion of the brain called the substantia nigra showed a deficit in one of the proteins that regulates iron status. Symptoms include an urge to move the legs often associated with uncomfortable feeling in the legs (e.g. tingling, creepy, itching, pulling or aching) during periods of inactivity, including both sleep and wakefulness. RLS is also called as nocturnal myoclonus which is a type of sleep disorder characterized by uncomfortable sensations in the legs and an uncontrollable desire to move the legs. These abnormal sensations usually occur in the lower legs shortly after going to bed. During the early stages of sleep, these episodes of leg movement often last up to an hour. The abnormal sensations of RLS are quite variable. They have been described as a crawling, creeping, pulling, drawing, tingling, pins and needles, or prickly discomfort. They are not cramping in character. People with RLS tend to have difficulty falling or staying asleep and suffer from chronic sleep loss, leaving them with the cognitive and tired feelings that occur with sleep loss. RLS can be relieved by drugs that affect the neurotransmitter dopamine, suggesting that dopamine abnormalities underlie these disorder’s symptoms. Some possible treatment for restless leg syndrome include: Behavior therapy, iron supplements and drug therapy (dopaminergics, benzodiazepines, opioids, and anticonvulsants).
_
Narcolepsy:
Narcolepsy is a disease of the central nervous system that results uniformly in excessive daytime sleepiness (EDS). Other primary symptoms of narcolepsy include the loss of muscle tone (cataplexy), distorted perceptions (hypnagogic hallucinations), and the inability to move or talk (sleep paralysis). Additional symptoms can include disturbed nocturnal sleep and automatic behaviors (affected persons carry out certain actions without conscious awareness). All of the symptoms of narcolepsy may be present in various combinations and degrees of severity. People with narcolepsy have frequent “sleep attacks” at various times of the day, even if they have had a normal amount of night-time sleep. These attacks last from several seconds to more than 30 minutes. Narcolepsy affects an estimated 250,000 Americans. Once narcolepsy is diagnosed, stimulants, antidepressants, or other drugs can help control the symptoms and prevent the embarrassing and dangerous effects of falling asleep at improper times.
_
Sleep apnea:
Sleep apnea is defined as the cessation of breathing during sleep. Apnea specialists generally agree that there are three different types of sleep apnea: obstructive, central, and mixed. Of these three, obstructive sleep apnea (OSA) is the most common; central sleep apnea (CSA) is rare; mixed sleep apnea is a combination of the previous two with treatment being the same as OSA. About 2% of women and at least 4% of men suffer from obstructive sleep apnea but experts estimate that it affects about 40% of people aged 65 and older. Obstructive sleep apnea is characterized by repetitive pauses in breathing during sleep due to the obstruction and/or collapse of the upper airway (throat), usually accompanied by a reduction in blood oxygen saturation, and followed by an awakening to breathe. This is called an apnea event. Respiratory effort continues during the episodes of apnea. Central Sleep Apnea is defined as a neurological condition causing cessation of all respiratory effort during sleep, usually with decreases in blood oxygen saturation. Note that CSA, which is a neurological disorder, is very different in cause than OSA, which is a physical blockage – though the effects are highly similar. The apnea must be at least 10 seconds in duration or longer. Specialists usually consider 5 or more of such apneas per hour to be of possible clinical significance (less than 5 per hour is normal). However, another important factor is whether the person is excessively tired during the day. Even though the brain senses that it isn’t receiving enough oxygen and sends a signal to the person to wake up, most people with sleep apnea do not realize that they are awakening to breathe many times during the night. The arousal is slight, and people become accustomed to this, but it is enough to disrupt the pattern of sleep so that they get very little deep sleep or REM sleep, and awaken feeling sleepy. A great many (probably most) apnea sufferers go through a large part of their lives unaware of their condition. It is unbelievable but true that sleep apnea sufferers may wake as often as 112 times per hour or more each night. That means a patient may stop breathing for at least 10 seconds about two times every minute.
_
Problems caused by sleep apnea:
When a blocked airway prevents oxygen from entering the body, blood vessels constrict and blood pressure rises as much as 25% to 30%. The sympathetic system gets activated as the oxygen saturation in the blood decreases and the apnea continues resulting in stimulation of sympathetic nerve and adrenaline release causing the blood vessels to constrict and to the heart to work harder. More blood is sent to brain and muscles when blood vessels constrict. This increases blood pressure, which makes the heart work harder for pumping blood through smaller blood vessel. So sleep apnea has also been linked to high blood pressure and to increased chances of heart disease, stroke, and irregular heart rhythms (arrhythmias). What’s more, sleep apnea causes hormone levels to change in a way that reduces the effectiveness of insulin, leading to higher blood sugar and potentially diabetes. If nothing else, the continual lack of quality sleep can affect your life in many ways including depression, irritability, loss of memory, lack of energy, a high risk of auto and workplace accidents, and many other problems. In children, sleep apnea can slow physical and mental growth and make it more difficult to learn.
_
Symptoms of sleep apnea:
Loud and frequent snoring is probably the best and most obvious indicator. Not everyone who snores has apnea, by any means, and not everyone with apnea necessarily snores (though most do). Your bedmate indicates that you periodically stop breathing during your sleep, or gasp for breath. Other symptoms include excessive daytime sleepiness/fatigue, unrefreshing sleep with feelings of grogginess, dullness, morning headaches and severe dryness of the mouth. High blood pressure is a warning sign of sleep apnea. Up to 60% of patients with sleep apnea may have hypertension. Hypertension in patients with sleep apnea is often resistant to antihypertensive therapy. Another study found 8 % hypertensive having sleep apnea as the cause of hypertension.
_
Management of sleep apnea:
The only definite way to diagnose OSA is to spend a night in a sleep lab undergoing a “polysomnogram,” (PSG – a sleep study). Treatment of OSA includes weight loss, surgery, dental appliances, and a breathing-assistance device like nasal continuous positive airway pressure (CPAP). Nasal CPAP is the most common treatment for sleep apnea. You wear a mask over your nose during sleep and pressure from an air blower forces air through your nasal passages. The air pressure is constant and continuous, and adjusted so that it is just enough to prevent your throat from collapsing during sleep. Nasal CPAP prevents airway closure while in use, however, apnea episodes return when CPAP is stopped or if used improperly, so it’s not a permanent fix.
_
Snoring:
Snoring is a very common sleep problem that limits either your or someone you sleep with, ability to sleep well. An estimated 45 percent of adults snore occasionally, and about 25 percent are habitual snorers, according to the American Academy of Otolaryngology. It’s more common in men, as well as people who are overweight, and usually gets worse as you get older. A study found that Child’s snoring may be cause of poor school performance. Snoring is caused by reduced airways, stemming from either your throat or nasal passageway, and it’s the vibrations as the air struggles to get through your soft palate, uvula, tongue, tonsils and/or muscles in the back of your throat that causes the snore. The conditions which can cause snoring include your mouth anatomy, being overweight, nasal problems, alcohol consumption and sleep apnea.
_
Primary Snoring, also known as simple snoring, snoring without sleep apnea, noisy breathing during sleep, benign snoring, rhythmical snoring and continuous snoring is characterized by loud upper airway breathing sounds in sleep without episodes of apnea (cessation of breath). Primary snoring differs from snoring in OSA by feeling refreshed when you wake up, no evidence of insomnia and you do not experience excessive sleepiness during the day.
_
Habitual snoring may be more than just a nuisance. Depending on the cause of your snoring, it may result in: daytime sleepiness, relationship problems , difficulty concentrating, a greater risk of high blood pressure, heart failure & stroke; an increased risk of behavior problems, such as attention-deficit/hyperactivity disorder (ADHD) in children with obstructive sleep apnea and an increased risk of motor vehicle accidents due to lack of sleep.
_
Various natural & simple ways to reduce snoring:
1) Sleep on your side, not your back — The reason why sleeping on your side instead of your back is recommended is because snoring is often due to lax muscles in your throat and tongue. When you lie on your back your throat and tongue muscles ease backward in your throat, causing a vibration as you struggle to breathe.
2) Raise the head of your bed – This simple tip can also help diminish the collapsing of your airways. Simply raise the head of your bed about four inches, by placing blocks or wedges under your mattress.
3) Normalize your weight — Carrying extra weight around your neck can also cause your throat to narrow when you lay down, hence the higher incidence of snoring if you’re overweight. Normalizing your body weight could make a big difference.
4) Do throat and tongue exercises — If they are stronger they are less likely to slip backward.
5) Use steam inhalation – steam inhalation just before going to bed, can also work wonders to clear out, and reduce any swelling in your nasal airway that might be a contributing factor and keep your sleeping environment as clean and dust free as possible.
6) Use nasal strips – If your problem stems from obstruction in your nasal passageway, using nasal air strips can help increase airflow.
7) Avoid alcohol – Alcohol, and other muscle relaxing or sleep aid drugs will relax your tongue and throat muscles even more, making your snoring worse.
8) Avoid milk – Yes, drinking milk, especially at night, can also make snoring worse as it leaves a layer of mucus in your mouth and throat, so stick to plain water.
9) Avoid big meals late in the evening — Don‘t eat a big meal right before bed time. If your stomach is full it can push up against your diaphragm, further limiting your ability to breathe easy.
10) A study recommends 10 mg of domperidone (dopamine receptor blocker prokinetic agent, which improves gastro-intestinal motility) with 60 mg of pseudoephedrine (nasal decongestant) taken 1 hour before sleeping to relieve benign primary snoring.
If all these measures fail, then treatment of snoring includes oral appliances, surgery and CPAP.
_
Sleepwalking:
Sleepwalking (Somnambulism) is a series of complex behaviors that are initiated during slow wave sleep and result in walking during sleep. Sleepwalkers arise from the slow wave sleep stage in a state of low consciousness and perform activities that are usually performed during a state of full consciousness. These activities can be as benign as sitting up in bed, walking to the bathroom, and cleaning, or as hazardous as cooking, driving, extremely violent gestures, grabbing at hallucinated objects, or even homicide. Sleepwalkers often have little or no memory of the incident, as they are not truly conscious. Although their eyes are open, their expression is dim and glazed over. Sleepwalking may last as little as 30 seconds or as long as 30 minutes. Polysomnographic monitoring demonstrates the onset of an episode during stage 3 or 4 sleep. The onset typically occurs in prepubertal children. It is more common in children than in adolescents and adults. Boys are more likely to sleepwalk than girls. The highest prevalence of sleepwalking was 16.7% at age 11 to 12 years of age. Medical reports show that about 18% of the population is prone to sleepwalking. It is difficult in arouse the patient during an episode and there is an amnesia following an episode. Sleepwalking could be inherited as an autosomal dominant disorder with reduced penetrance in a family. Other precipitating factors to sleepwalking are those factors which increase the slow wave sleep stage including sleep deprivation, fever, and excessive tiredness. If a child begins to sleepwalk at the age of 9, it often lasts into adulthood. The sleepwalker may feel embarrassment, shame, guilt, anxiety and confusion when they are told about their sleepwalking behavior. Some people mistakenly believe that a sleepwalker should not be awakened. It is not dangerous to awaken a sleepwalker, although it is common for the person to be confused or disoriented for a short time when they wake up. Another misconception is that a person cannot be injured while sleepwalking. Sleepwalkers are commonly injured when they trip and lose their balance. Most people don’t need any specific treatment for sleepwalking. Make sure you get plenty of rest; being overtired can trigger a sleepwalking episode. Ensure good sleep hygiene. Benzodiazepines have been proven to be useful in the treatment of this disorder. A person who has a sleepwalking disorder can take the following measures: get adequate sleep; meditate or do relaxation exercises; avoid any kind of stimuli (auditory or visual) prior to bedtime; keep a safe sleeping environment free of harmful or sharp objects; sleep in a bedroom on the floor if possible to prevent falls and avoid bunk beds; lock the doors and windows; and remove obstacles in the room as tripping over toys or objects is potential hazardous.
_
Sleep terror:
Sleep Terrors are characterized by a sudden arousal from slow wave sleep with a piercing scream or cry, accompanied by autonomic nervous system & behavioral manifestations of intense fear. Polysomnographic monitoring demonstrates the onset of episodes during stage 3 or 4 sleep. Other medical disorders like epilepsy is not the cause of the episode but other sleep disorders like nightmares can be present.
_
Sleep paralysis:
Have you ever felt like you were awake but unable to move? You might have even felt afraid but could not call for help? This condition is called sleep paralysis. An alarming 50 per cent of the population suffers from sleep paralysis. Sleep paralysis is a feeling of being conscious but unable to move. It occurs when a person passes between stages of wakefulness and sleep. During these transitions, you may be unable to move or speak for a few seconds up to a few minutes. Sleep paralysis is a paralysis associated with sleep that may occur in normal subjects or be associated with narcolepsy, cataplexy, and hypnagogic hallucinations. The pathophysiology of this condition is closely related to the normal hypotonia that occurs during REM sleep. It is a state of motor paralysis, and not mental illness. It happens during the Rapid Eye Movement (REM) sleep. In this condition, the body is asleep but the mind is awake and conscious of the surroundings. If the victims get nightmares just as they are waking up, they get frightened and find it difficult to move or speak. Sleep paralysis may leave you feeling frightened, especially if you also see or hear things that aren’t really there. Sleep paralysis may happen only once, or you may have it frequently — even several times a night. Sleep Paralysis is relatively common though rarely as a severe disorder. When under sleep paralysis, try to move a finger because that one movement is enough to break out of the episode.
_
Sexual behavior in sleep (SBS):
Sleepsex, sleep sex or sexsomnia or SBS is sexual behavior that occurs during sleep. Some people seem to enjoy it and view it with a sense of humor. However, it can be disturbing, annoying, embarrassing and is a potentially serious problem for some couples and individuals. Although it is recognized as a sub-type of parasomnia, “sexsomnia” is not included as a particular type of sleep disorder with its own diagnosis. In fact, when one discovers their own SBS, usually after being informed about their behavior by a bed partner, they themselves are unlikely to believe that could behave in such a fashion. At present most people know that people can walk and talk in their sleep. That sexual behavior also occurs in sleep is not at present a common knowledge.
_
Bedwetting:
Nocturnal enuresis, commonly called bedwetting is an involuntary urination while asleep after the age at which bladder control usually occurs. Most girls can stay dry by age six and most boys stay dry by age seven. Two physical functions prevent bedwetting. The first is a hormone ADH that reduces urine production at night. The second is the ability to wake up when the bladder is full. Children usually achieve nighttime dryness by developing one or both of these abilities. Bedwetting is the most common childhood urologic complaint and one of the most common pediatric-health issues. Most bedwetting, however, is just a developmental delay – not an emotional problem or physical illness. Only a small percentage (5% to 10%) of bedwetting cases is caused by specific medical situations. Studies show that at least 2% of adults have a lack of control of urination during the night. Nocturnal enuresis is not to be confused with nocturia or waking two or more times per night to void. Different types of enuresis exist, which need to be differentiated. Persistent Primary Nocturnal Enuresis is a condition that begins during childhood, where nighttime dryness has not been achieved for longer than six months. About 2-3% of male and female adults that are older than 18 years of age have this type of nocturnal enuresis. Adult Onset Secondary Enuresis is defined as nocturnal enuresis in which nighttime dryness is achieved at some point in life and, for some, dryness may have occurred for years, but nighttime wetting begins at an older age. Nocturnal enuresis has affected people for centuries. Evidence of this problem can be traced back as far as 1500 BC. While extensive research has been devoted to nocturnal enuresis in children, persistent primary enuresis and adult onset secondary enuresis in particular have not been studied as thoroughly. It must be understood that bedwetting is unintentional and is not something that can be voluntarily controlled. If you suffer from persistent primary nocturnal enuresis, you may see a family practice physician. However, individuals with adult onset nocturnal enuresis usually need to be referred to a specialist, such as an urologist or sleep disorder specialist. While you may be embarrassed to address the issue with others, a medical professional is able to give you options to help treat bedwetting. In many cases, bedwetting can be cured.
_
Scientific management of sleep disorders includes urinary neurotransmitter and salivary hormone assessments to objectively identify chemical imbalances to treat sleep disorders.
Each patient with sleep disorder has a different neurotransmitter imbalance and needs treatment to correct the imbalance with drugs which either increase or decrease a specific neurotransmitter.
_
5-hydroxytryptophan:
5-HTP (5-hydroxytryptophan) is a compound produced by the body from amino acid tryptophan. 5-HTP bypasses the brain’s light-regulation system that controls the secretion of melatonin. 5-HTP results in the increased production of neurotransmitters such as serotonin and norepinephrine that stimulate the noradrenergic receptors in the brain. This stimulation directly triggers the production and release of melatonin. Thus, when you take 5-HTP, it causes the release of melatonin irrespective of how much light is present. The higher levels of melatonin in circulation helps you to fall asleep and stay asleep better. People with low melatonin levels who take 5-HTP at nighttime can enjoy the same sleep enhancing benefits as they will from taking melatonin alone, but they will also be getting the broader spectrum of benefits that comes from increased serotonin levels. Even eating food containing higher amount of tryptophan (banana, walnuts) can increase production of 5-HTP.
_
It is crucial that you understand that improving your melatonin levels is key to getting a good night’s sleep, so make sure you have exposure to bright sunlight in the daytime and sleep in absolute darkness at night. It is recommended to install black out shades and/or curtains in your bedroom. It is important you sleep in cave-like darkness and can’t even see your hand in front of your face. Remember: No night-lights or clock radio lights. Also, never TURN ON the lights should you need to get up and use the bath room. Any small amount of light will instantly shut off your melatonin production.
_
Jet lag management:
After crossing several time zones in a short period of time, your internal clock, or circadian rhythm, becomes out of sync with the external environment’s clock. The best trick to tackle jet lag is to stay awake in your new destination until bedtime and take a dose of melatonin when you go to bed, and the next day you will have no jet lag. Melatonin is also useful to induce sleep in shift workers and blind people. To reduce the effects of jet lag, some doctors try to manipulate the biological clock with a technique called light therapy. They expose people to special lights, many times brighter than ordinary household light, for several hours near the time the subjects want to wake up. This helps them reset their biological clocks and adjust to a new time zone.
_
Night shift worker management:
Try not to work a number of night shifts in a row. Avoid frequently rotating shifts. Take scheduled naps. Keep your workplace brightly lighted to promote alertness. Use blackout blinds or heavy curtains to block sunlight when you sleep during the day. Sunlight is a potent stimulator of the circadian rhythm even if your eyes are closed, the sunlight coming into the room tells your brain that it’s daytime.
_
Sleep mask:
Probably the most simple, inexpensive and easy way to ensure that you have darkness when you are trying to sleep is to use a sleep mask (also known as an eye mask, sleeping mask, and sleep eye mask). Sleep masks are made of light-blocking material that cover your eyes and fasten around your head. They are capable of blocking nearly 100% of light. Most people find them to be effective and easy to get used to wearing. There are basically four different types of sleep masks: Nylon, Fleece, Foam and Silk. I recommend foam mask because you can experience total black out even with your eyes open. The fact that you can totally open your eyes while wearing a foam eye mask is truly wonderful. There are large indentations in the eye area so you there isn’t any contact with your eye lids or lashes. This allows you to open your eyes while wearing it. That feature is important because when you go through REM sleep cycles, your eyes often move quite a bit. This mask, with room to open and move your eyes helps you sleep better through the REM stages.
_
CAM:
Examples of complementary & alternative medicine (CAM) therapies used to treat sleep disorders include acupuncture, guided imagery, yoga, hypnosis, biofeedback, aromatherapy, relaxation, herbal remedies, massage, meditation, exercise and supplements.
_
Sleep and sex:
Sleep and sex is not a topic on which a lot of research has been done and there are a lot of ways that sleep affects one’s sex life. Separate beds or bedrooms may not be the answer either, as that could affect the psychological bond between the two of you. Just how are sleep and sex related? According to a 2005 study by the National Sleep Foundation, nearly 25% of couples in the United States admit to being so sleepy that they have lost interest in lovemaking. People who snore also appear to have inferior sex lives, as one-third of people say that snoring causes a problem in their relationship. Lack of sleep from sleep disorders has been proven to cause certain levels of sexual dysfunction. Lack of sleep causes moodiness, depression, and anxiety. These are emotions that obviously affect your drive for sex. Increased stress translates into less time for both sleep and sex. The medical condition most commonly associated with problems with sleep and sex is sleep apnea and men with sleep apnea tend to have lower levels of testosterone, which can lower libido. Other medical conditions that affect sleep and sex include diabetes, lung conditions, depression and heart disease. Symptoms of depression and anxiety can include both insomnia and a diminished sex drive. And many antidepressants, which can sometimes cause erectile dysfunction and/or a loss of libido, further complicate matters. People may be skimping on sleep and sex because of a hectic work schedule. Those who do shift work at night may find it especially hard to obtain both sleep and sex. Not only is it is difficult for shift workers and their partners to find a time when they’re both free to have sex, they are often too tired to get in the mood when time becomes available. Being awake at night also throws off the body’s internal clock, or circadian rhythms, which sleep medicine experts say can impair sexual functioning. The amazing part is that sex can actually really help you with sleep. You get into bed. You’re stressed. You’re uptight. And then you start getting stressed about not being able to fall asleep, and that keeps you even more sleepless. Instead, you should try having sex. It will help you sleep, because it releases endorphins and you feel better about yourself. Remember, good sex leads to good sleep and good sleep improves mood & vigor which leads to good sex drive and sleep-sex cycle continues to benefit the couple.
_
Sleep and pregnancy:
According to the National Sleep Foundation’s 1998 Women and Sleep poll, 78% of women report more disturbed sleep during pregnancy than at other times. Many women also report feeling extremely fatigued during pregnancy, especially during the first and third trimesters. Considering the physical and emotional demands of pregnancy and the prevalence of sleep disorders among pregnant women, it’s no wonder that expectant mothers become so tired. One of the reasons for fatigue and sleep problems during pregnancy are changing hormone levels. For example, rising progesterone levels may partly explain excessive daytime sleepiness, especially in the first trimester. Hormonal changes may also have an inhibitory effect on muscles, which may result in snoring and in obese women increase the risk of developing sleep apnea and may be partly responsible for the frequent trips to the bathroom during the night. These interruptions as well as those caused by nausea and other pregnancy-related discomforts can result in significant loss of sleep. Many women experience insomnia due to emotions and anxiety about labor and delivery, balancing motherhood and work, or their changing relationship with their partner. The common sleep problems associated with pregnancy include insomnia, restless leg syndrome, sleep apnea, nocturnal gastroesophageal reflux (nighttime GERD) and frequent nighttime urination. Treatment for sleep problems during pregnancy is complicated by the fact that drug therapy can harm a developing fetus. For example, most drugs that are used to treat insomnia carry some risk and are typically not recommended for women who are pregnant or nursing. However, by practicing good sleep hygiene, most women are able to manage pregnancy-related insomnia.
_
Sleep and fertility:
To discover the affect sleep has on fertility, researchers took a poll of women who have sleep-deprived professions, such as flight attendants and late shift nurses. According to the study, half of the women tested had irregular menstrual cycles, while others stopped ovulating altogether. Another influence on ovation and reproductive hormones is the amount of daily light exposure. Lack of sunlight can trigger depression, which in turn suppresses fertility. Further, researchers found that they could alter the length of women’s menstrual cycles by exposing them to artificial light (around the middle of their cycles) as they slept. They discovered that the hormones that trigger ovulation are tied to the body’s biological clock.
_
Why do we yawn?
Yawn is a reflex to open the mouth wide somewhat involuntarily with a prolonged, deep inhalation and sighing or heavy exhalation and usually accompanied by stretching of the eardrums. The average duration of a yawn is about 6 seconds. Yawning is associated with tiredness, sleepiness, stress, overwork, lack of stimulation, and boredom. In humans, yawning has an infectious quality (i.e., yawning precipitated by seeing a person yawning) which is a typical example of positive feedback and it has been also noted in chimpanzees and dogs. Everybody yawns – from unborn babies to the oldest great-grandparent to animals but why do people and animals yawn? No one knows for sure. Yawning is often considered rude due to the implication of boredom, and may even lead to penalties for contempt of court.
Theories of yawning:
1) Yawning helps us bring more oxygen into the blood and move more carbon dioxide out of the blood when you are tired and fatigued.
2) Yawning stretches the lungs and lung tissue. Stretching and yawning may be a way to flex muscles and joints, increase heart rate, and feel more awake.
3) Yawning is a protective reflex to redistribute the oil-like substance called surfactant that helps keep lungs lubricated inside and keeps them from collapsing.
4) Another notion states that yawning is the body’s way of controlling brain temperature. The process is thought to cool off the brain, much like a fan cools the inside of a computer.
5) Another hypothesis is that yawns are caused by the same chemicals (neurotransmitters) in the brain that affect emotions, mood, appetite, and other phenomena. These chemicals include serotonin, dopamine, glutamic acid, and nitric oxide. As more (or less) of these compounds are activated in the brain, the frequency of yawning increases.
6) Recent research indicates a connection (supported by neuro-imaging research) between empathic ability and yawning. It is believed that contagious yawning indicates empathy. It indicates an appreciation of other people’s behavioral and physiological state.
_
The majority of disorders associated with yawning are those of the central nervous system, including epilepsy, encephalitis, brain tumors, multiple sclerosis and progressive supranuclear palsy. Excessive yawning is also associated with opiate withdrawal and the consumption of a variety of drugs that affect neurotransmitters, such as drugs prescribed for Parkinson’s disease or depression. Studies have shown that people with brain lesions often yawn excessively while schizophrenics yawn very little. Yawning can also be the first sign of what is called the vasovagal reaction.
_
Dreams:
My personal experience of dreams suggests that dreams are recollections of conglomeration of past memories in illogical fashion. I have never seen my biological parents in my dreams because I have no memory of them in my brain. Accumulated observation has shown that dreams are strongly associated with REM sleep during which an EEG shows brain activity to be most like wakefulness. During a typical lifespan, a person spends a total of about six years dreaming (which is about two hours each night). Most dreams only last 5 to 20 minutes. It is unknown where in the brain dreams originate, if there is a single origin for dreams or if multiple portions of the brain are involved, or what the purpose of dreaming is for the body or mind. During REM sleep, the release of the neurotransmitters norepinephrine, serotonin and histamine is completely suppressed. As a result, motor neurons are not stimulated, a condition known as REM atonia. This prevents dreams from resulting in dangerous movements of the body. Now it is known that REM sleep can occur without dreaming and dreaming can occur without REM sleep. Although REM is triggered from the brainstem, it alone will not result in dream states. Dreams require input from the forebrain and structures in the limbic system. The forebrain mechanisms are the final common path to dreaming. The brainstem is just one of the many arousal triggers that can activate these forebrain mechanisms. Although REM sleep is controlled by the brainstem, dreaming seems to be controlled by these forebrain mechanisms. It is now acknowledged that REM sleep is not indispensable for dreaming, that dreaming can also occur during non-REM sleep, and that dream-like experiences can even be elicited during quiet wakefulness. This explains why so many individuals report bizarre vivid life-like dreams whilst on serotonin boosters SSRI antidepressants.
_
Why we forget our dreams?
Although we all dream every day when we sleep, we can seldom recollect more than a few minutes worth of our dreams after waking. Unless being recalled immediately after waking, dreams cannot be remembered. The reason that we forget our dreams is because our temporary memory store has been switched to retrieve-only mode in the sleeping brain for memory processing. Any brain mentation during this period could not be saved in the temporary memory store. Only the short-term memory (working memory) store is still available for memory storage during sleep. Since the short-term memory has a very limited capacity, decays rapidly and will be replaced by new incoming information if distracted, a sleeper can only recall the memory from the short-term memory store immediately after waking. This explains why one can recollect so little of their dreams.
_
Nightmare:
“Nightmare” is a dream which causes one to wake up in the middle of the sleep cycle and experience a negative emotion, such as fear and/or horror. They are not common in children under 5, but they are more common in young children (25% experiencing a nightmare at least once per week), most common in adolescents, and less common in adults. Nightmares can have physical causes such as sleeping in an uncomfortable or awkward position, having a fever, or psychological causes such as stress and anxiety. Eating before bed, which triggers an increase in the body’s metabolism and brain activity, is a potential stimulus for nightmares. Occasional nightmares are commonplace, but recurrent nightmares can interfere with sleeping patterns and cause insomnia that may require medical help.
_
Sleep hygiene:
Sleep hygiene can be defined as the controlling of all behavioral and environmental factors that precede sleep and may interfere with sleep. It is the practice of following guidelines in an attempt to ensure more restful, effective sleep which can promote daytime alertness and help treat or avoid certain kinds of sleep disorders. Trouble sleeping and daytime sleepiness can be indications of poor sleep hygiene. Good sleep hygiene practices include:
1) Avoid caffeine, nicotine, and alcohol use before bedtime. Some studies have shown that caffeine consumed early in the day can have an effect on the ability to fall asleep at night.
2) Have and adhere to a regular bedtime and waking schedule.
3) Maintain a comfortable sleep environment, including a comfortable temperature.
4) Do not lie down in bed awake, worrying about not sleeping (or anything else negative). This produces anxiety that can actually make the problem worse.
5) Get regular daily exercise (it is recommended that individuals avoid exercise two hours prior to bedtime).
_
Sleep position:
The sleeping position is the body configuration assumed by a person during or prior to sleeping. Various studies have shown that placing a young baby in a prone position increases the risk of sudden infant death syndrome (SIDS). Pregnant women are encouraged to sleep on side as it will increase the amount of blood and nutrients that reach the placenta and her baby. People who are at risk of obstructive sleep apnea must sleep on their side and with a 30° or higher elevation of the upper body. Snoring, which may be (but is not necessarily) an indicator of obstructive sleep apnea, may also be alleviated by sleeping on one’s side. Sleeping on your back can constrict upper airway causing OSA. Sleeping on your stomach can twist your neck into an awkward position, put excess pressure on your spine, and make it more difficult to inhale. Health wise, sleeping on either side curtails snoring, and resting on your left side keeps your stomach active and eases heartburn.
_
Mattress:
The greatest irony of human intelligence is that we spend one third of our lives sleeping but we hardly give any thought about a mattress on which we sleep. With so many choices — traditional coil, air, latex, and memory foam mattresses being some of the top contenders — buying a new mattress can be a nightmare. The right mattress should be firm enough to provide support to your back, neck, and legs, while still offering some cushion and recoil for comfort. You want a mattress that is firm enough to distribute your weight or you’ll wake up sore due to your shoulders sagging or your hips sinking. On the other hand, you don’t want to sleep on a board. Researchers have tried very hard to study mattress choice in a scientific fashion and have found that there is too much variability between people to come to any firm conclusions about what’s the best mattress. You have to devote time (15 to 20 minutes per mattress) actually testing various sleep surfaces before deciding to buy. Lie on your back, your belly, your side and judge yourself and then buy. Also, once you start using a mattress, it must be turned upside down regularly and changed every 7 or 8 years. The mattress & bed must be large enough to prevent falling and accommodate various sleep movements because the average person moves 65 times a night.
_
Co-sleeping of infant with parents:
The safest arrangement is for the infant to sleep between the breastfeeding mother and the edge of the bed, with an adequate barrier to prevent the baby from falling off. This removes any risks of suffocation from the father. Many experts have noted that there is a connection or awareness of the baby between mother & child that does not exist with the father. I would stress that this in no way means the father loves the baby any less. The mother’s special bond is simply a protective biological mechanism. Do not sleep with the baby if you have had any alcoholic beverages. Do not sleep with the baby if you are very overtired or fatigued enough to impair your ability to awaken during the night.
_
Sleep and EMF:
An electromagnetic field (EMF) is an invisible zone of energy that surrounds electric devices and wiring. There are serious scientific concerns about the radiation emitted from power lines, cell phones, TV, microwave oven, radio and many other sources of exposure to radiofrequencies and electromagnetic fields in daily life. Various studies have shown evidence that electromagnetic fields can affect gene and protein expression, have genotoxic effects – DNA damage, induce stress response (stress proteins), affect immune function, affect neurology and behavior, cause childhood cancers (Leukemia) and impact melatonin production etc. The vast majority of beds (90-95 percent) contain metal springs and/or frames. Unfortunately, these metal frames and metal box springs can amplify and distort the earth’s natural magnetic field, which can lead to a non-restful sleep. Cats, ants and termites have an unusual characteristic in common; they’re all attracted to Geopathic stress zones. Geopathic stress is natural radiation that rises up through the earth and becomes distorted by weak electro-magnetic fields, created by subterranean running water, certain mineral concentrations, fault lines, and underground cavities. Electropathological energy created by modern technology such as high and low frequency energy from telecommunication towers, electricity pylons, transformers, radar and radio towers can also contribute to Geopathic stress. If you are exposed to Geopathic stress during sleep, your brain never receives the full rest it requires to repair and regenerate. This is why it’s so important to avoid sleeping where your cat sleeps, as for if your home is located near a Geopathic stress fault, your cat will likely find it and sleep near it. If you don’t have a cat, look for areas where plants do not thrive, ant hills are built or termites congregate. These are all signs of a Geopathic stress zone. There are several steps you can take to lower your EMF burden. Turn off everything electrical in your sleeping area, including your Wi-Fi, cell and portable phones. Sleep on a non-metal bed and mattress.
_
Sleep related amnesia:
People awakened after sleeping more than a few minutes are usually unable to recall the last few minutes before they fell asleep. This sleep-related form of amnesia is the reason people often forget telephone calls or conversations they’ve had in the middle of the night. It also explains why we often do not remember our alarms ringing in the morning if we go right back to sleep after turning them off.
_
Are we monophasic or biphasic sleepers?
Polyphasic sleep refers to the practice of sleeping multiple times in a 24-hour period—usually more than two, in contrast to biphasic sleep (twice per day) or monophasic sleep (once per day). It does not imply any particular sleep schedule. More than 85% of mammalian species are polyphasic sleepers, meaning that they sleep for short periods throughout the day. I do not agree with the notion that humans are part of the minority of monophasic sleepers, meaning that our days are divided into two distinct periods, one for sleep and one for wakefulness. Monophasic sleep is not the natural sleep pattern of humans. It is common for small children and elderly people to take frequent naps and napping is a very important aspect of many cultures. Biological and evolutionary human development suggests that adult humans are biphasic sleepers. Research shows that the majority of people suffer from tiredness twice in every 24 hour period. In fact naps were a natural part of the human sleep cycle. It is found that, even after a full night’s sleep, people have a strong tendency to fall asleep in the early afternoon. When volunteers were put into a time-free environment, they tended to sleep in two time periods; one at night and another about twelve hours later in the early afternoon. The Circadian Rhythm of the body is actually 25 hours, so the sleep pattern in a time-free environment would get pushed forward an hour each day. We tend to ignore this for reasons of practicality and work routines by regulating our waking time to the same time each day. The second wave of tiredness happens about 8 hours after we wake up in the morning. So during the early afternoon between 1.30 pm and 3.00 pm, we are likely feel tired again. A short nap of 10-20 minutes can satisfy this desire for sleep and allow us to wake up feeling refreshed and much more alert. Many sleep researchers assert that polyphasic sleep in adult humans disrupt their circadian rhythms, will eventually cause them to suffer the same negative effects as those with other forms of sleep deprivation and circadian rhythm sleep disorders.
_
Naps & siesta:
A nap is a short period of sleep, usually during daytime. A siesta is a short nap taken in the early afternoon, often after the midday meal. The Siesta has existed for thousands of years and was previously regarded as a physical necessity rather than a luxury. Most people believe that humans, as all other highly developed tropical animals, have developed a siesta habit as a way of getting around the midday heat. This explanation has also some cultural background as napping is by far less popular in moderate and cold climate. The natural sleep cycle makes you feel less alert in mid-day. This period can easily be visualized using EEG measurements. In tropical countries this is the time for siesta. The drop in alertness is magnified by a rich meal and a short nap is likely to quickly bring you back to full alertness. However, the industrial nations do not seem ready to adopt a healthy habit of postprandial nap.
Advantages of naps:
1) Naps, rich in NREM sleep, result in a significant increase in alertness that will be highly appreciated by people in creative professions.
2) Napping may play a role in memory consolidation (this has not be proved one way or the other).
3) Napping may be a way of combating severe sleep deprivation. Some people even prefer to sleep in two four hour portions throughout their lives!
Disadvantages of siesta:
1) Late naps may worsen insomnia and as such are often discouraged.
2) Long naps (above 60 minutes) may result in temporary grogginess typical of awakening from Stage 4 NREM (so called sleep inertia). As a result, non-nappers and sleep-deprived people will often notice a decline in mental performance after a nap.
3) Long naps (above 60 minutes) can severely worsen insomnia. This is why so many sleep experts counter-recommend naps.
4) Napping requires good rest conditions, as well as solid napping skills and habits that may be difficult to develop for most people in industrial nations.
5) If you nap for more than 50 minutes, you probably need more sleep in the night because such a nap is a likely result of not sticking to the rules of free running sleep and is also likely to disrupt the cycle.
_
Napping less than 45 minutes during the day is not only an effective and refreshing alternative to caffeine, it can also protect your health and make you more productive. NASA has done studies for astronauts and pilots, to determine what the best sleep patterns are to maintain maximum performance. They discovered that after a short nap there was a 34% improvement in performance and 54% in alertness. Although these tests were performed for astronauts, the benefits would apply equally well to any industry. A study of 24,000 Greek adults showed that people who napped several times a week had a lower risk for dying from heart disease. Research (published 2007) by Harvard School of Public Health in the US and the University of Athens Medical School conducted over a 6 year period with 24,000 men and women have found that a short nap in the early afternoon can reduce the risk of heart disease by 34%. People who nap at work have much lower levels of stress. Napping also improves memory, cognitive function and mood. Researchers say daytime sleep has cardiovascular benefits that can help with recovery from mental stress as shown by lower blood pressure. A study, looking at the effect of a daytime nap on cardiovascular recovery following a stress test, found that those participants who slept for at least 45 minutes during the day had lower average blood pressure after psychological stress than those who did not sleep. I recommend a nap of 20 to 45 minutes between 2 pm to 3 pm for people who are regularly woken up at night like medical professionals, police, fire brigade and troops. I myself practice it and it works. I also recommend a nap of 10 to 20 minutes between 2 pm to 3 pm for even those people whose night sleep is not frequently disturbed.
_
Myths about sleep:
Myth 1: Getting just 1 hour less sleep per night won’t effect your daytime functioning.
Fact: You may not be noticeably sleepy during the day. But even slightly less sleep can affect your ability to think properly and respond quickly, and compromise your cardiovascular health, energy balance, and ability to fight infections.
_
Myth 2: Your body adjusts quickly to different sleep schedules.
Fact: Most people can reset their biological clock, but only by appropriately timed cues – and even then, by 1–2 hours per day at best. Consequently, it can take more than a week to adjust after traveling across several time zones or switching to the night shift.
_
Myth 3: Extra sleep at night can cure you of problems with excessive daytime fatigue.
Fact: Not only is the quantity of sleep important but also the quality of sleep. Some people sleep 8 or 9 hours a night but don’t feel well rested when they wake up because the quality of their sleep is poor.
_
Myth 4: You can make up for lost sleep during the week by sleeping more on the weekends.
Fact: Although this sleeping pattern will help relieve part of a sleep debt, it will not completely make up for the lack of sleep. Furthermore, sleeping later on the weekends can affect your biological clock so that it is much harder to go to sleep at the right time on Sunday nights and get up early on Monday mornings.
_
Myth 5: Elderly need less sleep.
Fact: The average adult needs a total sleep time of seven to nine hours per day. While sleep patterns usually change as we age, the amount of sleep we generally need does not. Older people may sleep less at night due, in part, to frequent night waking, but their need for sleep is no less than that of younger adults.
_
Myth 6: Snoring is not harmful.
Fact: Aside from bothering other people, snoring is not harmful but it can be a sign of sleep apnea, a sleep disorder that is associated with significant medical problems.
_
Myth 7: You can “cheat” on the amount of sleep you get.
Fact: Sleep experts say that most adults need between seven and nine hours of sleep each night for optimal health. Getting fewer hours of sleep will eventually need to be replenished with additional sleep in the next few nights. Our body does not seem to get used to less sleep than it needs.
_
Myth 8: Insomnia is characterized only by difficulty falling asleep.
Fact: One or more of the following four symptoms are usually associated with insomnia.
1) Difficulty falling asleep.
2) Waking up too early and not being able to get back to sleep.
3) Frequent awakenings.
4) Waking up feeling unrefreshed.
_
Myth 9: Your brain rests during sleep.
Fact: The body rests during sleep, not the brain. The brain remains active, gets recharged, and still controls many body functions including breathing during sleep.
_
Myth 10: You may loose weight if you get less sleep.
Fact: How much a person sleeps at night can impact their weight. This is because the amount of sleep a person gets can affect certain hormones, specifically the hormones leptin and ghrelin that affect appetite. Leptin and ghrelin work in a kind of “checks and balances” system to control feelings of hunger and fullness. Ghrelin, which is produced in the gastrointestinal tract, stimulates appetite, while leptin, produced in fat cells, sends a signal to the brain when you are full. When you don’t get enough sleep, it drives leptin levels down, which means you don’t feel as satisfied after you eat, and increases ghrelin levels, stimulating your appetite so you want more food. The two combined can set the stage for overeating, which in turn may lead to weight gain. So sleep deprivation leads to weight gain.
_
Myth 11: Daytime sleepiness means a person is not getting enough sleep.
Fact: While excessive daytime sleepiness often occurs if you don’t get enough sleep, it can also occur even after a good night’s sleep. Such sleepiness can be a sign of an underlying medical condition or sleep disorder such as narcolepsy or sleep apnea.
_
Myth 12: If you wake up in the middle of the night and can’t fall back to sleep, you should relax in bed and wait for sleep.
Fact: If you wake up in the night and can’t fall back to sleep within about 15-20 minutes, get out of bed and do something relaxing. Do not sit in bed and watch the clock. Experts recommend reading or listening to music till you feel tired.
_
Myth 13: Napping only makes you more tired.
Fact: Just 10 to 20 minutes is all you need to get the benefits of napping, such as alertness, improved performance, and better mood. However, after about 20 minutes, the sleeping brain may move into what’s called slow-wave sleep, which is the deepest phase of sleep. If you nap too long, you may feel groggy and disoriented upon awakening instead of refreshed because long naps are more likely to contain deep slow-wave sleep. If you do nap, keep it under 20 minutes and between 2 pm to 3:00 pm. If your night sleep is disturbed, nap up to 45 minutes because during such a nap, first REM sleep comes and then NREM sleep as due to night sleep disturbance, our body will not follow normal sleep cycle progression and try to compensate REM sleep first and so you are unlikely to reach slow-wave sleep despite sleeping up to 45 minutes.
_
Myth 14: Go to sleep earlier if you have insomnia.
Fact: A sleep homeostat is a hardwired system controlled by brain chemicals. Our sleep homeostat builds up a hunger for sleep based on how long you’ve been awake and how active you’ve been. When you have insomnia, experts recommend that you let your sleep homeostat adjust itself naturally, without trying to compensate with different bedtimes and catnaps.
_
Myth 15: Skipping a little sleep isn’t that horrible.
Fact: Missing even 90 minutes of sleep for just 1 night can reduce your daytime alertness by as much as 32%. That’s enough to impair your memory, your thinking ability, and your safety on the job and on the road. What’s worse, sleep deprivation also impairs your ability to recognize that you’re not running on all cylinders. In other words, your ability to judge how well you’re doing is probably one of the first things to go when you don’t get enough sleep.
_
Myth 16: Sleeping pills can help you sleep better.
Fact: Sleeping pills can help you sleep, but this sleep is of far less quality than naturally induced sleep. Sleeping pills can be useful in circumstances where sleep is medically vital and cannot be achieved by other means. Otherwise, avoid sleeping pills whenever possible.
_
Myth 17: Avoid naps.
Fact: Naps may indeed worsen insomnia in people suffering from delayed sleep-phase syndrome (DSPS), esp. if taken too late in the day. Otherwise, naps are highly beneficial to intellectual & health performance. It is possible to take a nap in late afternoon before 3 pm without affecting one’s sleeping rhythm. Naps at other times must fall before or inside the so-called dead zone where a nap does not produce a phase response (i.e. shift in the circadian rhythm).
_
Myth 18: Alarm clock can help regulate sleep rhythm.
Fact: Alarm clock can help you push your sleeping rhythm into your desired framework, but it will rarely help you accomplish a healthy sleeping rhythm. The only tried-and-true way to accomplish a healthy sleep and a healthy sleep rhythm is to go to sleep only then when you are really sleepy, and wake up naturally without external intervention.
_
Myth 19: Night shifts are unhealthy.
Fact: People working in night shifts are often forced out of work by various ailments such as a heart condition. However, it is not night shifts that are harmful. It is the constant switching of the sleep rhythm from day to night and vice versa. It would be far healthier to let night shift people develop their own regular rhythm in which they would stay awake throughout the night. It is not night wakefulness that is harmful. It is the way we force our body do things it does not want to do.
_
Myth 20: Being late for school is bad.
Fact: Kids who persistently cannot wake up for school should he left alone. Their fresh mind and health are far more important. Parents who regularly punish their kids for being late for school should immediately consult a sleep expert as well as seek help in attenuating the psychological effects of the trauma resulting from the never ending cycle of stress, sleepiness and punishment.
_
Myth 21: We can adapt to polyphasic sleep.
Fact: We are basically biphasic and all attempts to change the inbuilt rhythm will result in loss of health, time, and mental capacity. A simple rule is: when sleepy, go to sleep; while asleep, continue uninterrupted.
_
Myth 22: Silence and darkness are vital for sleep.
Fact: Silence and darkness may indeed make it easier to fall asleep. They may also help maintain sleep when it is superficial. However, they are not vital. The most important factor that makes us sleep well, assuming good health, is the natural circadian rhythm. People who go to sleep along their natural rhythm can often sleep well in bright sunshine. They can also show remarkable tolerance to a variety of noises (e.g. loud TV, family chatter, outside the window noise, etc.).
_
Myth 23: It is best to wake up with the sun.
Fact: You should wake up at the time when your body decides it got enough of sleep. If this happens to be midday, a curtain over the window will prevent you from being woken up by the sun. At the same time, sun may help you reset your body clock and help you wake up earlier. People who wake up naturally with the sun are indeed among the healthiest creatures on the planet.
_
Myth 24: Sleeping little makes you more competitive.
Fact: It is true that many geniuses slept little. However, the only good formula for maximum long-term competitiveness is via maximum health and maximum creativity. If you sleeps 3 hours per night and enjoys your work, you are likely to run it on alertness hormones (ACTH, cortisol, adrenaline, etc.) also known as stress hormones which will have a consequence of adverse health outcome including a heart attack in your forties.
_
Myth 25: You cannot change the inherent period length of your body clock.
Fact: With various chronotherapeutic tricks it is possible to change the period of the clock slightly. It can be reset or advanced harmlessly by means of melatonin, bright light, exercise, meal timing, etc. It can also be reset in a less healthy way: with an alarm clock.
_
Tips for a good night’s sleep:
1) Set a schedule. Go to bed at a set time each night and get up at the same time each morning. This will help your body to get into a sleep rhythm and make it easier to fall asleep and get up in the morning. Disrupting this schedule on holidays or Sundays may lead to insomnia. Avoid napping during the day except in late afternoon between 2 pm and 3 pm provided you limit the nap to 20 minutes and can sleep well at night.
_
2) Exercise 20 to 30 minutes at least 6 hours before sleeping. Do not exercise immediately before sleep.
_
3) Avoid caffeine, nicotine, and alcohol (vide supra).
_
4) Relax before bed. A warm bath, reading, or another relaxing routine can make it easier to fall sleep. You can train yourself to associate certain restful activities with sleep and make them part of your bedtime ritual.
_
5) Sleep until sunlight. If possible, wake up with the sun, or use very bright lights in the morning. Sunlight helps the body’s internal biological clock reset itself each day. Sleep experts recommend exposure to an hour of morning sunlight for people having problems falling asleep.
_
6) Don’t lie in bed awake. If you can’t get to sleep, don’t just lie in bed. Do something else, like reading, watching television, or listening to music, until you feel tired. The anxiety of being unable to fall asleep can actually contribute to insomnia.
_
7) Control your room temperature. Maintain a comfortable temperature in the bedroom. Extreme temperatures may disrupt sleep or prevent you from falling asleep. The temperature of your bedroom should not be more than 70 degree Fahrenheit (21 degree centigrade).
_
8) Light stimulates the release of cortisol and shuts down the release of melatonin. Make sure there is no light coming from other sources including your windows as this will seriously impair your body’s ability to produce melatonin and avoid all sources of noise. Avoid turning on the light if you have to go to the bathroom. Any bright light will shut off melatonin production.
_
9) Don’t drink any fluids within two hours of going to bed so you won’t have to get up to go the bathroom. Go to bathroom right before bed.
_
10) Take a hot bath 90 to 120 minutes before bedtime; it increases your core body temperature, and when it abruptly drops when you get out of the bath, it signals your body that you are ready for sleep.
_
11) Keep a notepad at your bedside — if you wake in the middle of the night with your mind going, you can transfer your to-do list to the page and return to sleep unworried.
_
12) Eat a handful of walnuts or banana before bed — they’re a good source of tryptophan, a sleep enhancing amino acid.
_
13) Stop watching TV or using your computer by 8 PM. Avoid junk sleep i.e. falling asleep with TV or computer on. Not only do these electronic items make it more difficult to fall asleep, but they also keep you from getting high-quality sleep if you fall asleep with them on.
_
14) Avoid snacking just before bedtime, particularly grains and sugars. These can raise your blood sugar and inhibit sleep. Then later, when your blood sugar drops, you might wake up and not be able to fall back asleep.
_
15) Keep electrical devices as far away from the bed as possible so their electromagnetic fields do not interfere with your nervous system.
_
16) Maintain ideal weight. Being overweight can increase the risk of sleep apnea, which will prevent a restful night’s sleep.
_
17) Remove your clock from view. It will only add to your worry when constantly staring at it…2 AM…3 AM…4:30 AM…
_
18) Get to bed as early as possible. Our systems, particularly the adrenals, do a majority of their recharging or recovering during the hours of 11 p.m. and 1 a.m. In addition, your gallbladder dumps toxins during this same period. Prior to the widespread use of electricity, people would go to bed shortly after sundown, as most animals do, and which nature intended for humans as well.
_
19) One in three couple reports that their partner’s sleep habits affected their own. If your partner is having snoring problem, you may recommend him sleep pillows designed to help prevent snoring by keeping the sleeper’s airway open. Separate beds or blankets can also help couples sleep.
_
20) Take care of several physical factors are known to upset sleep including arthritis, acid reflux with heartburn, menstruation, headaches and hot flashes.
_
21) Remember, many medications can cause sleeplessness as a side effect. Ask your doctor or pharmacist if medications you are taking can lead to sleeplessness.
_
22) If you have a sleeping partner, ask them if they notice any snoring, leg movements and/or pauses in breathing. Take this information and try the sleep test with polysomnography. You may have a sleep disorder or you may just need to increase your awareness about your own sleep need.
_
23) Increase your melatonin. Ideally it is best to increase levels naturally with exposure to bright sunlight in the daytime (along with full spectrum fluorescent bulbs in the winter) and absolute complete darkness at night.
_
24) Encourage your child to fall asleep independently to improve child’s sleep.
_
See a doctor if your sleeping problem continues who could be a family physician or if possible, a sleep specialist.
_
Does oversleeping harm us?
Getting either too much sleep or too little sleep are both out of harmony with a natural circadian rhythm. The study published in the Archives of General Psychiatry, included 1.1 million men and women and found the highest survival rate among those who sleep six to seven hours a night. The survival rate declines progressively among those who sleep eight hours or longer. The study showed people who slept nine or 10 hours per night had a risk of dying similar to that associated with moderate obesity. Risk of death increased by 15 percent for those who slept eight hours a night, 20 percent for those who get 9 hours of sleep and 35 to 40 percent for those who sleep 10 hours a night. In a study of almost 9,000 Americans, researchers found a relationship between oversleeping and the risk of diabetes. People who slept more than nine hours each night had a 50 percent greater risk of diabetes than people who slept seven hours per night. One recent study showed that people who slept for nine or 10 hours every night were 21 percent more likely to become obese over a six-year period. A study from the National Institutes of Health found that those who sleep nine hours or more each night are almost twice as likely to develop Parkinson’s disease as those who sleep six hours or less. A careful analysis of the data from the Nurses’ Health Study, which involved nearly 72,000 women, showed that women who slept nine to 11 hours per night were 38 percent more likely to have coronary heart disease. Another study found that more than 9 hrs/night increases your risk of cardiovascular disease by 50 percent. Roughly 15 percent of people with depression sleep too much. This may in turn make their depression worse, because regular sleep habits are important to the recovery process. Sleeping longer than usual can cause headache. Researchers believe this is due to the effect oversleeping has on certain neurotransmitters in the brain, including serotonin. Multiple studies have found that people who sleep nine or more hours a night have significantly higher death rates.
_
Sleep and poverty:
A study found that children from poorer backgrounds experienced higher levels of delinquency, aggression, anxiety, low self-esteem and depression when they slept poorly. When these children slept better, their levels of symptoms were in line with those of other children from non-poor families. Inadequate sleep, when combined with other stressful influences in the lives of low-income and minority children, contributed to higher levels of behavioral problems. The study suggested that a good night of sleep lessened the likelihood of adjustment problems for these children. The corollary is that when poor people get less sleep due to any cause including poverty itself or poor sleep hygiene due to poverty, they suffer from behavioral problems and poor performance resulting in worsening poverty.
_
Sleep and mosquitoes:
In a developing country like India, mosquitoes are seen everywhere. Fear of mosquito bite, mosquito bite itself and noise generated by mosquitoes can affect sleep. I know many people who just can not sleep if they see even one mosquito. It would be better spending a few minutes or even half an hour in trying to find it and kill it, rather then just not been able to go to sleep for the rest of the night. All measures to prevent mosquito bite right from mosquito net to mosquito repellents to closing windows of bedroom will help you getting good sleep besides protecting from vector-borne diseases.
_
THE MORAL OF THE STORY:
1) It was my ignorance not to discuss sleep for so long when one third of our lives are spent in sleeping.
_
2) Sleep is the most unrecognized and undervalued contributor to optimum heath and performance. Sleep is as important as food, air and water. Those who do not respect their sleep are not likely to live to their full mental and physical potential.
_
3) Sleep deprivation invites diseases and protracted sleep deprivation for years can reduce longevity by about 10 years.
_
4) To stay healthy, make sleep a priority.
_
5) Medical profession, police, fire brigade and military must keep adequate staff to avoid sleep deprivation problems.
_
6) The best sleep is the sleep when you wake up refreshed in the morning without the use of an alarm clock and feel energetic all day.
_
7) Optimum sleep improves memory, learning and creativity; and also prevents reckless decisions.
_
8) Let your body decide when to sleep, how much to sleep and when to wake up.
_
Dr.Rajiv Desai. MD.
March 17, 2011
_
Postscript:
How many people know that 18th march is a world sleep day? World sleep day is designed to raise awareness of sleep as a human privilege that is often compromised by the habits of modern life. My intention is to create awareness about the importance of sleep. Sleep still remains a biological enigma after going through all research work. Many aspects of sleep are contradictory and poorly understood. No doubt, sleep is as essential as oxygen and water. We need more science, more research, and more studies. I have neither laboratory nor funds to conduct research myself.


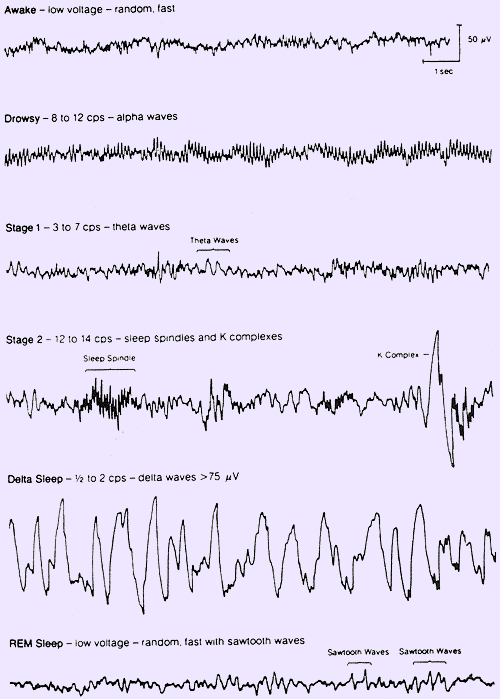
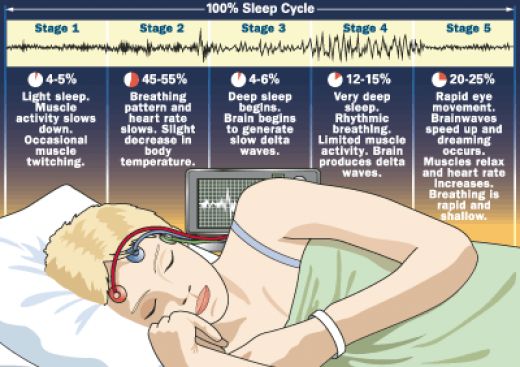
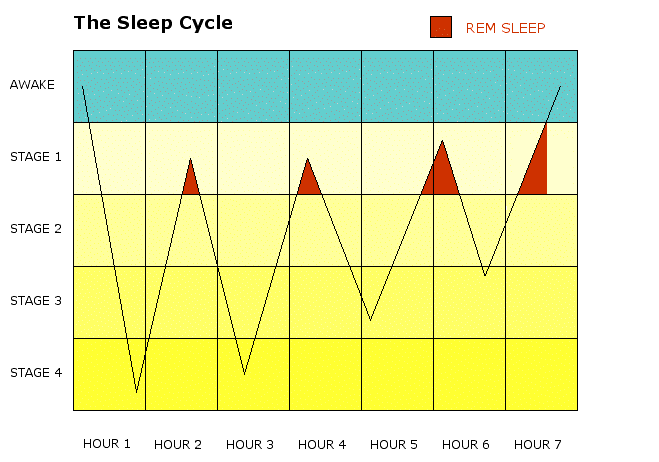
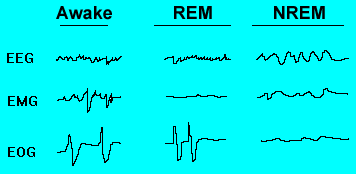
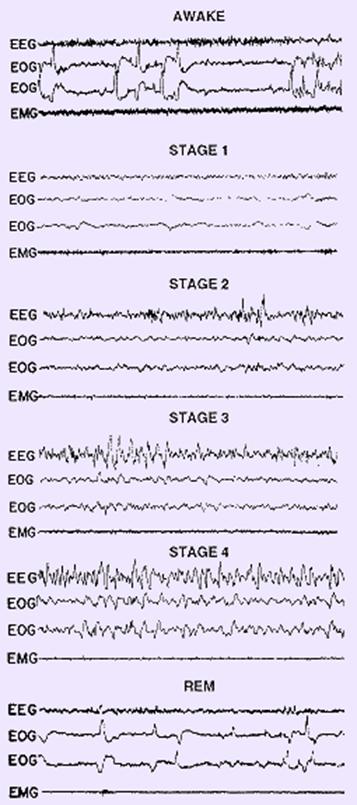
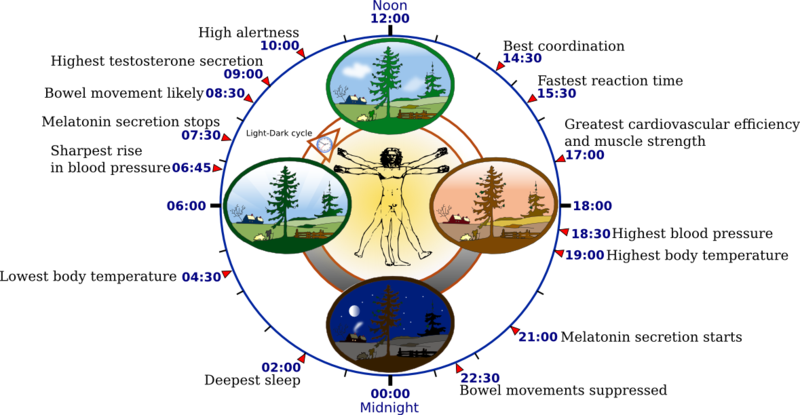
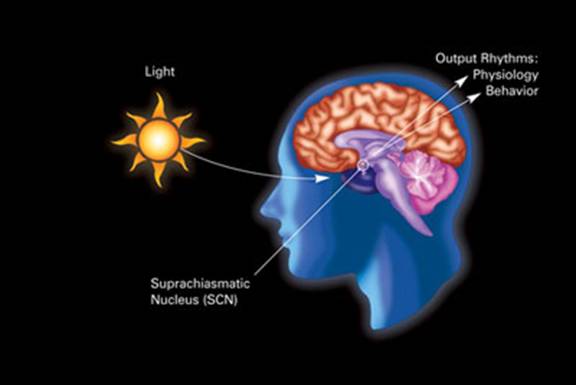
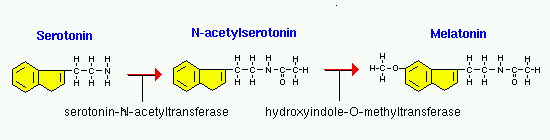
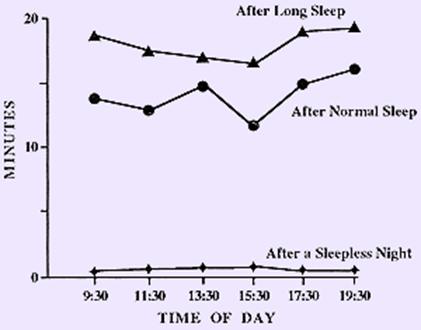
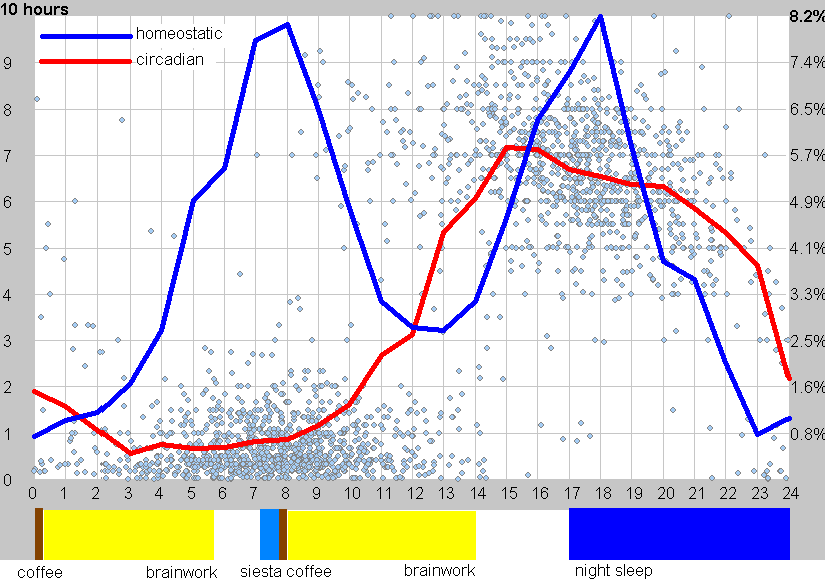
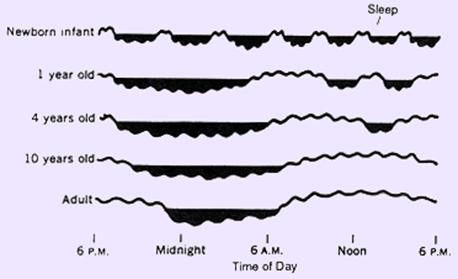
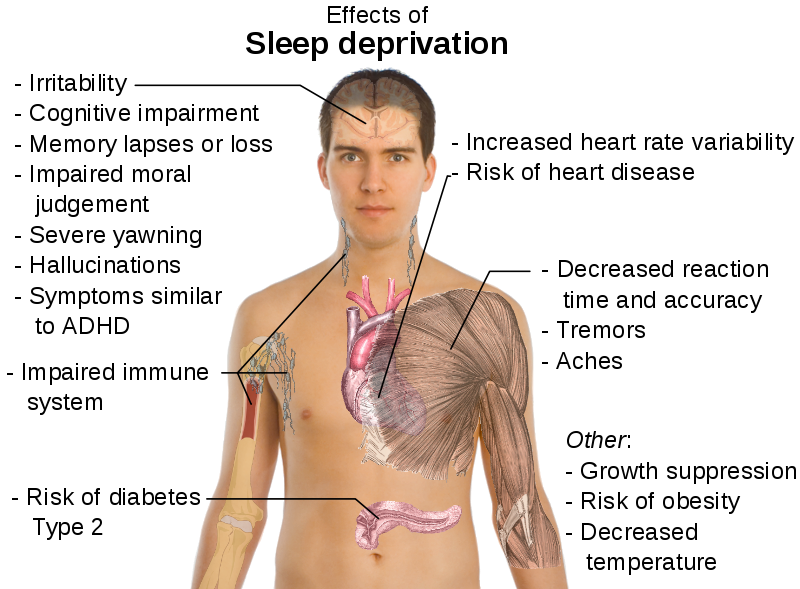
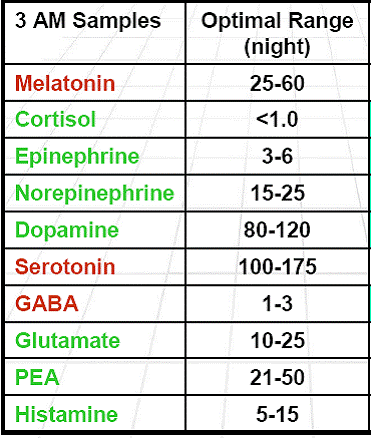
Major thankies for the post. Really Cool.
Your blog post efficiently provided an motivating message to your readers.
You have a fantastic eye for information! You constantly exceed and also past what is anticipated of you.
Sensational is a one-of-a-kind and effective way of living, supplement and also nutrition remedy.
Major thanks for the blog post.Much thanks again. Cool.
These are in fact fantastic ideas in concerning blogging.You have touched some fastidious points here.Any way keep up wrinting.
Really informative blog post. Really Cool.
You’re so cool! I do not believe I’ve truly read through a single thing like this before. So nice to discover somebody with a few original thoughts on this topic. Seriously.. thanks for starting this up. This website is something that is required on the web, someone with some originality!|
I’m not 100 convinced about this post. Your opening points are well structured, but conversely it’s unreliable to rely on what strangers may feel. Please expand this, because I believe you’re a worthy blogger and I would like to see more from you!
Hey! This is my first visit to your blog! We are a collection of volunteers and starting a new initiative in a community in the same niche. Your blog provided us beneficial information to work on. You have done a extraordinary job!|
This is one awesome article post.Much thanks again. Cool.
A round of applause for your article. Will read on…
Looking forward to reading more. Great blog.
“Very informative post. Keep writing.”
Wow, great blog article.Thanks Again. Great.
I cannot thank you enough for the blog post.Thanks Again. Awesome.
One more great benefit of Forskolin for the restless individuals is actually that the preliminary decrease in water weight may trigger a significant difference on the scale as early as the upcoming early morning.
That’s Great but Lyfe Tea worked wonders for me! I lost 8 pounds in two weeks…easy and yummy! Check it out at lyfetea.com